Services on Demand
Article
Indicators
Related links
-
 Cited by Google
Cited by Google -
 Similars in Google
Similars in Google
Share
SAMJ: South African Medical Journal
On-line version ISSN 2078-5135
Print version ISSN 0256-9574
SAMJ, S. Afr. med. j. vol.100 n.2 Pretoria Feb. 2010
ORIGINAL ARTICLES
The consequences upon patient care of moving Brits Hospital: A case study
C A PfaffI; I D CouperII
IMB BCh, MMed (Fam Med), DCH, DA, Dip HIV Man. Centre for Rural Health, University of the Witwatersrand, Johannesburg
IIBA, MB BCh, MFamMed. Centre for Rural Health, University of the Witwatersrand, Johannesburg
ABSTRACT
BACKGROUND: In 2001, North West Province took the decision to increase bed capacity at Brits Hospital from 66 beds to 267 beds. After careful consideration of costs and an assessment of available land, it was decided to demolish the existing hospital and rebuild the new hospital on the same site. It was planned that during this time clinical services would be moved to a temporary makeshift hospital and to primary health care clinics. This case study documents the consequences of this decision to move services to the makeshift hospital and how these challenges were dealt with.
METHODS: A cross-sectional descriptive study was undertaken. Ten key members of staff at management and service delivery level, in the hospital and the district, were interviewed. Key documents, reports, correspondence, hospital statistics and minutes of meetings related to the move were analysed.
RESULTS: The plan had several unforeseen consequences with serious effects on patient care. Maternity services were particularly affected. Maternity beds decreased from 30 beds in the former hospital to 4 beds in the makeshift hospital. As numbers of deliveries did not greatly decrease, this resulted in severe overcrowding, making monitoring and care difficult. Perinatal mortality rates doubled after the move. An increase in maternal deaths was noted. The lack of inpatient ward space resulted in severe overcrowding in Casualty. The lack of X-ray facilities necessitated patients being referred to a facility 72 km away, which often caused a delay of 3 days before management was completed. After-hours X-rays were done in a private facility, adding to unforeseen costs. Although the initial plan was for the makeshift hospital to stabilise and refer most patients, referral routes were not agreed upon or put in writing, and no extra transportation resources were allocated. The pharmacy had insufficient space for storage of medication. In spite of all these issues, relationships and capacity at clinics were strengthened, but not sufficiently to meet the need.
DISCUSSION: Hospital revitalisation requires detailed planning so that services are not disrupted. Several case studies have highlighted the planning necessary when services are to be moved temporarily. Makeshift hospitals have been used when renovating or building hospitals. During war or disasters, plans have been made to decant patients from one facility to another. From the Brits case study, it would appear that not enough detailed planning for the move was done initially. This observation includes failure to appreciate the interrelatedness of systems and the practicality of the proposal, and to budget for the move and not just the new structure.
CONCLUSION: The current service offered at the makeshift hospital at Brits is not adequate and has resulted in poor patient care. It is the result of a planning process that did not examine the consequences of the move, both logistic and financial, in adequate detail. Committed hospital staff have tried their best to offer good care in difficult circumstances.
In 1994, with the advent of democratic rule, South Africa embarked on a review of the national public health care system, including services created under apartheid rule that often did not reflect the service needs of the populations. The review also included a hospital revitalisation programme to upgrade the poor quality of certain health care infrastructure.1
As part of this process, North West Province undertook in 2001 a strategic review of district health services. Brits Hospital is situated in a rural farming and mining community 60 km north-west of Pretoria. It is the only hospital serving the Madibeng municipality, which has a population of about 338 262.2 At the time of the review, Bojanala district (in which Brits Hospital is situated) had 1 280 available beds, often with low rates of usage. The recommendation was to reduce this number to 617 district-level beds, simultaneously re-allocate the beds to correspond with geographical need, and increase Brits Hospital from a 66-bed facility to a 267-bed level 1 district hospital (unpublished data). Owing to the cost of renovating the old building, it was decided that a new hospital should be built. The nearest referral hospital is J S Tabane Hospital in Rustenburg, 72 km away.
Sanitation, water, electricity, other economic development in the area, land ownership, current use and soil type were considered in evaluating various options regarding the location of a future new hospital. It was concluded that the site of the existing hospital was the best location.
It was planned that, during construction of the hospital, clinical services would be moved to a makeshift hospital and to primary health care clinics. The makeshift hospital was to offer a very limited range of services; the casualty department was to stabilise critically ill patients before transferring them; the maternity department was to be for emergency deliveries only; and a short-stay ward was planned for overnight observation, with 15 beds. There were to be no X-ray or theatre facilities. Most outpatients were supposed to be seen in the clinics and not in the hospital. Similarly, most deliveries were to be done at the clinics and not at the hospital.
A nearby building was converted into a makeshift hospital comprising converted rooms for casualty, a labour ward and a maternity ward, a board room, a pharmacy and some offices. Two park homes for use as a sleep-over ward and one for the antiretroviral (ARV) clinic were later added. The move to the makeshift hospital in February 2008 had many unforeseen consequences with regard to clinical care. These are documented so that future hospital revitalisation planning may take note of lessons learned from the Brits case study.
Methods
A report to document the challenges and successes of the move was requested by the North West Provincial Department of Health. A cross-sectional descriptive study was undertaken in July 2009. Ten key members of staff at management and service delivery level, in the hospital and the district, were interviewed. Key documents, reports, correspondence, hospital statistics and minutes of meetings related to the move were analysed. Data were checked with local staff members and the draft report was submitted for comment and correction.
Results
Maternity services
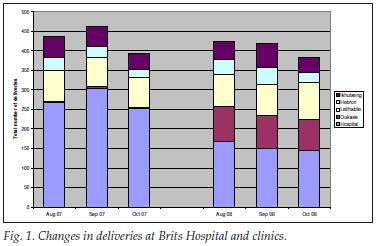
Maternity services were badly affected by the move to the makeshift hospital. The 30-bed maternity ward in the former hospital was reduced to a 4-bed unit in the makeshift hospital - a decrease in bed capacity of 85%. However, deliveries at the hospital only decreased by 30% in spite of deliveries at one clinic increasing from 4 to 84 per month (Fig. 1). As the makeshift hospital had no theatre, patients requiring caesarean section had to be transferred to a level 1 hospital in Gauteng Province (23 km away). Before the signing of a Memorandum of Understanding (MOU) with Gauteng, these patients were transferred to a level 2 hospital in North West (72 km away).
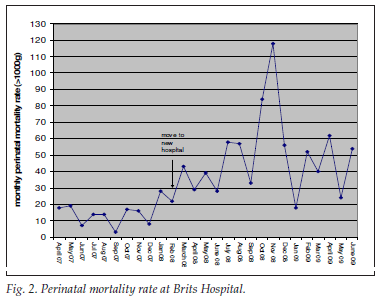
The decrease in beds resulted in severe overcrowding in the hospital maternity ward, with a decreased capacity to care for women and newborns. The perinatal mortality rate doubled after the hospital moved (Fig. 2), intrapartum asphyxia and pre-term labour being significant causes. Care of premature babies was particularly problematic. Maternal deaths also increased after the hospital closure.
Inpatient services
It was planned that the makeshift hospital would only stabilise and refer patients to other facilities and that few would be admitted as sleep-over patients for observation. For several reasons, this did not happen. Referral routes were not agreed upon before the move. The sleep-over beds were used as admission beds for female and paediatric patients. As only two park homes were provided for this service, male patients were supposed to be referred to facilities over 80 km away. Patients often refused to be transferred this distance and insisted on sleeping over in casualty instead, often resulting in severe overcrowding of casualty and patients being nursed on the floor. This problem was eventually resolved after the Department of Health supplied a third park home that was used as a male admission ward in December 2008.
It was planned that the majority of patients would be seen at clinics. Although numbers of patients seen at clinics increased, the numbers of patients seen in casualty did not decrease, further straining services (Table I).

X-ray services
The initial business plan for the makeshift hospital did not provide for X-ray facilities. Instead, patients were to be sent by bus during working hours to a level 2 hospital 72 km away. As patients often had to wait a day for the provided transport and then a day to be seen after their return with a radiograph, their clinical management could take up to 3 days from the time of initial consultation. For emergency X-rays, an arrangement was made with a private health facility. This also caused several critical delays in the care of severely injured patients, who had to wait to be transferred to and from this private facility, often accompanied by a staff member from Brits Hospital, resulting in considerable expense that was not budgeted for. In the 2008/9 financial year, 4 300 X-rays were taken at the level 2 hospital, at a cost of R532 737, and 694 emergency X-rays were done at a cost of R520 072.
Referral pathways
In spite of the plan for the makeshift hospital to stabilise and refer most patients, there was uncertainty at the time of the move around referral routes, with no clear written policy. The initial plan to refer patients to a level 1 hospital 23 km away was complicated by the moving of a provincial boundary. Until an MOU was signed between the two provinces 18 months later, patients were instead transferred to a level 2 hospital in Rustenburg.
Although it was planned that more patients would need transfer, capacity at emergency medical and rescue services (EMRS) was not increased and vehicle numbers remained the same as in 2006. In addition, no extra vehicle was supplied to EMRS for the purpose of transferring patients for X-rays. No addition of suitably trained EMRS staff was made, so that hospital staff were often used to escort patients in ambulances during transfer. Critically injured patients were brought to the hospital in spite of agreements that such patients should be transferred elsewhere, as emergency personnel felt that the distances to other facilities were too great and patients needed stabilisation first.
Pharmacy
The pharmacy in the makeshift hospital was about half the size of the pharmacy in the old hospital, resulting in severe space constraints for storage of medicines; one solution was to build shelves higher, raising concern over safety issues. Boxes were stored in passages, a basement store and a room containing a toilet cistern. Nevertheless, the pharmacy still handled prepackaging and supply to all 25 sub-district clinics, EMRS, old-age homes and the ARV clinic. The pharmacy failed an inspection by the South African Pharmacy Council in 2008.
Staff response
There were many other disruptions to clinical and administrative services. Nevertheless, many staff tried hard to offer care in difficult circumstances. Managers expressed repeated concerns over the situation and tried in many ways to alleviate the pressure. One positive outcome was an improved relationship between the hospital and the clinics, with bimonthly joint management meetings and increased numbers of patients seen at clinic level.
Discussion
A limitation of this case study was incomplete access to all information: many hospital documents were difficult to access and documents could not be found; some hospital computers were faulty; and some maternity statistics were recorded in two places and showed different figures. Background information on decisions taken was not available as several key informants could not be interviewed owing to the high turnover of staff.
Hospital revitalisation requires detailed planning so that services are not disrupted. Moving of services during hospital renovation by making use of a temporary makeshift hospital, as was done at Brits, has been done successfully elsewhere. In 1998, one of the largest hospitals in Malaysia used a mobile surgical unit while its main operating theatres were renovated.3 Similarly, a Malaysian hospital in Kota Kinabalu used container-based operating theatres adjoining the existing theatres while renovating the old theatres and building a new theatre complex.3
However, such processes cannot be undertaken lightly. Case studies have highlighted the planning necessary when services are to be moved temporarily. In renovating the emergency department of the Hospital for Sick Children in Toronto, Canada,4 a dedicated team was formed, representing all departments. The importance of communication was emphasised. The team developed a plan whereby lower-acuity patients were decanted to clinics rather than admitted to the emergency department. Some patients were admitted directly to beds in the wards. The team emphasised the importance of starting to change these processes before the physical space was renovated, to start early and challenge all plans and design processes. Even with this planning, they noted the need to modify the physical design during construction as some impacts of operational changes were discovered during construction. They advised those undertaking similar projects to study the impact of the reconstruction and the resulting gaps more carefully. The timing of the process changes was important.
Similar experiences in Australia highlighted these complexities. At the Orange Base Hospital, during the planning of constructing a new hospital, the responsibilities of the Project Company regarding decanting of patients were clearly written from the start of the project.5 These included meeting with the relevant departments at least 12 months before the decant and ascertaining the specific requirements at all stages. A written decant plan for each department was to be provided to the hospital. The contract stated that it must be ensured that there was no interruption to services at theatres, sterilising, emergency, imaging and intensive care.
In Bathurst, Australia, a new hospital was built and services were to be decanted from the old heritage building to the new hospital, in stages. In this process, a detailed decanting pack was made available to all staff to inform them of the planned changes.6 Recognising their critical role, emergency services and maternity services were the last to be moved, and most other services were to be in place at the time those services were moved. It was made clear that the old building was to be demolished only once all staff had moved into the new hospital. Despite such planning, the transfer of services did not proceed smoothly. At the time of moving, the new hospital was deemed to have serious safety and design flaws. All elective surgery was therefore cancelled and the planned demolition of the old hospital was postponed.7
Hospital reconstruction is not the only scenario where planning for the decanting of patients and moving of services are necessary. In planning for disasters in the UK's West Gloucester region, provisions were made for patients to be decanted to smaller hospitals so as to free beds in the larger hospitals.8 This was to be done by agreed-upon procedures outlined in the major incident plan and included additional resources for transport and management. Decanting was only done in line with the capacity of the smaller hospital to care for such patients.
In other situations, such as epidemics, war or disasters, plans have been made for patients to be decanted and services moved from one facility to another. The BMJ of October 1938 records a plan of being able to clear between 30% and 50% of beds in most hospitals by sending patients home should a disaster occur during a major war.9 The remaining patients were to be decanted to hospitals that were less suitable for receiving air raid victims. Thirty-four hospitals in London were identified for such decanting, and plans were made to move between 3 000 and 4 000 patients by ambulance trains to towns 50 miles or more from London. Transportation arrangements were clear, with exact directions on which trains would be converted and where they would run. There was to be good communication in the referral system, with conferences held with the hospitals to receive patients and decanting proposals explained in detail. Provision was also made to supply these centres with additional equipment and linen.
These cases illustrate the detailed planning required to ensure that services are not interrupted. They emphasise the importance of allocating additional resources during the decanting process. Even where this has taken place certain issues are often not considered and lessons are learnt in retrospect.
From the Brits case study, it appears that there was insufficient initial detailed planning for the move. This included failure to appreciate the inter-relatedness of systems, the impracticality of the proposal and failure to budget for the move to, and not just the additional running costs of, the new structure. It is critical that clinicians are involved in the planning and decision making because of the major consequences of such processes for clinical care.
Conclusion
The current service offered at the makeshift hospital at Brits is inadequate and has resulted in poor patient care. It is the result of a planning process that did not examine the consequences of the move, both logistic and financial, in adequate detail. While the adequacy of care provided by clinical and support staff was not assessed, it would be unfair to hold them solely responsible for the poor outcomes, which might have been worse without the dedication of many of them.
Sincere thanks to staff and management at Brits Hospital and Madibeng sub-district office for their assistance and perseverance in difficult circumstances.
References
1. Health Sector Strategic Framework 1999 - 2004. http://www.doh.gov.za/docs/policy/framewrk/chap03-f.html (accessed 3 November 2009). [ Links ]
2. Statistics South Africa. 2001 Census. http://www.statssa.gov.za/census01/html/ (accessed 2 November 2009). [ Links ]
3. Mobile, modular and expandable health care solutions. http://www.johnsonmedical.com/Mobile%20Solutions%20Brochure.pdf (accessed 11 October 2009). [ Links ]
4. Managing Clinical Process Change during Design, Renovation and Occupancy. http://www.childrenshospitals.net/Content/ContentGroups/EducationMeetings2/Conferences/FacilitiesDesignConference/2009/SessionPresentations/ManagingClinical_presentation.pdf (accessed 11 October 2009). [ Links ]
5. Orange and Associated Health Services PPP Project. Project Deed Schedule 4. Part A - Facility. http://www.health.nsw.gov.au/resources/assets/pdf/ppporange_4parta_policiesandgeneral_v2_3.pdf (accessed 11 October 2009). [ Links ]
6. Questions and answers about the transfer to the new Bathurst health service. http://www.gwahs.nsw.gov.au/userfiles/file/GWAH%20decanting%20low%20res%20for%20web.pdf (accessed 11 October 2009). [ Links ]
7. Bathurst Hospital suspends surgery after safety concerns. http://www.abc.net.au/news/stories/2008/02/18/2165162.htm (accessed 11 October 2009). [ Links ]
8. The West Gloucestershire Primary Care Trust Major Incident Plan (working document). http://www.glospct.nhs.uk/pdf/boardpapers/2008/march/item17_app2.pdf (accessed 11 October 2009) [ Links ]
9. Statement by Ministry of Health. Hospital accommodation for air raid casualties. BMJ 1938;2: 719-720. [ Links ]
Accepted 19 November 2009.
Corresponding author: C A Pfaff (colinpfaff@yahoo.co.uk)














