Services on Demand
Article
Indicators
Related links
-
 Cited by Google
Cited by Google -
 Similars in Google
Similars in Google
Share
SAMJ: South African Medical Journal
On-line version ISSN 2078-5135
Print version ISSN 0256-9574
SAMJ, S. Afr. med. j. vol.99 n.11 Pretoria Nov. 2009
ORIGINAL ARTICLES
Is routine pathological examination required in South African children undergoing adenotonsillectomy?
Anton C van LieropI; C A J PrescottII
IMB ChB, FCORL (SA), MMed (ORL). Division of Otolaryngology, University of Cape Town Medical School
IIMB ChB, FRCS (Eng). Department of Paediatric Otolaryngology, University of Cape Town Medical School
ABSTRACT
OBJECTIVE: We aimed to determine the incidence of abnormal pathological findings in the tonsils and/or adenoids of children undergoing tonsillectomy and/or adenoidectomy, and the incidence of tuberculosis of the tonsils and adenoids; suggest criteria to identify children at risk for adenotonsillar tuberculosis; and investigate the association between HIV and adenotonsillar abnormality, the cost-effectiveness of routine pathological examination of adenotonsillectomy specimens, and criteria to decide which specimens to send for histological examination.
METHODS: We undertook an 8-month prospective study on all children (>12 years) undergoing consecutive tonsillectomy or adenotonsillectomy (T&A) at Red Cross War Memorial Children's Hospital. Patients were assessed pre-operatively and tonsil sizes graded pre- and intra-operatively. Blood was taken for HIV testing, and all tonsils and adenoids were examined histologically. A cost-benefit analysis was done to determine the cost-effectiveness of adenotonsillectomy routine pathology.
RESULTS: A total of 344 tonsils were analysed from 172 children (102 boys, 70 girls); 1 patient had nasopharyngeal tuberculosis, and 1 lymphoma of the tonsils; 13 (7.6%) patients had clinically asymmetrically enlarged tonsils but no significant abnormal pathological finding. The average cost of detecting a clinically significant abnormality was R22 744 (R45 488 ÷ 2 abnormalities).
CONCLUSIONS: The following criteria could improve cost-effectiveness of pathological examination of adenotonsillectomy specimens: positive tuberculosis contact at home, systemic symptoms of fever and weight loss, cervical lymphadenopathy >3 cm, suspicious nasopharyngeal appearance, HIV-positive patient, rapid tonsillar enlargement or significant tonsillar asymmetry. On our evidence, routine pathological investigation for South African children does not seem to be justified.
Tonsillectomy and adenotonsillectomy are commonly performed on children.1 The indications are recurrent tonsillitis, obstructive sleep apnoea, peritonsillar abscess or suspicion of a serious underlying disorder. Tonsillar lymphoma is the major pathology of concern, but in South Africa and other countries with a high incidence of HIV infection adenotonsillar tuberculosis must also be considered.2
Routine histological examination of tonsillectomy and adenoidectomy specimens is performed in many parts of the world so as not to miss rare but significant pathological findings, to serve as a quality control measure, and to teach pathology to residents and fellows.1,3,4 However, the costeffectiveness of this routine examination has been questioned.2-9 Most studies are in developed countries,3,5-9 where the tonsils and adenoids disease spectrum differs from that of developing countries. Because of financial constraints at Red Cross War Memorial Children's Hospital (RCH) in Cape Town, histological analysis is requested only if a high index of suspicion for significant pathology exists. The cost-effectiveness of routine histology on adenotonsillectomy specimens in South African children is unknown.
The high prevalence of tuberculosis and HIV in RCH's Western Cape drainage area make circumstances different to those in developed countries. An HIV-positive patient is 30 times more likely to develop active tuberculosis, once infected. In South Africa, 40% of tuberculosis patients are HIV-positive. The incidence of pulmonary tuberculosis in the Western Cape in 1998 was 430/100 000.10 This figure had risen to 832/100 000 in 2002, owing mainly to the rising incidence of HIV infection. The prevalence of HIV-infected individuals in 2002 in the Western Cape was 12%.
At the turn of the previous century, before the advent of chemotherapy, 1.4% of all adenoids and 6.5% of all tonsils removed from asymptomatic patients were infected by tuberculosis.11 A high index of suspicion is needed to diagnose nasopharyngeal tuberculosis, owing to a lack of clinical signs. Criteria to identify adult patients at increased risk of tonsil malignancies have been suggested,7 and clinical criteria in the paediatric population to identify tonsillar lymphoma have been delineated.12 The risk of lymphoma in HIV-positive patients is 100 times that in the general population. Despite the high incidence of tuberculosis and HIV infection in the Western Cape, the incidence of HIV-related tonsillar abnormalities and adenotonsillar tuberculosis remains largely unknown.
Objectives
We aimed to: (i) describe the incidence of abnormal pathological findings in the tonsils and/or adenoids of children undergoing tonsillectomy or adenotonsillectomy at RCH; (ii) determine the incidence of tuberculosis of the tonsils and adenoids in children of the local population; (iii) suggest criteria to identify children at risk for adenotonsillar tuberculosis; (iv) determine the association between HIV and adenotonsillar abnormalities, including HIV-related lymphomas involving Waldeyer's ring; and (v) determine the cost-effectiveness of routine pathological examination of adenotonsillectomy specimens in our setting, and to suggest criteria to decide which specimens to send for histological examination.
Material and methods
We conducted a prospective study on all children (<12 years) undergoing routine consecutive tonsillectomy or adenotonsillectomy (T&A) at RCH during an 8-month period. We obtained approval from the University of Cape Town ethics committee, and informed consent was obtained for HIV testing. Patients were clinically assessed pre-operatively and the following data collected: indication for surgery, known tuberculosis contacts, constitutional symptoms (weight loss, poor weight gain, fevers), presenting symptoms (nasal obstruction, nasal discharge, sore throat), history of immunocompromise, presence and size of cervical lymphadenopathy, tonsil size, presence of tonsillar asymmetry (left- and right-side tonsils differ in grade), and visible tonsillar lesions.
Tonsil size was graded as follows:13 zero - the patient had a tonsillectomy (not applicable to this study); grade 1 - tonsils are in the tonsillar fossa, barely seen behind the anterior pillars; grade 2 - tonsils are visible behind the anterior pillars; grade 3 - tonsils extend 3/4 to the midline; grade 4 - tonsils completely obstruct the airway (also known as 'kissing' tonsils).
Blood was taken while under general anaesthetic for HIV testing. Intra-operative assessments of tonsillar and adenoidal appearance, size and symmetry and visible lesions were recorded.
Tonsillectomy or adenotonsillectomy was performed by dissection or bipolar diathermy. Specimens were divided and labelled and sent in formalin for histological analysis, and examined macroscopically before haematoxylin-and-eosin (H&E) staining; all were examined by light microscopy.
A cost-benefit analysis was done by multiplying the cost of histological examination of a tonsillectomy and adenotonsillectomy specimen by the number of specimens sent, from which the cost incurred to determine the presence of one clinically significant finding could be determined. Results were considered statistically significant if p<0.05.
Results
A total of 344 tonsils were analysed, from 172 children (102 boys, 70 girls) who had had a tonsillectomy or adenotonsillectomy. The mean age was 5.6 years (range 1 - 12 years). Adenotonsillectomies were performed on 154 (89.5%) children and tonsillectomy alone on 18 (10.5%) children. The clinical findings are summarised in Table I. Ten (5.8%) children had tuberculosis contacts and 4 (2.2%) had been treated for prior pulmonary tuberculosis. Thirteen (7.6%) children had clinically asymmetrical tonsil enlargement. The most common indications for surgery were recurrent tonsillitis (41%), obstructive sleep apnoea (31%), and a combination of the above (19%) (Table II).

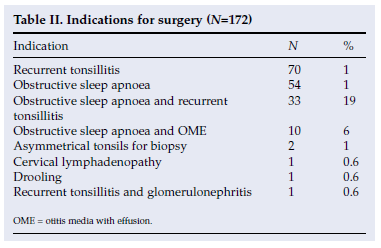
Table III lists the histological findings of the tonsil and adenoid specimens. Reactive lymphoid hyperplasia alone was the histological diagnosis in 139 (61%) patients, of whom 80 (5%) had reactive lymphoid hyperplasia in association with follicle lysis and, of these patients, 50% were HIV-positive (4 HIV-positive patients in total in the study group). Therefore all HIV-positive patients had reactive lymphoid hyperplasia with follicle lysis, on histological examination of the tonsils and adenoids.

Two (1.2%) patients had significant pathological diagnoses - one with nasopharyngeal tuberculosis (tuberculosis of the adenoids), and one with T-lymphoblastic lymphoma of both tonsils and adenoids. The patient with nasopharyngeal tuberculosis had had a positive tuberculosis contact, but no weight loss or fevers. He had cervical lymphadenopathy with bilateral multiple small nodes. His tonsils (grade 2) and adenoids were small. The indication for surgery was recurrent tonsillitis. Histological examination of his adenoids showed caseating and non-caseating granulomas and acid- and alcoholfast bacilli. He was HIV negative, a chest radiograph showed no signs of pulmonary tuberculosis, and the diagnosis was primary nasopharyngeal tuberculosis. He received a full course of antituberculosis treatment.
The patient with tonsillar lymphoma had weight loss, fever, rapid onset of upper airway obstruction, significant cervical lymphadenopathy (nodes >5 cm), and tonsil size grade 4 and clinically symmetrical. The indication for surgery was obstructive sleep apnoea and suspicion of lymphoma. He was also HIV negative, and histological examination revealed a Tcell lymphoma of the tonsils and adenoids.
Four (2.3%) children were HIV positive; 3 were known to be HIV positive before surgery, and only 1 patient (0.6%) was diagnosed on routine testing. The histological finding from all their tonsil and adenoid specimens was reactive lymphoid hyperplasia with follicle lysis.
Clinically asymmetrically enlarged tonsils (traditionally said to be an indication for significant pathology) was present in 13 (7.6%) patients. Neither of the 2 (1.2%) patients with significant pathological diagnoses had clinical asymmetry of the tonsils. We found 20 patients (11.6%) with actinomycosis in the tonsils and adenoids. The pathologist's review of the specimens revealed that in only 1 patient did the presence of actinomycosis evoke a minor cryptitis, and in 3 patients there was an associated acute tonsillitis. There was no specific evidence of tissue reaction to Actinomyces in any of the other specimens (16 patients) reviewed, and their presence was found to be due to colonisation of the tonsils only.
A cost-benefit analysis was done by multiplying the cost of histological examination of a tonsillectomy or adenotonsillectomy specimen by the number of procedures performed. The routine histopathological examination cost of an adenotonsillectomy specimen in the public health sector at the time was R272 (3 blocks for bilateral tonsillectomy and adenoidectomy), and for tonsillectomy alone R200 (2 blocks). The full cost of histological examinations on 154 adenotonsillectomy and 18 tonsillectomy specimens was therefore R45 488. As there were 2 significant pathological findings, the average cost to detect a clinically significant abnormality was R22 744 (R45 488 for 2 abnormalities).
Discussion
Limited resources and finances in the developing world make it impractical to send all adenotonsillectomy specimens for histological examination. Criteria and guidelines, relevant to the specific population, are needed to recognise patients at risk of significant pathology of the tonsils and adenoids, particularly adenotonsillar tuberculosis and lymphoma, and for deciding which adenotonsillectomy specimens to send for further histopathological examination.
Erdag et al. studied the incidence of significant pathology affecting the tonsils and adenoids4 and identified 12 articles of which 5 included only children,1,5,8,9,14 all bar one4 from developed countries. In the series which only included children,4 the incidence of malignancies in tonsillectomy and/ or adenoidectomy specimens varied between 0 and 0.18%; there were 6 cases of significant pathology in 13 360 specimens (incidence 0.04%). The incidence of significant abnormalities in our series was 1.2%, which is 30 times higher than the abovementioned rate. However, the small sample size and the limited time period may not be sufficient to make definitive conclusions.
There were no reported cases of adenotonsillar tuberculosis, which indicates the difference in the spectrum of pathology seen in the developing world. In 22 patients with tonsillar granulomas from 1940 to 1999 in Washington, USA, only 3 had tonsillar tuberculosis;15 this contrasts with 15 Thai patients6 and 20 Chinese patients with nasopharyngeal tuberculosis between 1990 and 2002,17 45 Thai patients with upper aerodigestive tract tuberculosis between 1991 and 2000,18 and 10 patients from Hong Kong with nasopharyngeal tuberculosis.19 Therefore, adenotonsillar tuberculosis remains a disease of the Third World, and criteria are required to identify patients at risk.
Nasopharyngeal tuberculosis may occur as a primary infection without pulmonary or systemic involvement.11,16-22 The most common presenting symptoms are a neck mass, followed by nasal obstruction, nasal discharge, epistaxis, otalgia and hearing loss.11,17-20 In 67 children with tuberculous cervical lymphadenopathy, 18 were found to have nasopharyngeal tuberculosis.20 Although cervical lymphadenopathy commonly accompanies nasopharyngeal tuberculosis, transient cervical lymphadenopathy is common in children. Systemic symptoms of weight loss and fever occur in 12 - 30% of nasopharyngeal tuberculosis patients.17-19 Examination of the nasopharynx revealed no abnormalities in 6 - 30%, although a nasopharyngeal mass or mucosal irregularity may be present.17,18 Lung involvement on chest X-ray is seen in <20% of cases19 and hilar lymphadenopathy in up to 50%.20 Our patient was HIV-negative and had no systemic symptoms, but had nasal obstruction and snoring, bilateral small cervical nodes, and small normal-appearing adenoids. We found a positive tuberculosis contact in the home, which should also be considered a risk factor.
The major pathology of the tonsils of concern in children is tonsillar lymphoma, usually non-Hodgkin's type.23,24 Comparing 46 children with unilateral tonsillar enlargement with 7 children diagnosed with tonsillar lymphoma,12 all the children with tonsillar lymphoma had progressive tonsillar enlargement over a period of 6 weeks or less, and 86% had symptoms including night sweats, fevers, significant cervical lymphadenopathy or hepatosplenomegaly.12 The authors concluded that diagnostic tonsillectomy should be performed in asymmetrically enlarged tonsils only where there is a history of progressive tonsillar enlargement, systemic symptoms, suspicious appearance of the tonsils, cervical lymphadenopathy or hepatosplenomegaly.12
In the only literature on HIV infection and tonsil disease, 45 patients with upper aerodigestive tract tuberculosis in Thailand were reviewed;25 26 had HIV tests and, of these, 5% were HIV-positive.25 All HIV-positive patients had nasopharyngeal tuberculosis. Because extrapulmonary tuberculosis is more common in HIV-positive patients,26 they suggested that all patients with upper aerodigestive tract tuberculosis undergo HIV testing.25
The pathological features of lymphoid tissue in HIV disease in the tonsils and adenoids indicative of HIV infection27 can be divided into early and late stages. In early HIV disease, florid lymphoid hyperplasia is characterised by enlarged and irregularly shaped germinal centres,27 and their surrounding mantle zones are attenuated.27 Small lymphocytes infiltrate the germinal centres, resulting in fragmentation and a moth-eaten appearance to the germinal centres. These changes are referred to as follicle lysis (Fig. 1). Advanced HIV disease includes effacement of the normal lymphoid architecture with absence of germinal centres.27 A dense infiltration of immunoblasts, plasma cells including Russel bodies and mature lymphocytes and a pronounced fibrovascular framework are also present.
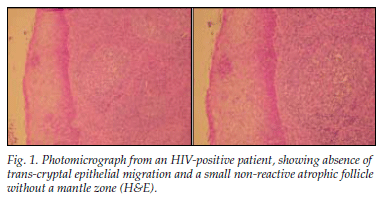
Histological features suggestive of HIV infection were present in 8 of our patients, of whom half were HIV-positive. Therefore, when lymphoid hyperplasia with follicle lysis is reported on pathological examination, patients should undergo HIV testing if their HIV status is unknown, as they have a high probability of HIV infection.
Determining the cost-effectiveness of a treatment or examination requires comparison of investigation cost against the information that can be gained from it. This concept is termed value-based pathology.3,28 Netser et al. conducted a costbenefit analysis of routine versus non-routine tonsillectomy and adenoidectomy specimens over a period of 11 years.3 Of their 2 700 patients, 27 had unusual pathological findings, of which 6 of the diagnoses might have had clinical consequences, but did not. The cost of the 2 700 specimens was $390 482, and no patient's management was affected by the pathology examinations.3
Raab, from a societal point of view, determined that at least 1 in 2 000 examinations would have to show clinically significant disease for histological examination to be costeffective.29 Evaluating routine pathology in other fields, such as appendices and elective joint replacement tissues, has shown similar results.3,30
In our series, R45 488 was the cost of detecting 2 abnormalities, at a rate of 1 significant abnormality in 86 patients. The patient with adenotonsillar lymphoma had a high suspicion for a significant pathological abnormality, and this examination could be termed non-routine. This leaves a rate of 1 in 172 pathological findings (costing R45 488 per significant finding), which affected patient management although it is debatable whether missing the diagnosis might have reduced the patient's life expectancy. Nevertheless, this is higher than Raab's suggested cost-effectiveness threshold,29 therefore implying that routine pathology in our setting may be costeffective but, owing to our small sample size, needs further studies to determine its validity.
Another factor to consider is the possibility of legal action resulting from a missed diagnosis. To determine the costeffectiveness of sending all routine nasal polyps for histology, Diamantopoulos et al. found 22 significant pathological findings in 2 021 polyp specimens.31 On the basis of 250 cases per year, the annual cost of laboratory and pathology services would be £12 000, compared with the estimated average medico-legal cost of £51 000 per year incurred as a result of delay in diagnosis together with resultant pain and suffering. They concluded that, even with the relatively high cost of pathological examinations, routine pathology would be costeffective, considering anticipated medico-legal costs.31 This is also a factor to consider in South Africa, although medico-legal costs are lower than in the UK.
References
1. Strong EB, Rubinstein B, Senders CW. Pathologic analysis of routine tonsillectomy and adenoidectomy specimens. J Otolaryngol Head Neck Surg 2001; 125: 473-477. [ Links ]
2. Ikram M, Khan MA, Ahmed M, Siddiqui T, Mian MY. The histopathology of routine tonsillectomy specimens: results of a study and review of literature. Ear Nose Throat J 2000;79: 880-882. [ Links ]
3. Netser JC, Robinson RA, Smith RJ, Raab SS. Value-based pathology: a cost-benefit analysis of the examination of routine and nonroutine tonsil and adenoid specimens. Am J Clin Pathol 1997; 108: 158-165. [ Links ]
4. Taner K, Erdag M, Cenk Ecevit E, Guneri A, Dogan E, Ikiz AO, Sutay S. Pathologic evaluation of routine tonsillectomy and adenoidectomy specimens in the pediatric population: Is it really necessary? Int J Pediatr Otorhinolaryngol 2005; 69: 1321-1325. [ Links ]
5. Younis RT, Hesse SV, Anand VK. Evaluation of the utility and cost-effectiveness of obtaining histopathologic diagnosis on all routine tonsillectomy specimens. Laryngoscope 2001; 111: 2166-2169. [ Links ]
6. Alvi A, Vartanian A. Microscopic examination of routine tonsillectomy specimens: is it necessary? J Otolaryngol Head Neck Surg 1998; 119(4): 361-363. [ Links ]
7. Beaty MM, Funk GF, Karnell LH, et al. Risk factors for malignancy in adult tonsils. Head Neck 1998; 20(5): 399-403. [ Links ]
8. Dohar JE, Bonilla JA. Processing of adenoid and tonsil specimens in children: a national survey of standard practices and a five-year review of the experience at the Children's Hospital of Pittsburgh. J Otolaryngol Head Neck Surg 1996; 115: 94-97. [ Links ]
9. Garavello W, Romagnoli M, Sordo L, Spreafico R, Gaini RM. Incidence of unexpected malignancies in routine tonsillectomy specimens in children. Laryngoscope 2004; 114: 1103-1105. [ Links ]
10. South African Demographic and Health Survey (1998). Pretoria, Department of Health, 1998: 178. [ Links ]
11. Willams RG, Douglas-Jones T. Mycobacterium marches back. J Laryngol Otol 1995; 109: 5-13. [ Links ]
12. Berkowitz RG, Mahadevan M. Unilateral tonsillar enlargement and tonsillar lymphoma in children. Ann Otol Rhinol Laryngol 1999; 108: 876-879. [ Links ]
13. Friedman M, Tanyeri H, Caldarelli D. Clinincal predictors of obstructive sleep apnea. Laryngoscope 1999; 109: 1901-1907. [ Links ]
14. Williams MD, Brown HM. The adequacy of gross pathological examination of routine tonsils and adenoids in patients 21 years old and younger. Hum Pathol 2003; 34: 1053-1057. [ Links ]
15. Kardon DE, Thompson LD. A clinicopathologic series of 22 cases of tonsillar granulomas. Laryngoscope 2000; 110: 476-481. [ Links ]
16. Chongkolwatana C, Nilsuwan A, Chongvisal S, Keskool P, Metheetrairut C. Nasopharyngeal tuberculosis. J Med Assoc Thai 1998; 81: 329-333. [ Links ]
17. Tse GMK, Ma TKF, Chan ABW, et al. Tuberculosis of the nasopharynx: a rare entity revisited. Laryngoscope 2003; 113: 737-740. [ Links ]
18. Srirompotong S, Yimtae K, Jintakanon D. Nasopharyngeal tuberculosis: manifestations between 1991 and 2000. J Otolaryngol Head Neck Surg 2004; 131: 762-764. [ Links ]
19. Waldron J, Van Hasselt CA, Skinner DW, Arnold M. Tuberculosis of the nasopharynx: clinicopathological features. Clin Otolaryngol 1992; 17: 57-59. [ Links ]
20. Mahindra S, Bazas Malik G, Sohail MA. Primary tuberculosis of the adenoids. Acta Otolaryngol 1981; 92: 173-180. [ Links ]
21. Bath AP, O'Flynn PO, Gibbin KP. Nasopharyngeal tuberculosis. J Laryngol Otol 1992; 106: 1079-1080. [ Links ]
22. Al Serhani AM, Al Rikabi AC, Assiry MA. Primary nasopharyngeal tuberculosis: case report and review of the literature. ENT J 1997; 76: 41-42. [ Links ]
23. Paulsen J, Lennert K. Low-grade B-cell lymphoma of mucosa-associated lymphoid tissue type in Waldeyer's ring. Histopathology 1994; 24: 1-11. [ Links ]
24. Menarguez J, Mollejo M, Carrion R. Waldeyer ring lymphomas. A clinicopathologic study of 79 cases. Histopathology 1994; 24: 13-22. [ Links ]
25. Srirompotong S, Yimtae K, Srirompotong S. Tuberculosis in the upper aerodigestive tract and human immunodeficiency virus coinfections. J Otolaryngol 2003; 32: 230-233. [ Links ]
26. Alpert PL, Munsiff SS, Gourevitch MN, Greenberg B, Klein RS. A prospective study of tuberculosis and human immunodeficiency virus infection: clinical manifestations and factors associated with survival. Clin Infect Dis 1997; 24: 661-668. [ Links ]
27. Wenig BM, Thompson LD, Frankel SS, et al. Lymphoid changes of the nasopharyngeal and palatine tonsils that are indicative of human immunodeficiency virus infection. A clinicopathologic study of 12 cases. Am J Surg Pathol 1996; 20: 572-587. [ Links ]
28. Fechner RE. Value-based surgical pathology: a valuable concept. Am J Clin Pathol 1997; 108: 123-126. [ Links ]
29. Raab SS. The cost-effectiveness of routine histologic examination. Am J Clin Pathol 1998; 110: 391-396. [ Links ]
30. Grzybicki DM, Callaghan EJ, Raab SS. Cost-benefit value of microscopic examination of intervertebral discs. J Neurosurg 1998; 89: 378-381. [ Links ]
31. Diamantopoulos II, Jones NS, Lowe J. All nasal polyps need histological examination: an audit-based appraisal of clinical practice. J Laryngol Otol 2000; 114: 755-759. [ Links ]
Accepted 24 July 2009.
Corresponding author: A C van Lierop (antonvl@worldonline.co.za)














