Services on Demand
Article
Indicators
Related links
-
 Cited by Google
Cited by Google -
 Similars in Google
Similars in Google
Share
SAMJ: South African Medical Journal
On-line version ISSN 2078-5135
Print version ISSN 0256-9574
SAMJ, S. Afr. med. j. vol.99 n.10 Pretoria Oct. 2009
SCIENTIFIC LETTERS
Effectiveness of community participation in tuberculosis control
T N AchokiI; C ShilumaniII; A BekeIII
IMB ChB, MPH, DTM&H. School of Health Systems and Public Health, University of Pretoria
IIBSc, MPH. School of Health Systems and Public Health, University of Pretoria
IIIMB ChB, MMed, DTM&H, DPH, DHSM, DOH. School of Health Systems and Public Health, University of Pretoria
To the Editor: Tuberculosis (TB) has re-emerged as an important global public health issue, particularly with the advent of HIV and AIDS.1-3 Sub-Saharan Africa has the highest incidence of TB in the world, estimated at over 350 cases per 100 000.1 With many of its provinces being rural and characterised by limited access to health services, South Africa ranked fifth globally among high TB burden countries in 2007.4 In low-resource settings where health systems barely cope with increased disease burdens, community participation has come to the fore as a pivotal measure for successful programming.
We sought to evaluate the performance of a community-based TB project piloted in a rural sub-district in the Eastern Cape province of South Africa. The project, implemented by an international non-governmental organisation (NGO) over 2 years, had the key objective of achieving the global target of an 85% treatment success rate1 among TB patients registered in the sub-district. It mainly comprised advocacy measures to increase community awareness on aspects of TB control which, it was envisaged, would enhance treatment-seeking behaviours at individual, household and community levels. It was implemented in close collaboration with community entities such as rural clinics, local schools and civil society organisations (CSOs). The CSOs received support to initiate community microprojects such as community gardens to enhance nutrition among affected communities, TB contact and defaulter tracing to improve adherence to treatment, and smoking cessation campaigns. However, in undertaking these activities there was little focus on the other technical components of an effective TB programme, such as quality microscopy, timely recording and reporting.
A total of 463 new TB patients were registered in the pilot sub-district over the 2-year period, 145 in 2004 and 318 in 2005, representing a >100% increase in new caseload without any reported exogenous contributory factor other than the introduction of the community project. A comparable neighbouring sub-district (N=631) registered an increase of only 3.0% during this time.
The average age of the patients was 38.0 years (95% confidence interval (CI) 36.52 -39.45). Males were older, with a mean age of 40.5 years (95% CI 38.56 -42.3 years) compared with 34.9 years (95% CI 32.7 - 37.2) for females. For both genders the age category with the highest proportion of patients was between 15 and 54 years; females peaked at 15 - 44 years and males at 25 -54.
We used data from the pilot sub-district's electronic TB register to analyse the quarterly performance of successive treatment cohorts and made comparisons over the period between quarter 1, 2004 and quarter 4, 2005. Bacteriological coverage declined from 80% to 50%, new smear conversion rates dropped from 60% to 30%, and treatment success rate dropped from 60% to 38%. TB patients reported as 'not evaluated' increased to 45% in quarter 4, 2005, from insignificant proportions reported in the preceding quarters.
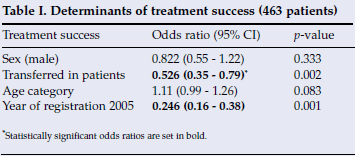
Analysing determinants of treatment success revealed that patients registered in 2005 were 75.4% less likely to achieve treatment success than those in 2004. Similarly, patients who transferred into the treatment centres located in the pilot sub-district during the same period were less likely to be successfully treated (Table I).
We are cognisant of limitations in this evaluation. Reliable causal inference to a specific intervention as responsible for the changes observed was difficult for a descriptive study of this nature. Reliance on secondary data, the quality of which cannot be readily ascertained, is also a weakness. However, attempts were made to mitigate for quality issues through rigorous data cleaning and collation before analysis.
We conclude that community participation alone is inadequate to improve the performance of a TB control programme. Planning a holistic and comprehensive approach should seek to strengthen the programme's technical and organisational capacity5 before engaging in purely community interventions. Failure to observe this logical relationship would result in suboptimal performance. Efforts to increase demand for health services should be cognisant of the health system capacity.
We recommend further research and sharing of best practices and evidence-based approaches of harnessing community-based interventions to improve health outcomes.
MEASURE Evaluation Fellowship Program provided financial support. The authors thank the Eastern Cape Provincial Department of Health staff for their assistance.
References
1. World Health Organization. Global Tuberculosis Control Report: Surveillance, Planning, Financing. 2007. http://www.who.int (accessed 17 November 2007). [ Links ]
2. World Health Organization (2003). Treatment of Tuberculosis: Guidelines for National Programmes. 2003. http://www.who.int (accessed 17 November 2007). [ Links ]
3. Department of Health (2000). The South African Tuberculosis Control Programme: Practical Guidelines. Available at http://www.doh.org.za (accessed 12 June 2006). [ Links ]
4. World Health Organization. Global Tuberculosis Control: Epidemiology, Strategy, Financing. 2009. http://www.who.int/tb/publications/global_report/en/index.html (accessed 9 May 2009). [ Links ]
5. World Health Organization. Community Contribution to TB Care: Practice and Policy. 2003. http://www.who.int (accessed 17 November 2007). [ Links ]
Accepted 27 May 2009.
Corresponding author: T N Achoki (n_achoki@yahoo.com)














