Servicios Personalizados
Articulo
Indicadores
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares en Google
Similares en Google
Compartir
SAMJ: South African Medical Journal
versión On-line ISSN 2078-5135
versión impresa ISSN 0256-9574
SAMJ, S. Afr. med. j. vol.99 no.9 Pretoria sep. 2009
ORIGINAL ARTICLES
Allergenicity of latex rubber products used in South African dental schools
Dikeledi O MabeI,*; Tanusha S SinghII; Braimoh BelloIII; Mohammed F JeebhayIV; Andreas L LopataV; Ahmed WadeeVI
IMSc (Med), National Institute for Occupational Health, Johannesburg
IIMSc (Med), National Institute for Occupational Health, Johannesburg
IIIMSc (Epidemiol), National Institute for Occupational Health, Johannesburg
IVMB ChB, PhD, Centre for Occupational and Environmental Health Research, School of Public Health and Family Medicine, University of Cape Town
VPhD, Department of Immunology, University of Cape Town, and School of Applied Sciences, Allergy Research Group, Royal Melbourne Institute of Technology (RMIT), Melbourne, Australia
VIPhD, School of Pathology, University of the Witwatersrand, and Department of Immunology, National Health Laboratory Services, Johannesburg
ABSTRACT
BACKGROUND: Latex sensitisation is recognised as a health problem among health care workers (HCWs) using latex products. The aim of this study was to quantify specific latex allergens in latex devices used in South African academic dental schools. The current study also compared the total protein content and the levels of specific allergens in these products.
METHODS: Fourteen latex examination gloves (powdered and non-powdered) and five dental rubber dams, representing 6 brands, from five dental academic institutions were analysed for latex allergens and total protein. Total protein content was determined using the BioRad DC protein assay kit and natural rubber allergen levels using a capture enyme-linked immunosorbent assay (ELISA) specific for Hev b 1, Hev b 3, Hev b 5 and Hev b 6.02.
RESULTS: Hev b 6.02 was found in higher concentrations than other natural rubber latex (NRL) allergens in the products analysed. Hev b 5 content ranged from 0 to 9.2 µg/g and Hev b 6.02 from 0.09 to 61.5 µg/g of sample. Hev b 1 levels were below the detection limit (DL) for 79% of the samples (15/19). Dental dams showed higher allergen levels (median 80.91 µg/g) than latex gloves (median 11.34 µg/g). Powdered rubber samples also showed higher allergen levels (median 40.54 µg/g) than non-powdered samples (median 5.31 µg/g). A statistically significant correlation was observed between total protein and total allergen (r=0.74, p<0.001) concentrations.
CONCLUSION: NRL allergen concentrations differ significantly by product and brand. This study has demonstrated that NRL allergens in latex-containing products used in South African dental institutions are present at sufficiently high levels to pose an allergic health risk.
Latex allergy is an occupational health problem among health care workers (HCWs), including dental health care professionals. Our aim was to quantify individual latex allergens to assess the allergenicity of latex products used in health care settings, to minimise the risk of sensitisation to these proteins.
Background
Allergens from latex products in health care settings are known to trigger latex-induced allergic reactions in HCWs. Adverse effects associated with the use of latex rubber products have been reported, ranging from rhinitis and conjunctivitis to life-threatening anaphylactic reactions,1 with a reported prevalence of 3 - 17% among HCWs.1,2 We investigated the latex allergen content in various rubber products used in dental schools at public health care institutions in South Africa.
Methods
Fourteen latex examination gloves (powdered and non-powdered) and 5 dental rubber dams, representing 6 brands, were obtained from 5 South African public sector academic dental institutions. The samples were cut into small pieces, weighed, extracted in phosphate-buffered saline with 0.1% Tween 20 (1:5 w/v) at pH 7.4 and centrifuged before analysis. Total protein content was determined using the Bio-Rad DC protein assay kit (Bio-Rad, Hercules, USA) and natural rubber allergen levels using a capture enzyme-linked immunosorbent assay (ELISA) (FITBiotech, Tampere, Finland) specific for Hev b 1, Hev b 3, Hev b 5 and Hev b 6.02. Data analysis was performed using STATA 9 computer software (StataCorp, 1984-2007, Texas, USA). Since the data had a skewed distribution, non-parametric tests were applied at an alpha level of 0.05.
Results
Hev b 6.02 was detected in all gloves and rubber dam samples, while Hev b 1 was only detected in 4 of the 5 rubber dam samples (Table I). The total protein content could only be measured in 12 samples and was below the detection limit (700 µg/g) for the remaining 7 (37%) extracts. The total allergen concentrations (µg/g) represented the sum of the 4 allergens analysed. Total allergen content of latex products was categorised as low (0.15 µg/g), moderate (>0.15 µg/g and <1.15 µg/g) and high (>1.15 µg/g).3
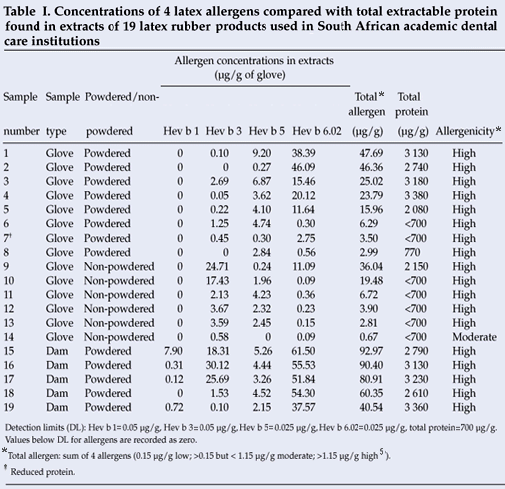
Allergen concentrations among different latex products differed significantly in Hev b 1 (p< 0.001) and Hev b 6.02 (p=0.0022) between gloves and dental rubber dams. Similarly, there was a significant difference (p=0.035) in allergen concentrations between powdered (median = 40.54 µg/g) and non-powdered (median = 5.31 µg/g) products. Total allergen from the 6 branded latex products also showed a significant difference (p=0.022) between products. Hygenic brand had the highest concentrations (median = 80.91 µg/g), followed by Medtex (median = 24.40 µg/g), Examtex (median = 11.34 µg/g), Evergreen (median = 36.04 µg/g), Afrika (median = 6.29 µg/g), and LSP E.Z. Fit Ultra (median = 2.09 µg/g). There was a high correlation between total allergen and total protein content in the latex rubber products analysed (r=0.74, p<0.001).
Discussion
Ours was the first systematic study to quantify latex allergen content in latex products used in dental health care settings in South Africa. While 37% of samples obtained from products were below the detection limit (DL) for total protein, they had lower total allergen concentrations, but were still in the 'high allergenicity' category of natural rubber latex (NRL) allergen content. These findings suggest that measuring protein alone is not useful for latex products containing proteins <700 µg/g of sample as the allergen content will be underestimated. Previous studies showed that the total protein levels of NRL gloves do not necessarily correlate with allergen content.4 However, a significant correlation between total allergen and total protein shown in this study suggests that total protein can be used to screen for indirect estimation of the allergenicity of latex products, especially in under-resourced countries, as this assay is more cost-effective than the capture-ELISA. However, the limitation of the protein assay method is that it cannot differentiate between allergenic and non-allergenic proteins,5 whereas the allergen content provides better insight into the concentrations of NRL allergenic proteins.
The allergenicity of NRL products can be estimated by measuring the levels of 4 allergens (Hev b 1, Hev b 3, Hev b 5 and Hev b 6.02)1,3 as used in our study. Yeang et al. suggested that Hev b 13 (combined with Hev b 5) could be used as allergen markers to estimate glove allergenicity.6 However, Hev b 13 was not measured in our study as it was not included in the available assay kit used for the product analysis. Furthermore, Hev b 1 could not be detected in gloves but was detectable in all dental rubber dams analysed. Hev b 1 was demonstrated to be the dominant allergen in latex gloves used by medical personnel in Taiwan.4 Hev b 5 and Hev b 6.02 allergens, which have been detected in gloves of HCWs,3 were present in all the samples in our study. The reported concentrations of Hev b 6.02 were generally higher compared with other allergens.3 All our samples exceeded the recommended cut-off limit by Palosuo et al. of 0.15 µg/g for low-allergenic gloves using the sum of 4 allergens, indicating that potentially there is a high risk of sensitisation to latex in South African dental workers using these products.3 Surprisingly, product 7, which declared on its packaging that it had reduced protein, confirmed that total protein content was<DL; however, the total allergen content was 3.5 µg/g for this sample, well above the 1.15 µg/g level indicative of high allergenicity. This observation confirms reports that some products have low extractable proteins but high allergenic proteins, and vice versa.2
Our study confirms studies demonstrating that latex allergen content is higher in powdered (P) gloves than in non-powdered (NP) gloves.7 Although NP gloves have a lower concentration of NRL allergens, they may be high enough to cause sensitisation, since 83% of these products tested are classifiable as being of high allergenicity and 17% of moderate allergenicity (Table I).
Our findings support reports showing significant differences in NRL allergen levels among different medical glove brands.2,7 We found the highest total allergen content in Medtex gloves and moderate content in LSP E.Z. Fit Ultra gloves. The higher NRL allergen content of the Hygenic brand in this study indicates that dental rubber dams can also pose an unexpected health risk to dental HCWs and patients. Owing to the absence of a global standard, safety claims would be premature. Nevertheless, it is probable that the sum of certain NRL allergens will be a useful practical guide to personnel responsible for glove purchasing in health care settings and to glove users in supporting their glove selections.
Conclusion
We demonstrated that NRL gloves used in dental health care settings in the public sector contain allergenic levels high enough to cause latex allergy. They continue to be used in the South African health care setting despite global initiatives to move away from such products. Dental staff can also be exposed to latex aeroallergens from powdered dental rubber dams that are usually stretched when used during dental procedures, so increasing the aerosolisation of NRL particles.8 International recommendations to use non-powdered low-protein latex products are poorly supported in South Africa, resulting in continued locally reported latex allergy compared with industrialised countries where the epidemic has abated.
We thank the Allergy Society of South Africa (ALLSA) and the Medical Research Council (MRC) of South Africa for funding this project, and academic dental institutions in South Africa for providing the latex products.
References
1. Koh D, Ng V, Leow YH, Goh CL. A study of natural rubber latex allergens in gloves used by healthcare workers in Singapore. Br J Dermatol 2005; 15: 954-959. [ Links ]
2. Palosuo T, Alenius H, Turjanmaa K. Quantitation of latex allergens. Method 2002; 27: 52-58. [ Links ]
3. Palosuo T, Reinikka-Railo H, Kautiainen H, et al. Latex allergy: the sum quantity of four major allergens shows the allergenic potential of medical gloves. Allergy 2007; 62: 781-786. [ Links ]
4. Lee M-F, Chen Y-H, Lin H-C, et al. Identification of Hevamine and Hev b 1 as major latex allergens in Taiwan. Int Arch Allergy Immunol 2006; 139: 38-44. [ Links ]
5. Audo C, Barbara J, Chabane H, et al. The en 455-3 modified Lowry assay does not yield a reliable estimate of the allergenicity level of latex gloves with low total protein content. Med Sci Monit 2004; 10 (7): 181-186.6. [ Links ]
6. Yeang H-Y, Arif SAM, Raulf-Heimsoth M, et al. Hev b 5 and hev b 13 as allergen markers to estimate the allergenic potency of latex gloves. J Allergy Clin Immunol 2004; 114: 593-598. [ Links ]
7. Kujala V, Alenius H, Palosuo T, et al. Extractable latex allergens in airborne glove powder and in cut glove pieces. Clin Exp. Allerg 2002; 32: 1077-1081. [ Links ]
8. Jones KP, Rolf S, Stingl C, et al. Longitudinal study of sensitization to natural rubber latex among dental school students using powder-free gloves. Ann Occup Hyg 2004; 5: 455-457.10. [ Links ]
Accepted 26 June 2009.
* Corresponding author: Dikeledi O Mabe (onnicah.mabe@nioh.nhls.ac.za)














