Services on Demand
Article
Indicators
Related links
-
 Cited by Google
Cited by Google -
 Similars in Google
Similars in Google
Share
SAMJ: South African Medical Journal
On-line version ISSN 2078-5135
Print version ISSN 0256-9574
SAMJ, S. Afr. med. j. vol.99 n.9 Pretoria Sep. 2009
ORIGINAL ARTICLES
Quality of cause of death certification at an academic hospital in Cape Town, South Africa
Beatrice NojilanaI,*; Pam GroenewaldII; Debbie BradshawIII; Gavin ReagonIV
IMPH, Burden of Disease Research Unit, Medical Research Council Tygerberg, W Cape
IIMB ChB, MPH, Burden of Disease Research Unit, Medical Research Council Tygerberg, W Cape
IIIDPhil (Oxon), Burden of Disease Research Unit, Medical Research Council Tygerberg, W Cape
IVMB ChB, FCPHM, School of Public Health, University of the Western Cape, Bellville, W Cape
ABSTRACT
OBJECTIVES: To investigate the quality of cause of death certification and assess the level of under-reporting of HIV/AIDS as a cause of death at an academic hospital.
DESIGN: Cross-sectional descriptive retrospective review of death notification forms (DNFs) of deaths due to natural causes in an academic hospital in Cape Town during 2004. Errors in cause of death certification and ability to code causes of death according to the 10th revision of the International Statistical Classification of Diseases and Related Health Problems (ICD-10) were assessed. The association between serious errors and age, gender, cause of death and hospital ward was analysed. A sample of DNFs (N =243) was assessed for level of under-reporting of HIV/AIDS.
RESULTS: A total of 983 death certificates were evaluated. Almost every DNF had a minor error; serious errors were found in 32.2% (95% confidence interval (CI) 29.3 - 35.1%). Errors increased with patient age, and cause of death was the most important factor associated with serious errors. Compared with neoplasms, which had the lowest error rate, the odds ratios for errors in endocrine and metabolic diseases and genito-urinary diseases were 17.2 (95% CI 8.7 - 34.0) and 17.3 (95% CI 7.8 - 38.2), respectively. Based on the sub-sample, the minimum prevalence of HIV among the deceased patients was 15.7% (95% CI 11.1 - 20.3%) and the under-reporting of deaths due to AIDS was 53.1% (95% CI 35.8 - 70.4%).
CONCLUSION: Errors were sufficiently serious to affect identification of underlying cause of death in almost a third of the DNFs, confirming the need to improve the quality of medical certification.
South Africa has a well-established system for vital registration and collection of mortality statistics, but is challenged by under-reporting of death statistics, particularly in rural areas and of young children.1 The quality of medical certification and misclassification of causes of death are also of concern.2-5 Errors could result from difficulties in clinical diagnosis, poor certification or statistical coding and data processing.6
Efforts have been made to improve cause of death information by standardising the reporting and coding of cause of death through the 10th revision of the International Statistical Classification of Diseases and Related Health Problems (ICD-10).7 This defines the underlying cause of death as the condition or injury that started the sequence of events leading directly to death and provides a standard format for medical certification on the death notification form (DNF). The DNF allows for four lines of information (labelled line a to line d in part I) on the causal sequence leading from the underlying cause to the immediate cause of death. The immediate cause should be listed in line a and the underlying cause on the lowest line. Contributory causes can also be listed in a second part (part II).
The underlying cause, which is extremely relevant for public health, should be a distinct entity on the DNF and aetiologically specific.8 South Africa adopted the international format of medical certification in the new DNF, the BI-1663,9 as part of revitalising death registration. Whether the death was natural or unnatural must also be indicated. Correct diagnosis and certification of the cause and manner of death are major determinants of the accuracy and completeness of mortality statistics. Problems in the quality of cause of death certification in South Africa have been identified.2,3,10
We aimed to quantify the extent and identify the types of errors in death certification that occurred at an academic hospital in Cape Town in order to improve its cause of death certification, and highlight concerns that these errors might be arising more generally. We assessed the ICD-10 codability of the information provided by doctors, the extent to which errors in certification of the cause of death were made, and the level of under-reporting of HIV/AIDS as a cause of death.
Methods
Study design and population
A retrospective cross-sectional descriptive study of death notifications and a sample of medical records was conducted at a tertiary hospital in Cape Town. Unnatural deaths were excluded because their DNFs are completed by a forensic pathologist, with additional information from an autopsy.
Ethics approval was obtained from the University of Cape Town and University of the Western Cape ethics committees.
Sample size and sampling
All DNFs from 1 January 2004 to 31 December 2004 were included. A sub-sample of the natural deaths was selected to assess completeness of the reporting of HIV/AIDS on DNFs. Using Epi-Info a sample size of 243 was estimated to provide an error margin of 10% at a 95% confidence level if the proportion of AIDS deaths with HIV indicated on the death notification was 30%. A systematic sample was drawn.
Data collection and processing
Information on age, sex, causes of death on the death notification and the ward where the patient died was collected. Cause of death information was processed using the Super Mortality Medical Indexing, Classification and Retrieval system (SuperMICAR) of the USA National Center for Health Statistics (NCHS) for coding of causes of death to ICD-10. Some records were rejected by SuperMICAR as being inadequate for coding to ICD-10, e.g. unknown abbreviations or use of the word 'pre-existing' in front of conditions. The cause of death specified on each line of the DNF was assessed as codable, or codable with difficulty (cause of death inadequate for coding and needed some modification to suit the ICD-10 rules, e.g. use of abbreviations, or two causes written on one line, or use of non-ICD nomenclature), or not codable (diagnosis vague and no ICD-10 code could be assigned).
Errors in cause of death certification were identified once the data had been processed using the NCHS Automated Classification of Medical Entities (ACME), the 'de facto' international standard for the selection of the underlying cause of death.6 Cases rejected by ACME were reviewed and the nature of the error on the DNF was assessed as major or minor, using adapted criteria.11-13 Errors were classified as major if they could have an impact on the identification of the underlying cause of death (underlying cause missing, competing potential underlying causes or improper sequencing) and minor if less likely to do so (use of abbreviations, absences of time interval, use of mechanism but with an underlying cause, underlying cause not specific enough). 'Serious major errors' included no acceptable underlying cause of death, competing causes and mechanisms without underlying cause, as such errors could prevent the correct identification of the leading causes of death.
Sub-sample review of HIV status in medical folder
Medical records of a sub-sample of deaths were reviewed to check whether HIV status or AIDS was recorded. We calculated the proportion of cases that were potentially due to AIDS and had HIV positive recorded on their medical records, and those that had AIDS reported on the DNF. Deaths potentially due to AIDS were infectious and parasitic communicable diseases (A00-B99, G00-G03); maternal and perinatal conditions (P05-P94); nutritional deficiencies (E40-E46, D50-D56); selected respiratory conditions, i.e. pneumoconiosis, pharyngitis, chronic rhinitis, chronic nasopharyngitis, adult respiratory distress syndrome, pleural conditions, peritonsillar abscess, chronic sinusitis disease of tonsils and adenoids (J10-J18, J20-J22, J86); other non-infectious gastro-enteritis and colitis (K52, K52); and selected cancers, i.e. vulval cancer, cervical cancer, Kaposi's sarcoma and non-Hodgkin's lymphoma (C46-C46, C51-C54, C81-C90, C97).
Statistical analysis
Descriptive statistics and 95% confidence intervals (CIs) were calculated for key proportions. A chi-square test was used to compare the sex distribution of deaths by ward and whether certain factors influenced the frequency of minor and major errors. Logistic regression analysed the association between various factors and serious major errors. Variables included were sex, age, ward, and the underlying causes.
Results
Response rate
In 2004, 1 523 deaths occurred. Of these records, 12 were duplicates and 161 were missing, leaving 88.6%. Of the remaining records 356 were due to unnatural causes and excluded; 994 deaths were from natural causes, but 11 (1.1%) contained no information about cause of death, leaving 983 natural deaths for analysis.
Basic characteristics
Of the deceased 51% were female. The median age at death was 57.9 years; 34.3% were aged ≥65, and 2.0% were neonates. The few deaths in those younger than 25 years reflect the fact that children are generally not treated at this hospital. Most deaths were in the age groups 55 - 64 years (22.2%) and 65 - 74 years (20.1%). On about 34% of the DNFs only a single cause of death was reported. On 12% of the DNFs a cause was listed on all four lines provided in part I, and in 13% a cause was listed in the section for contributory causes (part II). The underlying cause of death profile is presented in Table I by ICD-10 chapter.

Codability of information to ICD-10
Most causes (83.3%) (95% CI 81.7 - 84.8%) could easily be coded to ICD-10, 4% (95% CI 3.4 - 5.1%) could not be coded, and 12.5% could be coded with difficulty. The codability of causes decreased down the causal sequence from 91% (95% CI 89 - 92%) on line a to 72% (95% CI 63.5 - 80.0%) on line d. In the contributory cause section (part II), only 54% (95% CI 44.8 - 62.3%) could be coded. Non-ICD nomenclature such as 'immunocompromised', 'retroviral disease' and 'multiple organ failure' occurred more frequently in line d and part II than in the other lines. The surgical department had the highest level of non-codable causes at 7.3% (95% CI 5.0 - 9.5%). Ill-defined causes such as 'natural causes' and 'old age' were used in only 4 (0.4%) of the notifications.
Errors in certification of cause of death
Table II presents the frequency of major and minor errors. Only 8 (0.8%) records were completely error-free. At least 98.4% had one minor error and 45.4% at least one major error. Improper sequencing was the most frequent major error.

Factors associated with serious major errors
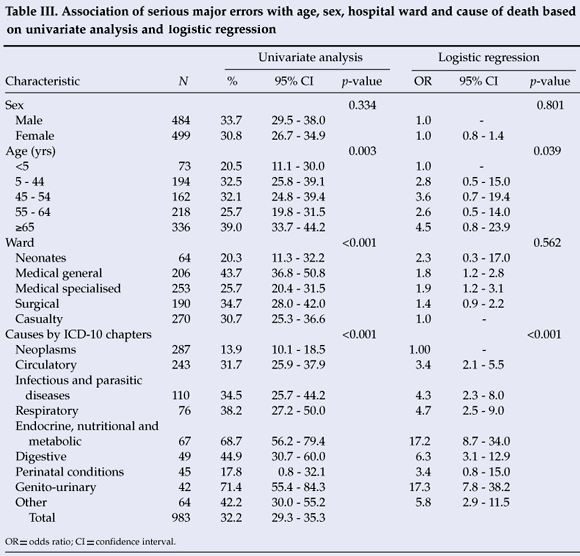
Serious major errors were found to be significantly associated with ward, cause of death and age of the deceased in the univariate analyses, but only with cause of death and age in the multivariate analysis (Table III). They increased with increasing patient age, and were 4.5 times higher in the ≥65 age group compared with the <5-year age group. Compared with neoplasms, the chance of errors was about 17 times higher for endocrine, nutrition and metabolic disorders, and for genito-urinary conditions. The pseudo-R2 was relatively low at 0.12, suggesting that there are factors which were not captured in this study.
Under-reporting of HIV deaths
One record from the sub-sample selected for review could not be found, and the remaining 242 were assessed blind to the death certificate information. Only 21.5% (95% CI 16.3 - 26.7%) had a clear indication of an HIV test in the medical records. Of these cases 38 were HIV positive, giving an HIV prevalence of 15.6% (95% CI 11.1 - 20.3%) in the sub-sample. Given the high proportion of cases without recorded information, this must be considered a minimum prevalence.
Out of the sub-sample of 243 records, 71 deaths were potentially related to HIV or AIDS, and 33 (46.5%) of these individuals had no indication of a HIV test in their medical record. Furthermore, of the 32 cases that were recorded as HIV positive in their medical record, only 15 (47%) had HIV/AIDS indicated on the death certificate. From the sample, it was found that 6 of the 38 patients recorded as being HIV positive died due to causes that were not directly related to HIV/AIDS. The causes included renal failure (N=2), stroke (N =2), hypertensive heart disease and ischaemic hepatitis associated with drug abuse and accounted for 15.8% (95% CI 4.2 - 27.4%) of the recorded HIV-positive patients.
Discussion
The WHO ICD-10 manuals are the international standard for mortality statistics. Information provided on DNFs at this hospital was well suited for coding to ICD definitions, and <1% had ill-defined signs and symptoms as the underlying cause. However, avoidable mistakes occurred in most death notifications. In 32% the errors were sufficiently serious to potentially affect the accuracy of cause of death coding. Errors occurred more frequently among causes of death certified to genito-urinary or endocrine and metabolic conditions. The error rate did not differ by gender but increased with patient age. This could possibly be associated with an increased tendency for co-morbidity in older people. The difference in error rates across wards appears to be explained by the patient profile rather than differences between wards.
The major error rate in this study of 45% is comparable to that of Burger et al.3 (43%). However, it is high compared with reports from an academic hospital in Canada (33%)12 and from a national population-based study in Taiwan (19%).14 The absence of indication of the time interval from onset of disease to death contributed to the 98% of minor errors in the DNFs, slightly higher than 82%3 in a population-based study in Cape Town, and much higher than 36% in a study in a teaching hospital in Canada.11
Our study reveals extensive under-reporting of HIV as the underlying cause of death. People with HIV are prone to other illnesses and infections, and HIV should be recorded as the underlying cause of death if it 'initiated the chain of morbid events leading directly to death'. The under-reporting of HIV on the DNF appears to have arisen from incomplete clinical information at the time of certification (nearly half potential AIDS cases had no record of an HIV test), and reluctance to certify HIV (in nearly half the HIV-positive cases, the DNF did not reflect this).
Reluctance to certify the presence of HIV may be due to concerns about confidentiality of the information on the DNF. The apparent lack of HIV testing was surprising. However, these data predated the antiretroviral roll-out in South Africa and coincided with the commencement of provision of ARVs at academic hospitals, so HIV testing may not have been required for appropriate clinical management. The magnitude of the AIDS epidemic and the need for reliable information require concerted efforts to improve the quality of medical certification and to enhance the system to ensure confidentiality of cause of death information.
The accuracy and completeness of cause of death statistics depend on the details provided by medical practitioners and their ability to correctly identify and certify the cause and manner of death.15 Medical students and doctors should have improved training in the completion of death notification. In Canada a brief educational intervention significantly reduced rates of major errors in the completion of death notifications.12 An intervention reported in this issue of SAMJ also found a significant reduction in the error rate after a short course accompanied by a pamphlet with guidelines. 16
Since death certificates are practically the only source of data on cause of death, this information must be as accurate as possible. International practice indicates that a system of review and feedback to the certifying doctors is needed. This should occur at several levels: the statistical office should have a system to check certificates that have major errors, and health care facilities should introduce strategies to encourage doctors and administrative staff to comply with the rules of 'international form of medical notification of cause of death' completion. These should be supported by the provincial and national Departments of Health.
This study has several limitations. One researcher determined the type of error, and this would have been improved methodologically by a second researcher independently cross-checking the findings. As it was conducted in a single facility the results apply to this study population only. Patients who died in this hospital may not be representative of South Africa as a whole, and the certifiers may not represent all doctors in South Africa. Nonetheless, it is anticipated that the findings have broader relevance.
Despite South Africa's improved cause of death statistics based on vital registration, in this study almost a third of errors were serious enough to affect selection of the underlying cause of death, confirming that the quality of medical certification must improve. In such cases the underlying cause of death remains unknown or uncertain, and this has serious public health and policy implications.
Despite errors and misclassification on DNFs, death notification data remain an essential source of information on the health status of the population. It is important to understand the limitations of the data and to make use of the burden of disease approach of checking the consistency of the data against other sources or models to derive meaningful estimates.
References
1. Dorrington R, Bradshaw D, Wegner T. Estimates of the Level and Shape of Mortality Rates in South Africa around 1985 and 1990 Derived by Applying Indirect Demographic Techniques to Reported Deaths . Tygerberg, W Cape: Medical Research Council, 1999. [ Links ]
2. Bah S. A Note on the quality of medical certification of deaths in South Africa, 1997-2001. S Afr Med J 2003; 93: 239. [ Links ]
3. Burger EH, Van der Merwe L, Volmink J. Errors in the completion of the Death Notification Form. S Afr Med J 2007; 97: 1077-1081. [ Links ]
4. Meel BL. Certification of death at Umtata General Hospital, South Africa. Journal of Clinical Forensic Medicine 2003; 10: 13-15. [ Links ]
5. Westwood ATR. Childhood deaths due to HIV: The role of the new death certificate. S Afr Med J 2000; 90: 877-878. [ Links ]
6. Johansson LA, Westerling R. Comparing Swedish hospital discharge records with death certificate: Implication for mortality statistics. Int J Epidemiol 2002; 9: 495-502. [ Links ]
7. World Health Organization. International Statistical Classification of Disease and Related Health Problems . 10th revision. Vol. 2. Geneva: World Health Organization, 1992. [ Links ]
8. Magrane BP, Gilliland MG, King DE. Certification of death by family physician. Am Fam Physician 1997; 56: 1287-1290. [ Links ]
9. Bradshaw D, Schneider M, Dorrington R, Bourne D, Laubscher R. South African cause of death profile in transition — 1996 and future trends. S Afr Med J 2002; 92: 618-623. [ Links ]
10. Groenewald P, Nannan N, Bourne D, Laubscher R, Bradshaw D. Identifying deaths from AIDS in South Africa. AIDS 2005; 19: 193-201. [ Links ]
11. Jordan JM, Bass MJ. Errors in death certificate completion in a teaching hospital. Clin Invest Med 1993; 16: 249-255. [ Links ]
12. Myers KA, Farquhar DRE. Improving the accuracy of death certifications. CMAJ 1998; 158: 1317-1323. [ Links ]
13. Weeramanthri T, Beresford B. Death certification in Western Australia: Classification of major errors in certificate completion. Aust J Public Health 1992; 16: 431-434. [ Links ]
14. Lu, TH, Lee MC, Chou MC. Accuracy of cause of death coding in Taiwan: Types of miscoding and effects on mortality statistics. Int J Epidemiol 2000; 29: 336-343. [ Links ]
15. Groenewald P, Pieterse D. Getting the facts of death right (Editorial). S Afr Med J 2007; 97: 1056-1058. [ Links ]
16. Pieterse D, Groenewald P, Bradshaw D, Buger L, Reagon G, Rodhe J. Death certificates: Let's get it right. S Afr Med J 2009; 99: 643-644 (this issue). [ Links ]
Accepted 22 July 2009.
* Corresponding author: B Nojilana (beatrice.nojilana@mrc.ac.za)














