Services on Demand
Article
Indicators
Related links
-
 Cited by Google
Cited by Google -
 Similars in Google
Similars in Google
Share
SAMJ: South African Medical Journal
On-line version ISSN 2078-5135
Print version ISSN 0256-9574
SAMJ, S. Afr. med. j. vol.99 n.9 Pretoria Sep. 2009
SCIENTIFIC LETTERS
Death certificates: let's get it right!
Desiree PieterseI; Pam GroenewaldII,*; Debbie BradshawIII; Elsie H BurgerIV; Jon RohdeV; Gavin ReagonVI
IMPhil (Public Health), Burden of Disease Unit, Medical Research Council, Tygerberg, W Cape
IIMB ChB, MPhil (Public Health), Burden of Disease Unit, Medical Research Council, Tygerberg, W Cape
IIIDPhil (Oxon), Burden of Disease Unit, Medical Research Council, Tygerberg, W Cape
IVMB ChB, MMed Forens Path, FC For Path (SA), Division of Forensic Medicine, University of Stellenbosch, and Forensic Pathology Services, W Cape
VBA, MD, FAAP, FCPM, DSci, 3 Moray Place, Oranjezicht, W Cape
VIMB ChB, FCPHMSchool of Public Health, University of the Western Cape, Bellville, W Cape
To the Editor: Burger et al.1 demonstrated that 43% of death notifications in a sub-district of Cape Town contained errors serious enough to affect the accuracy of identifying the underlying cause of death. They concluded that the development and testing of educational interventions to improve death certification amongst medical practitioners was urgently required.
We developed a death certification educational intervention consisting of a 45-minute didactic teaching session and an educational handout that covered: (i) the importance of mortality data for public health, (ii) process of death certification, (iii) concept of a causal sequence and the underlying cause of death, (iv) distinction between cause and mechanism of death, (v) appropriate terminology to use when writing cause of death statements and (vi ) common misconceptions.
Method and subjects
The intervention was tested at an academic tertiary hospital in 2007 among consenting medical interns who had completed at least 6 months of their internship. They were randomly allocated to two groups; one group received only the written educational handout while the other received the handout and the didactic teaching session. A self-administered questionnaire including three case scenarios was presented to each intern for completion prior to the educational intervention, and another was administered 2 weeks post-intervention. Participants were required to complete a model death certificate for each case scenario which was assessed for the following major errors: whether an acceptable underlying cause of death was listed; whether there were any errors in the causal sequence between immediate and underlying cause of death; and whether there were competing underlying causes of death listed. Minor errors were also assessed, namely whether the duration between the onset of the cause and time of death was listed, and whether abbreviations were used. Each cause listed was scored on a scale of 0 - 2, where 0 = does not conform to the guidelines (inaccurate and inappropriate); 1 = acceptable, but there is incomplete adherence to the guidelines; and 2 = exact adherence to the guidelines. The total possible score for each case scenario was 10, made up of a score of 6 for avoiding major errors and 4 for avoiding minor errors. As there were 3 case scenarios, the maximum score for avoiding all major errors was 18 and for avoiding all minor errors was 12, with a total possible score of 30 for avoiding all errors. A cut-off level which represents a level above which errors are unlikely to affect the correct identification of the underlying cause of death, was set by consensus at a score of 12 out of 18 for avoiding major errors, provided that they did not score 0 on any of the 3 questions assessing major errors. This cut-off was deemed appropriate as only major errors would affect the identification of the underlying cause of death. An exact test for symmetry was used to compare the two groups on proportions acceptable, and the matched pair's exact test was used to evaluate the change in pre- and post-test scores.
Results
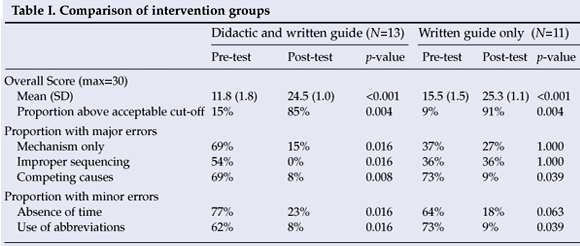
Of the 49 medical interns at the academic tertiary hospital, 32 consented and participated in the study. Only 24 of the 32 interns participated in the post-intervention test, giving a 75% follow-up response rate. Very low proportions achieved an acceptable score in the pre-intervention test, and both groups improved post-intervention (Table I). The improvement was significant in both groups. Although both groups improved significantly, there was no difference in the degree of improvement between them, indicating that the addition of a didactic teaching session did not contribute significantly towards the improved score. The improvement was therefore due to either or both the provision of the educational handout or the process of considering the case scenarios (i.e. the method of measurement itself resulted in improvement). There was no known co-intervention, and the time-period of 2 weeks between the assessments was too short for the acquisition of further experience to explain the improvement.
Conclusion
Medical interns have poor skills in death certification. However, an educational handout and the considering of case scenarios effectively provides them with the basic skills of death certification. Further research is required, using larger samples and controlling for the educational handout and the didactic teaching session, to confirm the efficacy of this intervention and to assess its applicability in other settings, e.g. among general practitioners. Nevertheless, this brief intervention, if implemented widely, could markedly improve the quality of cause-of-death statistics in South Africa.
References
1. Burger EH, Van de Merwe L, Volmink J. Errors in the completion of the Death Notification Form. S Afr Med J 2007; 97: 1077-1081. [ Links ]
* Corresponding author: Pam Groenewald (prenaud@compnet.co.za)














