Services on Demand
Article
Indicators
Related links
-
 Cited by Google
Cited by Google -
 Similars in Google
Similars in Google
Share
SAMJ: South African Medical Journal
On-line version ISSN 2078-5135
Print version ISSN 0256-9574
SAMJ, S. Afr. med. j. vol.99 n.7 Pretoria Jul. 2009
ORIGINAL ARTICLES
How do doctors learn the spoken language of their patients?
Colin PfaffI, *; Ian CouperII
IMB BCh, MMed (Fam Med), DCh, DA, Dip HIV Man, Division of Rural Health, Faculty of Health Sciences, University of the Witwatersrand, Johannesburg
IIBA, MB BCh, MFamMed, Division of Rural Health, Faculty of Health Sciences, University of the Witwatersrand, Johannesburg
ABSTRACT
BACKGROUND: In South Africa, many doctors consult across both a language and cultural barrier. If patients are to receive effective care, ways need to be found to bridge this communication barrier.
METHODS: Qualitative individual interviews were conducted with seven doctors who had successfully learned the language of their patients, to determine their experiences and how they had succeeded.
RESULTS: All seven doctors used a combination of methods to learn the language. Listening was found to be very important, as was being prepared to take a risk or appear to be foolish. The doctors found that it was important to try out the newly learned language on patients and additionally stressed that learning the language was also learning a culture. The importance of motivation in language learning, the value of being immersed in the language one is trying to learn, and the role of prior experience in language learning, were commonly mentioned. The doctors deeply valued the improved rapport and deeper relationships with patients that resulted from their language learning efforts.
In South Africa, many doctors consult across both a language and cultural barrier. However, studies have shown that patients prefer being addressed in their own language1 and that their satisfaction after a consultation in their own language is higher.2-5 The second-biggest obstacle, after income, in access to services was assessed to be doctors not being able to speak their patients' language, in a Cape Town study.5 In a similar study, doctors not being able to speak the same language as their patients caused ethical dilemmas, negative attitudes between staff and patients, and decreased quaility of care.6
Interpreters are used to overcome these limitations but involve disadvantages; they are frequently unavailable,6 may impose their own views on consultations,7 may make translation errors8-12 and cause frustration among staff who are asked to perform this role in addition to their other duties.13
In contrast, communication and understanding of patients' complaints after learning their language is improved.14 Ellis15 has described how to use the consultation effectively as an ideal language learning environment, gives suggestions on how to do so, and stresses the importance of learning culture and cultural metaphors of illness as part of language learning.
The theory of second-language learning has moved from the traditional grammar and translation methods to more communicative methods. Krashen's 'natural approach'16 suggests that language is acquired from the hearing of adequate input (as a child acquires a language) and not by learning formal grammatical rules. The latter can only correct language that has been acquired through listening. The Brewsters17 suggest an 'immersion experience' by living with speakers of the language. Ellis included several of their tools, such as loop tapes, as being useful in a consultation when learning a language.15 Others disagree with a purely communicative approach to language learning and emphasise the importance of learning formal grammar.18,19
Many doctors would like to be able to speak their patients' language.6 However, very little guidance exists on how to do this successfully in a busy practice. We aimed to investigate the experiences of doctors who had effectively learnt the language of their patients so as to guide those who also wish to do so.
Methods
A pertinent sample was selected of eight doctors who met the inclusion criteria of working with patients whose language was not the doctor's first language and being able to see patients without an interpreter, and who described their language proficiency as 'good'. Doctors were excluded if they had not learnt the second language while practising as a professional, had learnt it for other reasons (e.g. to try to find work), or had learnt a language similar to their first language.
Free attitude interviews were used. Subjects were asked the same exploratory question: 'How did you learn the spoken language of your patients and what were your experiences in learning the language?' The audio-taped interviews were transcribed verbatim. Themes were identified by using contrastive analysis by the researcher together with the supervisor. Cut-and-paste techniques were used to analyse common themes. Subjects validated the analysis of each interview.
Results
Our aim was to study eight doctors, but only seven were found who met the inclusion and exclusion criteria; one was excluded as he had started learning the language as a child and not as an adult professional. We recognised that if the degree of fluency required had been set lower, many others would have qualified. All the doctors interviewed were white males, partly owing to the exclusion criterion that the interviewees must not be from a language group similar to the language that they had learned.
Key themes emerged from analysis of the data. Many different methods were used by each interviewee to learn the languages. The consultation was commonly used for language learning by asking how to phrase certain questions, then trying them out with a patient and, over time, understanding what the patient was saying in reply. Immersing oneself in a community where the language was spoken was found to be useful, as was having a personal tutor. In contrast, formal language classes were felt to be unhelpful, and produced students who were good at grammar tests but unable to communicate with people. Book learning and UNISA courses both met with mixed success. Books were felt to be useful for learning grammar but not vocabulary. UNISA courses were felt by some not to be helpful early on in language learning but another felt that they enabled understanding of rules once the language was learnt. One doctor reported language tapes to be a failure and did not use these after they had been bought.
The importance of listening in learning a language was a very strong theme. Listening was important both in the consultation where two translations were constantly heard and also in non-medical situations such as church services. Listening was important to expand vocabulary and understanding of implied meaning and, as such, language learning was seen by one doctor as an indicator of how much the doctor was listening to and integrating with the second-language people. Learning by listening was also related to learning styles and preferences; one doctor felt that he had an 'ear orientation', and another that he had a 'musical ear'.
Being prepared to take a risk or appear foolish was another common theme. Several doctors told stories of mistakes that they had made with hilarious consequences. Pride, or being seen as distant from the people, was then seen as a hindrance to this process; this was closely linked to risk taking and was surmised to be a possible reason why some doctors learnt more than others.
Having to try out the language with patients was commonly mentioned, including listening to the phonetics and trying them out, attempting to work without an interpreter, or trying various words to see which were ones used locally.
The role of language in building deeper connections was a strong theme. Speaking the language was seen as establishing a deep relationship with patients; their faces changed, a rapport developed, hearts and doors were opened, and friendships developed. Speaking the language removed barriers between doctor and patient, helping them to communicate at another level, which was impossible using an interpreter. Confidentiality in the doctor-patient relationship was improved. Patients loved to speak their native language with the doctor, even if they could speak English.
Many participants described how learning a language was also learning a culture. This was particularly true for the principle of 'hlonipha' – meaning respect and how people deal with each other. This emotional bonding with a culture gave language learning added enjoyment. Learning the culture was also part of identifying with the local people.
Motivation was crucial to successful language learning, including being inspired by others who could speak well, frustration in working with interpreters, wanting to interact at a different level, or learning out of necessity as interpreters were not available. Other motivations included inherent interest in the grammar of the language or appreciating its beauty.
Being fully immersed in an environment where the language was spoken was very helpful in learning language and culture. Two doctors had a 'full immersion' experience in the language by living in the village where they were working. Two others mentioned regular short periods of immersion of a few days at a time of staying in the community or on church weekends. However, immersion in the environment by itself is insufficient for learning; one must have a good reason for wanting to learn.
Prior experiences of learning a language were very helpful in learning another language.
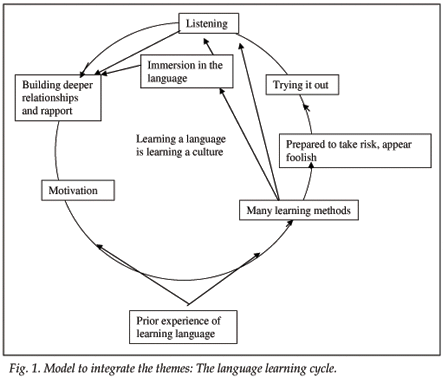
A diagrammatic representation of the above themes appears in Fig. 1.
Discussion
Theories of second-language learning have shifted from emphasising the grammar/translation method, to more communicative approaches. Our research showed that doctors used several approaches to language learning, but placed a strong emphasis on more communicative approaches. However, almost all used some grammar learning too, either with a tutor or from books. Although some communicative approach advocates have claimed that formal grammar learning is not necessary,16 others have criticised this purely communicative approach as it produced speakers who made many errors that could have been corrected easily by knowledge of a few simple rules.18
The emphasis of these doctors on a communicative approach is shown by the importance they placed upon the role of listening in language learning. Some linguists claim that meaningful language acquisition, as opposed to learning rules, can only be aquired by hearing enough spoken language, and they even suggest a silent period when all emphasis is placed on listening rather than trying out new words.16 These doctors found, as Ellis15 suggested, that consultations were ideal for this sort of language learning.
As language learning in this setting was voluntary, motivation clearly provided a key role. Motivation is often central in predicting language achievement20 and only thereafter do other cognitive and affective factors play a role.21 Even in a military setting, where soldiers learnt Korean or Spanish as part of their training, motivation and attitude were important predictors, after aptitude of second-language proficiency.21 Krashen suggests that attitude and motivation provide a 'filter' through which sounds must pass before they can become useful in acquiring language.16 Students with good attitude and strong motivation have a 'lower filter' and therefore learn quickly from what they hear; our research supports this theory. One doctor said that just being in a language-rich environment was not enough; rather, motivation to learn a new language was a key influence.
The motivation that sustains language learning often came from the rewards gained from deepening relationships with patients, staff and community members, again emphasising a communicative approach. These rewards in turn led to increased motivation to further improve learning of the language, so establishing a cycle of language learning (Fig. 1). Greater language proficiency, through various communicative methods of learning, further deepened relationships which in turn further increased motivation to learn more, and so the cycle gained momentum.
Conclusion
Language learning is often seen as a noble goal but one that is difficult to achieve, especially in the context of a busy working practice. Our research shows that it is achievable and provides pointers on how it can be done (Table I), the importance of a communicative approach, and the key role that motivation plays and how this motivation is sustained through the reward of deepening relationships. We hope that these findings will inspire more South Africans to embark on the journey of learning the language of their patients, so leading to improved patient care and satisfaction and understanding for doctor and patient.

References
1. Ahmed WIU, Kernohan E, Baker MR. Patients' choice of general practitioner: influence of patients' fluency in English and the ethnicity and sex of the doctor. J Roy Coll Gen Pract 1989; 39: 153-155. [ Links ]
2. Freeman GK, Rai H, Walker JJ, et al. Non English-speakers consulting with the GP in their own language – a cross-cultural survey. Brit J Gen Pract 2002; 52: 36-38. [ Links ]
3. Bucci W, Baxter M. Problems of linguistic insecurity in multi cultural speech contexts. Ann N Y Acad Sci 1984; 433: 185-200. [ Links ]
4. Carrasquillo O, Orav J, Brennan TA, Burstin HR. Impact of language barriers on patients' satisfaction in an emergency department. J Gen Int Med 1999; 14: 82-87. [ Links ]
5. Levin ME. Language as a barrier to care for Xhosa-speaking patients at a South African paediatric teaching hospital. S Afr Med J 2006; 96(10): 1076-1079. [ Links ]
6. Schlemmer A, Mash B. The effects of language as a barrier in a South African district hospital. S Afr Med J 2006; 96(10): 1084-1087. [ Links ]
7. Andreyev HJN. Getting the message across. BMJ 1987; 294: 1534-1535. [ Links ]
8. Wood B. Interpreters in the medical consultation – a literature review. S Afr Fam Pract 1993; 14: 347-53. [ Links ]
9. Launer J. Taking medical histories through interpreters: practise in a Nigerian outpatient department. BMJ 1978; 2: 934-935. [ Links ]
10. Marcos LR. Effects of interpreters on the evaluation of psychopathology in non English speaking patients. Am J Psychiat 1979; 136: 171-174. [ Links ]
11. Ebden P, Bhatt A, Carey O, Harrison B. The bilingual consultation. Lancet 1988; 1: 347. [ Links ]
12. Elderkin-Thompson V, Cohen-Silver R, Waitzkin H. When nurses double as interpreters: a study of Spanish-speaking patients in a US primary care setting. Soc Sci Med 2001; 52: 1343-1358. [ Links ]
13. Drennan G. Counting the cost of language services in psychiatry. S Afr Med J 1996; 86: 343-345. [ Links ]
14. Wright CM. Language and communication problems in an Asian community. J R Coll Gen Pract 1983; 33: 101-104. [ Links ]
15. Ellis C. Learning Language and Culture in the Medical Consultation. Johannesburg: Sue McGuniness Communications, 1999. [ Links ]
16. Krashen S. The Natural Approach. Oxford: Pergamon Press, 1983: 1-61. [ Links ]
17. Brewster ET, Brewster ES. LAMP (Language Acquisition Made Practical). Pasadena: Lingua House, 1976. [ Links ]
18. Hammerly H. Fluency and Accuracy: Toward Balance in Language Teaching and Learning. Bristol: Longdunn Press, 1991: 1-40. [ Links ]
19. Pica T. Questions from the Language Classroom: Research Perspectives. TESOL Quarterly 1994; 28: 49-79. [ Links ]
20. Beebe LM. Risk taking and the language learner. In: Seliger HW, Long MH. Classroom Orientated Research in Second Language Acquisition. Rowley, Mass.: Newbury House, 1983: 141-150. [ Links ]
21. Gardner RC, MacIntyre PD. A student's contributions to second language learning. Part II: Affective variables. Lang Teach 1993; 26: 1-11. [ Links ]
Accepted 20 February 2009.
* Corresponding author: C Pfaff (colinpfaff@yahoo.co.uk)














