Services on Demand
Article
Indicators
Related links
-
 Cited by Google
Cited by Google -
 Similars in Google
Similars in Google
Share
SAMJ: South African Medical Journal
On-line version ISSN 2078-5135
Print version ISSN 0256-9574
SAMJ, S. Afr. med. j. vol.99 n.7 Pretoria Jul. 2009
ORIGINAL ARTICLES
Rubella in South Africa: an impending Greek tragedy?
Barry D SchoubI, *; Bernice N HarrisII; Jo McAnerneyIII; Lucille BlumbergIV
IMB BCh, MMed, MD, DSc, FRCPath, FCPath (SA), FRSSAf, MASSAf, National Institute for Communicable Diseases, Sandringham, Johannesburg
IIMB ChB, MMed, National Institute for Communicable Diseases, Sandringham, Johannesburg
IIIRN, RM, Dip Data Dip Method, National Institute for Communicable Diseases, Sandringham, Johannesburg
IVMB BCh, MMed, DTM&H, DCH, DOH, National Institute for Communicable Diseases, Sandringham, Johannesburg
ABSTRACT
BACKGROUND: The incidence of congenital rubella syndrome (CRS) is unknown in South Africa. There is evidence that it may be significant and largely undetected, particularly in the upper socio-economic group. This may be due to incomplete routine administration of MMR vaccine in infancy and a build-up of susceptible females reaching the childbearing age group who could be exposed to the extensive reservoir of virus in the unimmunised public sector of the population.
OBJECTIVE: To assess the extent of the immunity gap to rubella by testing for protective IgG antibodies and the incidence of rubella infection by testing for IgM antibodies in sera. The data obtained would also be used to model the extent of CRS. Design. Residual laboratory serum specimens from public and private laboratories were serologically tested for rubella IgG antibodies to investigate the immunity gap in the population and IgM antibodies in sera collected from the measles rashlike illness surveillance programme. Modelling exercises calculated the force of infection and the predicted incidence of CRS in South Africa.
RESULTS: The serological immunity gap was significantly greater in the private sector specimens compared with the public sector – 10.7% versus 5.4%, respectively. In most years rubella caused much more rash-like illness than measles, with a significant number (5.1 - 9.6%) of rubella-positive IgM specimens occurring in women of childbearing age.
CONCLUSION: Modelling of the data suggests that the extent of CRS may be grossly underestimated in South Africa. Approximately 654 cases are calculated to occur every year. It is suggested that selective immunisation of girls before puberty should be instituted together with a routine rubella immunisation programme of infants to forestall a possible future outbreak of CRS, as occurred in Greece in 1993.
Rubella in children and adults is almost always a mild disease, with serious or long-term sequelae a rarity. The focus of concern is infection of susceptible women in the first 16 weeks of pregnancy. The risk of congenital rubella syndrome (CRS) in the first 8 - 10 weeks is up to 90%, after which it drops sharply and is virtually non-existent after 16 weeks other than rare mild systemic illnesses.1 The incidence of CRS globally has been estimated as between 0.1 and 0.2/1 000 live births in endemic periods and up to 1 - 4/1 000 live births following epidemics. The global toll of CRS is approximately 100 000 cases per year.1 In practice, however, relatively few cases of CRS are reported and many are unrecognised, as the clinical manifestations may be delayed until months or even years after birth. Globally only 37 cases were reported to the World Health Organization (WHO) in 1995, none of them from South Africa.2
Widespread use of rubella vaccine in the developed world has dramatically reduced the incidence of rubella and CRS. Soon after the vaccine became available in the early 1970s, many countries instituted vaccination programmes, targeting pre-adolescent girls at about 12 years of age before they become sexually active, to protect women when they reach childbearing age – so-called 'selective immunisation'. These programmes, while moderately successful in protecting the group at risk, failed to influence the circulation of the virus, mainly because children are the major reservoir of infection, and the risk to unvaccinated or unsuccessfully vaccinated women remained. Approximately a decade later the strategy was changed to eliminate the circulation of wild-type rubella virus by routine immunisation of all children between 12 and 15 months – so-called 'universal immunisation'. High vaccine coverage rapidly brought about a dramatic reduction of the incidence of rubella, to the extent that the Pan American Health Organization (PAHO) has now targeted 2010 as the goal for the elimination of rubella from the Western hemisphere3 and the European region of the WHO has simultaneously set a goal of 2010 for that region.4 In these countries the problem of rubella and CRS is now confined to non-vaccinated immigrant populations.
Rubella vaccine in contemporary use, RA27/3, is a safe effective vaccine, administered either as a monovalent vaccine or far more commonly in combination with measles (MR) or measles and mumps (MMR).1 Cost-benefit analyses in both developed and developing countries have shown ratios greater than 1.5 The impetus to introduce routine rubella immunisation is therefore great. MMR can also be given as effectively and safely at 9 months of age, when measles vaccination is routinely administered in many developing countries and in South Africa.6 However, experiences in several countries have shown that hasty introduction of universal rubella vaccination (usually as MMR) before adequate precautionary conditions have been put into place (i.e. an extensive selective immunisation programme in place until adequate MMR vaccination coverage is achieved) may, paradoxically, greatly increase the risk of CRS.7 This is due to the potential for an upwards shift in age of rubella infection because of the reduction of wild-type virus circulation and its consequent reduction in population immunity, resulting in increasing numbers of vulnerable women in the childbearing age group susceptible to a still-present reservoir of circulating wild-type virus.
In South Africa, a scenario could be building up similar to that in Greece in the 1990s before their unprecedented outbreak of CRS.7 Small but increasing use of MMR in the private sector may be building up a population of susceptible adolescents and young adults, while at the same time there is no programme for selective immunisation of girls. Indications are that the reservoir of the virus is large and could pose a serious threat for CRS.
South Africa has no programme for collecting data on clinically manifest CRS. We have attempted to model the theoretically expected extent of CRS and assess the potential risk for an outbreak of CRS.
Methods
Case-based surveillance
As part of the WHO programme to eliminate measles, all patients throughout South Africa presenting with a rash-like illness with pyrexia and one of the symptoms coryza, conjunctivitis or cough have a specimen of blood taken to test for measles IgM. In addition, all specimens are tested at the National Institute for Communicable Diseases (NICD) for rubella IgM.
Serosusceptibility to rubella
Residual sera from laboratory specimens and banked sera were collected to assemble a range of samples from women of all ages and throughout all provinces of the country from both the private sector laboratories and the public sector through the National Health Laboratory Service (NHLS).
Serology
Sera were tested for the presence of rubella IgM antibodies (to indicate active infection) and IgG antibodies (to indicate immunity or susceptibility) using commercial EIA kits. Rubella-specific IgM was tested using the Dade Behring EIA kit and IgG antibodies using Biorad Platelia ELISA kit according to the manufacturer's instructions. Rubella IgG levels >15 IU/ml were interpreted as indicating immunity.
Statistical analysis
The Statistical Package for Social Sciences (SPSS) (version 13) was used for statistical evaluation. Significance of differences was determined using a one-way analysis of variance (ANOVA). Pearson's correlation coefficient was determined within groups. Statistical significance was set at p-values <0.05.
Modelling methodology
To model the predicted incidence of CRS, data from the extent of rubella infection (IgG positive) and susceptibility data in women of childbearing age (12 - 49 years) were used. Age-stratified seroprevalence data were used to construct a simple catalytic model in Excel to calculate the force of infection (FOI), as described by Cutts and Vynnycky.8 The average age of onset of infection, basic reproductive rate and level of coverage needed to achieve herd immunity was calculated from this FOI using a standard equation as described by Anderson and May.9
To estimate the number of congenital rubella syndrome cases for 2005, the methodology described by Cutts and Vynnycky8 was used to first estimate the incidence (force) of rubella infection assuming an age-dependent infection rate. The proportion of seronegative pregnant women was assumed to be identical to that of the general population. The estimated FOI for the population 15 years and older and the proportion of seronegative pregnant women was used to calculate the estimated incidence of infection during gestation, assumed to be 40 weeks.
The risk of CRS was calculated as the weighted average of risk after infection in pregnancy from data of Miller et al.10 as 65% in the first 16 weeks and zero thereafter. The incidence of CRS per 100 000 live births was calculated by multiplying the proportion of live babies born to mothers first infected with rubella during the first trimester of pregnancy (identical to the cumulative incidence of rubella infection during the first 16 weeks of pregnancy) by this risk. The potential for fetal loss following rubella infection is not accounted for in these calculations. Statistics South Africa's 2005 mid-year estimate of the population under 1 year of age was used as a proxy for the number of pregnant women.
Results
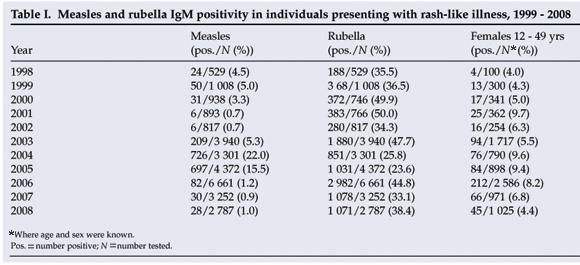
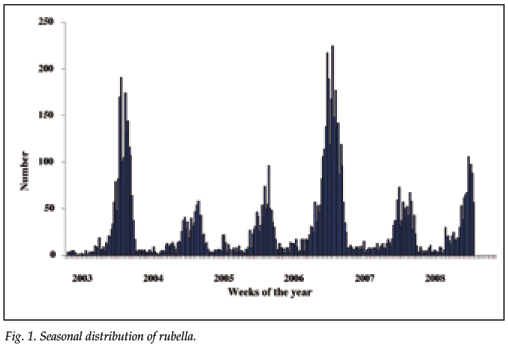
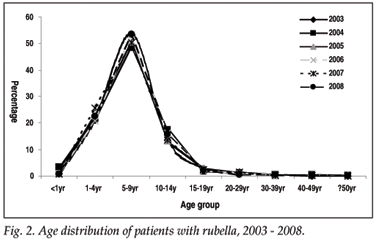
Patients presenting with a rash-like illness and clinically suspected measles were many times more likely to be IgM positive for rubella than for measles, except during the measles outbreak years of 2004 and 2005, and even in those years rubella positives exceeded measles positives (Table I). The seasonal distribution of rubella is shown in Fig. 1. The age distribution of IgM positives over the last 5 years is shown in Fig. 2 and ranges from 4 months to 64 years with a median of 7 years. However, a significant number of positives were also found in women of childbearing age group – the proportion of positive specimens in the age group 12 - 49 years, where age and gender were recorded, ranged from 5.1% in 2008 to 9.6% in 2004 (Table II).

A total of 8 940 samples were tested for rubella IgG antibodies (Table III). Of these, 1 295 were supplied by private laboratories, reflecting the higher socio-economic sector of the population, and 7 645 were public sector specimens from NHLS laboratories or banked serum specimens. The susceptibility gap (rubella IgG negative) for women 12 - 49 years of age in private sector specimens was significantly greater that in public sector specimens (10.7% and 5.4% respectively; p<0.0005). The inter-provincial differences were insignificant.

The modelling exercise to predict the number of expected CRS cases in South Africa is shown in Table IV. During 2005 there were projected to have been 69 CRS cases per 100 000 live births in South Africa, ranging from 16 per 100 000 live births in the Eastern Cape to 69 in the Free State. The confidence intervals for most estimates are wide except for Limpopo province and the South African total. On the basis of these estimates there may have been 654 cases in South Africa for that year. The expected yearly incidence of CRS will vary depending on the epidemic cycle of the area, i.e. more cases during a year with a larger epidemic. The variation in incidence between provinces may be an artefact of small numbers or due to provinces being at different stages of the rubella epidemic cycle.

Discussion
Rubella vaccine is not a component of the routine immunisation policy of South Africa, despite its being safe, effective and readily added to measles vaccine at minimal extra cost.
The annual incidence of CRS in South Africa is unknown – it is rarely diagnosed by clinicians. By modelling data collected from nationwide serological studies, we predict that there should be approximately 654 cases of CRS per year in South Africa, i.e. approximately 0.5/1 000 live births, a figure considerably higher than the WHO estimated figure of 0.1 - 0.2 in endemic periods but lower than the epidemic rates of 1 - 4 per 1 000 live births.1 Most CRS cases may well not manifest at birth, and physical, intellectual and developmental retardation or auditory or visual problems appearing later in life may well not be ascribed to CRS. Surveillance of CRS requires active programmes, which have been carried out in several developing countries, such as a congenital cataracts survey in India11 and clinical-virological surveillance in Myanmar.12 Similar studies, for example newborn hearing screening,13 need to be undertaken to determine the true incidence of CRS in South Africa.
Nevertheless, data from studies in South Africa and our recent serosurveillance study reported above indicate that a significant sero-immunity gap (i.e. an absence of detectable protective IgG antibodies) exists in the upper socio-economic sector of the population, with some 10% of women whose sera were tested in private laboratories being seronegative as opposed to 5% for public sector specimens. Similar findings of a 5 - 7% serological gap were reported in public sector sera from the Western Cape,14 Johannesburg15 and Maputo.16 The worryingly wide sero-immunity gap in women from upper socio-economic strata was also evident in several studies published from Cape Town (10 - 18% in hospital staff)17,18 and Johannesburg (10 - 18.4% in laboratory staff and students).15
The immunity gap in upper socio-economic group women largely reflects better living standards and less crowding. However, the influence of the small but significant administration of MMR by private vaccination clinics may well aggravate the situation. Some 58 800 doses of MMR were administered over a 12-month period in 2007/2008. We estimate that about 100 000 children per annum utilise private vaccination facilities (about two-thirds of the 14.7% of the population who are on a medical aid), giving estimated rubella coverage of approximately 59%. This could be enough to reduce the circulation of wild-type virus sufficiently to create a significant immunity gap in adolescent and young women in this population. The scenario of rubella vaccination not being part of public policy but given in the private sector is common to many developing countries. The impact of private sector MMR vaccination has been modelled mathematically.19 The risk for the development of CRS was shown to be determined by three factors: (i) the pre-vaccination force of infection; (ii) the extent of private vaccination; and (iii) random mixing between the two populations. In South Africa the FOI is high, as shown by the large numbers of rubella IgMs detected in the rash surveillance programme as well as the high seroprevalence in women from the public sector. The extent of private vaccination is high in the urbanised population, where extensive mixing is also a feature. These factors suggest that the endemic incidence of CRS may well be considerable, while the risk of CRS were a large-scale epidemic to occur would be much greater. Fig. 1 illustrates the seasonal curve of rubella in South Africa. Although data before 2007 are very incomplete, the curve suggests increased epidemic activity every 2 - 3 years, a feature typical of rubella in temperate climates in the pre-vaccination era.20 If this pattern is followed, in the year 2009 (spring/early summer) we may well see an upsurge in rubella and possibly an outbreak of CRS.
The temptation to rush into incorporating MMR into the routine immunisation programme should be resisted until adequate protective conditions have been put into place to prevent an upward age shift of infection. The tragic outbreak of CRS in Greece is a graphic example of what could happen if MMR is introduced into routine immunisation without other programmes being in place.7 MMR immunisation of 15-month-old infants was introduced in the private sector in Greece in 1975, achieving coverage of just under 50% during the 1980s. In 1989 it was introduced into the public sector for 15-month-old infants and in 1991 changed to a 2-dose schedule at ages 15 months and 11 years. Importantly, there was no selective immunisation programme in place for adolescent girls. A study of outpatient rubella cases showed a significant shift in the age of infection from a median of 7 years in 1988 to 15 years in 1993. The percentage susceptibility in pregnant women similarly rose from 11% in 1971/5 to 35% in 1990/1. A large outbreak of rubella in the early spring of 1993 was followed later that year by the largest outbreak of CRS ever recorded in that country – 24 CRS cases per 1 000 live births.
CRS can and should be eliminated from South Africa by simply making MMR part of routine immunisation. However, rushing into this without adequate safeguards may result in more harm than good. Before routine MMR is contemplated the following two precautionary conditions must be met:
-
A robust programme for selective immunisation of pre-pubertal/adolescent girls, best achieved by making immunisation a critical component of the school health system. This would also allow for other important adolescent vaccinations such as Td (tetanus and reduced-dose diphtheria vaccines), aP (acellular pertussis vaccine) and measles, and in future HPV and later HIV.
-
Routine measles immunisation coverage needs to be strengthened. A sustained coverage of >80% (the figure for the measles vaccine currently used, which is indicative of what the coverage would be if the combined MMR were to be introduced) in all districts is required in order to effect the reduction of circulating virus.1
References
1. World Health Organization. Rubella vaccines. Wkly Epidemiol Rec 2000; 75: 161-169. [ Links ]
2. World Health Organization. WHO Vaccine-preventable Diseases Monitoring System: 2006 Global Summary. Geneva, Switzerland: World Health Organization, 2006. http//www.who.int/vaccines-documents/GlobalSummary/GlobalSummary.pdf (accessed 17 December 2008). [ Links ]
3. Centers for Disease Control. Achievements in public health: Elimination of rubella and congenital rubella syndrome, United States, 1969-2004. MMWR Morb Mortal Wkly Rep 2005; 54: 1-4. [ Links ]
4. Spika JS, Hanon FX, Wassilak S, Pebody R, Emiroglu N. Preventing congenital rubella infection in the European Region of WHO: 2010 target. Euro Surveill 2004; 9(4): 4-5. [ Links ]
5. Hinman AR, Irons B, Lewis M, Kandola K. Economic analyses of rubella and rubella vaccines: a global review. Bull World Health Organ 2002; 80(4): 264-270. [ Links ]
6. Schoub BD, Johnson S, McAnerney JM, et al. Measles, mumps and rubella immunization at nine months in a developing country. Pediatr Infect Dis J 1990; 9(4): 263-267. [ Links ]
7. Panagiotopoulos T, Antoniadou I, Valassi-Adam E. Increase in congenital rubella occurrence after immunisation in Greece: retrospective survey and systematic review. BMJ 1999; 319: 1462-1467. [ Links ]
8. Cutts FT, Vynnycky E. Modelling the incidence of congenital rubella syndrome in developing countries. Int J Epidemiol 1999; 28(6): 1176-1184. [ Links ]
9. Anderson RM, May RM. Infectious Diseases of Humans: Dynamics and Control. Oxford: Oxford Science Publications, 2004. [ Links ]
10. Miller E, Cradock-Watson J, Pollock T. Consequences of confirmed maternal rubella at successive stages of pregnancy. Lancet 1982; 2: 781-784. [ Links ]
11. Malathi J, Therese KL, Madhavan HN. The association of rubella virus in congenital cataract - a hospital-based study in India. J Clin Virol 2001; 23(1-2): 25-29. [ Links ]
12. Kyaw-Zin-Thant, Win-Mar-Oo, Thein-Thein-Myint, et al. Active surveillance for congenital rubella syndrome in Yangon, Myanmar. Bull World Health Organ 2006; 1: 12-20. [ Links ]
13. Swanepoel D, Ebrahim S, Joseph A, Friedland PL. Newborn hearing screening in a South African private health care hospital. Int J Pediatr Otorhinolaryngol 2007; 71(6): 881-887. [ Links ]
14. Corcoran C, Hardie DR. Seroprevalence of rubella antibodies among antenatal patients in the Western Cape. S Afr Med J 2005; 95(9): 688-690. [ Links ]
15. Johnson S, McAnerney JM, Schoub BD, Kidd AH. Laboratory monitoring of rubella. S Afr Med J 1985; 67(18): 721-723. [ Links ]
16. Barreto J, Sacramento I, Robertson SE, et al. Antenatal rubella serosurvey in Maputo, Mozambique. Trop Med Int Health 2006; 11(4): 559-564. [ Links ]
17. Donald PR, Berlyn PJ, Becker WB. The rubella immune status of female hospital personnel. S Afr Med J 1983; 63(1): 4. [ Links ]
18. Schoub BD, Johnson S, McAnerney JM, Borkon L. Susceptibility to poliomyelitis, measles, mumps and rubella in university students. S Afr Med J 1990; 77(1): 18-20. [ Links ]
19. Vynnycky E, Gay NJ, Cutts FT. The predicted impact of private sector MMR vaccination on the burden of congenital rubella syndrome. Vaccine 2003; 21(21-22): 2708-2719. [ Links ]
20. Best JM, Banatvala JE. Rubella. In: Zuckerman AJ, Banatvala JE, Pattison JR, Griffiths PD, Schoub BD, eds. Principles and Practice of Clinical Virology. 5th ed. Chichester: John Wiley & Sons, 2004: 427-457. [ Links ]
Accepted 31 March 2009.
* Corresponding author: B D Schoub (barrys@nicd.ac.za)














