Servicios Personalizados
Articulo
Indicadores
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares en Google
Similares en Google
Compartir
SAMJ: South African Medical Journal
versión On-line ISSN 2078-5135
versión impresa ISSN 0256-9574
SAMJ, S. Afr. med. j. vol.99 no.7 Pretoria jul. 2009
SCIENTIFIC LETTERS
HIV-negative mother with an HIV-infected child: a diagnostic dilemma
Mohammed MithaI, *; Raveen ParboosingII; Andiswa NzimelaIII
IMB ChB, Department of Virology, University of KwaZulu-Natal, Durban
IIMB ChB, FCPath (Viro) (SA), Department of Virology, University of KwaZulu-Natal, Durban
IIIMB ChB, FCPaed (SA), Department of Paediatric Cardiology, Inkosi Albert Luthuli Central Hospital, Durban
To the Editor: Vertical transmission of the human immunodeficiency virus (HIV) accounts for the vast majority of HIV cases in children before, during and after birth.1 However, there are cases where the transmission mechanism is not fully explicable.2 We present such a case: an HIV-negative mother with a 6-month-old HIV-positive infant.
Case report
A term infant was delivered by caesarean section (CS) at King Edward VIII Hospital, a tertiary-level hospital in Durban. The CS was indicated by a previous CS, and the delivery was uneventful. The baby was exclusively breastfed by the mother for 2 months and formula-fed thereafter. The mother was the sole caregiver of the child. At 2 months of age, the child was admitted to hospital in respiratory distress and ventilated in the ICU. A diagnosis of acyanotic congenital heart disease was made. The child was admitted for cardiac surgery at age 6 months to Inkosi Albert Luthuli Central Hospital, a quaternary hospital in Durban. Two days after the operation, he developed cardiac arrest twice and was successfully resuscitated on both occasions; he also developed nosocomial sepsis. He was ventilated and received a blood transfusion during this period. An HIV test was done, as per routine ICU protocol, having not been tested for HIV prior to this admission. He tested positive with a 4th-generation HIV enzyme-linked immunosorbent assay (ELISA).3 An HIV DNA polymerase chain reaction (PCR)4 test confirmed the result. The CD4 count was 22%.
The mother had tested negative 6 times previously at various local government clinics, using rapid HIV diagnostic tests; 2 of these tests were performed after delivery.
The virologist was consulted and suggested an HIV ELISA on the mother and father, as well as a repeat HIV ELISA and DNA PCR on the infant. The repeat ELISA and DNA PCR was positive for the infant, and the mother's ELISA was negative on a 4th-generation immunoassay. Owing to the exceptional nature of the case, a DNA PCR test was also done on the mother, which was negative. The father tested positive on a rapid test, which was confirmed by DNA PCR (Table I).
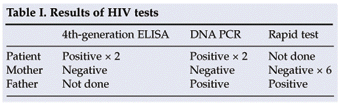
Since this was a sensitive matter with major emotional, social and diagnostic implications, clerical errors were excluded by verifying patient details and sample identification.
The diagnosis of an HIV-positive child and HIV-negative mother was confirmed after all samples had been verified. The mother was informed of the results and the possible explanations and consequences thereof, and was appropriately counselled.
Discussion
HIV infection is diagnosed in adults by the ELISA test which detects antibodies in serum, and, if positive, is confirmed by a Western blot or by a second sample. In children <18 months old, DNA PCR is used owing to the presence of maternal antibodies which may confound the result.5,6
The 4th-generation ELISA detects both the HIV antibody and the p24 antigen, and has a sensitivity of 100% and specificity of 99.86%.3 HIV DNA PCR has a sensitivity of 95% and specificity of 97%.5
In South Africa, rapid testing is widely used and has been found to be feasible, accurate and cost-effective.7 The kit routinely used in the KwaZulu-Natal public health sector has a sensitivity of 100% and specificity of 99.8%.8
There are several explanations for the discordant result between mother and baby:
-
The infant might have been infected in a health care environment, either by an infected needle or an intravenous line in a hospital. The patient had been hospitalised for 3 months. In the majority of similar cases identified, the affected infants had been hospitalised and had an intravenous access line and more frequent medical injections. There are, however, limited studies to prove this association.2,9,10
-
The child might have been infected by blood transfusion; however, the risk of contracting HIV by blood transfusion is estimated at 2 in a million cases.11 Antibodies generally appear 3 weeks after the infection12 and the patient tested positive for HIV on the same day that the transfusion was administered. Futhermore, there have been no documented cases of HIV transmission by blood transfusion in South Africa since nucleic acid testing was introduced in 2005.13 The blood donor was traced and tested negative for HIV, so effectively eliminating blood transfusion as a possible cause.
-
The possibility that the infant was not the mother's child owing to accidental switching of babies at birth was considered. After extensive counselling and at the parents' request, DNA analysis was done using the 15 short tandem repeat polymorphic markers and revealed that this was indeed the mother's child.
- Sexual abuse of the child was unlikely in view of the lengthy hospital stay and the lack of suggestive signs on physical examination.
There have been few cases of father-to-child transmission documented worldwide. The mechanisms of transmission have been speculative, requiring phylogenetic analysis of the virus in both father and child.14
The cause of HIV infection in this child poses a major diagnostic dilemma. The most likely explanation is iatrogenic transmission during his hospital admissions; however, other possibilities cannot be excluded. Cases like these must be actively reported to the registry created by Tygerberg Children's Hospital;9 alternatively, registries can be established at regional virology laboratories to determine the causes of horizontal or unexplained HIV transmission in children. This will provide a greater platform for future research.
The clinical virologist and laboratory staff play a crucial role in the releasing of confidential results. It is of the utmost importance that there is good quality control and that all samples are checked, verified and then released. It is also imperative that equipment is validated and calibrated and that diagnostic kits and reagents have not expired. The clinician should ensure that samples are correctly labelled and that tests are correctly ordered.
There have been very few cases of a discordant result regarding transmission of HIV between parent and child in the South African literature.9 The disclosure of a discordant result has tremendous psychological, social, emotional and legal implications for the family and health care personnel involved. The investigation of such a result requires a multidisciplinary approach to determine the exact cause of transmission.
References
1. Newell ML. Mechanisms and timing of mother-to-child transmission of HIV 1. AIDS 1998; 12: 831-837. [ Links ]
2. Gisselquist D, Potterat JJ, Brody S. HIV transmission during paediatric health care in sub-Saharan Africa – risks and evidence. S Afr Med J 2004; 94: 109-116. [ Links ]
3. HIV COMBI performed or used on ELECSYS. Mannheim, Germany: Roche Diagnostics. [ Links ]
4. Amplicor HIV 1 DNA tests, version 1.5. Branchburg, NJ: Roche Molecular Systems. [ Links ]
5. Rivera-Hernandez DM. HIV infection. eMedicine 11 June 2007. http://www.emedicine.com/ped/TOPIC1027.HTM (accessed 1 October 2008). [ Links ]
6. Gürtler L. Difficulties and strategies of HIV diagnosis. Lancet 1996; 348: 176-179. [ Links ]
7. Wilkinson D, Wilkinson N, Lombard C, et al. On-site HIV testing in resource-poor settings: is one rapid test enough? AIDS 1997; 11: 377-378. [ Links ]
8. SD Bioline HIV 1/2 3.0 Rapid Test Procedure. Suwon, Korea: Standard Diagnostics, Inc. [ Links ]
9. Hiemstra R, Rabie H, Schaaf HS, et al. Unexplained HIV-1 infection in children – documenting cases and assessing for possible risk factors. S Afr Med J 2004; 94: 189-193. [ Links ]
10. Baggaley R, Boily MC, White R, et al. Risk of HIV-1 transmission for parenteral exposure and blood transfusion: a systematic review and meta-analysis. AIDS 2006; 20: 805-812. [ Links ]
11. Schreiber GB, Busch MP, Kleinman SH, Korelitz JJ. The risk of transfusion-transmitted viral infections. N Engl J Med 1996; 334: 1685-1690. [ Links ]
12. Glass AJ. Diagnosis and monitoring of HIV infection. S Afr Fam Pract 2006; 48(8): 46. [ Links ]
13. Haemovigilance: Annual Report 2006. Johannesburg: South African National Blood Service. http://www.sanbs.org.za (accessed 1 October 2008). [ Links ]
14. Ceballos A, Andreani G, Gonzalez Ayala SE, et al. Epidemiological and molecular evidence of two events of father-to-child HIV type 1 horizontal transmission. AIDS Res Hum Retroviruses 2004; 20: 789-793. [ Links ]
Accepted 29 October 2008.
* Corresponding author: M Mitha (momitha@telkomsa.net)














