Serviços Personalizados
Artigo
Indicadores
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares em Google
Similares em Google
Compartilhar
SAMJ: South African Medical Journal
versão On-line ISSN 2078-5135
versão impressa ISSN 0256-9574
SAMJ, S. Afr. med. j. vol.99 no.5 Pretoria Mai. 2009
ORIGINAL ARTICLES
Mental health service use among South Africans for mood, anxiety and substance use disorders
Soraya SeedatI, *; David R WilliamsII; Allen A HermanIII; Hashim MoomalIV; Stacey L WilliamsV; Pamela B JacksonVI; Landon MyerVII; Dan J SteinVIII
IMB ChB, FCPsych (SA), PhD, MRC Stress and Anxiety Disorders Unit, Department of Psychiatry, Stellenbosch University, Tygerberg, W Cape
IIMPH, PhD, Department of Society, Human Development and Health, Harvard School of Public Health, and Department of African and African American Studies, Harvard University, Cambridge, Mass., USA
IIIMD, PhD, National School of Public Health, University of Limpopo (Medunsa Campus), Pretoria
IVMB BCh, DTM&H, DPH, MMed (Public Health), African Public Health Initiatives, Johannesburg
VPhD, Department of Psychology, East Tennessee State University, Johnson City, Tenn., USA
VIPhD, Department of Sociology, Indiana University, Bloomington, Ind., USA
VIIMB ChB, PhD, School of Public Health and Family Medicine, University of Cape Town
VIIIFRCPC, PhD, DPhil, Department of Psychiatry and Mental Health, University of Cape Town
ABSTRACT
BACKGROUND: Europe and North America have low rates of mental health service use despite high rates of mental disorder. Little is known about mental health service use among South Africans.
DESIGN: A nationally representative survey of 4 351 adults. Twelve-month DSM-IV (Diagnostic and Statistical Manual, 4th edition) diagnoses, severity, and service utilisation were determined using the World Health Organization Composite International Diagnostic Interview (CIDI). Twelve-month treatment was categorised by sector and province. South Africans in households and hostel quarters were interviewed between 2002 and 2004 in all nine provinces.
OUTCOME MEASURES: 4 317 respondents 18 years and older were analysed. Bivariate logistic regression models predicted (i) 12-month treatment use of service sectors by gender, and (ii) 12-month treatment use by race by gender.
RESULTS: Of respondents with a mental disorder, 25.2% had sought treatment within the previous 12 months; 5.7% had used any formal mental health service. Mental health service use was highest for adults with mood and anxiety disorders, and among those with a mental disorder it varied by province, from 11.4% (Western Cape) to 2.2% (Mpumalanga). More women received treatment, and this was largely attributable to higher rates of treatment in women with mood disorders. Age, income, education and marital status were not significantly associated with mental health service use. Race was associated with the treatment sector accessed in those with a mental disorder.
CONCLUSIONS: There is a substantial burden of untreated mental disorders in the South African population, across all provinces and even in those with substantial impairment. Greater allocation of resources to mental health services and more community awareness initiatives are needed to address the unmet need.
Of the national burden of disease, neuropsychiatric disorders are third only to HIV/AIDS and infectious disease, according to revised DALY (disability-adjusted life-years) estimates for the year 2000.1,2 Yet mental health services are grossly under-resourced and there are many barriers to health care for the mentally ill.3,4 Barriers include lack of accessibility, acceptability and availability of services, stigma, lack of awareness, perceptions that treatment may not be effective, cultural beliefs, and language problems.5,6 Failure and delays in treatment seeking for mental disorders are greater and more pervasive in developing countries, contributing to high levels of unmet need.7
South Africa has a legacy of racially inequitable, fragmented and inadequately resourced mental health care services,3,8 characterised by provincial variability.4 Findings suggest that two-thirds of patient contacts with mental health services occur through ambulatory care services, with low outpatient attendance rates corresponding with low admission rates in most provinces.9 No systematic data exist on (i) the current use of health (and non-health) services for the mentally ill, or (ii) the nature and extent of unmet treatment needs. Nationally it is critical to identify how to allocate resources more efficiently and equitably across provinces and ensure that the mentally ill receive adequate and appropriate care. To do this it is important to develop population-level insights into the unmet need for mental health services among individuals with mental disorders. As part of the South African Stress and Health (SASH) study, we examined 12-month mental health service use and its association with socio-demographic (gender, race, province) and mental disorder variables in the general population. We expand on findings10 by reporting on (i) provincial prevalence rates of service use for mental health reasons by type of service, and (ii) gender differences in patterns of use.
Methods
Data for the SASH study were collected between January 2002 and June 2004 from a national probability sample of 4 351 adult South Africans living in households or hostel quarters.11 Hostel quarters were included to maximise coverage of young working-age males. Individuals in institutions or the military were not included. All racial and ethnic backgrounds were included. The overall response rate was 85.5%. The sample was selected using a three-stage stratified and clustered area probability sample design. The first stage selected a stratified probability sample of primary sample areas based on the 2001 South African census enumeration areas (EAs). The second stage selected a probability sample of housing units from each EA. The third stage involved the random selection of one adult respondent in each sampled housing unit without replacement. The final sample of respondents was weighted to adjust for differential probabilities of selection within households, for differential non-response. A post-stratification weight was used to make the sample distribution comparable to the population distribution in the 2001 South African census for age, gender, and province.
Version 3.0 of the World Health Organization (WHO) Composite International Diagnostic Interview (CIDI 3.0) was used to assess the presence of DSM-IV (Diagnostic and Statistical Manual, 4th edition) disorders.12 SASH interviewers were lay individuals extensively trained in the use of the CIDI. The translation of the English version of the CIDI into the six other languages used in the SASH was carried out according to WHO recommendations of iterative back-translation conducted by panels of bilingual and multilingual experts. The interviews, lasting an average of 3½ hours, were conducted face to face in English, Afrikaans, Zulu, Xhosa, Northern Sotho, Southern Sotho or Tswana, many requiring more than one visit to complete. Mental disorders assessed in the SASH study were anxiety disorders (panic disorder, agoraphobia, social phobia, generalised anxiety disorder, post-traumatic stress disorder), mood disorders (major depressive disorder, dysthymia), substance use disorders (alcohol abuse, alcohol dependence, drug abuse, drug dependence), and intermittent explosive disorder.13 Disorders were further classified according to severity.12
Respondents were asked if they had seen any treatment provider for problems with their emotions, nerves, mental health or use of alcohol or drugs in the past 12 months. For each type of professional, the number of visits in the past 12 months, the duration of the visit, and treatment continuation/discontinuation were assessed. Treatment providers were classified into general medical provider (medical doctor, nurse or other health professional not in a mental health setting), mental health specialist (psychiatrist, psychologist, other mental health professional), human services (religious or spiritual advisor, social worker), and complementary and alternative medicine (CAM) (traditional healer, chiropractor or other healer not in a health setting). The mental health and general medical sectors together were also defined as 'any health care'.
The study was approved by the Human Subjects Committees of the University of Michigan and Harvard Medical School, and by a single project assurance of compliance from the Medical University of South Africa (MEDUNSA) that was approved by the National Institute of Mental Health (USA).
Analysis procedures
Patterns of service use were established by calculating proportions in treatment and the median numbers of visits among those in treatment. All gender-stratified and province-stratified analyses were limited to four service use categories (any mental health care, any health care, any non-health care, and any treatment). Logistic regression was used to assess socio-demographic and disease predictor variables of receiving any treatment within the past 12 months and reported as odds ratios (OR) and 95% confidence intervals (CI).
Socio-demographic variables included age (<35, 35 - 49, 50 - 64, >65 years), education (0 - 6, 7 - 9, 10 - 12, >13 years of education), gender, race (black, coloured, Indian, white), marital status (never married, separated/widowed/divorced, married/cohabiting), income (low, low average, high average, high), income quintiles (rands) (0, 1 - 1 500, 1 501 - 16 500, 16 501 - 97 500, >97 501); while diagnostic variables (yes/no) included any anxiety, any mood, and any substance use disorder. Racial categories were used as a marker of historical social and economic opportunity with respect to health-related outcomes. Weighting and geographical clustering of the data were taken into account in data analyses by using the Taylor series linearisation method in the SUDAAN statistical package.14 In logistic regression analysis, multivariate significance tests were calculated using Wald chi-square tests. Statistical significance was based on two-sided tests set at p<0.05.
Results
12-month use of mental health services: Gender, race, provincial correlates
Of the 4 317 respondents with complete data, 15.3% had sought treatment in the prior 12 months, including 25.2% with a DSM-IV disorder (21.8% of males and 27.8% of females) and 13.4% with no disorder (12.0% of males and 14.6% of females). There were no significant gender differences for any of these observations. Furthermore, only 5.7% of those with a mental disorder had received any mental health care (Table I). The sectors most frequently used were the general medical sector, followed by the mental health care sector. Generally, service use was highest among respondents with an anxiety disorder (27.6%). Use of the mental health service sector was highest for anxiety (6.8%) and mood disorders (6.8%). The association of service use with race also differed by sector. Among those with a 12-month disorder, blacks were most likely to have accessed the CAM sector (OR=25, χ2=12.81, p=0.005), while whites (OR=10.9) and coloureds (OR=4.1) were more likely than blacks to have seen a psychiatrist (χ2=19.62, p=0.0002). Whites with a 12-month disorder were also more likely than blacks to have used other mental health services (OR=5.29, χ2=14.73, p=0.0006). Although women had higher rates of treatment seeking overall, among 12-month cases there were no significant gender differences, except for mood disorders, for which the rate of treatment – particularly in the non-health care sector – was higher for women (Table II).

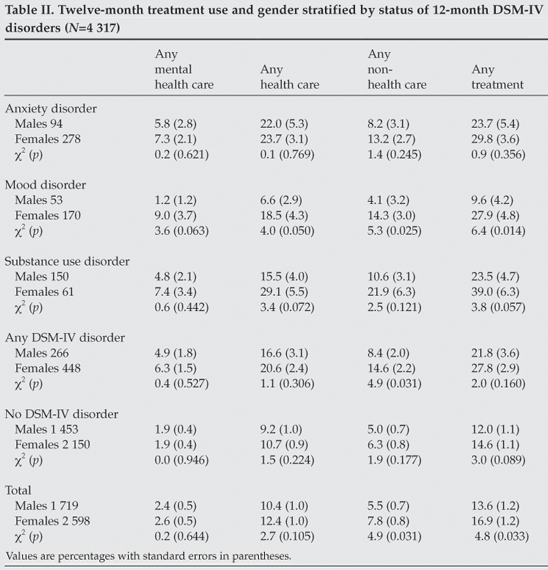
Table III shows 12-month treatment use stratified by province for respondents with and without a mental disorder. Across the nine provinces, the Western Cape had the highest rate of mental health use among respondents with a DSM-IV disorder (11.4%), while Mpumalanga had the lowest rate in that sector (2.2%). When respondents with no disorder were included, rates of mental health treatment ranged from 1.6% (Eastern Cape) to 4.4% (Western Cape).

Service use by severity
Only about one-fourth of respondents with either a moderate (26.6%) or a severe (26.2%) disorder had used services in the past year, with only 5.3% of moderate cases and 9.4% of severe cases receiving any mental health care. There were no significant gender differences between disorder severity and use of any mental health care.
Number of visits
The mean number of past year visits for those with a mental disorder in any sector was 5.1 (0.7). The highest number of visits occurred in the 'any mental health care' sector. Generally, there were no significant differences between males and females in the number of visits across sectors, except for any non-health care service use, where females had more visits than males (4.1±0.5 v. 2.8±0.2, t=–2.7, p=0.010). Respondents with an anxiety disorder in any treatment sector had the highest mean number of visits (6.4±1.2). Those who reported a substance use disorder had the lowest number of visits (3.8±0.5). The mean number of visits for those without a mental disorder was 4.4 (0.2).
Service use predictors
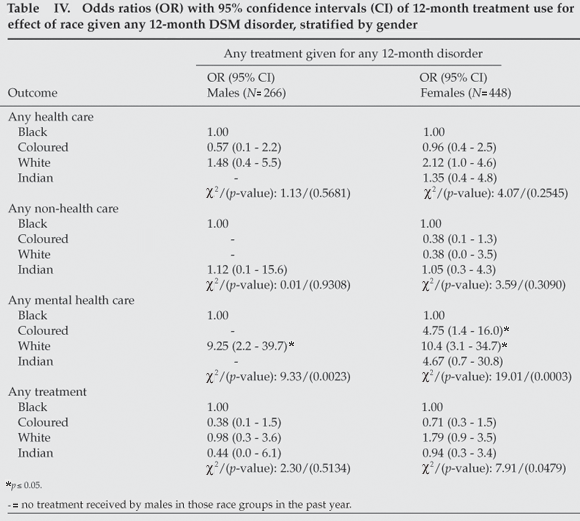
No socio-demographic variable predicted treatment within the previous 12 months in cases of anxiety, mood or substance use disorder. However, stratification by gender yielded the following predictors of service use: (i) among women with any mental disorder, age (35 - 49 years) (OR=4.26, χ2=8.21, p=0.041) and any substance use disorder (OR=1.85, χ2=4.54, p=0.033) were associated with an elevated odds of receiving any treatment; and (ii) among men with any mental disorder, the presence of a mood disorder was associated with a lower odds of receiving treatment in any sector. Considering the effect of race in respondents with a 12-month disorder, stratified by gender, white females and males and coloured females had the highest odds of seeking mental health services (Table IV).
Discussion
These results demonstrate a high level of unmet need for South Africans with common mental disorders. Even among severe and moderate cases, only about 1 in 4 had obtained some form of treatment for problems with their mental health or substance use in the 12 months before interview. The 15.4% of the population who reported any 12-month service use is similar to that in some WMH survey countries (e.g. USA and New Zealand), and substantially higher than rates in other low- and low- middle income countries (e.g. China, Nigeria, Ukraine, Mexico).15
More respondents used the general medical sector than the mental health sector for mental health problems. This is compatible with mental health services in the country, where access to specialty mental health care tends to be reserved for the very ill, and where the majority of those with mental disorders have first accessed community-level primary health care facilities. Overall, use of the CAM sector was common, especially among black respondents, who were the least likely to have accessed the mental health sector. This is not surprising given the high use of indigenous traditional healers by this group (Sorsdahl et al., unpublished data). Differences in perceived acceptability of using health services for mental health reasons may also be contributing to differences in service use.
Mental health consultation rates were highest among those with mood and anxiety disorders and lowest among those with substance use disorders. This is consistent with other surveys.16 We did not find any socio-demographic predictors of service use in respondents with these disorders. However, notable patterns of use emerged from the data. For example, there were provincial variations, with an up to fivefold difference in rates of mental health service use among those with mood, anxiety and substance use disorders, with the highest rates documented for the Western Cape province. This too is consistent with data on community indicators for patient service utilisation of mental health services, with the highest outpatient attendance rates in the Western Cape (458 patient attendances per 100 000 population) relative to the other provinces.9 In the aforementioned study, utilisation of both hospital and community services was low (below the national rate) in Mpumalanga, Limpopo, the Free State and KwaZulu-Natal, similar to our findings. Further study is needed to explain differences in the type of resource preferred and used for mental health reasons across provinces.
We found that gender was significantly related to any 12-month service use, particularly for mood disorders, with women more likely to seek treatment than men, mirroring other WMH surveys.15 The gender difference could be explained by women being more likely to acknowledge symptoms of affective distress than men.17
To our surprise, respondents without any of the disorders assessed in the survey accounted for a high proportion (13.4%) of respondents in treatment, with the highest proportion of treatment in the general medical sector, and few receiving care within the formal mental health care system. The potential draining of limited treatment resources to persons without apparent need is grounds for concern. It is likely that some respondents classified without a 12-month disorder actually had one, since the CIDI does not provide a fully comprehensive assessment of all DSM-IV disorders. Alternatively, a proportion of respondents may have been sub-threshold cases that were assessed with the CIDI18 but not captured by the categorical diagnostic ascertainment. High levels of service use for somatisation may also contribute to treatment seeking among those without diagnoses.
These findings should be interpreted with the following additional limitations. First, we relied on self-report measures of service use, which may have underestimated rates of unmet treatment need, particularly if mental health care seeking is stigmatised. Second, the influence of co-morbidity on service utilisation was not explored. Third, schizophrenia and other psychotic disorders were not evaluated, which is the case throughout the WMH surveys, as earlier validation studies have shown that these disorders lend themselves to over-estimation in lay-administered interviews. Fourth, reliability and validity of the six translated versions used in the survey were not established; in particular, the lack of a clear dose-response relationship may reflect inconsistencies and/or inaccuracies of disorder severity ratings by lay-administered interviewers using the CIDI. Fifth, persons in institutional settings and the military were excluded.
Nevertheless, this study provides the first national, population-level insights into mental health care seeking in South Africa. The findings are informative in guiding the distribution and targeting of resources and interventions for mental disorders across the country. Measures such as greater allocation of resources to mental health services and community initiatives to promote awareness of mental health and available services are needed to help address the huge unmet need.
Acknowledgements. The South African Stress and Health study was carried out in conjunction with the World Health Organization World Mental Health (WMH) Survey Initiative. We thank the WMH staff for assistance with instrumentation, fieldwork, and data analysis. These activities were supported by the US National Institute of Mental Health (R01MH070884), the John D and Catherine T MacArthur Foundation, the Pfizer Foundation, the US Public Health Service (R13-MH066849, R01-MH069864 and R01 DA016558), the Fogarty International Center (FIRCA R01-TW006481), the Pan American Health Organization, Eli Lilly and Company, Ortho-McNeil Pharmaceutical, Inc., GlaxoSmithKline, and Bristol-Myers Squibb. The South African Stress and Health study was funded by grant R01-MH059575 from the National Institute of Mental Health and the National Institute of Drug Abuse with supplemental funding from the South African Department of Health and the University of Michigan. Dan Stein and Soraya Seedat are also supported by the Medical Research Council of South Africa. A complete list of WMH publications can be found at http://www.hcp.med.harvard.edu/wmh/.
The authors thank Kathleen McGaffigan (Harvard University) for her assistance with the statistical analyses.
References
1. Bradshaw D, Groenewald P, Laubscher R, et al. Initial burden of disease estimates for South Africa, 2000. S Afr Med J 2003; 93(9): 682-688. [ Links ]
2. Bradshaw D, Norman R, Schneider M. A clarion call for action based on refined DALY estimates for South Africa. S Afr Med J 2007; 97(6): 438, 440. [ Links ]
3. Lund C, Flisher AJ. South African mental health process indicators. J Ment Health Policy Econ 2001; 4(1): 9-16. [ Links ]
4. Lund C, Flisher AJ. Staff/bed and staff/patient ratios in South African public sector mental health services. S Afr Med J 2002; 92(2): 157-161. [ Links ]
5. Kessler RC, Berglund PA, Bruce ML, et al. The prevalence and correlates of untreated serious mental illness. Health Serv Res 2001; 36(6 Pt 1): 987-1007. [ Links ]
6. Seedat S, Stein DJ, Berk M, Wilson Z. Barriers to treatment among members of a mental health advocacy group in South Africa. Soc Psychiatry Psychiatr Epidemiol 2002; 37(10): 483-487. [ Links ]
7. Wang PS, Angermeyer M, Borges G, et al. Delay and failure in treatment seeking after first onset of mental disorders in the World Health Organization's World Mental Health Survey Initiative. World Psychiatry 2007; 6(3): 177-185. [ Links ]
8. Emsley R. Focus on psychiatry in South Africa. Br J Psychiatry 2001; 178: 382-386. [ Links ]
9. Lund C, Flisher AJ. Community/hospital indicators in South African public sector mental health services. J Ment Health Policy Econ 2003; 6(4): 181-187. [ Links ]
10. Seedat S, Stein DJ, Herman A, et al. Twelve month treatment of psychiatric disorders in the South African Stress and Health Survey (World Mental Health Survey Initiative). Soc Psychiatry Psychiatr Epidemiol 2008; 43(11): 889-897. [ Links ]
11. Williams DR, Herman A, Kessler RC, et al. The South Africa Stress and Health study: rationale and design. Metab Brain Dis 2004; 19: 135-147. [ Links ]
12. Kessler RC, Ustun TB. The World Mental Health (WMH) Survey Initiative version of the World Health Organization (WHO) Composite International Diagnostic Interview (CIDI). Int J Methods Psychiatr Res 2004; 13(2): 93-121. [ Links ]
13. American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders. 4th ed. Washington, DC: APA, 1994. [ Links ]
14. Research Triangle Institute. SUDAAN: Professional Software for Survey Data Analysis [computer program]. Version 8.0.1. Research Triangle Park, NC: Research Triangle Institute, 2002. [ Links ]
15. Wang PS, Aguilar-Gaxiola S, Alonso J, et al. Use of mental health services for anxiety, mood, and substance disorders in 17 countries in the WHO world mental health surveys. Lancet 2007; 370: 841-850. [ Links ]
16. Andrews G, Issakidis C, Carter G. Shortfall in mental health service utilisation. Br J Psychiatry 2001; 179: 417-425. [ Links ]
17. Kessler RC, Brown RL, Broman CL. Sex differences in psychiatric help-seeking: evidence from four large-scale surveys. J Health Soc Behav 1981; 22(1): 49-64. [ Links ]
18. Druss BG, Wang PS, Sampson NA, et al. Understanding mental health treatment in persons without mental diagnoses: results from the National Comorbidity Survey Replication. Arch Gen Psychiatry 2007; 64(10): 1196-203. [ Links ]
Accepted 2 February 2009.
* Corresponding author: S Seedat (sseedat@sun.ac.za)














