Services on Demand
Article
Indicators
Related links
-
 Cited by Google
Cited by Google -
 Similars in Google
Similars in Google
Share
SAMJ: South African Medical Journal
On-line version ISSN 2078-5135
Print version ISSN 0256-9574
SAMJ, S. Afr. med. j. vol.99 n.5 Pretoria May. 2009
ORIGINAL ARTICLES
The South African Stress and Health (SASH) study: 12-month and lifetime prevalence of common mental disorders
Allen A HermanI, *; Dan J SteinII; Soraya SeedatIII; Steven G HeeringaIV; Hashim MoomalV; David R WilliamsVI
IMD, PhD, National School of Public Health, University of Limpopo (Medunsa Campus), Pretoria
IIFRCPC, PhD, DPhil, Department of Psychiatry and Mental Health, University of Cape Town
IIIMB ChB, FCPsych (SA), PhD, MRC Stress and Anxiety Disorders Unit, Department of Psychiatry, Stellenbosch University, Tygerberg, W Cape
IV PhD, University of Michigan, Ann Arbor, Mich., USA
VMB BCh, DTM&H, DPH, MMed (Public Health), African Public Health Initiatives, Johannesburg
VI MPH, PhD, Department of Society, Human Development and Health, Harvard School of Public Health, and Department of African and African American Studies, Harvard University, Cambridge, Mass., USA
ABSTRACT
BACKGROUND: The South African Stress and Health (SASH) study is the first large-scale population-based study of common mental disorders in the country. This paper provides data on the 12-month and lifetime prevalence of these conditions.
METHODS: Data from a nationally representative sample of 4 351 adults were analysed. Mental disorders were assessed with the Composite International Diagnostic Interview (CIDI). An extensive survey questionnaire detailed contextual and socio-demographic factors, onset and course of mental disorders, and risk factors. Simple weighted cross-tabulation methods were used to estimate prevalence, and logistic regression analysis was used to study correlates of 12-month and lifetime prevalence.
RESULTS: The lifetime prevalence for any disorder was 30.3%, and the most prevalent 12-month and lifetime disorders were the anxiety disorders. The Western Cape had the highest 12-month and lifetime prevalence rates, and the lowest rates were in the Northern Cape.
CONCLUSIONS: The SASH study shows relatively high 12-month and lifetime prevalence rates. These findings have significant implications for planning mental health services.
At the end of the apartheid era, the African National Congress (ANC) formulated a broad policy framework that forms the basis for the current enabling health care legislation in South Africa. The ANC government developed a health care delivery policy based on the district health system that was designed to extend the availability of appropriate health care. This policy placed most of the public mental health care within an integrated primary health care system. To achieve this primary health care goal, population-based data that identify the prevalence of mental health disorders, risk factors for these disorders, patterns of treatment, barriers to treatment, and the potential approaches to improving care are required.
The South African Stress and Health (SASH) study is the first large population-based mental health epidemiological survey in South Africa.1 It was carried out as part of the World Health Organization World Mental Health (WMH) Survey Initiative.2,3 The SASH study is placed within the historical context of early post-apartheid South Africa, where communities are still sharply divided by racial/ethnic and national identities and socio-economic disparities.4,5
In this paper we describe the 12-month and lifetime prevalence of mental health disorders, as well as their socio-demographic correlates. Additional analyses of the prevalence of 12-month and lifetime mental illness and 12-month treatment for mental illness are available,6,7 but the current paper includes new data such as provincial prevalence estimates.
Methods
Sampling methods and sample size
The SASH sample was a three-stage, area probability sample of 4 351 adults (aged >18 years) of all races and ethnic groups living in households and single-sex migrant labourer group quarters (hostels) in South Africa. The survey population did not include individuals living in prisons, hospitals and mental institutions or members of the military who resided on military bases. Sample selection and data collection were completed from 2003 to 2004. Details of the three-stage sampling procedure have been published elsewhere.8 A total sample of 5 089 households was selected. Field interviews were obtained from 4 433 (87.1%) of the designated respondents selected at random from the eligible persons in each sample household. On the basis of quality control criteria, including completion of critical sections in the SASH questionnaire, a total of 4 351 (98.1%) of the field interviews were retained for use in analysis.
Measures
Diagnostic assessment of lifetime and 12-month DSM-IV disorders
Diagnoses of DSM-IV (Diagnostic and Statistical Manual, 4th edition) disorders were made using Version 3.0 of the World Health Organization Composite International Diagnostic Interview (CIDI),9 a fully structured lay-administered diagnostic interview that generates diagnoses according to the definitions and criteria of both the ICD-10 (International Statistical Classification of Diseases and Related Health Problems, 10th revision)10 and DSM-IV11 diagnostic systems. The disorders included in the SASH study were anxiety disorders (panic disorder, agoraphobia without panic, social phobia, generalised anxiety disorder and post-traumatic stress disorder); mood disorders (major depressive episode); impulse control disorders (intermittent explosive disorder); and substance use disorders (alcohol abuse, alcohol dependence, substance abuse, substance dependence). Lifetime prevalence, age of onset and 12-month prevalence were assessed separately for each disorder. Bipolar disorder, oppositional-defiant disorder, conduct disorder, attention deficit/hyperactivity disorder, obsessive-compulsive disorder, specific phobia and separation anxiety disorder were not assessed in the SASH study. Twelve-month cases were classified by severity using a system described in detail elsewhere2 as serious, moderate, or mild.
Predictor variables
Predictor variables in analyses of lifetime data include age of onset (AOO) of the focal disorder, cohort (defined by age at interview), gender, race (black, coloured, white, Indian), education (current students or non-students with 0 - 11, 12, 13 - 15, or 16+ years of education), and marital status (currently married/cohabiting, previously married, or never married). Variables in analyses of 12-month data included gender, race, cohort, education and marital status (all categorised as described previously). In addition, family income (low, low average, high average, and high) and urban or rural status were included.
Analysis procedures
The data were weighted to adjust for differential probabilities of selection of respondents within households and differential non-response as well as to adjust for residual differences between the sample and the South African population on the cross-classification of socio-demographic variables. An additional weight was used to adjust for differences in probability of selection into that sample. Simple cross-tabulation methods were used to estimate prevalence. Logistic regression analysis12 was used to study correlates of 12-month and lifetime prevalence.
Results
Lifetime prevalence of DSM-IV mental disorders
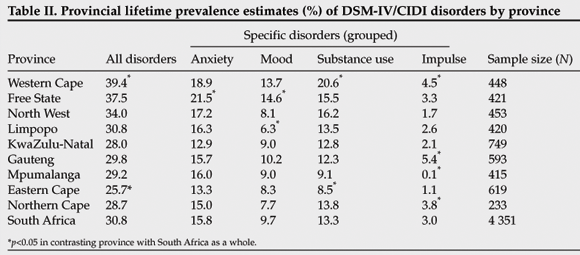
Table I shows the lifetime prevalence of mental disorders. The lifetime prevalence for any disorder was 30.3%; 11.2% of respondents had two or more lifetime disorders and 3.5% had three or more lifetime disorders. The most prevalent class of lifetime disorders was anxiety disorders (15.8%), followed by substance use disorders (13.3%) and mood disorders (9.8%). The most prevalent individual lifetime disorders were alcohol abuse (11.4%), major depressive disorder (9.8%) and agoraphobia without panic (9.8%).

Significant differences in lifetime prevalence of mental disorders occurred across the nine provinces, with the Western Cape having the highest rate at 42% and the Northern Cape the lowest at 29%. The Western Cape and Free State had prevalence rates that were significantly higher than the countrywide rates, and the Eastern Cape and Northern Cape had rates that were significantly lower (Table II). These provincial differences held for all mental disorders except impulse disorders, where the lowest provincial rates were found in Mpumalanga (0.2%) and the Eastern Cape (0.1%). Significant differences in prevalence with age occurred with panic disorder and generalised anxiety disorder (showing a general monotonic increase in rates with age) and drug abuse and drug dependence (showing a tendency to peak at 35 - 49 years). There was a marginally significant increase in the rate of mood disorders with increasing age.
The projected lifetime risk of any mental disorders of 47.5% was higher than the lifetime prevalence of 30.3%. The greatest difference between projected risk and prevalence was observed for anxiety disorders (30.1% v. 15.8%, a difference of 14.3%), followed by major depressive disorder. The smallest difference between lifetime risk and prevalence was observed for substance use disorders (17.5% v. 13.3%, a difference of 3.2%). Disorders with a later AOO had a greater difference between projected risk and prevalence.
Prevalence and severity of 12-month disorders
Table III shows the 12-month prevalence of mental disorders. Among the broad classes of disorders, anxiety disorders were the most prevalent (8.1%), followed by substance use disorders (5.8%) and mood disorders (4.5%). The most common disorders were major depressive disorder (4.9%), agoraphobia without panic (4.8%) and alcohol abuse (4.5%). Seventeen per cent of the respondents had one or more 12-month mental disorder; among these, more than half of cases had only one disorder (11%), with smaller proportions having two (3.9%) or more (1.4%).
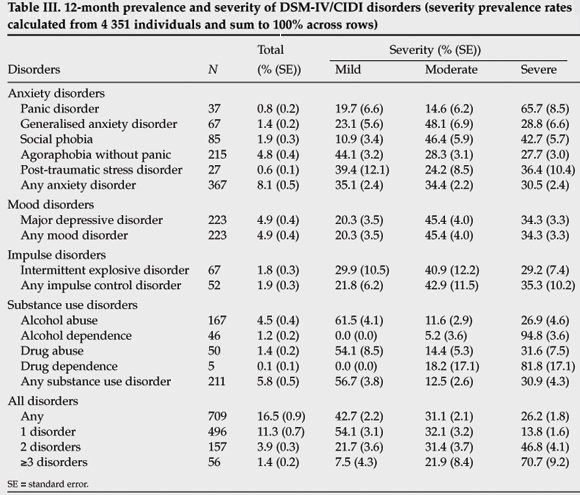
Of the 12-month prevalent cases, 26% were classified as severe, 31% as moderate and 43% as mild. A severe disorder was strongly associated with co-morbidity, with 14% of respondents with severe disorders having one diagnosis, 47% having two, and 71% having three or more. The proportion of severe disorders was similar in the four broad groups of disorders. The anxiety disorder with the greatest proportion of severe cases was panic disorder (66%), followed by social phobia (43%) and post-traumatic stress disorder (36%). Slightly more than one-third of individuals with major depressive episode had a severe disorder. Alcohol (95%) and drug (82%) disorders tended to be severe diagnoses.
The provincial rates of 12-month prevalence showed the same significant excess in the Western Cape and Free State (as seen in the lifetime prevalence rates) compared with the rest of the country. Much of the excess was reflected in an increase in moderate disorders in the Western Cape and Free State and an excess in serious disorders in the Western Cape (Table IV).

Socio-demographic correlates of 12-month disorders and treatment
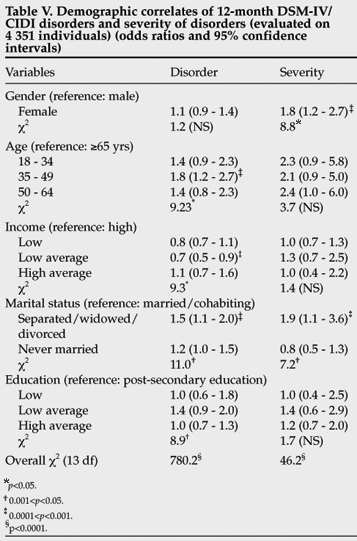
Being female was associated with increased severity of 12-month mental disorders. Compared with individuals aged 65 and older, there was an increased prevalence of any disorders in 35 - 49-year-olds. There was an increasing trend of treatment with increasing age to 64 years. Individuals with a low-average income had a decreased risk of disorders compared with individuals with high incomes. Individuals who were separated, widowed or divorced had an increased risk of any disorder and more severe disorders compared with married individuals (Table V).
Mood and anxiety disorders were more common among women, and substance use disorders were more common among men. Mood disorders and impulse-control disorders tended to be disorders of younger individuals, while substance use disorders were most common among 35 - 49-year-olds. Mood disorders were more frequent among separated, widowed and divorced individuals and among people with only an elementary school education. Anxiety disorders were associated with being female (except among those older than 65 years) and with an elementary education (especially among 35 - 49-year-olds). Mood disorders were associated with being female among 18 - 34-year-olds and individuals with an elementary and high-school education (especially 18 - 34-year-olds). Substance use disorders were more frequent among men (of all ages except >65-year-olds) and individuals with more than a high school education (compared with those who were still students). There were no interactions between age and education and age and sex for specific disorders.
Discussion
The interpretation of our results should take into account those limitations that are specific to the SASH study and common across WMH surveys: (i) we did not assess a number of key DSM-IV disorders, and some individuals who were assessed as having no disorder may have had a clinical disorder not evaluated in the SASH study; (ii) homeless and institutionalised persons were excluded; (iii) although the SASH study had a relatively high response rate, the biases that are common with non-response errors, errors in recall, non-reporting, and diagnostic errors are likely to lead to an underestimation of prevalence and unmet treatment needs; and (iv) the SASH interview was lay-administered, which may lead to systematic error.
South Africa has a relatively high 12-month prevalence of anxiety and mood disorders when compared with the other countries in the WMH Survey. Only Belgium, France, Germany, New Zealand, The Netherlands, Colombia, Lebanon and the USA have higher rates of anxiety disorders, and Belgium, Lebanon, Colombia, The Netherlands, France, Ukraine, Israel, New Zealand and the USA have higher rates of mood disorders. Twenty-six per cent of DSM-IV disorders in South Africa are considered severe, with only Belgium, Israel and The Netherlands having higher rates of severe DSM-IV disorders.
Only two African countries participated in the WMH Survey, South Africa and Nigeria. The Nigerian Survey of Mental Health and Well-Being was conducted in five of the six geopolitical regions of that country.13 Only 1 in 17 Nigerians had had a DSM disorder in the preceding 12 months, compared with around 1 in 6 South Africans. Only 1 in 10 Nigerians had a lifetime DSM disorder, compared with 1 in 3 South Africans. Compared with Nigerians, twice as many South Africans had lifetime anxiety disorders, 4 times as many had lifetime mood disorders, and almost 6 times as many had substance use disorders. Reasons for differences in prevalence of mental disorders in high- and low-income countries require further investigation.
The geographical differences in 12-month and lifetime prevalence rates across provinces are also striking. The Western Cape, which has the highest prevalence of common mental disorders, was the first region of South Africa to be colonised and has a high level of urbanisation. In contrast, rural provinces generally have lower rates of common mental disorders, with the lowest rates in the Eastern Cape.
A number of previous mental health surveys have been conducted in South Africa. Robertson and Juritz24 described rates of behaviour disorders among 10- and 13-year-olds as between 10% and 20% (teacher assessment v. parent assessment). Flisher et al.25 reported rates of attempted suicide of 7.8% and suicidal ideation of 19% among high-school students. These rates were similar to those described by Mhlongo and Peltzer26 and Wild et al.27 Tobacco, drug and alcohol use disorders are prevalent among adolescents28,29 and adults30-32 in South Africa. In a comparative study of post-traumatic stress disorder among Grade 10 schoolchildren in Kenya and South Africa, Seedat et al.33 reported similar rates of exposure to both more than one trauma and three traumas (83%, 85% and 44%, 45%) but very different rates of full-symptom post-traumatic stress disorder among South African (22%) and Kenyan (5%) adolescents.
Pillay and Kriel18 examined the use patterns of women in a district-level clinical psychology service provided at community mental health clinics, district general hospitals, and a primary health care centre serving a population of slightly more than 500 000 people. They reported rates of 21% for depression, 14% for suicidal behaviour and 9.5% for anxiety among women attending the service. Triant34 reported rates of 32% for depression and 13% for major depression, Bhagwanjee et al.35 reported a combined rate of generalised anxiety disorder and depression of 23.9%, Cooper et al.36 reported a rate of 34.7% for postpartum depression, and Carey et al.37 reported rates of 19.9% for post-traumatic stress disorder, 37% for depression and 18.4% for somatisation disorder among community health care centre attendees.
Most of the studies described in this discussion are clinic- or hospital-based studies or studies of children in a high-school setting. These data reflect variations in rates of mental illness but emphasise a large burden of mental health disease. The SASH study is the first large-scale study of the descriptive epidemiology of mental health in South Africa and gives us opportunities to describe the distributions of mental disorders, as well as their associated socio-demographic features.
Acknowledgements. The South African Stress and Health study was carried out in conjunction with the World Health Organization World Mental Health (WMH) Survey Initiative. We thank the WMH staff for assistance with instrumentation, fieldwork and data analysis. These activities were supported by the US National Institute of Mental Health (R01MH070884), the John D and Catherine T MacArthur Foundation, the Pfizer Foundation, the US Public Health Service (R13-MH066849, R01-MH069864, and R01 DA016558), the Fogarty International Center (FIRCA R01-TW006481), the Pan American Health Organization, Eli Lilly and Company, Ortho-McNeil Pharmaceutical, Inc., GlaxoSmithKline, and Bristol-Myers Squibb. The South African Stress and Health study was funded by grant R01-MH059575 from the National Institute of Mental Health and the National Institute of Drug Abuse with supplemental funding from the South African Department of Health and the University of Michigan. Dan Stein and Soraya Seedat are also supported by the Medical Research Council of South Africa. A complete list of WMH publications can be found at http://www.hcp.med.harvard.edu/wmh/
References
1. Williams DR, Herman A, Kessler RC, et al. The South Africa Stress and Health Study: Rationale and design. Metab Brain Dis 2004; 19: 135-147. [ Links ]
2. Kessler RC, Haro JM, Heeringa SG, Pennell BE, Üstün TB. The World Health Organization World Mental Health Survey Initiative. Epidemiol Psichiatr Soc 2006; 15: 161-166. [ Links ]
3. Demyttenaere K, Bruffaerts R, Posada-Villa J, et al. Prevalence, severity, and unmet need for treatment of mental disorders in the World Health Organization world mental health surveys. JAMA 2004; 291: 2581-2590. [ Links ]
4. Christopher AJ. Linguistic segregation in urban South Africa, 1996. Geoforum 2004; 35: 145-156. [ Links ]
5. Bornman E. National symbols and nation-building in the post-apartheid South Africa. International Journal of Intercultural Relations 2006; 30: 383-399. [ Links ]
6. Stein DJ, Seedat S, Herman A, et al. Lifetime prevalence of psychiatric disorders in South Africa. Br J Psych 2008; 192: 112-117. [ Links ]
7. Seedat S, Stein DJ, Herman AA, et al. Twelve-month treatment of psychiatric disorders in the South African Stress and Health Survey (World Mental Health Survey Initiative). Soc Psychiatry Psychiatr Epidemiol (in press). [ Links ]
8. Herman AA, Williams DR, Stein DJ, Seedat S, Heeringa SG, Moomal H. The South African Stress and Health Study (SASH): A foundation for improving mental health care in South Africa. In: Kessler RC, Ustun TB, eds. The WHO World Mental Health Surveys: Global Perspectives on the Epidemiology of Mental Disorders. Cambridge, UK: Cambridge University Press, 2008. [ Links ]
9. Kessler RC, Üstün TB. The World Mental Health (WMH) Survey Initiative version of the World Health Organization (WHO) Composite International Diagnostic Interview (CIDI). Int J Methods Psychiatr Res 2004; 13: 93-121. [ Links ]
10. World Health Organization. International Classification of Diseases (ICD-10). Geneva: World Health Organization, 1991. [ Links ]
11. American Psychiatric Association. Diagnostic and Statistical Manual. 4th ed. Washington, DC: American Psychiatric Association Press, 1994. [ Links ]
12. Hosmer DW, Lemeshow S. Applied Logistic Regression. New York: John Wiley & Sons, 1989. [ Links ]
13. Gureje O, Lasebikan VO, Kola L, Makuanjuola V. Lifetime and 12-month prevalence of mental disorders in the Nigerian Survey of Mental Health and Well-Being. Br J Psychiatry 2006; 188: 465-471. [ Links ]
14. Phillips HT. The 1945 Gluckman Report and the establishment of South Africa's health centers. Am J Public Health 1993; 83: 1037-1039 [ Links ]
15. Petersen I. Comprehensive integrated primary mental health care for South Africa. Pipedream or possibility? Soc Sci Med 2000; 51: 321-334. [ Links ]
16. Petersen I, Swartz L. Primary health care in the era of HIV/AIDS. Some implications for health systems reform. Soc Sci Med 2002; 55: 1005-1013. [ Links ]
17. Pillay AL, Lockhat MR. Developing community mental health services for children in South Africa. Soc Sci Med 1997; 45: 1493-1501. [ Links ]
18. Pillay AL, Kriel AJ. Mental health problems in women attending district-level services in South Africa. Soc Sci Med 2006; 63: 587-592. [ Links ]
19. Lund C, Flisher AJ. South African mental health process indicators. Journal of Mental Health Policy and Economics 2001; 4: 9-16. [ Links ]
20. Lund C, Flisher AJ. Community/hospital indicators in South African public sector mental health services. Journal of Mental Health Policy and Economics 2003; 6: 181-187. [ Links ]
21. Uys LR, Subedar H, Lewis W. Educating nurses for primary psychiatric care: A South African perspective. Archives of Psychiatric Nursing 1995; 9: 348-353. [ Links ]
22. Swartz L, MacGregor H. Integrating services, marginalizing patients: Psychiatric patients and primary health care in South Africa. Transcultural Psychiatry 2002; 39: 155-172. [ Links ]
23. Kohn R, Szabo CP, Gordon A, Allwood CW. Race and psychiatric services in post-apartheid South Africa: A preliminary study of psychiatrists' perceptions. International Journal of Social Psychiatry 2004; 50: 18-24. [ Links ]
24. Robertson BA, Juritz JM. Behavioural screening of 10- and 13-year-old pupils in selected schools in the Cape Peninsula. S Afr Med J 1988; 73: 24-25. [ Links ]
25. Flisher AJ, Ziervogel CF, Chalton DO, Leger PH, Robertson BA. Risk-taking behaviour of Cape Peninsula high-school students. Part VIII. Sexual behaviour. S Afr Med J 1993; 83: 495-497. [ Links ]
26. Mhlongo T, Peltzer K. Parasuicide among youth in a general hospital in South Africa. Curationis 1999; 22: 72-76. [ Links ]
27. Wild LG, Flisher AJ, Lombard C. Suicidal ideation and attempts in adolescents: Associations with depression and six domains of self-esteem. J Adolesc 2004; 27: 611-624. [ Links ]
28. Flisher AJ, Parry CD, Evans J, Muller M, Lombard C. Substance use by adolescents in Cape Town: Prevalence and correlates. J Adolesc Health 2003; 32: 58-65. [ Links ]
29. Brook JS, Morojele NK, Pahl K, Brook DW. Predictors of drug use among South African adolescents. J Adolesc Health 2006; 38: 26-34. [ Links ]
30. Michalowsky AM, Wicht CL, Moller AT. The psychosocial effects of living in an isolated community. A community health study. S Afr Med J 1989; 75: 532-534. [ Links ]
31. London L. Alcohol consumption amongst South African farm workers: A challenge for post-apartheid health sector transformation. Drug Alcohol Depend 2000; 59: 199-206. [ Links ]
32. Parry CD, Bhana A, Myers B, et al. Alcohol use in South Africa: Findings from the South African Community Epidemiology Network on Drug Use (SACENDU) project. J Stud Alcohol 2002; 63: 430-435. [ Links ]
33. Seedat S, Nyamai C, Njenga F, Vythilingum B, Stein DJ. Trauma exposure and post-traumatic stress symptoms in urban African schools. Survey in Capetown and Nairobi. Br J Psychiatry 2004; 184: 169-175. [ Links ]
34. Triant VA. The recognition and determinants of depression at a South African primary care clinic. PhD dissertation, Yale University School of Medicine, 2002. [ Links ]
35. Bhagwanjee A, Parekh A, Paruk Z, Petersen I, Subedar H. Prevalence of minor psychiatric disorders in an adult African rural community in South Africa. Psychol Med 1998; 28: 1137-1147. [ Links ]
36. Cooper PJ, Tomlinson M, Swartz L, Woolgar M, Murray L, Molteno C. Post-partum depression and the mother-infant relationship in a South African peri-urban settlement. Br J Psychiatry 1999; 175: 554-558. [ Links ]
37. Carey PD, Stein DJ, Zungu-Dirwayi N, Seedat S. Trauma and posttraumatic stress disorder in an urban Xhosa primary care population: Prevalence, comorbidity, and service use patterns. J Nerv Ment Dis 2003; 191: 230-236. [ Links ]
Accepted 1 April 2009.
* Corresponding author: A A Herman (allenherman@earthlink.net)














