Servicios Personalizados
Articulo
Indicadores
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares en Google
Similares en Google
Compartir
SAMJ: South African Medical Journal
versión On-line ISSN 2078-5135
versión impresa ISSN 0256-9574
SAMJ, S. Afr. med. j. vol.99 no.5 Pretoria may. 2009
ORIGINAL ARTICLES
STUDENT PAPER
Metabolic syndrome and obesity among workers at Kanye Seventh-day Adventist Hospital, Botswana
Roberto A GarridoI, *; María B SemeraroI; Samuel M TemesgenIII; Marcelo R SimiII
ISeventh-year medical student, River Plate Adventist University, Entre Rios, Argentina
IIMD, PhD, River Plate Adventist University, Entre Rios, Argentina
IIIMD, Kanye Seventh-day Adventist Hospital, Kanye, Botswana
ABSTRACT
INTRODUCTION: Metabolic syndrome and obesity are risk factors for developing type 2 diabetes mellitus and/or cardiovascular disease, especially stroke. There is evidence worldwide of the high prevalence of these pathologies in health care providers.
OBJECTIVES: To determine the frequency of metabolic syndrome, overweight, obesity and risk of developing metabolic syndrome in workers at Kanye Seventh-day Adventist Hospital, Kanye, Botswana.
METHODS: An observational and cross-sectional study. For the detection of metabolic syndrome, the criteria of the Adult Treatment Panel III were used; for obesity, the body mass index of 150 workers was applied. Data were grouped and analysed according to gender, age and type of work.
RESULTS: Thirty-four per cent of the hospital's workers had metabolic syndrome, the same percentage were at high risk of developing metabolic syndrome, 28.7% were obese, and 27.3% were overweight. Female gender was found to be strongly associated with obesity and metabolic syndrome. The age group of 35 - 54 years was most affected.
CONCLUSIONS: There is a high prevalence of obesity and metabolic syndrome among Kanye Seventh-day Adventist Hospital workers. We recommend the implementation of programmes to screen these risk factors by means of routine medical exams and improving the lifestyles of Botswana health care workers. The study findings could be the basis for future research among hospital staff and the general population.
Metabolic syndrome (MS) is a set of disorders including central obesity, raised fasting blood glucose (FBG) levels, elevated serum triglycerides (TG), low high-density lipoprotein (HDL) values and high blood pressure (HBP). Other definitions include impaired plasma insulin regulation and body mass index (BMI) changes.1 Whichever definition is used, the presence of MS is associated with a doubled risk of cardiovascular disease (CVD),2,3 and especially stroke,4 and type 2 diabetes mellitus (DM2).5 The population at large, despite being under-diagnosed,6 is estimated to have a high prevalence of MS, leading to higher morbidity and mortality.
Health care workers have a high prevalence of MS. In South America, about a third of nurses had HBP, and 16.6% were obese,7 while 26% of all health workers had HBP.8 In Europe, there was a high prevalence among doctors of components of MS and a greater risk than the general population of developing any form of CVD.9 In the USA, a large increase in the components that constitute MS was found in doctors, as part of the Physician's Health Study (PHS); of the total of 22 046 doctors, 354 presented with >3 metabolic changes at the beginning of the study, reaching 2 050 at the end of the observation.10 A study of 1 027 health workers found that the prevalence of excess weight and obesity was 17.6% and 14.5% respectively at the start of the investigation. A strong association was established between high BMI and the development of metabolic disorders within the subsequent 10 years of follow-up.11
There is little information on the prevalence of MS and obesity among hospital staff in Africa. We therefore aimed to determine the frequency of MS, excess weight, obesity and the risk of developing MS, and to establish the relationship between MS and age, gender and type of work, and the frequency of the biological changes that comprise MS, among Kanye Seventh-day Adventist Hospital (KSDAH) workers.
Materials and methods
A cross-sectional and descriptive study was conducted between 15 December 2007 and 15 February 2008 among KSDAH workers, in Kanye, Botswana, in the context of a general medical examination proposed by the chief medical officer of the hospital in response to the Wellness Program for Health Workers (WPHW) initiative by the Botswana Ministry of Health.12
Data were collected from all workers who voluntarily attended the medical examination on the designated days; 228 (74%) of a total of 301 workers attended. Participants with incomplete data and/or DM2, and pregnant women, were excluded. As a result, 78 (34.2%) were excluded – 66 for incomplete data, 10 for DM2, and 2 pregnant women. The final study population therefore consisted of 150 (49.8%) of the 301 hospital employees. Student's t-test was applied to the included and excluded groups, and no significant difference for the variables was shown (p>0.05).
Data from all participants who signed the informed consent form were included, comprising sex, age, working place/department, weight, height, abdominal circumference (AC), blood pressure (BP), TG, HDL and FBG values. Those with known HBP according to the Adult Treatment Panel III (ATP III) definition were also included.
BP was measured on the left arm, with a properly calibrated aneroid sphygmomanometer, as described in The Seventh Report of the Joint National Committee on Prevention, Detection, Evaluation and Treatment of High Blood Pressure (JNC 7).13
AC was measured by a flexible, conventional, non-elastic tape measure, midway between the last costal margin and the upper border of the iliac crest, and weight and height were measured to determine the BMI of all participants. To measure HDL and TG values, participants were instructed to fast for 8 hours before attending the KSDAH laboratory, where their blood samples were drawn and then analysed by an ABX PENTRA 400 spectrophotometer. FBG values were obtained by test strip. Participants whose FBG levels were >7 mmol/l repeated the laboratory test on the following day under the same fasting conditions, and the lower value was recorded.
To detect MS, the ATP III definition from the National Cholesterol Education Program (NCEP) was used, according to which 3 or more of the following are sufficient for a diagnosis: FBG >6.1 mmol/l; HDL <1.0 mmol/l in men or <1.3 mmol/l in women; TG >1.7 mmol/l; AC >102 cm in men and 88 cm in women; systolic BP >130 mmHg and/or diastolic >85 mmHg, or a person on antihypertensive treatment.1,2
To detect excessive weight and obesity, the WHO BMI was used: underweight = BMI <18.5; normal = BMI 18.5 - 24.9; overweight = BMI 25 - 29.9; and obese = BMI >30.14
To estimate the risk of developing MS, participants with 2 criteria were considered to be high risk, and those with 1 or no criteria to be low risk.
To establish the relationship between MS and age, participants were grouped into 3 age groups: <35, 35 - 54, and >55 years.
To correlate MS with workplace, participants were divided into 3 groups: (i) office workers (doctors, pharmacy personnel, laboratory staff, administrative staff, accounts, records and secretaries); (ii) nurses and health orderlies; and (iii) industrial workers (cleaners, maintenance staff, drivers, stores staff and kitchen staff).
Ethical approval was obtained from the Bioethical Committee of the River Plate Adventist University and from the Human Research Office of the Ministry of Health, Botswana.
Data were analysed by means of a descriptive technique of frequency and percentage, using measures of dispersion for the numerically continuous variables. The level of association was determined using the chi-square test for categorical variables, with 95% confidence interval (p<0.05). Statistical analysis was done by the Statistical Package for Social Sciences (SPSS) 11.5.
Results
Of the total study population of 150, 44 (29.3%) were men and 106 (70.7%) women; 144 (96%) were black and 6 (4.0%) were white. The average age was 39.2±11.1 years, the youngest 22 and the oldest 65 years of age; 67 (44.7%) were 20 - 34 years of age, 66 (44%) were 35 - 54 years, and 17 (11.3%) were >55 years.
Grouped by type of work, 46 (30.7%) were office workers (group 1), 56 (37.3%) were nurses and health orderlies (group 2), and 48 (32.0%) were industrial workers (group 3).
The average height, weight and BP of participants were 163.8±7.6 cm, 72.1±15.9 kg, and 121±21.1 mmHg systolic and 80.2±14.1 mmHg diastolic, respectively. The average FBG, HDL, TG and AC values were 5.5±0.9 mmol/l, 0.8±0.3 mmol/l, 1.0±0.6 mmol/l, and 87.4±13.7 cm, respectively.
Of the 150 participants, 51 (34.0%) had MS, i.e. more than 3 out-of-range findings, according to this study's definition; another 51 had 2 metabolic disorders, and therefore a high risk of developing MS.
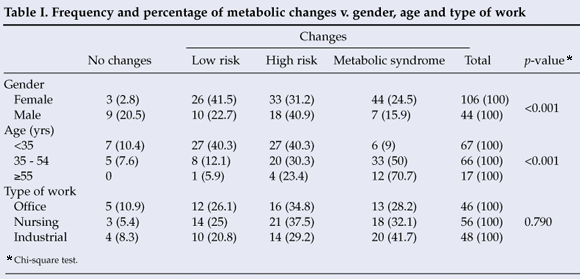
A strong association was observed between female gender and high prevalence of MS, which was present in 44 (24.5%) of all women. Women also comprised the highest percentage (31.2%) at risk of developing MS. A high frequency (50%) of MS was found in the 35 - 54-year-old age group (Table I).
The most prevalent metabolic change observed was low HDL values, present in 120 (80%) participants; 66 (44% of the total) had HBP or were on treatment for HBP; AC was excessive in 63 (42%); FBG values were abnormally high in 40 (26.7%) subjects, and 21 (14%) had raised TG levels.
There was a high association between altered HDL and AC values, and female gender (Table II); however, high plasma TG levels were associated more with men than women (Table II).

Raised BP, TG and AC values were strongly associated with the age group 35 - 54 years, in which raised FBG and HDL values were also prevalent, but these were not statistically significant (Table III).

An association was found between increased AC values among the industrial workers (44.5% of participants with higher values were in this group). However, the nursing staff also had a high frequency of greater AC.
The frequency of obesity was 43 (28.7%), with a BMI of more than 30 kg/m2; 41 participants (27.3%) were overweight with a BMI between 25 and 29.9 kg/m2; only 56 (37.3%) were of normal weight, and 10 (6.7%) were underweight.
The frequency of abnormal AC values was 44.5% among industrial workers and 34.9% among nurses (p=0.011 for different type of work).
There was a high frequency of overweight (23.6%), and even higher for obesity (37.7%, p=0.002 for gender differences), among the women.
Relating age and weight, the 35 - 54-year age group was the most affected, with 30.3% being overweight and 40.9% obese (p<0.001 for gender differences).
There was no significant correlation between type of work and weight of the participants.
Discussion
The high prevalence of MS found in KSDAH workers is difficult to compare with other studies on health personnel because most evaluated only some of the components of MS.7-11 Botswana has no record of the frequency of these pathologies in the general population. However, this prevalence was higher than that among South African executives15 who, despite belonging to a different population group, share some features with health workers. Both groups work indoors throughout the day and are subjected to high levels of work stress. In the hospital group, stress is accentuated by continuous contact with disease and death. In our study area, where there is a high prevalence of HIV/AIDS, health personnel must deal with the constant risk of contracting the virus. Hospital work requires day and night shifts and, together with work stress, could lead to an increased incidence of MS.16,17
The prevalence of overweight and obesity found in this study was higher than that for Taiwanese hospital staff,11 possibly because of racial differences; however, the difference could also be due to regulations for health workers being better applied in developed countries than in developing countries, including mandatory regular physical and biological check-ups. Such policies do not apply to KSDAH because the workers reported that this was the first time that blood-based biochemical studies of this nature had been done on them as part of a routine medical review.
While the female staff of KSDAH were most affected, with more than a third obese, only 5% of women in Taiwan had this pathology; the former tendency could be because of social and cultural characteristics typical of this region of Africa, where substantial body mass in women is associated with higher economic status and a symbol of beauty and health. Furthermore, a slender build is associated with the stigma attached to the HIV/AIDS pandemic, and therefore people are less inclined to lose weight intentionally, so tending to promote obesity among Botswana women.
In this study, the intermediate age group (35 - 54 years) was the most affected, whereas it is the elderly who are usually expected to have a higher prevalence of hypertension, abnormal cholesterol, or being overweight, because age is a non-modifiable risk factor for these conditions. One reason for this finding is that the population of Botswana is changing from its traditional lifestyle to westernised ways and so becoming more subject to similar diseases, the young being more prone in this regard. In contrast, older people, who are less inclined to change their habits, reflected healthier findings. It would be beneficial to identify lifestyle changes among the youth that could determine the increased tendency to develop risk factors for the diseases of developed countries. It would also be interesting to determine to what extent these risk factors are associated with CVD, stroke and/or DM2 among Botswana's population, since most studies have been conducted in Caucasian populations.
Conclusion
This study is the first of its kind in Botswana, comprising a relatively small and specific group of people, and the results may not necessarily be extrapolated to hospital staff throughout the country, let alone to the general population. However, the results show that there is a high risk of lifestyle-associated diseases within a group of people who are responsible for promoting health and healthy values and behaviours among the population. We therefore recommend that the detection of risk factors for CVD among health personnel in Botswana be included as part of a routine medical review. Such interventions would be more expeditious among health personnel who have the advantage of immediate access to medical care. Moreover, if it were possible to perform these routine tests at all health care facilities in the country, the number of participants similar to those in our study would be more representative. Programmes that promote healthy lifestyles among government employees, particularly in the health sector, are also highly desirable.
We acknowledge the support that we received from the Adventist Hospital directorship in Kanye, and especially Dr Rose Llaguno for administrative assistance.
References
1. Lionel H. Metabolic syndrome. Circulation 2007; 115: 32-35. [ Links ]
2. Dekker J, Girman C, Rhodes T, et al. Metabolic syndrome and 10-year cardiovascular disease risk in the Hoorn Study. Circulation 2005; 112: 666-673. [ Links ]
3. Isomaa B, Bouter L, Tiinamaija T, et al. Cardiovascular morbidity and mortality associated with the metabolic syndrome. Diabetes Care 2001; 24: 683-689. [ Links ]
4. Hsin-Jen C, Chyi-Huey B, Wen-Ting Y, Hou-Chang C, Wen-Harn P. Influence of metabolic syndrome and general obesity on the risk of ischemic stroke. Stroke 2006; 37: 1060-1064. [ Links ]
5. Wannamethee S, Shaper A, Lennon L, Morris R. Metabolic syndrome vs Framingham Risk Score for prediction of coronary heart disease, stroke, and type 2 diabetes mellitus. Arch Intern Med 2005; 165: 2644-2650. [ Links ]
6. Mosca L, Linfante A, Benjamin E, et al. National Study of Physician Awareness and Adherence to Cardiovascular Disease Prevention Guidelines. Circulation 2005; 111: 499-510. [ Links ]
7. Leão de Aquino E, Magalhães L, Araújo M, Chagas de Almeida M, Leto J. Hypertension in a female nursing staff – pattern of occurrence, diagnosis, and treatment. Arq Bras Cardiol 2001; 76(3): 203-208. [ Links ]
8. Mion D, Pierin A, Bambirra A, et al. Hypertension in employees of a university general hospital. Rev Hosp Clin Fac Med Sao Paulo 2004; 59(6): 329-336. [ Links ]
9. Nakládalová M, Sovová E, Ivanová K, Kaletová M, Lukl J, Fialová J. Risk factors for cardiovascular diseases in physicians. Biomed Pap Med Fac Univ Palacky Olomouc Czech Repub 2005; 149(2): 293-295. [ Links ]
10. Stürmer T, Buring J, Lee I, Gaziano J, Glynn R. Metabolic abnormalities and risk for colorectal cancer in the Physicians' Health Study. Cancer Epidemiol Biomarkers Prev 2006; 15(12): 2391-2397. [ Links ]
11. Hwang LC, Tsai CH, Chen TH. Overweight and obesity-related metabolic disorders in hospital employees. J Formos Med Assoc 2006; 105(1): 56-63. [ Links ]
12. Republic of Botswana. Ministry of State President National AIDS Coordinating Agency. 2008 Progress Report of the National Response to the UNGASS Declaration of Commitment on HIV/AIDS. Government of Botswana Country Report, United Nations General Assembly Special Session on HIV/AIDS. 22 Dec 2007. [ Links ]
13. National High Blood Pressure Education Program. The Seventh Report of the Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure. Bethesda, MD: National Heart, Lung, and Blood Institute, 2003. [ Links ]
14. James. P, Leach R, Kalamara E, Shayeghi M. The worldwide obesity epidemic. Obes Res 2001; 9 Nov (suppl 4): 228-233. [ Links ]
15. Ker J, Rheeder P, Van Tonder R. Frequency of the metabolic syndrome in screened South African corporate executives. Cardiovasc J S Afr 2007; 18: 30-33. [ Links ]
16. Vitaliano P, Scanlan J, Zhang J, Savage M, Hirsch I, Siegler I. A path model of chronic stress, the metabolic syndrome, and coronary heart disease. Psychosom Med 2002; 64: 418-435. [ Links ]
17. Karlsson B, Knutsson A, Lindahl B. Is there an association between shift work and having a metabolic syndrome? Results from a population based study of 27 485 people. Occup Environ Med 2001; 58: 747-752. [ Links ]
18. Grundy S, Cleeman J, Merz C, et al. Implications of recent clinical trials for the National Cholesterol Education Program Adult Treatment Panel III Guidelines. Circulation 2004; 110: 227-239. [ Links ]
Accepted 11 December 2008.
* Corresponding author: R Garrido (robertito52@yahoo.es)














