Services on Demand
Article
Indicators
Related links
-
 Cited by Google
Cited by Google -
 Similars in Google
Similars in Google
Share
SAMJ: South African Medical Journal
On-line version ISSN 2078-5135
Print version ISSN 0256-9574
SAMJ, S. Afr. med. j. vol.99 n.5 Pretoria May. 2009
ORIGINAL ARTICLES
Clinical and financial burdens of secondary level care in a public sector antiretroviral roll-out setting (G F Jooste Hospital)
Sebastian KevanyI, *; Graeme MeintjesII; Kevin RebeIII; Gary MaartensIV; Susan ClearyV
IMPH, Health Economics Unit, University of Cape Town and Center for AIDS Prevention Studies, University of California, San Francisco
IIMB ChB, MRCP (UK), FCP (SA), DipHIVMan (SA), G F Jooste Hospital, Manenberg, Cape Town and Department of Medicine, University of Cape Town
IIIMB ChB, FCP (SA), DipHIVMan (SA), DTM&H, G F Jooste Hospital, Manenberg, Cape Town and Department of Medicine, University of Cape Town
IVMB ChB, MMed, FCP (SA), DTM&H, Division of Clinical Pharmacology, Department of Medicine, University of Cape Town
VPhD, Health Economics Unit, University of Cape Town
ABSTRACT
BACKGROUND: Antiretroviral therapy (ART) is being extended across South Africa. While efforts have been made to assess the costs of providing ART via accredited service points, little information is available on its downstream costs, particularly in public secondary level hospitals.
OBJECTIVES: To determine the cost of care for inpatients and outpatients at a dedicated antiretroviral referral unit treating and caring for antiretroviral-related conditions in a South African peri-urban setting; to identify key epidemiological cost drivers; and to examine the associated clinical and outcome data.
METHODS: A prospective costing study on 48 outpatients and 25 inpatients was conducted from a health system perspective. Incremental economic costs and clinical data were collected from primary sources at G F Jooste Hospital, Cape Town, over a 1-month period (March 2005).
RESULTS: Incremental cost per outpatient was R1 280, and per inpatient R5 802. Costs were dominated by medical staff costs (62% inpatient and 58% outpatient, respectively). Infections predominated among diagnoses and costs – 55% and 67% respectively for inpatients, and 49% and 54% respectively for outpatients. Most inpatients and outpatients were judged by attending physicians to have improved or stabilised as a result of treatment (52% and 59% respectively).
CONCLUSIONS: The costs of providing secondary level care for patients on or immediately preceding ART initiation can be significant and should be included in the government's strategic planning: (i) so that the service can be expanded to meet current and future needs; and (ii) to avoid crowding out other secondary level health services.
To limit the public health consequences of HIV/AIDS, the South African government implemented a comprehensive treatment programme in April 2004.1 While antiretroviral therapy (ART) dramatically increases life expectancy for infected individuals,2,3 there is often significant morbidity and mortality among patients with advanced HIV infection who start ART, and care is required after treatment has failed.4 Expanding the ART programme requires increased health care system capacity, including that of secondary hospitals, to provide treatment at the appropriate scale and without crowding out other essential health services.
The introduction of ART has resulted in interventions increasingly aimed at aggressively treating opportunistic infections and resuscitating patients with advanced HIV so that they may benefit from longer-term ART. The increased survival time of patients on ART will probably result in higher levels of demand for secondary hospital treatment and increased need for management of antiretroviral (ARV)-related toxicity and immune reconstitution inflammatory syndromes (IRIS). These treatment requirements can be expected to increase in proportion to the level and scale of the national ART roll-out. To ensure that South African secondary level health services are not overburdened in caring for these patients, specific operational and financial provisions need to be made.
Despite these considerations, current operational and financial planning for the ARV roll-out is focused on dedicated ARV clinics, and the cost of secondary level care and referral services is excluded from the Treasury's Conditional Grants for HIV and AIDS.5 In the Western Cape province, while many patients are initiated and managed on ART at the primary level, the development of complications frequently requires referral to secondary hospitals. Secondary facilities therefore also face significant resource demands to investigate and treat patients on or preparing for ART and presenting with opportunistic infections, IRIS, and drug side-effects. This situation is exacerbated by the fact that most patients commencing ART have advanced immunosuppression, with a median CD4 count of 43 cells/µl recorded at ART initiation in Khayelitsha,6 although this level has risen with expanded ART access.7 Opportunistic infections and IRIS are much more likely in such patients.
Background and setting
This study was conducted at G F Jooste Hospital at Manenberg in Cape Town. G F Jooste is a public sector secondary hospital serving the Klipfontein Health District, and is administered by the Provincial Government of the Western Cape. An ARV clinic was established in the hospital in 2003, and secondary level referral services are provided for ARV clinics in its catchment area, namely Mitchell's Plain, Gugulethu, Crossroads, Site B Khayelitsha and Nolungile ART clinics. G F Jooste serves a population of approximately 1.2 million people, including socially and economically disadvantaged communities. The unemployment rate in the Khayelitsha and Mitchell's Plain areas has been estimated as 46.3%.8 The antenatal HIV prevalence in communities served by G F Jooste is up to 33% (Provincial Administration of the Western Cape, personal communication, 2005) and access to private health care is limited.
G F Jooste ARV referral unit
The G F Jooste ARV Referral Unit (ARU) was established in August 2004 in response to a high level of casualty admissions for patients on ART. It was designed to relieve demand on the hospital's emergency department and as a referral service for complex cases, so that primary care clinics could focus on initiating large numbers of patients on ART. Significant and sustained levels of demand for this service prompted the unit's expansion into an independent clinical service, providing specialist-directed investigation and treatment. During the study, the ARU was staffed by 2 infectious disease (ID) specialists (part-time), 2 medical officers, 1 registered nurse (providing outpatient care only), and an admissions clerk.
The ARU provides comprehensive outpatient care and inpatient consultation services to hospital patients in the medical wards. Any patient on ART developing clinical complications or any patient preparing for ART initiation may be referred. Outpatient consultations in the hospital's outpatient department require the ad hoc use of examination rooms in the absence of designated facilities. Inpatient consultation is provided to patients in the medical wards, whose day-to-day care remains the responsibility of Medicine Department staff. Approximately 40% of ARU patients referred to the outpatient service require admission for inpatient care (unpublished audit).
ARU patients are referred from the G F Jooste ARV Clinic and the 5 local primary ART clinics for assessment and management. Potential referrals are initially discussed telephonically. Patients are triaged to: (i) immediate inpatient admission through the casualty department; (ii) an outpatient appointment at the ARU (generally within 48 hours); or (iii) continued primary care with specialist telephonic assistance. Outpatients are evaluated by the attending ARU clinician(s), and an investigation and management plan is developed, with the outcome being admission, follow-up at the ARU, or referral back to primary care.
Methods
Data were collected on all new and existing patients treated by the ARU from 1 to 31 March 2005. Information on inpatient length of stay after termination of the study period was collected during April and May 2005. All ARU patients had to be resident in the hospital catchment area, HIV-infected, >13 years of age, attending a designated ART clinic, and on or preparing for ART.
Incremental economic costs were assessed from a health systems perspective since the choice of costing perspective needs to be appropriate to the study question. Only costs incurred by the service provider or the State, and donated items that could fall within the provider's budget in the future or in other settings, were included. While the alternative societal or patient perspectives elucidate a wider range of productivity, time, and indirect costs,9 these were excluded as they were not directly applicable to the study question. Incremental costs include patient-specific and medical staff costs, but exclude capital and overheads which have previously been assessed for G F Jooste.10
Clinical, resource use and treatment data were collected daily from ARU staff, with separate data capture forms for inpatients and outpatients. Patient-specific resource requirements were recorded and classified according to: (i) laboratory testing; (ii) imaging and radiology; (iii) medical and surgical procedures; (iv) medication; (v) intravenous fluids; (vi) medical consumables; and (vii) counselling services. A self-administered data capture form determined the level and distribution of clinical staff time. Clinical, investigation and treatment data were gathered according to a set of broad categories. Response to treatment was determined by the attending physician.
Laboratory costs were sourced from the hospital laboratory and National Health Laboratory Services (NHLS) estimates;11 pharmaceutical and intravenous fluid costs from the hospital pharmacy and the 2004 Community Health Services Organisation Drug Price Listings;12 the donated drug fluconazole cost was provided by the drug manufacturer; and imaging, radiology, medical and surgical procedure costs from the 2005 South African Uniform Patient Fee Schedule13 and from the hospital's finance department. All procedures unavailable at G F Jooste Hospital and conducted at Groote Schuur tertiary hospital were included. Medical and non-medical consumable costs were sourced from the hospital supplies department. Counselling costs were provided by the Lifeline HIV Counselling Service, which manages G F Jooste counsellors. Other medical staff costs were provided by the hospital finance department, including benefits, scarce skills bonuses, commuted overtime, pension fund and medical aid contributions. All costs are presented in South African rands at 2005 rates.
A bottom-up, micro-costing procedure was employed for all patient-specific costs.14 Total costs across each costing category were assessed for each outpatient visit and inpatient admission. Average patient-specific costs per outpatient visit and per inpatient day were calculated by dividing costs by total outpatient visits and inpatient days, respectively. Total monthly clinical personnel costs were calculated by combining data on clinical staff time distribution with associated monthly salary figures. The allocation of shared personnel costs was based on accepted economic evaluation allocation procedures.15 Monthly medical staff costs were then divided by total outpatient visits and inpatient days to determine total cost per outpatient visit and per inpatient day. Patient-specific costs (including imaging, laboratory testing, medication, procedures and counselling costs) were linked to diagnoses on a patient-by-patient basis during the data collection process. Data sorting, cleaning and analysis were performed using EXCEL Version 9.0 (Seattle, Washington: 2000).
Results
Information on 48 new or existing outpatients and 25 new or existing inpatients (approximately 3.3% of those currently on ART in the referral area – information from provincial HIV directorate) was collected. A total of 63 outpatient visits and 240 inpatient days were recorded. Inpatients were followed up until final date of discharge (Table I). A high proportion were female and between 20 and 30 years of age; mean age was 36 years for outpatients at date of visit, and 34 years for inpatients at date of admission; 21 (44%) of 48 outpatients were diagnosed as WHO HIV clinical stage 4, and 9 (19%) presented with a CD4 count <50 cells/µl; the mean outpatient CD4 count was 175 cells/µl; 22 (88%) of 25 inpatients were diagnosed as clinical stage 4, and 52% presented with a CD4 count <50 cells/µl; the mean inpatient CD4 count was 78 cells/µl.
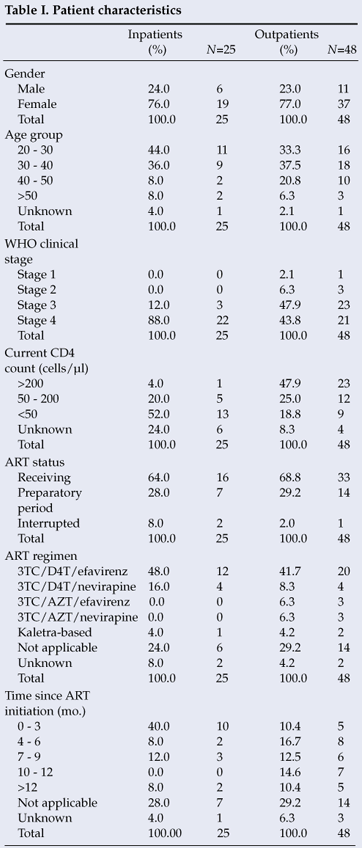
Of the outpatients, 33 (69%) were receiving ART and 14 (29%) were preparing for ART initiation. Among those on ART, the median time from initiation was 8 months. For inpatients, 16 (64%) were receiving ART and 7 (28%) were preparing for treatment initiation. Among those on ART, the median time from initiation was 2 months. One outpatient and 2 inpatients had interrupted ART treatment.
The mean length of inpatient stay was 14.6 days (this figure includes all inpatient days accrued in advance and after termination of the study period (365 inpatient days)). Average inpatient length of stay during the 1-month study period was 9.6 days (240 days); 7 inpatients (28%) were hospitalised for 7 days or less, 14 (56%) were admitted for 7 - 21 days, and a further 4 patients (16%) for >3 weeks. The average outpatient length of visit was 47 minutes.
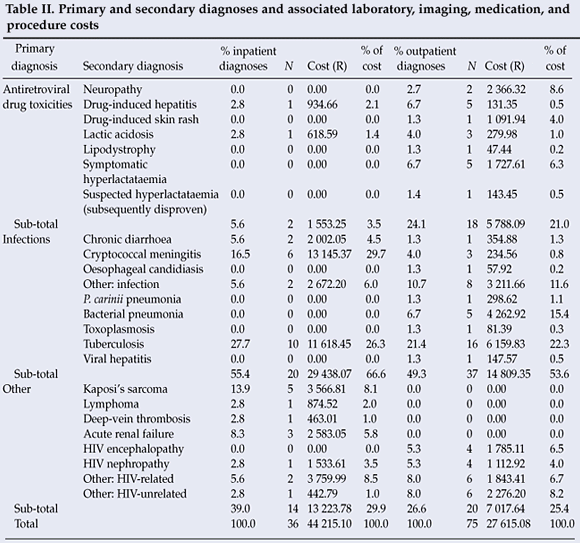
Patients frequently presented with multiple diagnoses, and a total of 75 outpatient diagnoses and 36 inpatient diagnoses were recorded; infections dominated (55% inpatient, 49% outpatient), tuberculosis being a high proportion of inpatient and outpatient infection diagnoses. ARV drug toxicities were infrequent in inpatients (2 diagnoses, or 6% of all inpatient diagnoses) compared with outpatients (18 diagnoses or 24%) (Table II).
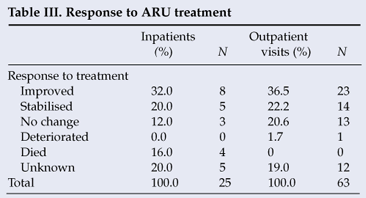
Outpatient outcomes were based on the results of each outpatient visit, rather than individual patients. A high proportion of inpatients and outpatients either improved with treatment or were stabilised (Table III).
Inpatient-specific and outpatient-specific costs were dominated by infections (67%; 54%). For inpatients, 30% of costs were related to the treatment of cryptococcal meningitis and 26% to tuberculosis treatment. For outpatients, 22% of costs were related to the treatment of tuberculosis, and 15% to bacterial pneumonia (Table II).
Patient-specific costs for inpatients and outpatients were dominated by laboratory tests, medical and surgical procedures, and imaging and radiology costs. Medication costs were a low proportion of total patient-specific costs, as most patients were supplied with ART by their primary care clinics (Table IV).
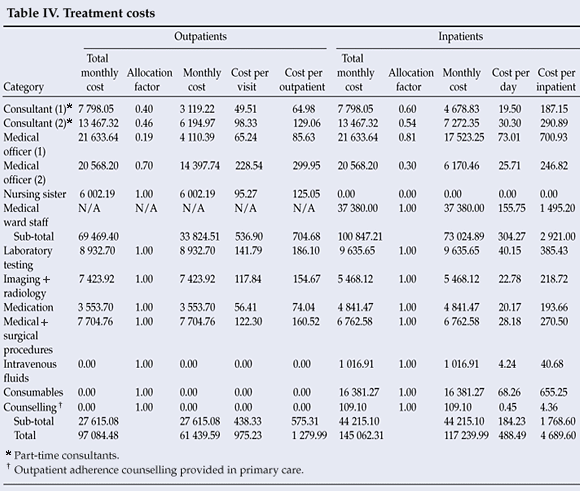
Laboratory testing costs were dominated by blood tests. Imaging and radiology costs were primarily accrued by CT scanning. Medication costs were dominated by non-ARV antimicrobials and ARV drugs. Medical and surgical procedure costs were dominated by ambulatory rather than theatre-based procedures, particularly lumbar punctures and upper gastro-intestinal endoscopies.
Medical staff costs accounted for the highest proportion of total inpatient and outpatient costs, dominated by clinician costs, with medical officer costs accounting for a high level of outpatient staff costs (55%).
Costs per outpatient visit and per inpatient day are presented in Table IV. The total costs of inpatient care (R145 062) were 49% higher than total outpatient costs (R97 084), and the cost of care per inpatient (R5 802) was approximately 4.5 times higher than the cost per outpatient (R1 280).
Discussion
Most patients presented with an opportunistic infection, reflecting the initiation of ART with low CD4 counts in our population and suggesting the need for further research into their expedited primary-level diagnosis. In particular, interventions that expedite the diagnosis and treatment of tuberculosis at the primary level may reduce associated morbidity and secondary level referral.
As the lamivudine (3TC), D4T and efavirenz/nevirapine regimen is the national treatment programme standardised first-line ART regimen, no relationship between specific drug use and the need for secondary level treatment can be inferred. Eighteen outpatient diagnoses (24%) and 2 inpatient diagnoses (6%) were related to ARV toxicities.
ARU patient outcomes showed reasonable improvement (31 patients) or stabilisation (19 patients) because of investigations and treatment. The proportions of patients improving and stabilising were similar for inpatients and outpatients. Further research into the morbidity of patients commencing ART is required, to assist in planning and developing appropriate interventions. The increased costs of interventions for the earlier detection of HIV/AIDS may be offset by savings in secondary level treatment and care. The earlier patients are diagnosed, enrolled in HIV care and initiated on ART when indicated, the less likely are complications by opportunistic infections.
The mean length of stay for inpatients is higher than prior findings for HIV-positive patients at G F Jooste Hospital.16 Because of improved ART availability, physicians may be less inclined than previously to send patients for palliative care. Average outpatient visit duration was higher than average primary-level consultation times for both ART and non-ART patients10 but was still <1 hour.
Treatment costs were dominated by medical staff costs, accounting for 58% of outpatient and 62% of inpatient costs, which supports the investment in medical staff. Vertical health system interventions, including the ARV roll-out, may frequently concentrate resources on the provision of short-term consumable items. Parallel and complementary investment in infrastructure and clinical personnel is also necessary.
The high proportion of inpatient and outpatient costs as a result of infections suggests that the treatment of infections is critical in secondary level care for ART patients, especially for tuberculosis, cryptococcal meningitis and bacterial pneumonia. Treatment of infections remains one of the most costly and complex aspects of HIV care.
The mean CD4 count for outpatients was higher than for inpatients, and there were also lower total and per-patient costs of care per outpatient than per inpatient. This finding illustrates the importance of earlier diagnosis and initiation onto ART to avert these high inpatient costs. The difference in total costs between outpatients and inpatients suggests that earlier referral and easier access to referral services for ART patients should be provided, rather than allowing patients to become so ill that they require inpatient care.
Limitations
Cost analyses are required over a significant time period for meaningful results, and have been described as 'complex, difficult and time-consuming to perform'.17 In costing a pilot project, costs must be determined without the assistance of a costing template or associated studies. Limitations on the availability of appropriate datasets can diminish the accuracy of cost analysis results. All key primary datasets for this research were sourced directly from G F Jooste Hospital.
Conclusion
Our study of the costs of secondary level treatment for patients on or preparing for ART provides policymakers, planners and health system administrators with information on the potential hidden impact of ARV treatment. While a dedicated ARU is one model for meeting the secondary level needs of these patients, and other models may be more integrated within existing services, many clinical and financial needs may be similar. It is essential to include these costs in the government's strategic planning for HIV treatment and Treasury budgets, to ensure adequate quality of care. Costing data are critical to the resource allocation process;18 however, limited information is available on public sector expenditure required to meet the needs of HIV-infected patients across the continuum of care.19
This study neither undermines nor questions the affordability and viability of the ARV roll-out but complements studies on the costs of scaling up ART in South Africa.4,5,20 The results expedite research into technical and allocative efficiency in the South African health system and may be used by secondary hospitals to assess the resources required for these treatments. While local considerations may require variations on the G F Jooste model, this evaluation may assist in the delivery of specialised secondary care. Estimates of secondary level treatment costs may be useful in assessing the macro-economic effects of HIV/AIDS in South Africa.
The successful implementation of the ARV treatment programme depends on a strengthened health system.21 In assessing the viability of specific health interventions, policymakers must consider their impact at all levels of the health system. The load on secondary level HIV referral services will inevitably increase as the ART roll-out expands, as evidenced by the same ARU at G F Jooste which had approximately 250 outpatient visits per month during 2007 (unpublished data). Costs of care are significantly higher for patients on ART in South Africa.22 The development of ARUs, specifically to assess and treat patients on or preparing for ART, and the expansion of associated secondary hospital services, should be considered in planning the national ARV roll-out. Only through the comprehensive assessment of resource requirements across the health system can vertical interventions be fully audited, and scarce resources be distributed appropriately.
We thank Nontobeko Dyakopu, Jane Kawadza, Cordelia Faleni and David Stead for their assistance with data collection.
References
1. Department of Health. National Antiretroviral Treatment Guidelines. Pretoria: Department of Health, 2004. [ Links ]
2. Forsythe S, Gilks C. Economic Issues and Antiretroviral Therapy in Developing Countries. Trans R Soc Trop Med Hyg 1999; 93(1): 1-3. [ Links ]
3. Casseb J, Fonseca LA, Veiga AP, et al. AIDS Incidence and mortality in a hospital-based cohort of HIV-1-seropositive patients receiving highly active antiretroviral therapy in Sao Paulo, Brazil. AIDS Patient Care STDS 2003; 17(9): 447-452. [ Links ]
4. Arens FJ, Maartens G. Treatment Costs for HIV/AIDS in a Managed Care Setting in South Africa. Presentation to the 38th Annual Congress of the South African Pharmacology Society, Bloemfontein, 24 - 27 October 2004. [ Links ]
5. Cleary S, Blecher M, Boulle A, et al. The costs of the National Strategic Plan on HIV and AIDS & STIs 2007-2011. http://www.tac.org.za/documents/NSPCostingFinal.doc (accessed 1 June 2007). [ Links ]
6. Coetzee D, Hildebrand K, Boulle A, et al. Outcomes after two years of providing antiretroviral treatment in Khayelitsha, South Africa. AIDS 2004; 18: 887-895. [ Links ]
7. Boulle A. Antiretroviral Therapy and Early Mortality in South Africa. Bull World Health Organ 2008; 86 (8). [ Links ]
8. Nattrass N, Leibbrant M, Seekings J, et al. Khayelitsha/Mitchell's Plain Survey 2000: Survey Report and Baseline Information. Cape Town: Centre for Social Science Research, University of Cape Town and the Population Studies Center, University of Michigan, 2003. [ Links ]
9. Drummond M, McGuire A, eds. Economic Evaluation in Health Care: Merging Theory with Practice. Oxford: Oxford University Press, 2001. [ Links ]
10. Cleary S, McIntyre D, Boulle A. The cost-effectiveness of antiretroviral treatment in Khayelitsha, South Africa: a primary data analysis. Cost-Effectiveness and Resource Allocation 2006; 4: 20. [ Links ]
11. National Health Laboratory Service. Laboratory Costs Estimates. Johannesburg: National Health Laboratory Service, 2004. http://www.nhls.ac.za (accessed 1 June 2005). [ Links ]
12. Community Health Services Organisation (2004) Community Health Services Organisation Drug Price Listings. Cape Town: Community Health Services Organisation, 2004. [ Links ]
13. Department of Health. Uniform Fee Payment Schedule. Pretoria: Department of Health, 2005. [ Links ]
14. Shepard S. Analysis of Hospital Costs: A Manual for Managers. Geneva: World Health Organization, 2000. [ Links ]
15. Creese A, Parker D. Cost Analysis in Primary Health Care: A Training Manual for Programme Managers. Geneva: World Health Organization, 1994. [ Links ]
16. Haile B. Costs of Adult Inpatient Care for HIV Disease at GF Jooste Hospital. MPH thesis, University of Cape Town, 2000. [ Links ]
17. Beck EJ, Miners AH, Tolley K. The cost of HIV treatment and care: A global review. Pharmacoeconomics 2001; 19(1): 13-39. [ Links ]
18. Beck EJ, Santas XM, DeLay PR. Why and how to monitor the cost and evaluate the cost-effectiveness of HIV services in countries. AIDS 2008; 22 suppl 1: S75-S85. [ Links ]
19. Walker D. Cost and cost-effectiveness of HIV/AIDS prevention strategies in developing countries: Is there an evidence base? Health Policy and Planning 2003; 18 (1): 4-17. [ Links ]
20. Cleary S, Boulle A, Castillo-Riquelme M, et al. The burden of HIV/AIDS in the public health system. S Afr J Economics 2008; 76 suppl 1: S3-S14. [ Links ]
21. Guthrie T, Hickey A. Funding the Fight: Budgeting for HIV/AIDS in Developing Countries. Cape Town: IDASA, 2004. [ Links ]
22. Thomas LS, Manning A, Holmes CB, et al. Comparative costs of inpatient care for HIV-infected and uninfected children and adults in Soweto, South Africa. J AIDS 2007; 46(4): 410-415. [ Links ]
Accepted 22 December 2008.
* Corresponding author: Sebastian Kevany (sebastian.kevany@ucsf.edu)














