Services on Demand
Article
Indicators
Related links
-
 Cited by Google
Cited by Google -
 Similars in Google
Similars in Google
Share
SAMJ: South African Medical Journal
On-line version ISSN 2078-5135
Print version ISSN 0256-9574
SAMJ, S. Afr. med. j. vol.99 n.5 Pretoria May. 2009
SCIENTIFIC LETTERS
Management of cryptoccocal meningitis in resource-limited settings: a systematic review
Derek SloanI; Sipho DlaminiII; Martin DedicoatIII, *
IMRCP, Department of Infectious Diseases, University of Liverpool, Liverpool, UK
IIMB ChB, Department of Internal Medicine, University of Cape Town
IIIPhD, Department of Internal Medicine, Polokwane Mankweng Hospital Complex, University of Limpopo, Polokwane
To the Editor: Cryptococcal meningitis (CM) remains a serious cause of mortality and morbidity in individuals infected with the human immunodeficiency virus (HIV). The optimal treatment of CM is unknown. We conducted a systematic review to determine the best treatment for CM with an emphasis on resource-poor settings. Six studies met the inclusion criteria; none was found that compared amphotericin B with fluconazole. From the available evidence, it is not possible to determine which treatment is superior for CM.
Background
Despite the increasingly wide availability of antiretroviral therapy (ART), CM remains a significant cause of mortality and morbidity among HIV-infected individuals; untreated, its outcome is universally fatal.1 In South Africa, despite the availability in the public sector of antifungal therapy (fluconazole (FLU) and amphotericin B (AmB)) for treating CM, inpatient mortality is around 25%.2 The ideal management of CM remains unclear. Many patients with HIV infection who present for the first time to health services with a major opportunistic infection such as CM are unaware of their status. We aimed to assess the evidence for which antifungal regimen and other management to use, emphasising resource-poor settings, for treating CM in HIV-infected individuals to enable them to survive and benefit from ART.
Methods
Relevant studies were identified using the Cochrane HIV/AIDS group search strategy from databases from January 1980 to June 2008. Key search words included meningitis, Cryptococcus neoformans, treatment, trial, human immunodeficiency virus, acquired immunodeficiency syndrome, antifungal agents, AmB, flucytosine (FLC), FLU, azole, lumbar puncture, cerebrospinal fluid (CSF) pressure and acetazolamide. Trials deemed suitable were randomised trials of HIV-infected adults with a first episode of CM diagnosed on CSF examination, by India ink staining, CSF culture or cryptococcal antigen testing. The authors extracted data using standardised forms and performed analysis using Rev Man 4.2.7 software.
Results
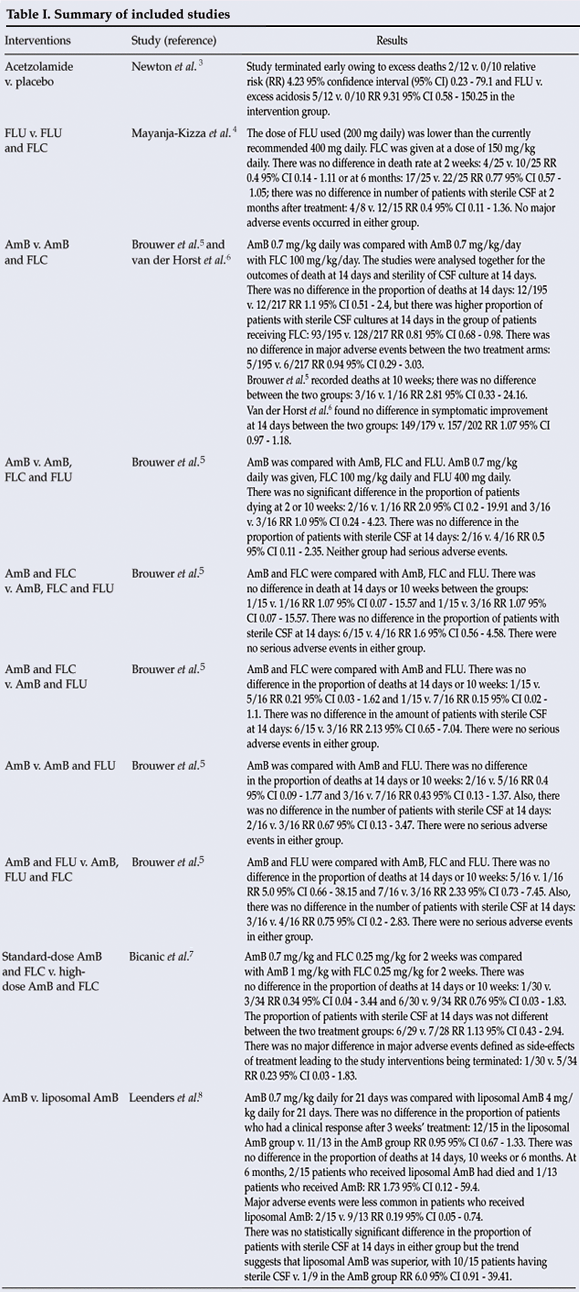
Six studies are included in the review;3-8 5 compared antifungal treatments.4-8 One study that addressed lowering intracranial pressure using oral acetazolamide to lower intracranial pressures was stopped early because of excessive metabolic acidosis3 (Table I). No study demonstrated differences in survival between groups.
Conclusions
We aimed to determine the best treatment for CM in resource-limited settings in which only AmB and FLU were usually available. No suitable studies comparing these two drugs were found; therefore, we cannot recommend either treatment as superior to the other. Although AmB-containing regimens have caused more rapid sterilisation of CSF compared with FLU,9 we found no evidence of improved survival. The optimal dosing and duration of AmB remains unclear; the Southern African HIV Clinicans Society recommended dose is 1 mg/kg daily for 14 days, followed by FLU 400 mg daily for 8 weeks, then FLU 200 mg daily for life; if AmB is not available or its use is contraindicated, then FLU should be used as first-line treatment.10
Liposomal AmB is associated with less adverse events than AmB and may be useful in selected patients where resources allow.
FLC (not available in South Africa) in combination with AmB leads to faster and increased sterilisation of CSF compared with using AmB alone. This finding does not correlate with improved clinical outcomes. Infectious Diseases Society of America guidelines recommend that AmB be given in combination with FLC.11
Future research into the management of CM in resource-limited settings should focus on the most effective use of medications available in these settings as well as other management modalities such as control of intracranial pressure. The other major issue is the optimal timing of initiation of ART either during or after initial treatment of CM, with the aim of maximising early immunological benefit and reducing the incidence of immune reconstitution-related complications.
A full version of this review is available in the Cochrane database.12
References
1. Mwaba P, Mwansa J, Chintu C, et al. Postgrad Med J 2001; 77: 769-773. [ Links ]
2. Schaars CF, Meintjes GA, Morroni C, Post FA, Maartens G. Outcome of AIDS-associated cryptococcal meningitis initially treated with 200 mg/day or 400 mg/day of fluconazole. BMC Infect Dis 2006; 6: 118. [ Links ]
3. Newton PN, Thai le H, Tip NQ, et al. A randomized, double-blind, placebo-controlled trial of acetazolamide for the treatment of elevated intracranial pressure in cryptococcal meningitis. Clin Infect Dis 2002; 35: 769-772. [ Links ]
4. Mayanja-Kizza H, Oishi K, Mitarai S, et al. Combination therapy with fluconazole and flucytosine for cryptococcal meningitis in Ugandan patients with AIDS. Clin Infect Dis 1998; 26: 1362-1366. [ Links ]
5. Brouwer AE, Rajanuwong A, Chierakul W, et al. Combination antifungal therapies for HIV-associated cryptococcal meningitis: a randomised trial. Lancet 2004; 363: 1764-1767. [ Links ]
6. van der Horst CM, Saag MS, Cloud GA, et al. Treatment of cryptococcal meningitis associated with the acquired immunodeficiency syndrome. National Institute of Allergy and Infectious Diseases Mycoses Study Group and AIDS Clinical Trials Group. New Engl J Med 1997; 337: 15-21. [ Links ]
7. Bicanic T, Wood R, Meintjes G, et al. High-dose amphotericin B with flucytosine for the treatment of cryptococcal meningitis in HIV-infected patients: a randomized trial. Clin Infect Dis 2008; 47: 123-130. [ Links ]
8. Leenders AC, Reiss P, Portegies P, et al. Liposomal amphotericin B (AmBisome) compared with amphotericin B both followed by oral fluconazole in the treatment of AIDS-associated cryptococcal meningitis. AIDS 1997; 11: 1463-1471. [ Links ]
9. Bicanic T, Meintjes G, Wood R, et al. Fungal burden, early fungicidal activity and outcome in cryptococcal meningitis in antiretroviral-naïve or antretroviral experienced patients treated with amphoteracin B or fluconazole. Clin Infect Dis 2007; 45: 76-80. [ Links ]
10. McCarthy K, Meintjes G. Guidelines for the Prevention, Diagnosis and Management of Cryptococcal Meningitis and Disseminated Cryptococcosis in HIV Infected Patients. Southern African Journal of HIV Medicine 2007; Spring: 25-35. [ Links ]
11. Saag MS, Graybill RJ, Larsen RA, et al. for the mycoses study group cryptococcal subproject. Practice guidelines for the management of cryptococcal disease. Clin Infect Dis 2000; 30: 710-718. [ Links ]
12. Sloan D, Dlamini S, Paul N, Dedicoat M. Treatment of acute cryptococcal meningitis in HIV infected adults, with an emphasis on resource-limited settings. Cochrane Data Base Systematic Review 2008; CD005647 [ Links ]
Accepted 17 December 2008.
* Corresponding author: M Dedicoat (mdedicoat@doctors.org.uk)














