Services on Demand
Article
Indicators
Related links
-
 Cited by Google
Cited by Google -
 Similars in Google
Similars in Google
Share
SAMJ: South African Medical Journal
On-line version ISSN 2078-5135
Print version ISSN 0256-9574
SAMJ, S. Afr. med. j. vol.99 n.4 Pretoria Apr. 2009
SCIENTIFIC LETTERS
Management of anterior vaginal prolapse in South Africa: national survey
E W HennI; J A van RensburgII; H S CronjeIII
IMB ChB, MMed (O et G), FCOG (SA). Department of Obstetrics and Gynaecology, University of the Free State, Bloemfontein
IIMMed (O et G), FCOG (SA), MD. Department of Obstetrics and Gynaecology, University of the Free State, Bloemfontein
IIIMB ChB, MMed (O et G), FCOG (SA). Department of Obstetrics and Gynaecology, Stellenbosch University, Tygerberg, W Cape
To the Editor: A national survey was done on the management of anterior vaginal prolapse (AVP) by registered gynaecologists and urologists in South Africa. Of 822 questionnaires posted, 30.2% were returned completed (23.2% from gynaecologists and 7.0% from urologists). The information supplied was anonymous and is probably a true reflection of current practice. Of concern were the 36.3% of respondents who did not use a recognised staging system, a low rate of pre-operative urodynamic investigation by gynaecologists (8.4%) and a high rate of synthetic mesh use by urologists (75.9%), even for primary procedures.
This first survey among South African prolapse surgeons provides valuable insight into clinical practice.
Background
Among parous women, the prevalence of pelvic organ prolapse (POP) is 50%, increasing with advancing age. The lifetime risk of surgery for urinary incontinence or POP has been estimated at approximately 11%, with 30% needing a second operation within 2 years.1 AVP is the most common type of POP and can significantly impact on a woman's quality of life.
The International Continence Society standardised the terminology for prolapse grading and recommended the term 'anterior vaginal prolapse' for what was traditionally known as 'cystocele'. Most women who have AVP are asymptomatic. Symptoms only tend to arise once the leading part of the prolapse extends past the hymenal ring. The main problem surrounding AVP is a high failure rate for surgery, so there is controversy regarding the best method of treatment. A wide variation of 20 - 70% for recurring prolapse following traditional surgery has been reported. The use of synthetic mesh in this surgery may be associated with complications, but the incidence of recurring prolapse at approximately 1 year's follow-up seems to be lower, usually below 20%. Since there is no generally agreed upon standard method for the surgical correction of AVP, we surveyed the methods used in evaluating and treating this form of prolapse in South Africa.
Materials and methods
The survey was aimed at gynaecologists and urologists. A 25-question questionnaire was developed that dealt with clinical assessment, conservative therapy, type of anaesthetic, surgical technique and preferences, surgery for stress urinary incontinence, postoperative management and demographic information. A total of 822 questionnaires were mailed once only to 659 gynaecologists and 163 urologists in South Africa along with a stamped return envelope. The respondents remained anonymous. Results were summarised using frequencies and percentages. Responses by urologists and gynaecologists were compared using chi-square tests and 95% confidence intervals for differences in percentages.
Results
Of the questionnaires 30.2% were completed and returned to us, 180 (23.2%) by gynaecologists and 54 (7.0%) by urologists. Most respondents were from the private sector - 77% of gynaecologists and 83% of urologists. A minority of the respondents had a special interest in urogynaecology (19% of gynaecologists and 22% of urologists). More than 60% had been practising as specialists for 10 years or more.
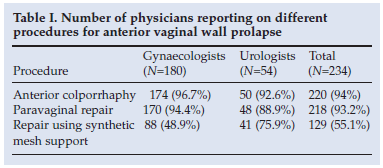
The POP-Q system was the dominant grading system for prolapse (37.6%), followed by the Baden-Walker system (12.0%); 36.3% of the respondents did not use any recognised system. Urodynamic investigation was performed preoperatively by 8.4% of the gynaecologists and 20.8% of the urologists (p=0.0121). Imaging procedures were used as part of the preoperative assessment by 27.8% of the respondents, ultrasound (gynaecologists) and voiding cysto-urethrograms (urologists) being the most common. Vaginal pessaries were used at times by 50.6% of the gynaecologists and by only 16.1% of the urologists (p<0.0001). Pelvic floor exercises were prescribed pre-operatively by 68.4% of the respondents and postoperatively by 53.9%. More gynaecologists made use of these exercises. Anterior fascial repair was the most commonly performed surgical procedure for AVP (Table I), with a comparable frequency for gynaecologists and urologists. This was followed by paravaginal repair and lastly use of synthetic mesh for correcting the defects. Synthetic mesh was used more often by urologists (p=0.0001). During anterior colporraphy, gynaecologists exclusively used the Kelly suture (54%). Where synthetic mesh was used, the Prolift system (Johnson & Johnson) was the most frequently used, particularly by urologists (45.5% v. 68.9%, p=0.0081). The most common additional procedures done at the time of anterior repair were vaginal hysterectomy and/or posterior repair for gynaecologists (75.7%) and an anti-incontinence sling procedure and/or posterior repair for urologists (95.6%). Most respondents performed surgery for the correction of stress urinary incontinence (SUI) concomitant with AVP repair (83.3% of gynaecologists and 66.7% of urologists, p=0.0129). The transobturator sling approach was mostly used by gynaecologists (55.5% v. 29.2%, p=0.0018) and the retropubic sling by urologists (45.8% v. 29.3%, p=0.0403).
Discussion
Only 30% of the questionnaires were returned in our survey, but the disciplines were approximately evenly represented with regard to the percentage of responses. The reason for the low response rate is unclear. The returned completed questionnaires were representative of all the provinces in South Africa and are therefore a probable reflection of AVP management in South Africa.
There was considerable variation in the evaluation of patients with AVP. The POP-Q system is currently the internationally recognised standard for evaluating prolapse. It was surprising to note that more than a third of the respondents were not using any recognised classification system.
Conservative treatment, most commonly pelvic floor exercises and use of vaginal pessaries, is generally considered for women with a mild degree of prolapse, those wishing to have more children, frail patients or those who are unwilling to undergo surgery. Pelvic floor exercises, although effective for SUI, have not been shown to be effective in reducing AVP. Most respondents favoured pelvic floor exercises as part of preoperative management, which is sensible as it may improve the quality of life for these women. Most respondents would not normally make use of pessaries, especially urologists, of whom more than 80% reported never using them. This may reflect the fact that many clinicians receive little or no training in the use of pessaries.
The best choice of surgical treatment for AVP remains controversial. Current level I evidence suggests that the optimal procedure for anterior vaginal repair is abdominal sacrocolpopexy combined with a Burch colposuspension and paravaginal repair. This combination is superior to anterior colporrhaphy or sacrospinous colpofixation with or without vaginal paravaginal repair. Anterior colporrhaphy is currently the surgical procedure of choice among the majority of respondents. This finding is similar to a recent UK survey in which 77% of respondents also favoured anterior colporrhaphy.2
The use of synthetic mesh in the anterior compartment is still controversial and clear indications and evidence of longterm efficacy are lacking. In this survey, most respondents in both disciplines would rarely use synthetic mesh in a primary anterior vaginal wall repair. All practising gynaecologists and urologists know that AVP often coexists with prolapse in the apical and/or posterior vaginal compartments. It is therefore not unusual to combine anterior repair with another procedure, as confirmed in our survey. Procedures most often performed in combination with an anterior repair were vaginal hysterectomy and posterior repair. Correcting concomitant SUI at the time of anterior vaginal surgery might offer a superior anatomical outcome compared with anterior colporrhaphy alone.3 Our survey showed a minor difference regarding choice of continence procedure; most gynaecologists preferred the transobturator sling, whereas most urologists preferred the retropubic sling, for reasons that are not clear.
References
1. Olsen AL, Smith VJ, Bergstrom VO, Colling JC, Clark AL. Epidemiology of surgically managed pelvic organ prolapse and urinary incontinence. Obstet Gynecol 1997; 89: 501-506. [ Links ]
2. Jha S, Moran PA. National survey on the management of prolapse in the UK. Neurourol Urodyn 2007; 26: 325-331. [ Links ]
3. Meschia M, Pifarotti P, Spennacchio M, Buonaquidi A, Gattei U, Somigliana E. A randomized comparison of tension-free vaginal tape and endopelvic fascia plication in women with genital prolapse and occult stress urinary incontinence. Am J Obstet Gynecol 2004; 190: 609-613. [ Links ]
Accepted 8 January 2009.
Corresponding author: E W Henn (hennew.md@ufs.ac.za)














