Serviços Personalizados
Artigo
Indicadores
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares em Google
Similares em Google
Compartilhar
SAMJ: South African Medical Journal
versão On-line ISSN 2078-5135
versão impressa ISSN 0256-9574
SAMJ, S. Afr. med. j. vol.99 no.3 Pretoria Mar. 2009
ORIGINAL ARTICLES
Child's play: exposure to household pesticide use among children in rural, urban and informal areas of South Africa
Sandy TolosanaI; Hanna-Andrea RotherII; Leslie LondonIII
IBA, BA (Hons), MSc, DOH. Asbestos Relief Trust, UCT Boehringer Ingelheim Lung Institute, Observatory, Cape Town
IIBA, MA, PhD. Occupational and Environmental Health Research Unit, School of Public Health and Family Medicine, University of Cape Town
IIIMB ChB, BSc (Hons), DOH, MD, MMed. Occupational and Environmental Health Research Unit, School of Public Health and Family Medicine, University of Cape Town
ABSTRACT
BACKGROUND: As part of a larger dermatological investigation undertaken in 1999 - 2001 involving the Department of Dermatology, Groote Schuur Hospital (Cape Town, South Africa) and Nottingham University (UK), household pesticide use was investigated among Xhosa-speaking families living in three areas in South Africa (a rural area, an urban township and an informal settlement).
OBJECTIVES: The aim was to characterise pesticide use patterns and potential exposures through skin absorption, ingestion and inhalation for this group of South African children.
METHODS: A standardised questionnaire, which included a section investigating household pesticide use, was administered by four trained fieldworkers to the parents/guardians of the 740 children (25%) aged between 3 and 11 years identified as having atopic dermatitis either by clinical examination or according to the UK criteria (rural N=387, urban N=292, informal N=61).
RESULTS: Of the children with atopic dermatitis, 539 (73%) had been exposed to household pesticides. Most childhood exposure (89%) occurred in the informal settlements, followed by 78% in the urban area and 63% in the rural area.
CONCLUSIONS: This research highlighted considerable home environment pesticide exposure of South African children in lower socio-economic groups in rural, urban and informal areas. As children are particularly vulnerable to the short- and long-term health effects of pesticide exposure, further indepth investigation is needed to ascertain and document the health effects associated with such exposure in the home.
With increasing evidence of the high prevalence of pesticide use and the considerable risk it poses to children, it is of concern that there has been little research into the health implications of household pesticide use in South Africa. Research has drawn attention to the negative long-term health effects of pesticide exposure on children.1 Children are exposed to pesticides in various ways, for example through the food they eat and through use of pesticides at home, at school, in shops, clinics and hospitals and in public areas. Generally, children in lower income households endure poor housing quality with lack or poor provision of water, sanitation and refuse collection. This, coupled with poor indoor air quality and household pests such as rats, cockroaches and flies, directly impacts on health status.2 A study in Port Elizabeth found that aerosol insecticides were used regularly to combat pests in 20% of homes.3 Rats were such a common problem that half the people of low income in the study ignored them while the others used rat traps. The investigators also found that the cost of pesticides had a negative impact on lower income household budgets.
Several factors make children particularly vulnerable to the effects of pesticides. Children have a lower body weight and larger skin surface than adults, making skin exposure, the main route of pesticide absorption, more of a danger. Besides their immature developmental processes being vulnerable to disruption, children are less able to detoxify and excrete certain toxins and have a longer time in which to develop chronic diseases caused by early pesticide exposure. Children eat more for their size than adults, which increases their exposure if food is contaminated by pesticides, and because they tend to play on the ground they are likely to ingest residues in dust and sand, and to inhale pesticides present in low-lying layers of air.1,4
Research suggests that household pesticides are associated with an increased risk of childhood leukaemia, especially when mothers are exposed to indoor pesticide use during pregnancy.5 In utero and early childhood exposure may affect the development of the reproductive system, resulting in testicular cancer in males and early onset of puberty in females,1 including abnormal breast development.6 Low birth weight in newborns has been associated with exposure of pregnant women to pesticides.7,8 Prenatal exposure to pesticides used to control fleas and ticks has also been significantly associated with the development of paediatric brain tumours,9 as has residential pesticide exposure with childhood neuroblastoma.10 Organophosphate exposure in early childhood has been associated with various motor, learning and cognitive impairments.11 A South African study found that babies with birth defects were seven times more likely to be born to women exposed to garden and agricultural pesticides than to those not exposed.12
To our knowledge no study in South Africa has characterised household pesticide use patterns and resulting exposures. Pesticide surveillance, lacking in South Africa, is key to assessing the scope of pesticide-related effects on children's health and to developing appropriate legislation to protect children.13 We therefore aimed to characterise pesticide use patterns and potential childhood exposures.
Methodology
Data were obtained from a collaborative investigation in 1999 - 2001 by the Department of Dermatology, Groote Schuur Hospital (Cape Town, South Africa) and Nottingham University (UK) to assess the prevalence of atopic dermatitis in children living in rural, urban and informal areas, and to determine whether the UK criteria for diagnosing this condition were applicable in South Africa.14 The study findings on household pesticide use in South Africa were derived from this larger study.
Study areas
The study was undertaken in three areas in South Africa: a rural area in the Eastern Cape, an established urban township, and two informal settlements in the Western Cape. The urban township consisted of a combination of predominantly settled low- and middle-income housing interspersed with informal dwellings. The informal settlements consisted of unplanned dwellings (e.g. shacks).
The rural area studied included randomly selected villages or settlements within a 50 km radius of a hospital in the Transkei area, Eastern Cape, approximately 150 km from East London on the east coast of South Africa. The urban township studied is situated some 12 km from the Cape Town city centre. One informal settlement study area is located outside the Cape Town city centre in a high-density area, while the other is located within a lower-density housing area. Data from the two informal settlements were combined for analysis as their living conditions were similar.
In the rural study area most homes were solid mud structures with thatch roofing but no electricity, water or sanitation. Water was carried from boreholes or rivers or delivered by trucks. Sanitation was provided by separate structures with bucket facilities, although people mainly used the surrounding bush.
Homes in the urban township ranged from middle-income conventional structures with all amenities to low-income houses and flats with varying quality of water, electricity, sanitation and refuse removal provision. Some sections of the urban area included shacks similar to those found in the informal settlements.
Homes in the informal settlements were either constructed of wood or corrugated iron with cardboard and paper insulation. Lights were provided in open areas, but no legal electricity was available in the shacks, and paraffin was predominantly used for cooking. Free-standing toilet facilities and refuse collection were provided by the local authorities in both informal settlements.
Subjects
Three thousand Xhosa-speaking children between the ages of 3 and 11 years were randomly selected for inclusion in the original larger study, 1 000 each from the rural and urban township areas, and 500 from each of the two informal settlements. An attempt was made to select an equal number of male and female children from each area representing each age. Random sites within all four study areas were obtained by placing a grid over topographical maps and randomly selecting study sites within these grids. All available children in each area were examined for atopic dermatitis until the required number was reached. In the urban township and informal settlements of Cape Town, children were selected randomly by door-to-door visits and later examined at schools or facilities within the community (e.g. sports clubs).
In the rural study site, random door-to-door recruitment was not possible as homes were grouped in small clusters over a vast inaccessible area. A fieldworker obtained permission from community leaders to conduct research and arrange for parents and children to meet at the 10 schools that serviced their population. Study children were examined by one of the three dermatologists from Groote Schuur Hospital (UCT) and four trained fieldworkers administered the questionnaires.
Information on pesticide use was obtained from a separate questionnaire administered to the parents or guardians of the 740 children (25%) identified as having atopic dermatitis either by response to the questionnaires or by clinical examination (rural N=387; urban N=292; informal N=61).14 Questionnaires were filled out per child and not per household. Caregivers who completed questionnaires were predominantly mothers, but fathers, grandparents or other family members acted as respondents when mothers were not available. Fig. 1 shows the age distribution of the study population. There were more female children included in the rural (54%) and urban township areas (55%), but in the informal settlements there were more males (55%) than females.

Design
The questionnaire included open-ended questions on household pesticide use to assess children's potential exposures. Parents or guardians were asked what type of pests were a problem; whether they used poisons to kill these pests, and if so which poisons they used; how often they used these products, and whether they were in spray, liquid or powder form; whether they were used inside or outside the home; and whether they sprayed the beds or bedding.
The original reason for including a section on pesticide use in the larger study was to provide data for a possible follow-up study on the causes of atopic dermatitis. The questionnaire was piloted in the urban area, translated into Xhosa and back-translated into English.
Four trained Xhosa-speaking fieldworkers, two of whom were nursing sisters, were trained to administer the questionnaire by staff at the Department of Dermatology. The questionnaire data were entered into and analysed with Excel and Epi Info.
Results
Adult respondents in all areas specified rats (79%), fleas (51%), cockroaches (50%), mosquitoes (32%), bedbugs (16%) and ticks (4%) as being problematic household pests. Rats were by far the most cited, especially in the informal settlements (85%) and rural area (82%). Fleas were frequently listed in the informal areas (79%), while cockroaches troubled mostly urban residents (78%). To combat these pests, respondents reported use of several household pesticides. For rats, Rattex (a coumarin derivative) was quoted by 6% of respondents. In terms of level of toxicity of the pesticide products to which the children were exposed, 18% were classified by the World Health Organization (WHO) (www.who.int/ipcs/publications/en/pesticides_ hazard) as class Ia and b (i.e. extremely hazardous), 45% as class II (moderately hazardous), and 36% as class III (slightly hazardous) (Table I).
In total, 73% of children were reported to live in homes where pesticides were used. Eighty-nine per cent (N=54) of children in the informal settlements were exposed to pesticides, followed by 78% (N=302) in the urban township and approximately 63% (N=183) in the rural area. Besides Doom and Fastkill, Target was a popular pesticide in the urban township, and Fastkill was most commonly used in the rural area (Fig. 2).
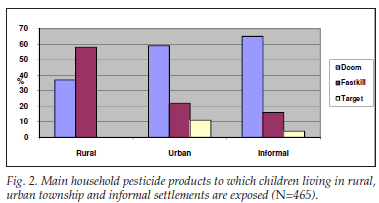
Overall, 97% of children were exposed to Doom and Fastkill as an inside aerosol, and 100% of those using Target sprayed this pesticide inside the home. Three per cent of children were exposed to chlorpyrifos, an organophosphate (Baygon contains chlorpyrifos as an active ingredient). Use of Rattex to combat rats was quoted 31 times. Although not a pesticide, Jeyes Fluid (a carbolic acid) was mentioned by two respondents as being used to control pests.
Most of the exposure of children to pesticides (89%) involved spraying of pesticides inside the home, typically irregularly in response to pest infestations (54%). Five per cent of children were exposed to daily spraying of pesticides and 19% to weekly spraying; of these most lived in the rural area (16%).
The pesticide to which children were exposed most frequently was a product marketed as Doom, which includes different formulations and agents. Products listed under this trade name with their active ingredients are tabulated in Table II.
In addition to general indoor pesticide use, beds and bedding were also sprayed. Children living in the urban township study area are most exposed to this type of pesticide use, followed by those living in the informal settlement areas (Table III).

Discussion
Children are particularly vulnerable to the effects of pesticides through skin absorption, ingestion and inhalation, with an increased risk of childhood leukaemia,5 brain tumours,9 neuroblastoma,10 damage to the developing reproductive system6 and cognitive impairment.11 Even though a South African study12 has indicated that babies are seven times more likely to be born with defects when women were exposed to garden and agricultural pesticides during pregnancy, there is no ongoing local research into the health effects of household and other pesticide use on children.
Climatic conditions and the poor housing structures in which most study children live contribute to the proliferation of household pests promoting disease and discomfort.2,3 To control these pests, many resort to the use of pesticides, often with little knowledge of their potential hazards. Some pesticide products identified in this study are classified by the WHO as extremely and moderately toxic, placing children exposed to them at risk of short- and long-term health effects.
The use of Jeyes Fluid for pest control highlights the need to investigate further what products not registered as pesticides are used to control household pests and could put children at further risk.
Parents did not mention head lice, although this is a problem for schoolgoing children regardless of socio-economic status. It is presumed that most children are exposed at some stage to pesticide shampoos that contain lindane as an active ingredient, which due to severe adverse health effects (e.g. suspected carcinogen) is banned in over 50 countries (www.panna.org). All the products mentioned by respondents are registered for use in South Africa under the Department of Agriculture's Act 36 of 1947 and commercially manufactured. Unlike the Port Elizabeth study,3 where half of the respondents used rat traps, in this investigation rats were the most commonly mentioned pest, but using rat traps for control was not mentioned.
The spraying of beds and bedding with pesticides is of particular concern as it exposes children for long periods of time. Bed spraying is a common cause of severe childhood poisoning requiring hospital admission.15 Parents and caregivers are generally unaware of the risks associated with pesticide use and do not have ready access to risk information.
Conclusion
An in-depth assessment of household pesticide use was not possible, although this research highlighted the considerable potential for household pesticide exposure of children in the lower socio-economic groups in rural, urban and informal areas.
Childhood exposure to pesticides is of concern internationally and in South Africa, as health hazards associated with household pesticide use can be severe and cause long-term developmental effects. Children who live in farming communities are furthermore exposed to both agricultural and household pesticides. Child exposure risks must be highlighted to all child carers in South Africa, as with better understanding adults become a vital link in risk reduction. Education programmes are also needed to create an understanding of hazard warnings on pesticide labels and improve risk awareness, particularly in vulnerable populations. Research and interventions are needed into cost-effective and readily available alternative methods of pest eradication in the home. It is therefore imperative that a more comprehensive exposure and assessment of the health risks to children be undertaken. To drive these initiatives, policy needs to be redrafted to include child-specific legislation to take into account the special vulnerabilities of this age group.
We thank Professor Gail Todd for permission to report on this part of the larger study, Professor Norma Saxe and Sarah Woods for their help, and Professor Hywel Williams of Nottingham University for his support. The study design was approved by the University of Cape Town's Health Sciences Faculty Research Ethics Committee.
References
1. Landrigan PJ. Pesticides and PCBs: Does the evidence show that they threaten children's health? Contemporary Pediatrics 2001; 2:110. [ Links ]
2. Mathee A, Swart A. A description of living conditions and health status in indoor informal settlements in Johannesburg. Urban Health and Development 2001; 4: 15-18. [ Links ]
3. Thomas EP, Seager JR, Viljoen E, et al. Household Environment and Health in Port Elizabeth, South Africa. Executive Summary. Port Elizabeth: South African Medical Research Council, University of Port Elizabeth, and Stockholm: Environment Institute, Sweden, 2001. [ Links ]
4. Eskenazi B, Bradman A, Castorina R. Exposures of children to organophosphate pesticides and their potential adverse health effects. Environ Health Perspect 1999; 107: Suppl 3, 409-419. [ Links ]
5. Ma X, Buffler PA, Gunier RB, et al. Critical windows of exposure to household pesticides and risk of childhood leukemia. Environ Health Perspect 2002: 110(9): 955-960. [ Links ]
6. Guillette EA, Conrad C, Lares F, et al. Altered breast development in young girls from an agricultural environment. Environ Health Perspect 2006; 114(3): 471-475. [ Links ]
7. Perera FP, Rauh V, Whyatt RM, et al. Effect of prenatal exposure to airborne polycyclic aromatic hydrocarbons on neurodevelopment in the first 3 years of life among inner-city children. Environ Health Perspect 2006; 114(8):1287-1292. [ Links ]
8. Eskenazi B, Marks AR, Bradman A, et al. In utero exposure to dichlorodiphenyltrichloroethane (DDT) and dichlorodiphenyldichloroethylene (DDE) and neurodevelopment among young Mexican American children. Pediatrics 2006; 118(1): 233-241. [ Links ]
9. Pogoda JM, Preston-Martin S. Household pesticides and risk of pediatric brain tumors. Environ Health Perspect 1997; 105: 1214-1220. [ Links ]
10. Daniels JL, Olshan AF, Teschke K, et al. Residential pesticide exposure and neuroblastoma. Epidemiology 2001; 12(1): 20-27. [ Links ]
11. Kofman, O, Berger A, Massarwa A, et al. Motor inhibition and learning Impairments in school-aged children following exposure to organophosphate pesticides in infancy. Pediatr Res 2006 Jul; 60(1): 88-92. [ Links ]
12. Heeren GA, Tyler J, Mandeya A. Agricultural chemical exposures and birth defects in the Eastern Cape Province, South Africa - a case-control study. Environmental Health: A Global Access Science Source 2003; 2: 11. [ Links ]
13. Rother H-A. Pesticides and children's health in South Africa: Research priorities emerging for policy consultations and a local case study. Urban Health and Development Bulletin 2001; 4(2): 45-49. [ Links ]
14. Chalmers DA, Todd G, Saxe N, et al. Validation of the United Kingdom Working Party diagnostic criteria for atopic eczema in a Xhosa speaking African population. Br J Dermatol 2007; 156(1): 111-116. [ Links ]
15. London L. Childhood pesticide poisoning - a clarion call for action on children's vulnerability (Editorial). S Afr Med J 2005; 95(9): 673-674. [ Links ]
Accepted 3 December 2008.
Corresponding author: S Tolosana (stolosana@telkomsa.net)














