Servicios Personalizados
Articulo
Indicadores
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares en Google
Similares en Google
Compartir
SAMJ: South African Medical Journal
versión On-line ISSN 2078-5135
versión impresa ISSN 0256-9574
SAMJ, S. Afr. med. j. vol.99 no.1 Pretoria ene. 2009
ORIGINAL ARTICLES
Rural-origin health science students at South African universities
J M TumboI; I D CouperII; J F M HugoIII
IMB ChB, MCFP (SA), MFamMed. Department of Family Medicine and Primary Health Care, University of Limpopo, Ga-Rankuwa
IIBA, MB BCh, MFamMed. Division of Rural Health, Department of Family Medicine, University of the Witwatersrand, Johannesburg
IIIMB ChB, MFamMed. Department of Family Medicine, University of Pretoria
ABSTRACT
BACKGROUND: Rural areas in all countries suffer from a shortage of health care professionals. In South Africa, the shortage is particularly marked; some rural areas have a doctor-to-population ratio of 5.5:100 000. Similar patterns apply to other health professionals. Increasing the proportion of rural-origin students in faculties of health sciences has been shown to be one way of addressing such shortages, as the students are more likely to work in rural areas after graduating.
OBJECTIVE: To determine the proportion of rural-origin students at all medical schools in South Africa.
DESIGN: A retrospective descriptive study was conducted in2003. Lists of undergraduate students admitted from 1999 to2002 for medicine, dentistry, physiotherapy and occupationaltherapy were obtained from 9 health science faculties. Origins of students were classified as city, town and rural by meansof postal codes. The proportion of rural-origin students was determined and compared with the percentage of rural people in South Africa (46.3%).
RESULTS: Of the 7 358 students, 4 341 (59%) were from cities, 1 107 (15%) from towns and 1 910 (26%) from rural areas. The proportion of rural-origin students in the different courses nationally were: medicine - 27.4%, physiotherapy - 22.4%, occupational therapy - 26.7%, and dentistry - 24.8%.
CONCLUSION: The proportion of rural-origin students in South Africa was considerably lower than the national rural population ratio. Strategies are needed to increase the number of rural-origin students in universities via preferential admission to alleviate the shortage of health professionals in rural areas.
Rural areas globally experience shortages of health care professionals. In South Africa, 46% and 46.3% of the population lived in rural areas in 1996 and 2001 respectively,1,2 but doctors were not similarly distributed. In 1993, the poorest districts in the country, which were largely rural, had 5.5 doctors per 100 000 population, compared with 35.6 in the wealthiest districts.3 The situation has not improved subsequently; in 2003, in the public sector, the mainly rural Eastern Cape and North West provinces had 12.7 and 11.5 doctors per 100 000 population; in comparison, the Western Cape and Gauteng had 31.9 and 25.4 doctors per 100 000 population, respectively.3 The corresponding figures for other health care professionals are similar or worse. Internationally, this disproportionate distribution of health care professionals has been shown to be influenced by factors such as domestic origin of the professionals, career choice, social amenities in urban areas, and the availability of specialists to support doctors.4 In Australia (a developed country with a substantial rural population), the main determinants for doctors remaining in rural practice have been shown to be rural background of medical students and a specialty choice in family practice.5
Increasing the proportion of rural-origin medical students in medical schools has the potential of alleviating the shortage of doctors in rural areas. Evidence from various countries that rural background is strongly associated with rural practice6-8 has been confirmed in South Africa.9 Nevertheless, no co-ordinated strategy exists for increasing the enrolment of ruralorigin students in South African health science faculties. We evaluated the admission data of rural-origin students to enable selection committees to formulate policies in this regard and to inform the national Department of Health (DoH) about the medical manpower needs of rural populations.
Method
A retrospective descriptive study was conducted in 2003 that included 9 health science faculties in South Africa from the universities of Cape Town (UCT), Free State (UFS), Limpopo (UL - formerly Medical University of South Africa (MEDUNSA)), KwaZulu-Natal (UKZN), Pretoria (UP), Stellenbosch (SU), Walter Sisulu University (WSU - formerly University of Transkei), Western Cape (UWC) and Witwatersrand (Wits).
Lists of undergraduate students enrolled for medicine, dentistry, occupational therapy and physiotherapy between 1999 and 2002 were obtained from the deans of the 9 faculties. Details of all students' addresses at the time of enrolment were obtained. Postal codes were used to classify addresses as city, town or rural. For this study, city was classified as major metropoles and provincial capitals, towns as regional centres, and rural as areas outside major urban areas, provincial capitals and towns. Students from foreign countries (128) and those without postal codes were excluded. Names of individual students were not used.
Ethical approval for conducting this study was obtained from the Research Ethics and Publication Committee of UL.
Results
Full data for the 4 years and courses were obtained from 7 of the 9 universities. UCT supplied data for 2001 and 2002 only, and SU for 2002 only. UWC did not offer medicine, and UCT did not offer dentistry. Information on 7 358 students was obtained from all 9 universities. Of the students, 4 341 (59%) were from cities, 1 107 (15%) from towns and 1 910 (26%) from rural areas.
In 5 of the 9 universities, the proportion of rural-origin students was <25%. UL and UFS had >40% rural-origin students (Table I). UL consistently had a proportion of ruralorigin students equal to or greater than the national rural population proportion of 46%.

All four disciplines had a rural-student proportion <30% (Table II).
In all courses, the proportion of rural-origin students was less than a third of the total student population (Fig. 1). The proportion of rural students was 16% in one instance. There was no significant trend in any direction in the proportions of rural students admitted over the 4-year period.
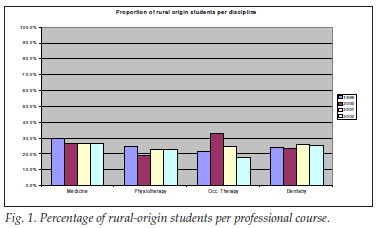
Discussion
These results provide baseline information regarding the domestic origins of health science students at 9 South African universities. The selected professional disciplines play a critical role in the care of patients at public health institutions. The average proportion of rural-origin health science students nationally over the 4-year period was 26%. In the 4 abovementioned disciplines, the average proportion of rural-origin students ranged between 22.3% and 27.5%, compared with the rural population of 46%.
There was a steady increase in the total number of health science students in South African universities between 1999 and 2002, ranging from 20% in medicine to 67% in occupational therapy. However, the proportion of rural-origin students did not increase and, in occupational therapy, the proportion of rural-origin students halved over a 3-year period. These findings are in contrast with Australia and the USA, where deliberate strategies have increased the admission of ruralorigin students.5,10
A South African study showed that 38.4% of rural-origin graduates were in rural practice, and 45.9% of doctors in rural areas were of rural origin,9 which is similar to patterns in other countries. In Norway, 56% of graduates from rural areas continued to work in such areas.10 Rural-origin graduates from the Universities of Missouri, Columbia,5 and Jefferson Medical College, Pennsylvania,11 were respectively 3 and 5 times more likely to remain in rural practice than those of urban origins, which suggests that the origin of students in the health science professions is an important determinant in predicting where they eventually practise. The relatively low number of rural-origin students in South African universities indicates that this factor has not been addressed in connection with the shortage of health professionals in rural South Africa.
The low proportions of rural-origin students in health science faculties could also be the result of lack of policy on preferential admission, poor academic performance of applicants from rural areas, disparity in the levels of education between urban and rural schools, and lack of access by students in rural areas to career guidance and information on university admission criteria. Inconsistency in the proportions of rural-origin students possibly points to the absence of national guidelines or policy regarding preferential admission of students from rural areas. The 2001/2002 DoH annual report acknowledged the significant contribution that selective recruitment and training of people from rural areas could have in solving the human resource problem in rural areas.12 In the report, the DoH committed to provide conditional grants and to remove disincentives that discourage doctors and other health professionals from working in rural areas. Our study supports the need for such interventions to increase the proportion of students of rural origin. The DoH National Health Summit in 2001 recommended that solving rural manpower shortages would require revised admission criteria, creative recruitment strategies, effective support for students from rural areas, and bursary arrangements to ensure a supply of students from rural and under-served areas.13,14 Specific bursaries and scholarships to rural-origin students, as supported by the World Organization of Family Doctors (WONCA) working party on training for rural practice,15 could also increase admissions on the model of rural scholarship schemes.16 Such strategies have not yet been developed.
The Higher Education Act (Act 101 of 1997, section 37) stipulates that '... the admission policy of a public higher education institution must provide appropriate measures for the redress of past inequalities and may not unfairly discriminate in any way'.17 Some universities have implemented this policy. UCT differentiates applicants on a racial basis, with different minimum entry requirements for each race to allow for black students with lower points than their white counterparts. UCT's criterion for admission of black students into medicine in 2009 is 36 points, compared with 42 for white students.18 A similar admission policy should be adopted by all universities and extended to include rural-origin students, who are at a disadvantage as a result of poor educational background and lack of facilities comparable with those in urban areas.
Our study did not seek to identify reasons for the rural distribution; it was also limited by inadequacy of data regarding students' demographic characteristics. Most universities would not provide even anonymous demographic data, citing the need to maintain student confidentiality. It was therefore not possible to evaluate the situation regarding pertinent characteristics such as race, sex and high-school locale. The imprecision of using postal codes to differentiate between rural and non-rural areas is acknowledged; however, they provide a reasonable proxy for students' backgrounds. In the absence of better means of categorisation, the researchers' knowledge of these areas augmented the final characterisation.
Conclusion
In South African universities, the proportion of health science students from rural areas remains low. In terms of the principle of equity, one might argue that the proportion of rural-origin students at universities should reflect national demographics.
The lower proportion of rural-origin students may partly be attributed to poor education in rural areas and the absence of a policy on preferential admission. There is a need for educational institutions, including universities, to become involved in rural schools and so uplift education levels. Increasing the proportion of rural-origin students at universities will tend to provide more health care workers who are more likely to serve in rural areas. Therefore, South Africa needs to develop an affirmative action strategy for rural-origin students. Incentives, guidelines and quotas to increase the admission proportion of rural-origin students are also needed. These steps should lay the foundation for a lasting solution to alleviating personnel shortages in rural areas.
This article was supported by the Rural Doctors Association of South Africa (RuDASA) and the Madibeng Centre for Research (MCR).
References
1. Census South Africa 1996. Pretoria: Statistics South Africa. http://www.statssa.gov.za (accessed 26 November 2002). [ Links ]
2. Census South Africa 2001. Pretoria: Statistics South Africa. http://www.statssa.gov.za (accessed 20 November 2002). [ Links ]
3. Day C, Gray A. Health and related indicators. In: Ijumba P, Barron P, eds. South African Health Review 2002. Durban: Health Systems Trust, 2003. [ Links ]
4. Cullison S, Reid C, Colwill JS. Medical school admissions, speciality selection and distribution of physicians. JAMA 1976; 235: 502-505. [ Links ]
5. Rabinowitz HK. A program to increase the number of family physicians in rural and underserved areas. Impact after 22 years. JAMA 1999; 281: 255-260. [ Links ]
6. Playford D, Larson A, Wheatland B. Going country: rural student placement factors associated with future rural employment in nursing and allied health. Aust J Rural Health 2006; 14(1): 14-19. [ Links ]
7. Laven G, Wilkinson D. Rural doctors and rural backgrounds: how strong is the evidence? A systematic review. Aust J Rural Health 2003; 11: 277-284. [ Links ]
8. Easterbrook M, Godwin M, Wilson R, et al. Rural background and clinical rural rotations during medical training: effect on practice location. CMAJ 1999; 160(8): 1159-1163. [ Links ]
9. De Vries E, Reid S. Do South African medical students of rural origin return to rural practice? S Afr Med J 2003; 93: 789-793. [ Links ]
10. Magnus JH, Tollan A. Rural doctor recruitment: Does medical education in rural districts recruit doctors to rural areas? Med Educ 1993; 27: 250-253. [ Links ]
11. Rabinowitz HK. Evaluation of a selective medical schools admission policy to increase the number of family physicians in rural and underserved areas. N Engl J Med 1998; 319: 480-486. [ Links ]
12. Human Resources and Equity: Department of Health Annual Report 2001/2002. Pretoria: Department of Health, 2002. [ Links ]
13. National Health Summit Proceedings, April 2001. Pretoria: Department of Health, 2001. [ Links ]
14. Lehmann U, Andrews G, Sanders D. Change and innovation in South African medical schools. South African Health Review 2000. Durban: Health Systems Trust, 2001: 10-11. [ Links ]
15. WONCA working party on training for rural practice. Policy on Training for Rural Practice. http://www.wonca.org (accessed 11 November 2003). [ Links ]
16. Ross AJ, Couper ID. Rural scholarship schemes: A solution to the human resource crisis in rural district hospitals. S Afr Fam Pract 2004; 46(1): 5-6. [ Links ]
17. The Higher Education Act 1997. Pretoria: South African Government Information. www.info.gov.za/gazette/acts/1997 (accessed 10 April 2008). [ Links ]
18. The University of Cape Town Admissions Policy. Cape Town: University of Cape Town, 2008. www.uct.ac.za/apply/prospectus/ugprospecus2009 (accessed 12 May 2008). [ Links ]
Accepted 26 August 2008.
Corresponding author: J Tumbo (tumbo@lantic.net)














