Services on Demand
Article
Indicators
Related links
-
 Cited by Google
Cited by Google -
 Similars in Google
Similars in Google
Share
SAMJ: South African Medical Journal
On-line version ISSN 2078-5135
Print version ISSN 0256-9574
SAMJ, S. Afr. med. j. vol.99 n.1 Pretoria Jan. 2009
ORIGINAL ARTICLES
Procedure for prolapsed haemorrhoids versus excisional haemorrhoidectomy - a systematic review and meta-analysis
T E MadibaI; T M EsterhuizenII; S R ThomsonIII
IMB ChB, MMed, PhD, FCS (SA), FASCRS. Department of Surgery, University of KwaZulu-Natal, Durban, and Colorectal Unit, Inkosi Albert Luthuli Central Hospital, Durban
IIMSc (Epidemiol). College of Health Sciences, University of KwaZulu-Natal, Durban
IIIMB ChB, ChM, FRCS (Edin). Department of Surgery, University of KwaZulu-Natal, Durban
ABSTRACT
BACKGROUND: The procedure for prolapse and haemorrhoids (PPH) was introduced to address the postoperative pain following excisional haemorrhoidectomy (EH).
OBJECTIVE: To assess the efficacy of both procedures to treathaemorrhoids.
DATA SOURCES: Literature review using MEDLINE. Articles addressing PPH and EH were included.
STUDY SELECTION: RCTs comparing EH and PPH with >20 patients.
DATA EXTRACTION: Primary endpoints were pain, operative time, hospital stay, satisfaction with procedure and time to return to normal activity. Secondary endpoints such as recurrence and complications were collated for descriptive analysis. A meta-analysis was performed using the random effects model on studies reporting 'mean' and SD or SEM.
DATA SYNTHESIS: PPH was associated with less postoperative pain, less operative time, shorter hospital stay and earlier return to normal activities compared with EH. There appears to be no significant difference in satisfaction with the procedure. There was no difference between the two procedures in terms of complications. There were more recurrences after PPH.
CONCLUSION: Compared with EH, PPH is associated with less postoperative pain, reduced operative time and hospital stay and earlier return to normal activity, and a trend towards improved patient satisfaction. The rate of recurrence appears higher with PPH.
First- and second-degree haemorrhoids as well as relatively small third-degree haemorrhoids can be treated nonoperatively, and surgery is generally reserved for patients with large third- or fourth-degree haemorrhoids, haemorrhoids with an extensive and symptomatic external component, or patients who have undergone less aggressive therapy with poor results.1-4 The definitive surgical procedure is excisional haemorrhoidectomy (EH), which can be performed as either an open (Milligan-Morgan) or a closed (Ferguson) operation.1,5 More recently, Antonio Longo introduced the procedure for prolapse and haemorrhoids (PPH).6 Both procedures can be undertaken under general or regional anaesthesia7,8 and are suitable for ambulatory surgery.7,9-15
Whereas EH removes the prolapsed haemorrhoids, it does not address the underlying cause of both mucosal and haemorrhoidal prolapse; conversely PPH, by 'lifting' the prolapsed haemorrhoids and mucosa, re-places the haemorrhoidal cushions high in the anal canal, thus reestablishing the topographical relationship between the anal cushions and the rectal muscle layer.16 Since the staple line is situated in the lower rectal mucosa as opposed to the anal mucosa, and there is no skin incision, it should in theory be associated with less postoperative pain.6,11 PPH has also been called stapled haemorrhoidectomy, stapled haemorrhoidopexy, stapled anopexy and stapled mucosectomy. This meta-analysis was undertaken to critically compare these two procedures and assess their efficacy in the treatment of haemorrhoids.
Methods
All articles addressing haemorrhoidectomy were identified using the MEDLINE electronic search engine. The keywords used were 'haemorrhoids', 'haemorrhoidectomy', 'stapled haemorrhoidectomy' and 'PPH', with the period of review extending from January 2000 to December 2007. Articles addressing PPH and EH were then reviewed. The search included all languages. All randomised controlled comparative trials and patient samples of >20 patients were considered for the meta-analysis. The primary endpoints assessed were pain, operative time, hospital stay, time taken to return to normal activity, and satisfaction with the operation. The first three were the most robust and the last two less so because of definition variability and fewer studies. Secondary endpoints were bleeding, complications and residual symptoms, recurrence rates and re-interventions. One author (TEM) performed the search and applied the inclusion criteria.
Studies addressing PPH alone were reviewed but not included in the comparison or meta-analysis. The different approaches (open v. closed) and techniques of EH used in the different studies were noted, but no distinction was made between them during the meta-analysis. For the purpose of this meta-analysis 'return to work' and 'return to normal activity' were treated as the same endpoint and 'examination under anaesthesia' performed subsequent to the procedure without an intervention was not regarded as re-intervention. Comparative studies on manometry and cost were also reviewed.
Meta-analysis
All studies using statistically valid outcome comparisons were used and random effects models were applied because of the heterogeneity of the studies. The studies reporting 'mean' and either 'standard deviation' or 'standard error of the mean' (mean ± SD/SEM) for all or some of the outcomes of interest were evaluated. Outcomes of interest that had been analysed in fewer than two studies and studies that had been analysed non-parametrically and reported medians were not used in the meta-analysis. The software, NCSS (Number Cruncher Statistical Systems, Kaysville, Utah, USA),17 was used for the meta-analysis and forest plots. All the complications were pooled together and odds ratios were calculated using a random effects model. Where a meta-analysis could not be calculated, the outcomes were qualitatively reviewed. The meta-analysis was performed by one of the authors (TME).
Results
Selection of data sets for analysis
Thirty-seven studies with 2 559 patients were identified comparing the two procedures (Fig. 1). Table I lists the alpha level, power and type II error for the identified studies in peer-reviewed journals. Two studies were excluded because they were not randomised.18,19 Two studies20,21 were mediumterm follow-ups of patients from two previous randomised controlled trials.22,23 Their data were only reviewed as follow-up data of the index studies. One further study24 had a subsequent follow-up study by the same authors.25
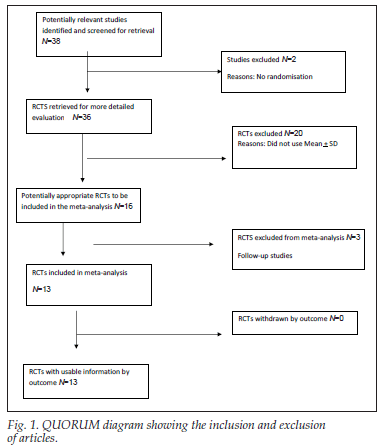
Inclusion and exclusion criteria were reported in all studies, but were varied. Eleven studies using the mean and standard deviation, and three using the mean and standard error of the mean, were used in one or other aspect of the meta-analysis. The excluded studies included median and range, mean and range or graphs and lack of randomisation. The total number of patients assessed was therefore 2 370 (EH = 1 170 and PPH = 1 200).
Limitations of the studies
The indications for haemorrhoidectomy were inconsistent in that second-, third- and fourth-degree haemorrhoids were included. The parameters and outcome measures were not uniform and were either not clearly defined or defined differently in different studies. 'Time to return to work' and 'time to return to normal activity' were used interchangeably in some studies and differently in others. The morbidity was neither defined nor standardised. The postoperative review was undertaken by an independent observer in only 12 studies.10,22,24,26-34 Information on recurrence was inconsistent because of variable definitions (recurrent symptoms, prolapse, or haemorrhoids alone or in combination) and their timelines. The patients studied were therefore not homogeneous.
As there is no bail-out procedure for haemorrhoidectomy it seems that the initial analysis was by 'intention to treat' and, since not all patients returned for follow-up in all studies, it is implicit that follow-up analysis must have been 'per protocol'.
Data analysis
Pain was assessed in all studies and was measured with a 10-point visual analogue score (VAS) in 23 studies (Table II). One study31 demonstrated a higher pain score for PPH in all categories of pain. Two studies showed similar maximal30,35 and average30 pain scores for both procedures. All other studies showed superiority of PPH in terms of less pain for PPH. Operating time was compared in 27 studies and PPH was associated with less operating time in all except three.30,31,36 Hospital stay was assessed by 20 studies, and it was either similar or less for PPH. Time taken to return to normal activity was shorter for PPH in all 23 studies (Table III). The level of satisfaction was shown to be similar in both procedures (Table IV). The overall recurrence rate was 1% following EH and 4% following PPH, making it four times higher after PPH (Tables IV and V).
When all complications were pooled together (Table V), the average postoperative morbidity for all studies was 48% following EH and 47% following PPH. Incontinence-related problems were similar in both groups (20% v. 24% for EH and PPH respectively). Immediate postoperative bleeding occurred in 2% and 3% in EH and PPH respectively and late bleeding (1 week to 12 months) occurred in 9% and 7% respectively in EH and PPH (Table V).
Re-interventions were necessary in 31 patients following EH (3%) and 42 patients (4%) after PPH. Re-interventions were for bleeding (20 following EH, 21 following PPH), residual haemorrhoids (2 for EH and 8 for PPH), fistula (3 after EH), skin tags (3 after EH and 4 after PPH), fissure (3 after EH), incision of thrombosed external pile (1 after PPH), incision and drainage of a peri-anal abscess (1 after EH), excision of mucosal prolapse (1 for EH and 1 for PPH). When all studies were considered, 11 patients in whom PPH failed underwent EH and 4 underwent unspecified revisional surgery; none of the patients developing recurrence or recurrent symptoms following EH required PPH.
Six studies compared costs but yielded conflicting results.18,26,30,37-39 The overall cost (including hospital expenses and procedure) for PPH was higher than for EH in 2 studies,26,30 1 of which used Ligasure for EH;26 it was higher for EH in 1 study.37 The cost per operation was higher for PPH in 2 studies18,39 and higher for EH in 1 study.38
Meta-analysis
The studies used in the meta-analysis addressed return to normal activity (12 studies, 1 178 patients), operative time (11 studies, 1 037 patients), hospital stay (9 studies, 891 patients), pain (8 studies, 815 patients), and satisfaction (4 studies, 387 patients). All effect sizes refer to the comparison of patients undergoing PPH (experimental arm) versus those undergoing EH (control arm). Most of the studies reviewed have been underpowered, and this has necessitated a meta-analysis. A sensitivity analysis was done and showed that the fixed effects analysis was not robust enough. Furthermore the tests for heterogeneity in all the studies used for the meta-analysis showed them to be heterogeneous (p<0.0001). For these reasons the random effects model was used.
The outcome of the meta-analysis is shown graphically by the forest plots of the effect sizes of the various individual studies and the combined effects in Figs 2 - 6 for each outcome. These figures show that the 95% confidence intervals (CIs) for the combined effect do not overlap with the null value (indicated by the vertical line at zero on the x-axis), except for satisfaction. The patients undergoing PPH therefore experienced a significantly lower mean score for pain, operative time, hospital stay and return to normal activity than did the patients in the control group (EH). The mean score for satisfaction was significantly higher for patients undergoing PPH in 2 studies,40,41 similar in 128 and higher in those undergoing EH in 1.30 The overall effect was strongly in favour of PPH. This meta-analysis therefore shows that PPH is superior to EH in terms of postoperative pain, operative time, hospital stay and time to return to normal activity.
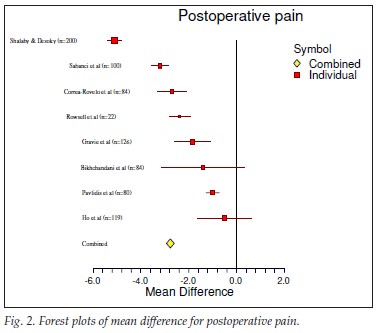
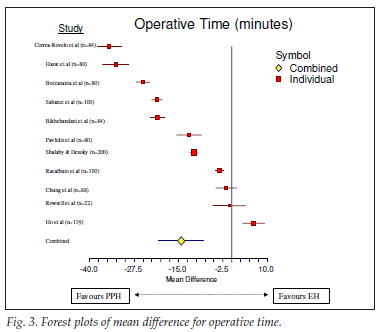
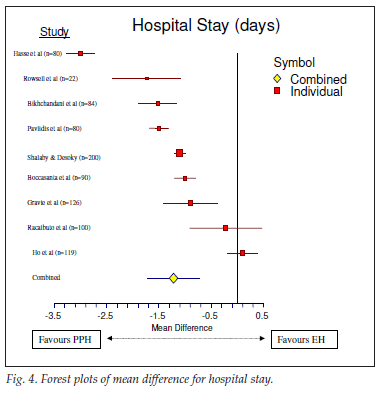
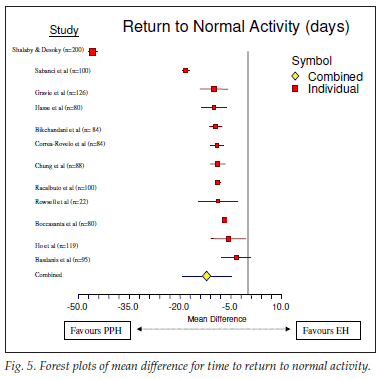
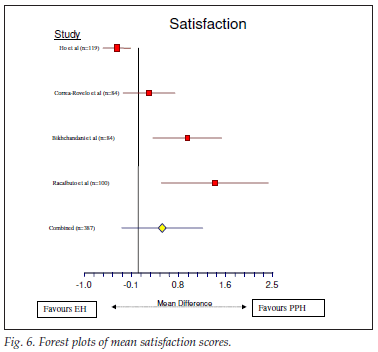
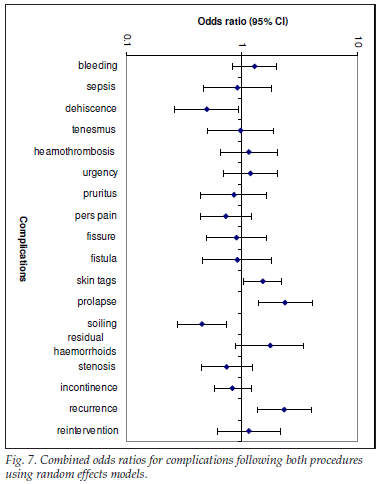
Fig. 6 shows pooled results of complications following both procedures. Combined odds ratios (ORs) using random effects model are shown. ORs favour PPH significantly in terms of dehiscence and soiling, they favour EH significantly in terms of prolapse and recurrence, and there were no differences in terms of all the other complications since the 95% CI for the combined effects ORs overlapped with the null value of 1.
Discussion
PPH shows superiority over EH in that it takes less time to perform and is associated with less postoperative pain, a shorter hospital stay and more rapid return to normal activity. Both procedures were followed by a number of complications and residual symptoms, but certain complications tended to occur more after one procedure than the other and vice versa.
The higher stenosis rate following EH was not surprising, as this is a known complication of EH. The presence of more prolapses after PPH was unexpected considering that PPH is designed to limit mucosal prolapse. However, the subjective feeling of a recurrent prolapse is difficult to confirm clinically42 and, since it may be difficult for patients to distinguish from skin tags, prolapse may be over-estimated.42,43
The original PPH stapler (PPH 01, Ethicon Endo-Surgery, Cincinnati, USA) has been modified in an attempt to reduce postoperative bleeding, the main feature being the closed staple height of 0.75 mm compared with 1 mm in the original stapler.44 Two studies have assessed the PPH 03 stapler and have shown it to be a safe and relatively short procedure with a low rate of postoperative complications such as bleeding.44,45 It also has the potential to reduce the risk of excision of the internal sphincter and rectal stenosis. Since patients who bleed from the staple line during surgery have an increased chance of postoperative bleeding, such bleeding should be managed by meticulous haemostatic suture placement.43
The cause of persistent anal pain after PPH in some patients remains uncertain.42 Cheetham et al.46 blamed persistent pain in 5 of 22 patients undergoing PPH on the presence of retained smooth muscle in the doughnut. However, a subsequent study by the same group47 interestingly failed to demonstrate prolonged pain despite the presence of smooth muscle in the doughnuts. Furthermore 13 of 22 other studies10,23,27-33,38,39,47,48 showed no association between smooth muscle in doughnuts and persistent pain. It seems therefore that the cause of persistent pain after PPH in a small number of patients remains obscure.
Significant complications specifically associated with PPH have been reported. These include rectal stenosis (10),49,50 persistent pain (5),46 rectal perforation (5),51-53 anal sphincter injury (1),54 retroperitoneal sepsis (1),55 rectal obstruction (1),56 intra-abdominal bleeding (1),57 rectal bleeding (1),58 retroperitoneal bleeding (1),59 and pelvic sepsis (1).60 Perforation of the rectum following PPH has been blamed on double firing of the stapler53 or staples cutting through an enterocele.57 Bleeding may be due to residual staples58 or seam insufficiency.59 Admittedly these are isolated case reports and no similar complications are reported relating to EH. Furthermore, when these exceptionally rare complications occur, they can be devastating. With the exception of bleeding, none of these complications was readily found in any of the studies included in the meta-analysis. They may therefore be expected more during the early learning phase of the procedure. Whereas some authors blame the PPH dilator for fragmentation of the internal sphincter,30 others have failed to demonstrate this effect.16 We are in agreement with Ravo et al.61 and Longo62 that most complications of PPH can be avoided by respecting the rectal wall anatomy in the performance of the procedure.
Although none of the studies had recurrence as a primary endpoint it should be a focus of future studies since, from the data presented here, the rate of recurrence was four times higher following PPH. It is interesting that the number of re-interventions (albeit variable in nature) was similar in both groups. Since none of the studies used repeat PPH to address PPH failure, it seems that failed PPH can only be corrected by EH and EH therefore cannot be completely replaced by PPH. Most of the studies have had short-term follow-up, with only four having >24 months' follow-up.19-21,41,63 We are in agreement with Brusciano et al.64 that a failed or complicated PPH is better treated by an experienced colorectal surgeon.
An increase in the acute-phase reactants results in acute pain and may be responsible for longer hospitalisation and time off work following EH.65 Furthermore, low-grade inflammation at the site of the staple line causes both anal pain and faecal urgency.42,66 Early discharge from hospital is favoured by most patients, and it can be reflected in good patient satisfaction and good quality of life. Factors associated with EH such as debilitating pain and poor wound healing may lead to longer hospital stay and later return to normal activity.
The earlier return to normal activity after PPH is multifactorial and, although some of the purely operation-dependent factors such as reduced pain, shorter hospital stay and reduced soiling play a role, other social and cultural practices also affect this parameter.22,67 Cephalad placement of the staple line has also been shown to be associated with quicker return to work.15
Despite arbitrary definitions, patient satisfaction was generally good for both procedures. Less pain leads to early return to work, and both outcomes are associated with better quality of life and a happy patient. The shorter operative time for PPH was in terms of minutes and is unlikely to have a bearing on satisfaction. Other factors that lead to dissatisfaction include pain, prolapse, bleeding and persistent soiling.42
The use of costly energy devices for haemostasis such as Ligasure and harmonic scalpel in EH equalises the in-hospital procedural costs of the PPH stapler, and is far more expensive than scissors and diathermy. The overall cost of the operation not only includes the cost of operating time, instruments and hospital stay, but also time off work, recurrent medication for symptoms, or recurrence and re-interventions. Hence overall cost, which has not been very well addressed in the literature, should be the benchmark for future financial comparisons.
Four other systemic reviews and meta-analyses8,68-70 have been published in the past 6 years. The first, by Sutherland et al.,70 reviewed 7 randomised controlled studies of which 6 were used in that meta-analysis. They used a fixed effects model rather than a random effects model. They included 4 of the 13 studies used for our random effects model analysis, which contains 9 studies conducted since their analysis. They stated that there was a 'reasonably clear evidence in favour of PPH in terms of reduced bleeding at two weeks and reduced length of hospital stay'.
Nisar et al.8 in 2004 reviewed 15 randomised controlled trials with 1 077 patients and undertook a meta-analysis on the pooled data. They noted PPH to be associated with less pain as well as shorter hospital stay, reduced operative time and more rapid return to normal activity. PPH, however, had a higher recurrence rate at minimum follow-up of 6 months. They concluded that EH was still a gold standard. Another systematic review of 10 randomised trials was published by Lan et al. in 2006.68 They only used studies in which the EH was performed by the Milligan-Morgan technique and they utilised only 3 of the studies employed in our random effects model analysis. They noted clear evidence in favour of PPH for reduced operative time, length of hospital stay, pain, anal discharge and increased satisfaction. PPH was no more superior to EH with regard to postoperative bleeding, resumption of normal activity, incontinence, anal resting and squeeze pressures. The most recent meta-analysis was published by Shao et al. in 2008.69 They analysed safety of the procedure and noted that there was insufficient evidence to advocate performing PPH in a day-case setting; they further concluded that PPH was at least as safe as EH and that it can be supported by a reasonable conventional operation for third- and fourth-degree haemorrhoids.
The former 3 systematic reviews used fewer studies than the present meta-analysis, and that by Shao et al.69 was more comprehensive. The present systematic review has included 33 studies, has undertaken meta-analysis in 13 studies, and has made use of forest plots to tabulate the trends graphically, thus making the data more robust than the data in the other 4 analyses. We have also assessed statistical power and likelihood of type II error of the studies, although this was not used to exclude the studies. There are several facets of this meta-analysis which provide better definition of the way forward in future studies, including the use of only third-degree haemorrhoids; recurrent bleeding, recurrent haemorrhoids and complications all need to be clearly defined endpoints. In long-term studies better data on overall costs are required, as PPH may lead to increased procedural cost. Furthermore, overall cost should take cognisance of the time taken to return to normal activity.
All the meta-analyses including the present meta-analysis are in agreement that there was significant heterogeneity between the results of trials available for the meta-analysis caused by relatively small sample sizes, variation in severity of disease, type of haemorrhoidectomy performed and method of reporting outcomes, and that trial results are difficult to interpret owing to variation in patient selection and methods of reporting endpoints, short follow-up times and poor reporting of complications. This significant heterogeneity is still evident in the studies we have added in this review and continues to detract from the robustness of the analysis. The possibility of publication bias cannot be excluded. The data available on long-term outcomes are also limited. More rigorous studies are needed with longer-term follow-up and larger sample sizes.
The appraisal committee of the recently published NICE technology appraisal on PPH4 also reached the same conclusions as the present meta-analysis. Other more recently published studies continue to show this trend, even in thrombosed haemorrhoids.71
Summary
Short-term results demonstrate superiority of PPH over EH in terms of pain, earlier return to normal activity and a minor reduction in operative time. This must be tempered by what appears to be a higher risk of recurrence which may or may not require further surgery. This long-term recurrence risk has never been a primary endpoint and, until more long-term data from better stratified series are reported, PPH cannot usurp EH as the best long-term cure for haemorrhoids. There are compelling reasons for EH which cannot be met by PPH, including acutely incarcerated and thrombosed haemorrhoids, presence of gangrene, the need for limited haemorrhoidectomy and the presence of numerous skin tags.2,71
Since both operations are associated with satisfactory results and since failure of PPH can be managed by EH, it is advisable that all surgeons learn both techniques. Surgeons should be aware that PPH may result in damage to the internal anal sphincter and other complications which, although exceptionally rare, may be life-threatening, and that EH is associated with its own set of more common but highly disturbing problems such as postoperative pain and anal stenosis. A surgeon competent to perform either PPH or EH should decide on the specific technique only after adequate discussion with his patient, including a detailed explanation of alternatives, benefits and procedure-related complications.
References
1. Madoff RD, Fleshman JW. American Gastroenterological Association technical review on the diagnosis and treatment of hemorrhoids. Gastroenterology 2004; 126: 1463-1473. [ Links ]
2. Sardinha TC, Corman ML. Hemorrhoids. Surg Clin North Am 2002; 82: 1153-1167. [ Links ]
3. Senagore AJ. Surgical management of hemorrhoids. J Gastrointest Surg 2002; 6: 295-297. [ Links ]
4. Tucker H, George E, Barnett D, et al. NICE technology appraisal on stapled haemorrhoidopexy for the treatment of haemorrhoids. Ann R Coll Surg Engl 2008; 90: 82-84. [ Links ]
5. McRae HM, McLeod RS. Comparison of hemorrhoidal treatment modalities. A meta-analysis. Dis Colon Rectum 1995; 38: 687-694. [ Links ]
6. Longo A. Treatment of haemorrhoidal disease by reduction of mucosa and haemorrhoidal prolapse with a circular suturing device: a new procedure. Proceedings of the 6th World Congress of Endoscopic Surgery, Rome, 3-6 June 1998, 777-784. [ Links ]
7. Esser S, Khubchandani I, Rakhmanine M. Stapled hemorrhoidectomy with local anesthesia can be performed safely and cost-efficiently. Dis Colon Rectum 2004; 47: 1164-1169. [ Links ]
8. Nisar PJ, Acheson AG, Neal KR, et al. Stapled hemorrhoidopexy compared with conventional hemorrhoidectomy: systemic review of randomized, controlled trials. Dis Colon Rectum 2004; 47: 1837-1845. [ Links ]
9. Hunt L, Luck AJ, Rudkin G, et al. Day-case haemorrhoidectomy. Br J Surg 1999; 86: 255-258. [ Links ]
10. Kairaluoma M, Nuorva K, Kellokumpu I. Day-case stapled (circular) vs diathermy hemorrhoidectomy. Dis Colon Rectum 2003; 46: 93-99. [ Links ]
11. Singer MA, Clintron JR, Fleshman J, et al. Early experience with stapled hemorrhoidectomy in the United States. Dis Colon Rectum 2002; 45: 360-367. [ Links ]
12. Guy RJ, Seow-Choen F. Septic complications after treatment of haemorrhoids. Br J Surg 2003; 90: 147-156. [ Links ]
13. Thompson-Fawcett MW, Cook TA, Baigrie RJ, et al. What patients think of day surgery proctology. Br J Surg 1998; 85: 1388. [ Links ]
14. Beattie GC, MacAdam TK, McIntosh SA, et al. Day case stapled haemorrhoidopexy for prolapsing haemorrhoids. Colorect Dis 2006; 8: 56-61. [ Links ]
15. Plocek MD, Kondylis LA, Duhan-Floyd N, et al. Hemorrhoidopexy staple line height predicts return to work. Dis Colon Rectum 2006; 49: 1905-1909. [ Links ]
16. Altomare DF, Rinaldi M, Sallustio PL, et al. Long-term effects of stapled haemorrhoidectomy on internal anal function and sensitivity. Br J Surg 2001; 88: 1487-1491. [ Links ]
17. Hintze J. NCSS and PASS. Number Cruncher Statistical Systems. www ncss com 2001 (accessed 29 October 2008). [ Links ]
18. Goulimaris I, Kanellos I, Christoforidis E, et al. Stapled haemorrhoidectomy compared with Milligan-Morgan excision for the treatment of prolapsing haemorrhoids: a prospective study. Eur J Surg 2002; 168: 621-625. [ Links ]
19. Mattana C, Coco C, Manno A, et al. Stapled hemorrhoidopexy and Milligan Morgan hemorrhoidectomy in the cure of fourth-degree hemorrhoids: Long term evaluation and clinical results. Dis Colon Rectum 2007; 50: 1770-1775. [ Links ]
20. Au-Yong I, Rowsell M, Hemingway DM. Randomised controlled clinical trial of stapled haemorrhoidectomy vs conventional haemorrhoidectomy: a three and half year follow-up. Colorect Dis 2004; 6: 37-38. [ Links ]
21. Smyth EF, Baker RP, Wilken BJ, et al. Stapled versus excision haemorrhoidectomy: long term follow-up of a randomised controlled trial. Lancet 2003; 361: 1437. [ Links ]
22. Mehigan BJ, Monson JRT, Hartley JE. Stapling procedure for haemorrhoids versus Milligan-Morgan haemorrhoidectomy: randomised controlled trial. Lancet 2000; 355: 782-785. [ Links ]
23. Rowsell M, Bello M, Hemingway DM. Circumferential mucosectomy (stapled haemorrhoidectomy) versus conventional haemorrhoidectomy: randomised controlled trial. Lancet 2000; 355: 779-781. [ Links ]
24. Ganio E, Altomare DF, Gabrielli F, et al. Prospective randomised multicentre trial comparing stapled with open haemorrhoidectomy. Br J Surg 2001; 88: 669-674. [ Links ]
25. Ganio E, Altomare DF, Milito G, et al. Long-term outcome of a multicentre randomised clinical trial of stapled haemorrhoidectomy versus Milligan-Morgan haemorrhoidectomy. Br J Surg 2007; 94: 1033-1037. [ Links ]
26. Basdanis G, Papadopoulos VN, Michalopoulos A, et al. Randomized clinical trial of stapled hemorrhoidectomy vs open with Ligasure for prolapsed piles. Surg Endosc 2005; 19: 235-239. [ Links ]
27. Chung CC. Stapled hemorrhoidectomy vs harmonic scalpel hemorrhoidectomy: A randomized trial. Dis Colon Rectum 2005; 48: 1215-1219. [ Links ]
28. Correa-Rovelo JM, Tellez O, Obregón L, et al. Stapled rectal mucosectomy vs closed hemorrhoidectomy. A randomised, clinical trial. Dis Colon Rectum 2002; 45:1367-1375. [ Links ]
29. Hetzer FH, Demartines N, Handschin AE, et al. Stapled vs excision hemorrhoidectomy. Long term results of prospective randomized trial. Arch Surg 2002; 137: 337-340. [ Links ]
30. Ho Y-H, Cheong W-K, Tsang C, et al. Stapled hemorrhoidectomy - cost and effectiveness. Randomised controlled trial including incontinence scoring, anorectal manometry and endoanal ultrasound assessments at up to three months. Dis Colon Rectum 2000; 43: 1666-1675. [ Links ]
31. Lau PYY, Meng WCS, Yip AWC. Stapled haemorrhoidectomy in Chinese patients: A prospective randomised control study. Hong Kong Med J 2004; 10: 373-377. [ Links ]
32. Ortiz H, Marzo J, Armendariz P. Randomised clinical trial of stapled haemorrhoidopexy versus conventional diathermy haemorrhoidectomy. Br J Surg 2002; 89: 1376-1381. [ Links ]
33. Ortiz H, Marzo J, Armendariz P, et al. Stapled hemorrhoidectomy vs diathermy excision for fourth degree hemorhoids: a randomised clinical trial and review of the literature. Dis Colon Rectum 2005; 48: 809-815. [ Links ]
34. Pavlidis T, Papaziogas B, Souparis A, et al. Modern stapled Longo procedure vs conventional Milligan-Morgan hemorrhoidectomy: a randomised controlled trial. Int J Colorect Dis 2002; 17: 50-53. [ Links ]
35. Palimento D, Picchio M, Attanasio U, et al. Stapled and open hemorrhoidectomy: randomized controlled trial of early results. World J Surg 2003; 27: 203-207. [ Links ]
36. Brown SR, Ballan K, Ho E, et al. Stapled mucosectomy for acute thrombosed circumferentially prolapsed piles: a prospective randomised comparison with conventional haemorrhoidectomy. Colorect Dis 2001; 3: 175-178. [ Links ]
37. Boccasanta P, Capretti PG, Venturi M, et al. Randomized controlled trial between stapled circumferential mucosectomy and conventional circular hemorrhoidectomy in advanced hemorrhoids with external mucosa prolapse. Am J Surg 2001; 182: 64-68. [ Links ]
38. Hasse C, Sitter H, Brune M, et al. Hämorrhoidektomie: Konventionelle exzision versus resektion mit dem klammernahtgerät. Prospektiv, randomisierte studie. Dtsch Med Wochenschr 2004; 129: 1611-1617. [ Links ]
39. Wilson MS, Pope V, Doran HE, et al. Objective comparison of stapled anopexy and open haemorhoidectomy. A randomized controlled trial. Dis Colon Rectum 2002; 45: 1437-1444. [ Links ]
40. Bikhchandani J, Agarwal PN, Kant R, et al. Randomized controlled trial to compare the early and mid-term results of stapled versus open hemorrhoidectomy. Am J Surg 2005; 189: 56-60. [ Links ]
41. Racalbuto A, Aliiotta I, Corsaro G, et al. Hemorrhoidal stapler prolapsectomy vs Milligan-Morgan hemorrhoidectomy: a long term randomized trial. Int J Colorect Dis 2004; 19: 239-244. [ Links ]
42. Fueglistaler P, Guenin MO, Montali I, et al. Long-term results after hemorrhoidopexy: High patient satisfaction despite frequent postoperative symptoms. Dis Colon Rectum 2007; 50: 204-212. [ Links ]
43. Koh DC, Cheong DM, Wong KS. Stapled haemorrhoidectomy: bothersome staple line bleeding. Asian J Surg 2005; 28: 193-197. [ Links ]
44. Lim YK, Eu K-W, Ho KS, et al. PPH03 stapled hemorrhoidectomy: our expereince. Tech Coloproctol 2006; 10: 43-46. [ Links ]
45. Angelone G, Giardiello C, Prota C. Bleeding after stapled haemorrhoidopexy using the PPH 03 stapler device. Chir Ital 2007; 59: 225-229. [ Links ]
46. Cheetham MJ, Mortensen NJM, Nystrom P-O, et al. Persistent pain and faecal urgency after stapled haemorrhoidectomy. Lancet 2000; 356: 730-733. [ Links ]
47. Cheetham MJ, Cohen CRG, Kamm MA, et al. A randomized, controlled trial of diathermy hemorrhoidectomy vs stapled hemorrhoidectomy in an intended day-care setting with longer follow-up. Dis Colon Rectum 2003; 46: 491-497. [ Links ]
48. Khalil KH, O'Bichere A, Sellu D. Randomised clinical trial of sutured versus stapled closed haemorrhoidectomy. Br J Surg 2000; 87:1352-1355. [ Links ]
49. Yao L, Zhong Y, Xu J, et al. Rectal stenosis after procedures for prolapse and hemorrhoids (PPH) - a report from China. World J Surg 2006; 30: 1311-1315. [ Links ]
50. Peterson S, Hellmich G, Schulmann D, et al. Early rectal stenosis following stapled rectal mucosectomy for hemorrhoids. BMC Surg 2004; 4: 6. [ Links ]
51. Herold A, Kirsch J, Staude G, et al. A German multicentre study on circular stapled haemorrhoidectomy. Colorect Dis 2000; 2(suppl): 18. [ Links ]
52. Wong LY, Jiang JK, Cang SC, et al. Rectal perforation: a life-threatening complication of stapled hemorrhoidectomy: report of a case. Dis Colon Rectum 2003; 46: 116-117. [ Links ]
53. Ripetti V, Caricato M, Arullani A. Rectal perforation, retropneumoperitoneum and pneumomediastinum after stapling procedure for prolapsed hemorrhoids: report of a case and subsequent considerations. Dis Colon Rectum 2002; 45: 268-270. [ Links ]
54. Ho Y-H, Seow-Choen F, Tsang C, et al. Randomised trial assessing anal sphincter injuries after stapled haemorrhoidectomy. Br J Surg 2001; 88: 1449-1455. [ Links ]
55. Maw A, Eu K-W, Seow-Choen F. Retroperitoneal sepsis complicating stapled hemorrhoidectomy: report of a case and review of the literature. Dis Colon Rectum 2002; 45: 826-828. [ Links ]
56. Cipriani S, Pescatori M. Acute rectal obstruction after PPH stapled haemorrhoidectomy. Colorect Dis 2002; 4: 367-370. [ Links ]
57. Aumann G, Petersen S, Pollack T. Severe intra-abdominal bleeding following stapled mucosectomy due to enterocoele: report of a case. Tech Coloproctol 2004; 8: 41-43. [ Links ]
58. Quah HM, Hadi HIA, Hay DJ, et al. Residual staples as a possible cause of recurrent rectal bleeding after stapled haemorrhoidectomy. Colorect Dis 2003; 6: 196. [ Links ]
59. Meyer P, Stieger R. Retroperitoneales hämatom mit sekundärer nahtinsuffizienz komplikation einer staplermukosektomie hemorrhoidectomy. Chirurg 2004; 75: 1125-1127. [ Links ]
60. Molloy RG, Kingsmore D. Life threatening pelvic sepsis after stapled haemorrhoidectomy. Lancet 2000; 355: 810. [ Links ]
61. Ravo B, Amato A, Bianco V, et al. Complications after stapled haemorrhoidectomy: Can they be prevented? Tech Coloproctol 2002; 6: 83-88. [ Links ]
62. Longo A. PPH at 10 years. Paper presented at the Cleveland Clinic Florida 18th Annual International Colorectal Disease Symposium, 15-17 February 2007, Fort Lauderdale, Florida. [ Links ]
63. Van de Stadt J, D'Hoore A, Duinslaeger M, et al. Long-term results after excision haemorrhoidectomy versus stapled haemorrhoidectomy for prolapsing haemorrhoids. A Belgian prospective randomized trial. Acta Chir Belg 2005; 105: 44-52. [ Links ]
64. Brusciano L, Ayabaca SM, Pescatori M, et al. Re-interventions after complicated or failed stapled hemorrhoidectomy. Dis Colon Rectum 2004; 47: 1846-1851. [ Links ]
65. Krška Z, Kvasnièka J, Faltýn J, et al. Surgical treatment of haemorrhoids according to Longo and Milligan Morgan: an evaluation of postoperative tissue response. Colorect Dis 2003; 5: 573-576. [ Links ]
66. Thaha MA, Irvine LA, Steele RJ, et al. Post-defaecation pain syndrome after circular stapled anopexy is abolished by oral nifedipine. Br J Surg 2005; 92: 208-210. [ Links ]
67. Senagore AJ, Singer MA, Abcarian H, et al. A prospective randomized, controlled multicenter trial comparing stapled hemorrhoidopexy and Ferguson hemorrhoidectomy: peri-operative and one-year results. Dis Colon Rectum 2004; 47: 1824-1836. [ Links ]
68. Lan P, Wu X, Zhou X, et al. The safety and efficacy of stapled hemorrhoidectomy in the treatment of hemorrhoids: a systematic review and meta-analysis of ten randomised control trials. Int J Colorect Dis 2006; 21: 172-177. [ Links ]
69. Shao W-J, Li G-CH, Zhang ZH-K, et al. Systematic review and meta-analysis of randomised controlled trials comparing stapled haemorrhoidopexy with conventional haemorrhoidectomy. Br J Surg 2008; 95: 147-160. [ Links ]
70. Sutherland LM, Matsuda BK, Sweeny JL, et al. A systematic review of stapled hemorrhoidectomy. Arch Surg 2002; 137: 1395-1406. [ Links ]
71. Wong JCH, Chung CC, Yau KK, et al. Stapled technique for acute thromobosed hemorrhoids: a randomised controlled trial with long term results. Dis Colon Rectum 2008; 51: 397-403. [ Links ]
72. Helmy MA. Stapling procedure for haemorrhoids versus conventional haemorrhoidectomy. J Egypt Soc Parasitol 2000; 30: 951-958. [ Links ]
73. Shalaby R, Desoky A. Randomised clinical trial of stapled versus Milligan-Morgan haemorrhoidectomy. Br J Surg 2001; 88: 1049-1053. [ Links ]
74. Gravié JF, Lehur P-A, Huten N, et al. Stapled hemorrhoidopexy versus Milligan-Morgan hemorrhoidectomy. A prospective randomized multicenter trial with 2-year postoperative follow-up. Ann Surg 2005; 242: 29-35. [ Links ]
75. Kraemer M, Parulava T, Roblick M, et al. Prospective randomised study: Proximate PPH vs Ligasure for haemorrhoidal surgery. Dis Colon Rectum 2005; 48: 1517-1522. [ Links ]
76. Sabanci U, Ogun I, Candemir G. Stapled haemorrhoidopexy versus Ferguson haemorrhoidectomy: a prospective study with 2-year postoperative follow-up. J Int Med Res 2007; 35: 917-921. [ Links ]
77. Ascanelli S, Gregorio C, Tonini G, et al. Long stapled haemorrhoidectomy versus Milligan-Morgan procedure: short and long term results of a randomised, controlled prospective trial. Chir Ital 2005; 57: 439-447. [ Links ]
Accepted 23 October 2008.
Corresponding author: T E Madiba (madiba@ukzn.ac.za)














