Services on Demand
Article
Indicators
Related links
-
 Cited by Google
Cited by Google -
 Similars in Google
Similars in Google
Share
SAMJ: South African Medical Journal
On-line version ISSN 2078-5135
Print version ISSN 0256-9574
SAMJ, S. Afr. med. j. vol.98 n.12 Pretoria Dec. 2008
ORIGINAL ARTICLES
Effect of African potato (Hypoxis hemerocallidea) on the pharmacokinetics of efavirenz
Seloi MogatleI; Michael SkinnerII; Edward MillsIII; Isadore KanferIV
IBSc (Pharm), BSc (Hons), PhD.Division of Pharmaceutics, Faculty of Pharmacy, Rhodes University, Grahamstown, E Cape
IIMPharm (Hons). Division of Pharmaceutics, Faculty of Pharmacy, Rhodes University, Grahamstown, E Cape
IIIBPharm, PhD. Biopharmaceutics Research Institute, Rhodes University, Grahamstown
IVMSc, PhD. British Columbia Centre for Excellence in HIV/AIDS, St. Paul's Hospital, Vancouver, Canada
ABSTRACT
PURPOSE: The purpose of this study was to evaluate the effect of the African potato (AP) on the pharmacokinetics of efavirenz.
METHODS: A single-dose, two-phase sequential study was conducted over 31 days in 10 healthy volunteers. On day 1 of the study, volunteers were administered a 600 mg efavirenz tablet, and blood samples were collected before dosing and at 0.5, 1, 1.5, 2, 2.5, 3, 3.5, 4, 5, 6, 8, 12, 18, 24, 36 and 48 hours after dosing. From day 16, a traditionally prepared AP decoction was administered daily until day 30. On day 29, volunteers were administered a single 600 mg dose of efavirenz, as was done on day 1. Plasma samples were harvested immediately after blood sample collection and frozen at -80°C until assayed. Plasma concentrations of efavirenz were determined by a validated high performance liquid chromatography (HPLC) method with UV detection, and pharmacokinetic parameters were calculated. Geometric mean ratios of Cmax and AUC0-48 of efavirenz before and after co-administration of 14 successive daily doses of AP were compared.
RESULTS: All subjects completed the study. The geometric mean ratios of Cmax and AUC0-48 were 97.30 and 102.82 with corresponding 90% confidence intervals (CIs) of 78.81 - 120.14 and 89.04 - 118.80, respectively.
CONCLUSION: Pharmacokinetic data generated during this study indicated that AP did not significantly alter the pharmacokinetics of efavirenz. Hence, co-administration of AP is unlikely to affect the clinical usage of efavirenz.
The use of natural health products (NHPs) as traditional medicines (TMs) among people living with HIV/AIDS is widespread, although their effects on the pharmacokinetics of antiretroviral medicines (ARVs) have not been established. The African potato (AP) received strong support from the former Minister of Health for use as an immune booster for HIV-positive patients, and is purported to be one of the best-selling NHPs in South Africa. Those taking TMs believe that they are effective and have few or no side-effects compared with current ARVs.1 The use of TMs is high among indigenous people in South Africa,2,3 with 33.5% of those living with HIV/AIDS4 using them to manage HIV symptoms. Patients receiving ARVs commonly take NHPs concurrently with their therapy despite there being little or no published information on the effectiveness and possibility of inter-interactions. In the Eastern Cape province of South Africa, the highest selling NHP was AP, at 11 tons/year.5 The corm of the AP is traditionally used for the treatment of urinary infections;6,7 among people living with AIDS, 64% of those who use TMs, use the AP.2In vitro and in vivo data have suggested that the AP has immune-boosting properties.8,9
Concomitant use of NHPs with orthodox medicines may affect the pharmacokinetics and pharmacodynamics through drug interaction mechanisms.10-12 NHPs can affect CYP450 enzymes and result in an increase or decrease in plasma concentrations of substrates which are metabolised by these enzyme systems. Possible effects of co-administration of NHPs and ARVs include increased side-effects of ARVs and losing the control of viral replication, which could lead to non-compliance and therapeutic failure, respectively.13,14
Hypoxoside, the main component of the AP,15 is not absorbed through the gut but is extensively metabolised in the colon by β-glucosidase to rooperol, which is then absorbed into the bloodstream16,17 and undergoes further metabolism to glucuronides and sulphates. In vitro studies have shown that hypoxoside induces the transporter protein, p-glycoprotein (P-gp) in Caco-2 cells, and stigmasterol, which is a constituent of AP, and rooperol both exhibited high inhibition of CYP3A4, 3A5 and CYP19 enzymes.18 Ingestion of the AP may therefore have the potential to affect both transporters and enzymes and consequently interfere with the absorption and metabolism of concurrently administered therapeutic agents.
Efavirenz is a non-nucleoside reverse transcriptase inhibitor (NNRTI) which is effective against HIV-1 infection and is the backbone of highly active antiretroviral therapy (HAART) in South Africa.19 Efavirenz is a substrate of both CYP3A4 and CYP2B6,20 and the metabolites are 7-hydroxyefavirenz, 8-hydroxyefavirenz and 8,14-dihydroxyefavirenz. It has a long half-life (of 52 - 76 hours) when administered as a single dose and 40 - 55 hours after multiple doses. The reduced half-life after multiple doses is due to metabolic auto-induction. Efavirenz is not a substrate of P-gp21 and therefore the absorption of efavirenz is unlikely to be affected by inducers or inhibitors of P-gp.
Since efavirenz and AP have been shown to be CYP450 enzyme substrates, the possibility exists of interaction between them when simultaneously administered. Reports have indicated that AP inhibits CYP3A4 in vitro.18 However, to our knowledge there is no published information that this occurs in vivo. We therefore investigated whether the concurrent administration of AP would affect the pharmacokinetics and subsequent clinical performance of efavirenz in human subjects.
Materials and methods
The HPLC system consisted of a Waters model 515 HPLC pump, a model 715 autosampler and a model 2995 PDA UV detector (Waters, Milford, MA, USA). Efavirenz was donated by Aspen Pharmacare (Port Elizabeth) and diclofenac sodium (DIC) was purchased from Sigma-Aldrich (Johannesburg). Acetonitrile and methanol of HPLC grade were purchased from Romil Ltd, Cambridge, UK, and formic acid 99.9% from Associated Chemical Enterprises, Johannesburg. Water was purified by reverse osmosis and filtration through a Milli-Q purification system (Millipore, Milford, MA, USA). Human plasma with potassium edentate (K-EDTA) as an anticoagulant was obtained from South African National Blood Services, Port Elizabeth.
Study population
Ten healthy, non-smoking, HIV-negative male subjects were enrolled after giving informed consent. Eligibility criteria included age between 18 and 55 years and a body mass index (BMI) between 19 and 30 kg/m2. Pre-study medical screening was performed within a month of initiating the study, and volunteers who passed the physical, medical and laboratory screening tests were enrolled. Laboratory tests included tests for liver function, hepatitis B and C, HIV, blood biochemistry, urinalysis and drugs of abuse (including amphetamines, barbiturates, benzodiazepines, cocaine, methamphetamine, morphine, phencyclidine, THC and TCA).
Prescription and over-the-counter medicines were restricted from 1 week before each phase until the last blood sample had been taken at the end of the study. Consumption of alcohol was forbidden from 4 days before the study, and caffeine and grapefruit juice were restricted from 48 hours before the study. Volunteers were prohibited from strenuous exercise from 24 hours before the study.
Study design
Ethical approval was granted by the Rhodes University Ethical Standards Committee; the study was conducted according to the South African Good Clinical Trials guidelines22 and Declaration of Helsinki and its amendments.
A single-dose, two-phase sequential study was conducted in healthy male volunteers under fasting conditions. Phase 1 started on day 1 and phase 2 started on day 29, each phase lasting 3 days. The washout period between the administration of the efavirenz doses was 28 days. The night before the study (day 0) volunteers were checked into the clinic and tested for drugs of abuse and alcohol consumption and questioned to ensure that they had complied with the study restrictions. Volunteers fasted for 10 hours before they were administered a 600 mg efavirenz tablet with a 240 ml glass of water. Standard meals were provided until 24 hours after dosing, and the times at which meals were started and finished were recorded as well as the amounts consumed. Blood samples were collected in Vacutainers containing potassium EDTA as the anticoagulant at the following time intervals: before dosing (0) and at 0.5, 1, 1.5, 2, 2.5, 3, 3.5, 4, 5, 6, 8, 12, 18, 24, 36 and 48 hours after dosing.
From day 16 until day 30 of the study, volunteers were administered a freshly prepared traditional AP decoction, at a dose of 15 mg/kg/day of hypoxoside, at the same time daily for 14 consecutive days. The AP decoction was prepared and assayed for hypoxoside content prior to administration. After receiving 12 consecutive daily doses of the AP decoction, phase 2 was initiated on day 28, when each of the volunteers received a 600 mg dose of efavirenz as at the beginning of the study. Blood samples were collected at the same time intervals as in phase 1.
Blood samples were centrifuged at 2 800 rpm for 10 minutes at 4°C, and plasma was harvested into two 2 ml polypropylene tubes (original and duplicate) and stored at -80°C until assayed.
Safety and tolerability
Baseline laboratory and medical data were documented before the study. During the study, volunteers were monitored for any adverse events, which were documented. Blood pressure, pulse and body temperature were taken before and 4 hours after dosing with efavirenz. During the study, volunteers were asked open questions about their wellbeing. Post-study laboratory and medical tests were conducted within 4 days of the end of phase 2 and the results compared with the baseline data.
Preparation and analysis of AP
The AP decoction was prepared in the traditional manner as follows: After removing the roots, the corms (~250 g) were washed with clean water, grated and weighed, boiled in 2.5 litres of water for 45 minutes, allowed to cool, and then mixed and strained with a clean muslin cloth before analysis. Two
10 ml samples of the AP preparation were placed in 20 ml Kimax centrifuge tubes and centrifuged in an IEC HN-SII centrifuge (Damon/IEC Division, Needham HTS, Massachusetts, USA) at 3 000 rpm for 10 minutes. The supernatant was filtered using a 0.44 µm filter and the internal standard, sulphamerazine, was added to the mixture, which was diluted by a factor of 500 and re-filtered. The samples were analysed according to a method reported by Nair.23
Analysis of plasma samples
Plasma samples were analysed by a validated HPLC method, and separation was achieved on a Phenomenex Luna a C18(2) (5 µm, 150 x 5 mm i.d.) column maintained at a temperature of 40±2°C. The mobile phase consisted of acetonitrile: 0.1M formic acid (pH 2.30): methanol (52:43:5 v/v/v) at a flow rate of 0.3 ml/min. The injection volume was 10 µl and the observed run time was less than 9 min. The eluent was monitored at λ = 247 nm and 275 nm for efavirenz and the internal standard, diclofenac sodium (DIC) respectively, using a photodiode array (PDA) detector.
An aliquot of 100 µl of plasma was precipitated with 200 µl DIC in mobile phase, the mixture was vortexed for 50 seconds and then centrifuged for 10 minutes at 13 500 rpm (10 000 g). About 100 µl of the supernatant was transferred to a micro-insert and injected into the HPLC system.
Pharmacokinetic analysis
The pharmacokinetic parameters of efavirenz before and after co-administration with AP were determined using a non-compartmental model.24 Exposure measures such as area under the curve (AUC) of the plasma concentration-time profiles from 0 hours to 48 hours (AUC0-48), and peak plasma EVF concentrations (Cmax) were used to assess the effect of AP on the pharmacokinetics of efavirenz. Other parameters that were monitored included the elimination half-life (t1/2), time taken to reach peak plasma concentration (tmax) and the elimination rate constant (k). The AUC0-48 and Cmax were calculated and the trapezoidal rule was used to estimate AUC0-48.
Statistical analysis
ANOVA analysis was conducted on Cmax and AUC0-48 using log-transformed data and the geometric mean ratios were calculated. The two one-sided t-test was used to determine the respective 90% CIs. An interaction would be concluded if the 90% CIs for Cmax and/or AUC0-48 were found to be outside the limits of 80 - 125%.25
Results
Demographic characteristics
Of the 10 enrolled healthy male volunteers, 9 (90%) were black and 1 (10%) was white; their mean age was 23 (range 19 - 27 years) and their BMIs ranged from 19.42 to 27.90 kg/m.2 All volunteers completed the study.
Pharmacokinetics of efavirenz
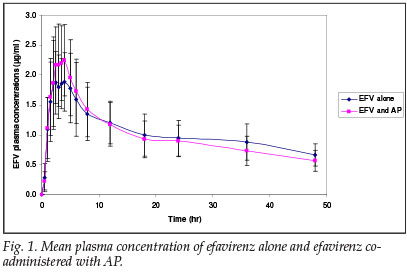
The mean plasma concentration/time profiles of efavirenz alone (phase 1) and efavirenz co-administered with AP (phase 2) are shown in Fig. 1. Visual inspection of the profiles suggests that plasma concentrations of efavirenz were not significantly affected by co-administration of AP. The geometric mean ratios of Cmax and AUC0-48 were 97.30 and 102.82, and the corresponding 90% CIs were 78.81 - 120.14 and 89.04 - 118.80, respectively. Whereas the 90% CI of the Cmax fell slightly outside the lower limit (78.81), the corresponding AUC0-48 values were within the limits of 80 - 125%. Hence, co-administration of AP with efavirenz did not appear to affect the pharmacokinetics of efavirenz. Table I summarises the pharmacokinetic parameters.
Safety and tolerability
Laboratory tests for all volunteers were normal; no serious adverse effects were reported or noted during the study. However, 2 subjects reported dizziness, euphoria and sleepiness during phase 2; they had peak plasma efavirenz concentrations of 3.26 and 3.34 µg/ml, respectively, while the other volunteers had peak plasma concentrations <3.05 µg/ml.
Discussion
Although the 90% CIs for Cmax did not fall within the 80 - 125% interval, the acceptance limits for this parameter are generally considered to be less important than the AUC. Hence, the findings from this study suggest that interactions as a result of the co-administration of AP and efavirenz are unlikely. There was no significant change in the measured pharmacokinetic parameters of efavirenz when administered alone or concomitantly with AP.
In vitro hypoxoside inhibits CYP3A4 enzymes and also induces P-gp.18 This differs in vivo since hypoxoside is rapidly metabolised to rooperol following oral administration in humans16 and is not absorbed per se. Therefore, only rooperol, the hypoxoside metabolite, enters the systemic circulation, where it is metabolised to form highly water-soluble glucuronides and sulphates. Hence, any effect on the CYP3A4 enzymes following AP administration is unlikely to be due to hypoxoside. On the other hand, owing to the effective metabolism of rooperol, it is possible that concentrations of rooperol in the blood after oral consumption of AP are too low to significantly affect the activity of the CYP3A4 enzyme system.
It is suggested that efavirenz is mainly metabolised by CYP2B6 and to a lesser extent CYP3A4.20 Whereas hypoxoside and rooperol have been shown to affect CYP3A4 in vitro, and since the pharmacokinetics of efavirenz were not altered following co-administration of AP, components of AP probably do not affect CYP2B6 enzymes. Some other constituents of AP such as stigmasterol, however, were also found to inhibit CYP3A4 in vitro but the activity of stigmasterol in vivo did not alter the pharmacokinetics of efavirenz in this study.
Even though hypoxoside is not absorbed into the blood, it could still induce P-gp in the stomach and small intestine because it is only metabolised in the colon; therefore, absorption of therapeutic agents which are substrates of P-gp could be affected. Notwithstanding, such an interaction is not expected to influence the plasma concentration of efavirenz since efavirenz is not a substrate of P-gp.21
Conclusions
The co-administration of AP with efavirenz in our study does not appear to affect the pharmacokinetics of efavirenz; hence, interference with efavirenz therapy is not expected. There is, however, a need to investigate the effect of AP on other ARVs, particularly those ARVs which are P-gp substrates or whose major metabolic pathway is via CYP3A4 isozymes.
We gratefully acknowledge financial support from the Ontario HIV/AIDS Network (OHTN) and the Medical Research Council (MRC) of South Africa, and author SM thankfully acknowledges the Botswana Government for a scholarship.
References
1. Leonard B, Huff H, Merryweather B, Lim A, Mills E. Knowledge of safety and herb-drug interactions amongst HIV+ individuals: A focus group study. Can J Clin Pharmacol 2004; 11(2): e227-231. [ Links ]
2. Babb DA, Pemba L, Seatlanyane P, Charalambous S, Churchyard GJ, Grant AD. Use of traditional medicine by HIV-infected individuals in South Africa in the era of antiretroviral therapy. Psychol Health Med 2007; 12: 314-320. [ Links ]
3. Cocks M, Dold A. The role of 'African chemists' in the health care system of the Eastern Cape province of South Africa. Soc Sci Med 2000; 51: 1505-1515. [ Links ]
4. Sukati NA, Mndebele SC, Makoa ET, et al. HIV/AIDS symptom management in Southern Africa. J Pan Symptom Manage 2005; 29: 185-192. [ Links ]
5. Dold A, Cocks M. The trade in medicinal plants in the Eastern Cape province, South Africa. S Afr J Sci 2002; 98: 589-597. [ Links ]
6. Buwa LV, Van Staden J. Antibacterial and antifungal activity of traditional medicinal plants used against venereal diseases in South Africa. J Ethnopharmacol 2006; 103: 139-142. [ Links ]
7. Louw CAM, Regnier TJC, Korsten L. Medicinal bulbous plants of South Africa and their traditional relevance in the control of infectious diseases. J Ethnopharmacol 2002; 82: 147-154. [ Links ]
8. Bouic PJD, Clark A, Brittle W, Lamprecht JH, Freestone M, Liebenberg RW. Plant sterol/ sterolin supplement use in a cohort of South African HIV-infected patients - effects on immunological and virological surrogate markers. S Afr Med J 2001; 91: 848-850. [ Links ]
9. Breytenbach U, Clark A, Lamprecht J, Bouic P. Flow cytometric analysis of the Th1-Th2 balance in healthy individuals and patients infected with the human immunodeficiency virus (HIV) receiving a plant sterol/sterolin mixture. Cell Biol Int 2001; 25: 43-19. [ Links ]
10. Jiang X, Williams KM, Liauw WS, et al. Effect of St John's wort and ginseng on the pharmacokinetics and pharmacodynamics of warfarin in healthy subjects. Br J Clin Pharmacol 2004; 57: 592-599. [ Links ]
11. Kawaguchi A, Ohmori M, Tsuruoka S, et al. Drug interaction between St John's wort and quazepam. Br J Clin Pharmacol 2004; 58: 403-410. [ Links ]
12. Tushar T, Vinod T, Rajan S, Shashindran C, Adithan C. Effect of honey on CYP3A4, CYP2D6 and CYP2C19 enzyme activity in healthy human volunteers. Basic Clin Pharmacol Toxicol 2007; 100: 269-272. [ Links ]
13. Mills E, Foster BC, Van Heeswijk R, et al. Impact of African herbal medicines on antiretroviral metabolism. AIDS 2005; 19: 95-97. [ Links ]
14. Mills E, Cooper C, Seely D, Kanfer I. African herbal medicines in the treatment of HIV: Hypoxis and sutherlandia. An overview of evidence and pharmacology. Nutr J 2005; 4: 19. [ Links ]
15. Betto P, Gabrielle R, Galeffi C. Determination of the norlignan glucosides of hypoxidaceae by high-performance liquid chromatography. J Chromatogr 1992; 594: 131-135. [ Links ]
16. Kruger PB, Albrecht C F de V, Liebenberg RW, van Jaarsveld PP. Studies on hypoxoside and rooperol analogues from Hypoxis rooperi and Hypoxis latifolia and their biotransformation in man by using high-performance liquid chromatography with in-line sorption enrichment and diode-array detection. J Chromatogr B Biomed Sci Appl 1994; 662: 71-78. [ Links ]
17. Albrecht CF, Kruger PB, Smit BJ, et al The pharmacokinetic behaviour of hypoxoside taken orally by patients with lung cancer in a phase I trial. S Afr Med J 1995; 85: 861-865. [ Links ]
18. Vipin D P, Nair BC, Foster J, Arnason T, Mills EJ, Kanfer I. In vitro evaluation of human cytochrome P450 and P-glycoprotein-mediated metabolism of some phytochemicals in extracts and formulations of African potato. Phytomedicine 2007; 14: 498-507. [ Links ]
19. Department of Health. National Antiretroviral Treatment Guidelines. Pretoria: Department of Health, 2004. [ Links ]
20. Ward BA, Gorski JC, Jones DR, Hall SD, Flockhart DA, Desta Z. The cytochrome P450 2B6 (CYP2B6) is the main catalyst of efavirenz primary and secondary metabolism: Implication for HIV/AIDS therapy and utility of efavirenz as a substrate marker of CYP2B6 catalytic activity. J Pharmacol Exp Ther 2003; 306: 287-300. [ Links ]
21. Stormer E, Von Moltke LL, Perloff MD, Greenblatt DJ. Differential modulation of P-glycoprotein expression and activity by non-nucleoside HIV-1 reverse transcriptase inhibitors in cell culture. Pharm Res 2002; 19: 1038-1045. [ Links ]
22. Department of Health. Guidelines for Good Practice in the Conduct of Clinical Trials in Human Participants in South Africa. Pretoria: Department of Health, 2000. [ Links ]
23. Nair VDP, Kanfer I. High-performance liquid chromatographic method for the quantitative determination of hypoxoside in African potato (Hypoxis hemerocallidea) and in commercial products containing the plant material and/or its extracts. J Agric Food Chem 2006; 54: 2816-2821. [ Links ]
24. Gibaldi M, Perrier D. Pharmacokinetics-Vol 15, Drugs and the Pharmaceutical Sciences. 2nd ed. New York: Marcel Dekker, 1982. [ Links ]
25. U.S. Department of Health and Human Services. Guidance for Industry - In vivo Drug Metabolism/Drug Interaction Studies - Study Design, Data Analysis and Recommendations for Dosing and Labelling. Rockville, MD: U.S. Department of Health and Human Services. Food and Drug Administration, Center for Drug Evaluation and Research (CDER), Center for Biologics Evaluation and Research (CBER), November 1999. [ Links ]
 Correspondence:
Correspondence:
I Kanfer
(I.Kanfer@ru.ac.2a)














