Serviços Personalizados
Artigo
Indicadores
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares em Google
Similares em Google
Compartilhar
SAMJ: South African Medical Journal
versão On-line ISSN 2078-5135
versão impressa ISSN 0256-9574
SAMJ, S. Afr. med. j. vol.98 no.8 Pretoria Ago. 2008
ORIGINAL ARTICLES
Hypertension and diabetes: Poor care for patients at community health centres
Krisela SteynI; Naomi S LevittII; Maya PatelIII; Jean FourieIV; Nomonde GwebusheV; Carl LombardVI; Kathy EverettVII
IMSc, NED, MD; Department of Medicine, University of Cape Town, and Chronic Diseases of Lifestyle Unit, Medical Research Council, Tygerberg, W Cape
IIFCP, MD; Department of Medicine, University of Cape Town
IIIMB ChB, FCRad (Diag) SA, MMed; Chronic Diseases of Lifestyle Unit, Medical Research Council
IVBA (Nursing), MPhil (Translation); Chronic Diseases of Lifestyle Unit, Medical Research Council
VBSc Hons; Biostatistics Unit, Medical Research Council
VIMSc, PhD; Biostatistics Unit, Medical Research Council
VIIBA (HDE), Diploma in Health Promotion; Chronic Diseases of Lifestyle Unit, Medical Research Council
ABSTRACT
OBJECTIVES: To identify health care provider-related determinants of diabetes and hypertension management in patients attending public sector community health centres (CHCs).
METHODS: A random sample of 18 CHCs in the Cape Peninsula providing hypertension and diabetes care was selected. Twenty-five patients with diabetes and 35 with hypertension per clinic were selected and interviewed by trained fieldworkers, and their medical records were audited. Regression analyses identified predictors of controlled hypertension (<140/90 mmHg) and diabetes (HbA1c <7%). In-depth interviews with nurses and doctors explored their experiences in working at the CHCs. Height, weight and blood pressure (BP) were measured for all patients and random blood samples collected for lipids, glucose, HbA1c and creatinine.
RESULTS: Of the participants 923 had hypertension and 455 diabetes (289 had both conditions). Of the hypertensive patients 33% had a BP <140/90 mmHg, while 42% of the patients with diabetes had non-fasting glucose levels below 11.1 mmol/l. Patients' knowledge about their conditions was poor. Prescriptions for drugs were not recorded in medical records of 22.6% of the patients with diabetes and 11.4% of those with hypertension.
CONCLUSIONS: Primary care for patients with hypertension and diabetes at public sector CHCs is suboptimal. This study highlights the urgent need to improve health care for patients with these conditions in public sector clinics in the Cape Peninsula.
Public sector clinics dealing with patients with acute conditions rarely provide adequate care for those with chronic conditions or attempt to address their risk factors, and generally lack patient-centred initiatives to empower patients to become active partners in their own care. Planning to improve the way primary health care services deal with acute and chronic conditions is lacking.1 Consequently levels of control of hypertension, with age-adjusted prevalence rates of 20 - 30%, and diabetes, with age-adjusted prevalence rates of 4 - 10%, are poor, leading to high rates of complications.2,3
Most people with hypertension and diabetes in South Africa receive treatment in the public health care system, and in Cape Town they attend the community health centres (CHCs). These are known to have deficiencies in levels of care,4,5 with a high prevalence of unrecorded diabetic complications, suboptimal glycaemic and blood pressure (BP) control, 'routinised' care and polypharmacy.4 Despite improvements in frequency of BP measurement, follow-up and compliance, hypertension has been found to be uncontrolled in approximately 50% of patients.5 We surveyed patients with diabetes and those with hypertension attending CHCs to identify their treatment status and audited the clinic records to assess the recorded responses of health care providers in managing their patients. In-depth interviews with doctors and nurses investigated their experiences in working at the CHCs.
Setting and sampling
The CHCs that provide primary health care in the Cape Peninsula can be reached easily by most patients and attendance is free of charge. Registered nurses and general medical practitioners (medical officers) provide the care and refer patients to secondary hospitals when required. Each medical officer (MO) manages between 40 and 70 patients per day. Medication from an essential drugs list is dispensed from a CHC pharmacy.
During 1999, 18 of 35 possible CHCs in Cape Town were randomly selected for this cross-sectional study, and 35 patients with hypertension and 25 with diabetes were selected per clinic. Inclusion criteria were age 15 years or older, being a documented attendee at the particular CHC with at least four visits during the previous year for hypertension or diabetes, and having received treatment for these conditions at each visit. Participants who were unable to provide answers to a questionnaire, previously piloted and translated into Afrikaans and isiXhosa, were excluded.
The audit covering the preceding year included all participating patients' medical records for diabetes (N=454) and hypertension (N=923). The medications prescribed at the last visit to the CHC for common chronic conditions were classified according to the Anatomical Therapeutic Chemical (ATC) classification codes, which allow the identification of medications for some common chronic conditions.6
Ten open and flexible in-depth interviews were conducted in private with nurses and doctors purposefully sampled from six of the participating clinics. These allowed respondents to explore issues in their own terms and raise other topics for discussion.
Measurements
BP was measured using the South African Hypertension Society's guidelines and controlled hypertension was defined as a BP below 140/90 mmHg.7
Non-fasting blood glucose (cut-off point <11.1 mmol/l) and total cholesterol (TC) (cut-off point <5 mmol/l) were measured in all patients, while glycosylated haemoglobin (HbA1c) was only measured in the patients with diabetes. For diabetes the 'acceptable' glycaemic target was an HbAlc level of <5.9%.8
Statistical analyses
Data were coded and computerised, and analyses provided descriptive statistics of the study population.
To identify the variables associated with BP and diabetes control, a tree regression analysis was conducted.9 Possible variables associated with BP or diabetes control were then used for the univariate logistic regression analyses, and tested in a multiple logistic regression adjusted for the clustering within clinics, to identify characteristics that were independently related to BP and diabetes control.10
In-depth interviews were analysed and coded, while emerging categories and themes underpinned the development of an analytical framework that was applied across all the interviews. This analytical process of open, selective and axial coding followed previously described processes.11,12
Results
Of the 1 089 participants, 923 were hypertensive and 455 were diabetic (289 had both conditions); most (78.8%) were women. Their mean age was 60.3±11.1 years, more than half were pensioners or received a disability grant, and only about 20% were employed. About half the participants had either primary school or no education.
The survey data showed poor levels of hypertension and diabetes control (Table I). Of the patients with hypertension 67.2% had a BP of >140/90 mmHg, and 76.1% of those with diabetes had BPs above the recommended cut-off point of 130/85 mmHg. Furthermore, 76% of patients with diabetes had HbA1c levels >1% above the upper limit of normal (5.9%). Associated risk factors were poorly controlled, e.g. about 70% of the participants had a total cholesterol (TC) level above the cut-off point of 5 mmol/l (Table II).

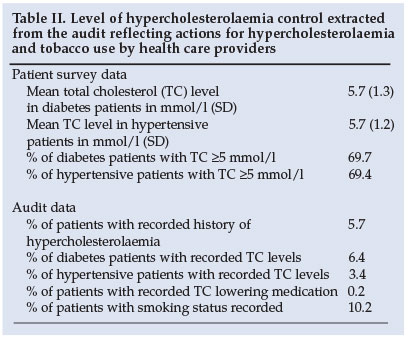
Patients had little knowledge about their chronic condition. Of the hypertensive patients 63% knew that their condition causes stroke, but knowledge about the consequences of untreated hypertension was otherwise poor, and less than 1% knew that renal failure could result from poor treatment. Diabetes patients had little understanding of how to manage hyper- or hypoglycaemia and inadequate knowledge of the impact of poor diabetes control. About 80% of patients said that they took their medication as prescribed. However, only 66.2% and 74% of patients with hypertension and diabetes, respectively, had taken their medication on the morning of their clinic visit. Unhealthy lifestyles were common, with just over 20% smoking at least one cigarette a day. Of those who had ever smoked daily, about a third had tried to quit smoking and most had started smoking again.
Medical records revealed that poor BP and blood glucose control tended to be of long standing. BPs and blood glucose were recorded for 98% of the patients (Table I), and the records reflected few aspects of good hypertension and diabetes care and follow-up. Co-morbid conditions, special investigations and clinical signs of target organ damage were seldom noted; for example only 11.3% of patients with diabetes had a record of examination of their feet, and only 2.6% had a record of HbA1c measurements.
Drug prescriptions were not recorded in 22.6% and 11.4% of the diabetes and hypertensive patient records, respectively, while 73.9% of patients with diabetes and 80.8% of those with hypertension had one appropriate drug recorded for their condition. Of the patients with diabetes 9.5% used insulin and 68.8% oral anti-diabetic agents. Of the patients with hypertension only 35.4% used diuretics, 13% angiotensin-converting enzyme (ACE) inhibitors, 11% beta-blockers and 6% reserpine and methyldopa. Medication for other chronic conditions was recorded in about 10% of patients in both groups, while less than 0.5% were prescribed cholesterol-lowering drugs.
When comparing the BP and HbA1c levels along with those levels that are controlled in patients attending CHCs with and without dedicated hypertension or diabetes clinics, no significant differences were observed after adjusting for the clustering effect of the sample. However, a simple univariate analysis showed that patients attending dedicated hypertension clinics at CHCs had significantly lower systolic BP levels (6.7 mmHg, p<0.05) than those who did not attend such clinics. Adjusting for the clustering effect of the CHCs, the comparison was not significant (p=0.101).
Results of the multivariate regression analyses, after adjustment for the clustering in CHCs used to identify the predictors of controlled hypertension and diabetes among patients whose BP and HbA1c levels were below 140/90 mHg and 7% respectively, are shown in Table III. Older hypertensives and men had significantly poorer BP control; patients receiving a disability grant had better BP control than those who were employed; and those reporting a higher BP at the previous visit had significantly poorer BP control. Patients with a urinary dipstick measurement had significantly poorer BP control than those without such recordings.
Major themes that emerged from analysis of the in-depth interviews included that doctors and nurses were working under increasingly difficult circumstances; staff shortages were the main barriers to effectively managing patients with diabetes and hypertension; the complexity of cases previously managed by specialists at tertiary hospitals was of concern; and there was much dissatisfaction at the lack of financial resources to conduct special investigations. All respondents felt angry and frustrated about their work situation.
Discussion
The longstanding poor control of chronic diseases by despondent health care providers in CHCs evident from previous smaller studies3-5 is confirmed by the 1999 data. There was no improvement in the treatment of hypertension and diabetes, despite the institution of consensus-based guidelines for their management in public sector CHCs. These were publicised and widely disseminated by the Western Cape Department of Health in 1996. Patients were not actively involved in their own care and provision had to be made for large numbers of patients at the CHCs. The situation was severely strained because of limited resources and failure to plan for the large number of patients shifted from secondary and tertiary levels of care.
Successful treatment of people with hypertension, diabetes and other chronic diseases has many facets and requires a collaborative approach from all involved. In the final analysis, patients with chronic conditions self-manage their disease,13 with improved compliance leading to improved outcomes:14 'Patients are in control. No matter what we as health professionals do or say, patients are in control of these important self-management decisions. When patients leave the clinic or office, they can and do veto recommendations a health professional makes.'15 In contrast, patients with acute illnesses are treated without necessarily having to participate actively. The role of the patient and the health care system is emphasised: 'an effective chronic care model is achieved when a prepared, proactive practice team interacts with an informed, activated patient'.13
This study shows that the people who attend public sector CHCs in Cape Town for treatment of hypertension and diabetes are not 'informed activated patients' and that health care provider inertia is rife. This finding should not be surprising given our political history, which demanded passivity of the poor and disenfranchised. The authoritarian style of health care providers and the lack of culturally appropriate health-promotion tools to support patients in effective self-management contribute to this situation. An evaluation of the self-care patterns among white, black and coloured South Africans found marked culturally linked differences16 and concluded that a uniform self-care development programme for all South Africa's groups is not viable.
Guidelines for supporting self-management skills tailored to the cultural backgrounds of patients with chronic disease emphasise communication between relevant role players.17,18 Patient behaviours identified for long-term BP control for hypertension were that patients must: (i) personally decide to control their BP; (ii) take their medication as prescribed; (iii) monitor their progress towards their BP goal; and (iv) personally decide on actions to resolve the problems preventing achievement of BP control.19 Studying and understanding the knowledge base, skills, cultural understanding and attitudinal elements that underpin each of these required behaviours are essential,19 including the patient's perception of the psychological and logistic barriers to adherence to chronic disease care. Only then can participatory decision making programmes be developed to enhance self-care skills in patients. The development and implementation of culturally appropriate, effective patient self-care programmes for all South African groups are essential to improve health care delivery for patients with hypertension and diabetes.
CHCs with dedicated chronic disease clinics were closer to the proposed patient-centred approach and were run by trained nurse clinicians supported by an MO. Careful study of this model is needed so that it can be implemented at CHCs across the country. The role of trained community health workers linked to such clinics and patient empowerment initiatives, including examining the usefulness of CHC or community patient support groups, needs to be explored. Drug delivery systems ensuring the availability of chronic disease drugs at all times are required. Providing chronic drugs for only 1 month for stabilised patients should be re-examined as this results in unnecessary visits to CHCs with increased demands on nurses and pharmacists.
Although the quality of care received by patients with chronic conditions at primary health care level in 1999 was poor, the National Department of Health (NDOH) has made policy progress and established chronic disease care on the health agenda. National and provincial strategies and practical tools, such as essential drug lists and therapeutic guidelines for the care of patients with chronic conditions and their risk factors, have been formulated. The patient-centred approach for chronic disease care is central to the planning of the NDOH. Provincial departments of health must implement and operationalise health care for patients within their budgets. Data collected in 2005 on the treatment status of patients with hypertension at two CHCs in Cape Town still show deficiencies in that only 40% of the hypertension patients surveyed had a BP <140/90 mmHg. Many aspects of good hypertension care were still absent and overcrowding remains a problem.20
The Healthcare 2010 Plan of the Western Cape addresses many of the factors influencing poor chronic disease care (www.capegateway.gov.za). It emphasises the development of a previously non-existent community-based service delivery platform. Strengthening this level of service delivery should reduce pressure experienced at the primary health facilities. Although services at this platform will be rendered mainly by community health workers, they will be funded, trained and performance managed by managers based at district and sub-district offices of the health department. It is intended that empowering and supporting communities to take greater responsibility in the provision of their health needs will improve outcomes, particularly for those with chronic diseases. Furthermore, the Western Cape is formulating a strategic plan to address chronic diseases.
These proposed community-based platforms using trained community health workers to run support groups in the community for patients with chronic conditions in close collaboration with the health care providers based at the CHCs should improve the care for patients with chronic conditions. Furthermore, the pressure on the CHC-based health care providers and the health care provider inertia that was so prominent in 1999 will be reduced.
References
1. Holman H, Lorig K. Patients as partners in managing chronic disease. Partnership is a prerequisite for effective and efficient health care. Editorial. BMJ 2000; 320: 526-527. [ Links ]
2. Steyn K, Fourie J, Temple N, eds. Chronic Diseases of Lifestyle in South Africa: 1995 - 2005. Technical Report. Cape Town: South African Medical Research Council, 2006. [ Links ]
3. Steyn K, Fourie J, Lombard CJ, Katzenellenbogen JM, Bourne LT, Jooste P. Hypertension in the black community of the Cape Peninsula, South Africa. East Afr Med J 1996; 73: 758-763. [ Links ]
4. Levitt NS, Bradshaw D, Zwarenstein MF, Bawa AA, Maphumolo S. Audit of public sector primary diabetes care in Cape Town, South Africa: high prevalence of complications, uncontrolled hyperglycaemia, and hypertension. Diabet Med 1997; 14: 1073-1077. [ Links ]
5. Lunt DWR, Edwards PR, Steyn K, Lombard CJ, Fehrsen GS. Hypertension care at a Cape Town community health centre. S Afr Med J 1998; 88: 544-548. [ Links ]
6. WHO Collaborating Centre for Drugs Statistics Methodology. Anatomical Therapeutic Chemical (ATC) Classification Index with Defined Daily Doses (DDDs). Oslo: World Health Organization, 1998. [ Links ]
7. Executive Committee of the Hypertension Society of Southern Africa. Guidelines for the management of hypertension at the primary care level. S Afr Med J 1995; 85: 1321-1325. [ Links ]
8. Revised SEMDSA Guidelines for diagnosis and management of type 2 diabetes mellitus for primary health care in 2002. http://www.samdsa.org.za/files/dm2-guidelines.pdf (accessed 23 July 2007). [ Links ]
9. Breiman L, Friedman JH, Olshen RA, Stone CJ. Classification and Regression Trees. Belmont, Calif.: Wadsworth International Group, 1984. [ Links ]
10. Brown H, Prescott R. Applied Mixed Modeb in Medicine. 2nd ed. South Gate, Chichester: John Wiley, 2006. [ Links ]
11. Tesch R. In: Creswell JW, ed. Research Design: Qualitative and Quantitative Approaches. Thousand Oaks, Calif.: Sage, 1990: 154-155. [ Links ]
12. Strauss A, Corbin J. Basics of Qualitative Research: Grounded Theory Procedures and Techniques. Newbury Park, Calif.: Sage, 1990. [ Links ]
13. Bodenheimer T, Lorig K, Holman H, Grumbach. Patient self-management of chronic disease in primary care. JAMA 2002; 288: 2469-2475. [ Links ]
14. Maenpaa H, Heinonen OP, Manninen V. Medication compliance and serum lipid changes in the Helsinki Heart Study. Br J Clin Pharmacol 1991; 32: 409-415. [ Links ]
15. Glasgow RE, Anderson RM. In diabetes care, moving from compliance to adherence is not enough. Something entirely different is needed. Diabetes Care 1999; 22: 2090-2092. [ Links ]
16. Van Zyl-Schalekamp CJ. Preventive self-care in three Free State communities. Curationis 1991;14: 23-26. [ Links ]
17. Miller NH, Hill M, Kottke T, Ockene IS. The multilevel compliance challenge: recommendations for a call to action. A statement for healthcare professionals. Circulation 1997; 95: 1085-1090. [ Links ]
18. Working Group to define critical patient behaviors in high blood pressure control. Patient behavior for blood pressure control. Guidelines for professionals. JAMA 1979; 241: 2534-2537. [ Links ]
19. Epstein RM, Alper BS, Quill TE. Communicating evidence for participatory decision making. JAMA 2004; 291: 2359-2366. [ Links ]
20. Rayner B, Blockman M, Baines D, Trinder Y. A survey of hypertensive practices at two community health centres in Cape Town. S Afr Med J 2007; 97: 280-284. [ Links ]
 Correspondence:
Correspondence:
K Steyn
(krisela.steyn@mrc.ac.za)
Accepted 3 April 2008.














