Servicios Personalizados
Articulo
Indicadores
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares en Google
Similares en Google
Compartir
SAMJ: South African Medical Journal
versión On-line ISSN 2078-5135
versión impresa ISSN 0256-9574
SAMJ, S. Afr. med. j. vol.98 no.8 Pretoria ago. 2008
FORUM
SPORTS MEDICINE
Jim Peters' collapse in the 1954 Vancouver Empire Games marathon
Tim NoakesI; Jackie MeklerII; Dan Tunstall PedoeIII
IDiscovery Health Professor of Exercise and Sports Science at the University of Cape Town. A runner for 40 years, he has a special interest in the history of marathon running and the medical complications of the sport. For his work that established the cause of exercise-associated hyponatraemic encephalopathy, he was chosen in 2006 as one of the 40 most important 'persons or events' in the past 40 years of running
IISouth African ultra-marathon running, having won the 90 km Comrades Marathon 5 times besides setting a series of world ultramarathon running records in the 1950s and 1960s
IIIFormer competitive mile runner, is a London-based physician who has served as Medical Director of the London Marathon since its inception in 1981
ABSTRACT
On 7 August 1954, the world 42 km marathon record holder, Jim Peters, collapsed repeatedly during the final 385 metres of the British Empire and Commonwealth Games marathon held in Vancouver, Canada. It has been assumed that Peters collapsed from heatstroke because he ran too fast and did not drink during the race, which was held in windless, cloudless conditions with a dry-bulb temperature of 28°C.
Hospital records made available to us indicate that Peters might not have suffered from exertional heatstroke, which classically produces a rectal temperature >42°C, cerebral effects and, usually, a fatal outcome without vigorous active cooling. Although Peters was unconscious on admission to hospital approximately 60 minutes after he was removed from the race, his rectal temperature was 39.4°C and he recovered fully, even though he was managed conservatively and not actively cooled.
We propose that Peters' collapse was more likely due to a combination of hyperthermia-induced fatigue which caused him to stop running; exercise-associated postural hypotension as a result of a low peripheral vascular resistance immediately he stopped running; and combined cerebral effects of hyperthermia, hypertonic hypernatraemia associated with dehydration, and perhaps undiagnosed hypoglycaemia. But none of these conditions should cause prolonged unconsciousness, raising the possibility that Peters might have suffered from a transient encephalopathy, the exact nature of which is not understood.
Two of the most dramatic moments in athletics history occurred within minutes of each other in 1954 at the British Empire and Commonwealth Games in Vancouver, Canada. First, Roger Bannister of England and Australian John Landy completed the 'Mile of the Century'. Later, the English world record holder in the 42 km marathon, Jim Peters, collapsed repeatedly during the final 385 m of the marathon race which he had led from the start. A medical bulletin from Shaughnessy Hospital, Vancouver, informed the world that he was close to death.
From some of Peters' medical records from Professor R B Kerr, Head of the Department of Medicine, University of British Columbia, we now attempt to answer the questions:
- Why did Peters collapse?
- Did he develop heatstroke?
- If not, what explanations are there for his collapse?
- What relevance has this for the care of marathon runners more than 50 years later?
The 1954 Empire Games marathon
The 42 km marathon footrace began at 12h30 on 7 August 1954. Each entrant was required to pass a medical examination on the morning of the race.
From the start, the 35-year-old (55 kg, 1.68 m) Peters ran with his compatriot Stanley Ernest Walker Cox and Scotsman Joseph McGhee.1 Co-author Jackie Mekler (JM) recalls that the course travelled through suburban areas before continuing through industrial blocks. Conditions were hot (28°C), cloudless and windless. At 14.5 km, Peters increased his pace and, by 16 km (reached in 55 minutes), he led Cox by 300 m. This pace would have resulted in a sub-2 hour 20 minutes marathon time - 3 minutes slower than his world record set 42 days earlier. After 20 km, Peters' lead over Cox was still 300 m. He increased his pace. At the final aid station at 41 km, Peters '... still thought that Stan was close behind',2 though his lead was more than 5 km. Peters ran up the hill leading to the stadium, entering over a steep ramp which then descended to the stadium track.
He had been running for about 2 h 22 min. Peters reports that as he ascended the ramp, he 'wobbled a bit'2 and felt giddy. He fell as he reached the track 350 m from the finish: 'I just couldn't understand what had happened. For a moment, I was completely bewildered.' He made up his mind to finish as he did not want to disgrace his wife and kids.2 One onlooker described Peters' appearance: 'His glassy eyes stared straight ahead and his mouth hung open.' Another wrote: 'I've never seen such a ghastly look in any face except on those of wounded or dying men in battle.' A physician at the trackside reportedly said that Peters' face'... looked like a dead man's'.
The hospital discharge letter stated: '[Peters] believes that he was in good condition until about one-half mile from the Stadium, when he became very tired but was able to continue, with no mental or visual disturbance at that time. He recalls entering the Stadium and being aware of his surroundings, when suddenly he found that he had fallen. He vaguely recalls getting to his feet again and then falling on several occasions. His vision was blurred, and he recalls making a final effort and blacking out. He recalls a brief period in the ambulance but remembers nothing further until about two or three hours after admission to hospital.'
Peters collapsed repeatedly while covering the first 200 m of the Stadium track (Fig. 1). He lay down for 5 or more minutes in the shade in front of the grandstand. Partially recovered, he set off to complete the final 180 m. A film clip in a BBC interview 14 years later shows Peters striding resolutely albeit with a marked lean to his right, just 140 m from the finish. At that point, the British team physiotherapist, Mickey Mayes, strode purposefully onto the track, grabbed Peters around the waist, and stopped his further progress. Peters recalled Mayes saying: 'Well done, Jim', then lost consciousness. He was carried to the medical facility at the track.

When interviewed, Peters defended his previous statement: 'They should have let me go on. I could have finished if they had just let me go round the corner', adding 'I was very fit and very determined and I knew that I hadn't broken the tape'. He thought that Mayes removed him from the race because '... he was convinced that I had crossed the finish line ... I honestly believe that when he did it, he thought that I had won the race'.2
Clinical examination found that Peters was semi-conscious and unaware of his surroundings. He was throwing his arms about and groaning. He was pale but not cyanosed, and hyperventilating; his skin was warm and he was sweating profusely; pulse 55 - 60, regular and of good volume. He coughed up thick tenacious sputum. He was given 200 ml of a sugar-containing drink and oxygen by mask which he removed. Peters recalls that he regained consciousness for a short time, asking an attending nurse: 'Did I win?' She replied with a smile, 'You did very well.'2 Peters was transferred by ambulance to the Shaughnessy Hospital at approximately 16h00, about 68 minutes after he first collapsed. In the ambulance, Peters continued to sweat profusely but his pulse became 'thready and irregular' and he appeared 'somewhat cyanotic'.
Additional clinical findings on hospital admission were that his eyes were sunken and his tongue was dry; his pulse was a regular 110 - 120; blood pressure 110/55 mmHg; rectal temperature 39.4°C; a grade II systolic murmur was heard at the cardiac apex; and reflexes were absent in the lower limbs but the plantar reflexes were normal (flexor). He vomited a small volume of fluid and passed a large, watery stool.
Of note in the laboratory findings were the marked hypernatraemia (serum [Na+]=152 mmol/l) and the raised haemoglobin concentration (17.7 g/dl). The white cell count was also increased (19 500/106) but the serum potassium concentration was normal (3.8 mmol/l). Over the next 12 hours, he received intravenously 1.8 l of 5% glucose in 0.9% saline.
At 18h00, Peters regained consciousness and responded to questions; his pulse rate had fallen and systolic blood pressure increased to 120 mmHg. By 19h30 he was fully conscious and rational but extremely thirsty. He had no headache, chest or abdominal pain or leg muscle cramps. He passed 3 loose bowel movements and vomited twice. His pulse rate had slowed further and his rectal temperature was normal (37.8°C). An adventitious diastolic sound was heard along the left sternal border of the chest, the nature of which was not determined, and it had disappeared 2 hours later. By the following morning, his serum sodium concentration (140 mmol/l), haemoglobin (14.0 g/dl) and haematocrit (44%) were all normal, and his white cell count was lower (16 650/106). Over the next few days, Peters continued to improve after initially experiencing tiredness, headaches, nausea, vomiting and liquid bowel movements. He was discharged from hospital, clinically recovered.
Interviewed on his discharge, Peters stated that, as was his usual practice,3 he had not ingested any fluid, salt or glucose during the race. This was only the second time he had not finished a marathon race; in the 1952 Olympic Games marathon in Helsinki, he had retired at 32 km with severe left leg cramps. He had commonly experienced symptoms of nausea, vomiting and diarrhoea for 12 - 24 hours after a marathon race. This time, the symptoms persisted for longer.
Professor Kerr concluded: 'It was felt that he had suffered a severe exhaustion. The fact that his temperature was elevated, suggested some factor of heatstroke. Whether marked hypoglycaemia was present, is not known. The changes in the electrocardiograms have presented considerable problems of interpretation. It has not been felt that a definite infarction occurred (there has been no other corroborative evidence). However, it is considered that some myocardial changes have taken place - metabolic, electrolytic or otherwise - which have been responsible for the nonspecific changing electrocardiographic picture. It is suggested that it is most important for him to be under medical supervision in order to determine if he can continue competitive running.'
In a letter dated 11 September 1954 to (Sir) Roger Bannister, Sir (Dr) Adolphe Abrahams, author of an early British textbook of sports medicine, wrote: 'I am greatly obliged for the notes sent on Peters from which several interesting features emerge.
1. It appears pretty clear that his appearance gave an impression of a much more distressed and serious condition than his subjective sensation. This is the usual experience of all distressed athletes especially after intense rather than sustained efforts; the appearance is extremely alarming to the on-lookers.
2. It is quite evident that salt depletion played no part.
3. Nor hypoglycaemia, if one may judge from the report that a drink with sugar immediately administered led to no improvement. I should have been surprised if hypoglycaemia had been identified (despite the Americans).
4. There appears to have been considerable variations in his pulse rate and character. One would have preferred cardiac revelations as to the frequency, correlated with the pulse. Moreover, I presume the observations are not all by the same man so their value and validity are dubious. I do not attach any importance to ECG findings. Queer conditions may occur in any athlete after exercise. And why should an infarct occur or indeed why impinge the heart at all?
5. The condition was that of Heat Exhaustion.'
The attending physician, Dr R B Kerr, did not offer a specific diagnosis other than 'severe exhaustion', without any definite evidence for heart damage.
Discussion
The differential diagnosis for collapse with loss of consciousness of a previously healthy athlete during or immediately after a marathon race includes:
1. Latent medical conditions unrelated to exercise that may occur more frequently during prolonged exercise of moderate to high intensity. Such conditions (including cardiac arrest, myocardial infarction or a cerebrovascular accident) can be ruled out by the clinical evidence. Although the electrocardiogram (Fig. 2) was unusual, the changes were nonspecific.
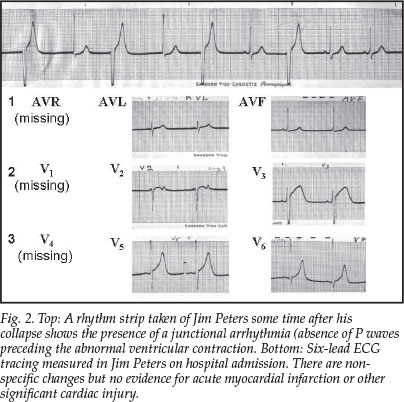
2. Conditions specific to prolonged exercise include heatstroke, hypoglycaemia, hypernatraemia associated with a reduction in total body water, postural hypotension, or exercise-associated hyponatraemia (EAH) associated with an increase in total body water.4,5 The elevated serum sodium concentration excludes a diagnosis of EAH. Hypoglycaemia can be excluded as it is not associated with prolonged loss of consciousness in athletes. Other possibilities in order of decreasing probability are:
Exertional heatstroke
Peters' collapse is highly suggestive of heatstroke as then understood - 'a combination of impaired consciousness and a temperature of over 41°C must be treated as heat stroke until the diagnosis is disproved'.6 He was unconscious for some time during the first 4 hours after his collapse. The race was run in warm (28°C), windless, cloudless conditions, considered conducive to the development of heatstroke. Peters had not trained to race in the heat as the value of heat acclimatisation was not then appreciated. Only in 1964 did an American runner resident in England pre-adapt himself by training in the cool English conditions while wearing several layers of clothing.3
Factors that are not usually found in patients with exertional heatstroke included that Peters' rectal temperature, when first measured approximately 68 minutes after he collapsed, was 39.4°C. This is within the normal range in healthy, fully conscious runners completing long-distance races in equivalent or warmer conditions.7-9 Heatstroke is usually associated with rectal temperatures in excess of 42°C.10
Even if Peters' temperature had been >42°C at the time he collapsed, it is unusual for the temperature to fall without active cooling, as the rectal temperature in true heatstroke remains elevated until death or active cooling intervenes,10 perhaps as a result of a continuing hypermetabolic state.11,12 Spontaneous cooling probably resulted from the absence of a hypermetabolic state and his continued sweating during recovery.
Peters' choice not to drink has also been used as anecdotal 'proof' that he must have developed heatstroke, based on the theory that dehydration impairs sweating, leading to heatstroke.7 Yet the South African athletes in the race who finished second (JM) and third (Jan Barnard) also did not drink much, other than a few sips of lemon squash mixed with glucose and salt. Levels of dehydration even in excess of 4% of body weight do not reduce the capacity to lose heat by sweating.3 The extent to which athletes drink during exercise does not predict their post-exercise rectal temperatures13 nor, apparently, their risk of developing heatstroke, since most heatstroke cases occur in subjects who have not exercised sufficiently to develop marked levels of 'dehydration (>8 -10%).14 Similarly, clinically important dehydration is present in only about 35% of patients with classic heatstroke,15 suggesting that dehydration is often associated with heatstroke but is not necessarily causal.
Furthermore, the environmental conditions during the race were not exceptionally hot by the standards of the 1950s or indeed today. JM recalls running marathon races starting at 13h00 in temperatures of 32°C in South Africa and England in those years.
The use of conventional equations16 shows that heatstroke can occur in conditions in which the rate of heat production is not sufficient to explain the measured core temperature at the time of collapse.11 These calculations (Table I) show that if the humidity during the Vancouver marathon had been 80%, Peters would have been unable to achieve thermal balance during the race and would have finished with a core temperature of ~41.4°C. Had the humidity been less, he would have achieved thermal balance, finishing with a core temperature closer to 39 - 40°C. It seems improbable that the humidity was 80%.
Exercise-associated postural hypotension with hyperthermic and hypernatraemic encephalopathy
Exercise performance in the heat is regulated by a complex, intelligent system that ensures that excessive heat accumulation does not occur and lead to heatstroke.17 Consequently, athletes usually alter their behaviour and run slower in the heat (as did the other leading runners) (Table II). As these control mechanisms should prevent the development of heatstroke, Peters' altered state of consciousness might have been caused by something other than heatstroke.
A sufficiently high core temperature will cause the onset of walking or termination of exercise. Postural hypotension could have developed once Peters stopped running.18 His low heart rate at the time of his collapse is compatible with a state of increased parasympathetic activity and maximally stimulated sympathetic tone that cannot increase further to prevent the development of orthostatic hypotension. Profound hypotension would explain why Peters' face looked 'like a dead man's' at the finish.
If postural hypotension had been Peters' main complaint, lying supine in the shade for a few minutes might have allowed a partial recovery. Abruptly stopping him once he resumed running would have re-activated the postural hypotension, perhaps sufficiently to lose consciousness. But if this were the sole explanation, Peters should have recovered consciousness as soon as he again lay supine. Therefore, other factors must have caused his continued state of unconsciousness.
The unusual gait adopted by Peters has been filmed more recently in at least 3 athletes at the finish line of the 242 km Hawaiian Ironman Triathlon. All athletes were conscious and none suffered from heatstroke. This behaviour suggests that there is a form of transient exercise-related encephalopathy not yet properly understood.
In the absence of a proven cause, we propose that the combined effects of a moderately severe hyperthermia (perhaps ~41.5OC), hypertonic hypernatraemia caused by reduced total body water content and which delays post-exercise recovery,19 associated with a possible hypoglycaemia, might have combined to cause a transient encephalopathy in Peters. However, this conclusion is speculative and hence ultimately unsatisfactory.
We gratefully acknowledge the assistance of Sir Roger Bannister in particular by providing access to the late Professor Kerr's case notes and the letter from the late Sir Adolphe Abrahams. The first author's research was funded by the University of Cape Town, the Medical Research Council of South Africa, Discovery Health Pty Ltd and the National Research Foundation through the Technology and Human Resources for Industry Programme (THRIP) initiative.
1. Martin DE, Gynn RWH. The Marathon Footrace. Springfield, Ill.: Charles C Thomas, 1979. [ Links ]
2. Peters JH, Johnston J. In the Long Run. London: Cassell, 1955. [ Links ]
3. Noakes TD. Lore of Running. Champaign, Ill.: Human Kinetics Publishers, 2003. [ Links ]
4. Holtzhausen LM, Noakes TD. Collapsed ultraendurance athlete: proposed mechanisms and an approach to management. Clin J Sport Med 1997; 7: 292-301. [ Links ]
5. Noakes TD, Sharwood K, Speedy D, et al. Three independent biological mechanisms cause exercise-associated hyponatremia: evidence from 2,135 weighed competitive athletic performances. Proc Natl Acad Sci USA 2005; 102: 18550-18555. [ Links ]
6. Williams JGP, Sperryn PN. Sports Medicine. London: Edward Arnold, 1976. [ Links ]
7. Wyndham CH, Strydom NB. The danger of an inadequate water intake during marathon running. S Afr Med J 1969; 43: 893-896. [ Links ]
8. Pugh LG, Corbett JL, Johnson RH. Rectal temperatures, weight losses, and sweat rates in marathon running. J Appl Physiol 1967; 23: 347-352. [ Links ]
9. Buskirk ER, Beetham WPJ. Dehydration and body temperature as a result of marathon running. Medicina Sportiva 1960; XIV: 493-506. [ Links ]
10. Roberts WO. Exertional heat stroke during a cool weather marathon: a case study. Med Sci Sports Exerc 2006; 38: 1197-1203. [ Links ]
11. Rae DE, Swart J, Knobel GJ, Mann T, Tucker R, Noakes TD. Heatstroke during endurance exercise: Is there evidence for excessive endothermy? Med Sci Sports Exerc 2008 (in press). [ Links ]
12. Broessner G, Beer R, Franz G, et al. Case report: severe heat stroke with multiple organ dysfunction - a novel intravascular treatment approach. Crit Care 2005; 9: R498-R501. [ Links ]
13. Noakes TD. Study findings challenge core components of a current model of exercise thermoregulation. Med Sci Sports Exerc 2007; 39: 742-743. [ Links ]
14. Kark JA, Burr PQ, Wenger CB, Gastaldo E, Gardner JW. Exertional heat illness in Marine Corps recruit training. Aviat Space Environ Med 1996; 67: 354-360. [ Links ]
15. Seraj MA, Channa AB, al Harthi SS, Khan FM, Zafrullah A, Samarkandi AH. Are heat stroke patients fluid depleted? Importance of monitoring central venous pressure as a simple guideline for fluid therapy. Resuscitation 1991; 21: 33-39. [ Links ]
16. Brotherhood JR. Heat stress and strain in exercise and sport. J Sci Med Sport 2008; 11: 6-19. [ Links ]
17. Tucker R, Marle T, Lambert EV, Noakes TD. The rate of heat storage mediates an anticipatory reduction in exercise intensity during cycling at a fixed rating of perceived exertion. J Physiol 2006; 574: 905-915. [ Links ]
18. Noakes TD. Reduced peripheral resistance and other factors in marathon collapse. Sports Med 2007; 37: 382-385. [ Links ]
19. Hew-Butler T, Sharwood K, Boulter J, et al. Dysnatremia predicts a delayed recovery in collapsed ultramarathon runners. Clin J Sport Med 2007; 17: 289-296. [ Links ]
 Correspondence:
Correspondence:
T Noakes
(timothy.noakes@uct.ac.za)














