Services on Demand
Article
Indicators
Related links
-
 Cited by Google
Cited by Google -
 Similars in Google
Similars in Google
Share
SAMJ: South African Medical Journal
On-line version ISSN 2078-5135
Print version ISSN 0256-9574
SAMJ, S. Afr. med. j. vol.98 n.7 Pretoria Jul. 2008
SAMJ
REVIEW
The South African Bone Marrow Registry (SABMR) and allogeneic bone marrow transplantation
Paul RuffI; Terry SchlaphoffII; Ernette du ToitIII; Anthon HeynsIV
IPaul Ruff is Professor and Head of Medical Oncology, University of the Witwatersrand Faculty of Health Sciences and Donald Gordon Medical Centre, Johannesburg, and a member of the SABMR Board
IITerry Schlaphoff is Chief Medical Technologist at the Laboratory for Tissue Immunology, National Health Laboratory Service (NHLS), Cape Town, and Deputy Director of the SABMR
IIIErnette du Toit is Emeritus Associate Professor of Immunology, University of Cape Town, Head of the Laboratory for Tissue Immunology, NHLS, Cape Town, and Medical Director of the SABMR
IVAnthon Heyns is Chairman of the SABMR and Programme Director of the SA National Blood Service PEPFAR programme on blood safety
In 1939 Osgood et al.1 reported infusing bone marrow into patients with severe aplastic anaemia without any clinical benefit. Rekers and Coulter2 attempted to reconstitute marrow function in irradiated dogs by marrow infusions. Both failed because of insufficient irradiation to produce immunosuppression necessary for engraftment. In 1957 Donnall Thomas and co-workers3 showed that marrow can be collected, stored in significant quantities and safely administered. Marrow transplants remained unsuccessful, however, although patients with refractory leukaemia given supralethal irradiation recovered after marrow infusion from identical twins.4 Allogeneic marrow transplants usually resulted in failed engraftment, or engraftment followed by lethal graft-versus-host disease (GVHD). Further discoveries were the HLA complex and transplantation antigens,5 and that successful allogeneic engrafting depends upon donor/recipient histocompatibility.6
These studies pointed the way for human marrow grafting using HLA-matched sibling donors. Thomas et al.4 showed that it was possible to cure leukaemia, aplastic anaemia, thalassaemia and inherited marrow disorders using a histocompatible sibling donor. The finding that methotrexate and subsequent immunosuppressive agents such as azathioprine, cyclosporine and tacrolimus, reduced GVHD as well as graft failure, improved results of marrow transplantation.
Haematopoietic growth factors
The discovery of haematopoietic growth factors, granulocyte-colony-stimulating factor (G-CSF) and granulocyte-macrophage-colony-stimulating factor (GM-CSF) in the 1980s had a major impact on marrow transplantation. CSFs stimulate haematopoietic progenitor cells, permitting rapid proliferation and repopulation of marrow by engrafted cells.7 Recombinant DNA technology enabled CSFs to be synthesised for clinical use.
The physiological effect of G-CSF in mobilisation of haematopoietic stem cells into peripheral blood enabled peripheral blood stem cell harvesting to replace marrow harvesting to obtain stem cells. A cell separator harvests stem cells from peripheral blood, obviating general anaesthesia to aspirate marrow. Donors are given a 5-day course of 5 - 10 µg/ kg subcutaneous G-CSF before the stem cells are harvested. It takes 4 - 6 hours to obtain sufficient cells for the infusion.
Graft-versus-host disease
Although some early transplants were successful, problems occurred due to graft failure, rejection and acute GVHD. Some patients receiving marrow from siblings developed a potentially fatal syndrome of an erythematous desquamating rash, watery diarrhoea and jaundice.
The most successful transplants, with minimal rejection and GVHD, are between identical twins, i.e. syngeneic transplantation.
Immunosuppressive agents
Immunosuppression, first developed in renal transplantation, was then applied to marrow transplantation. Immunosuppressive agents included azathioprine, cyclosporine, antithymocyte globulin, antilymphocyte globulin and later tacrolimus, antiCD25 (T-cell receptor) monoclonal antibodies basiliximab and dacluzumab, and mTOR (mammalian target of rapamycin) inhibitors, sirolimus and everolimus.
Murine anti-CD52 monoclonal antibody, Campath-1G, when added to the harvested stem cells bag, removes almost all lymphoid cells, limiting GVHD although increasing the risk of leukaemia relapse. Humanised anti-CD52 monoclonal antibody, alemtuzumab, used intravenously before infusing stem cells, reduces murine protein anaphylactic reactions and the development of human anti-mouse antibodies (HAMA).8
Graft-versus-leukaemia effect
A major reason for success of allogeneic transplantation in myeloid and possible lymphoid malignancies was the suppressant effect of donor T lymphocytes and NK cells on the underlying malignancy. This graft-versus-leukaemia (GVL) effect has to be balanced against the risk of GVHD. Mild GVHD with GVL is ideal, whereas severe GVHD is undesirable. Patients receiving T-cell-depleted stem cells or syngeneic transplantation have a higher risk of relapse of their underlying disease.9
Lack of sibling donors
As donors for an allogeneic stem cell transplant require an exact HLA Class I (A, B, C) and Class II (DR, DQ) match with the recipient, most patients requiring transplantation do not have a readily available donor. Siblings are the usual source of donors, being the only available matched family members. Today, with smaller families, only about 10% of patients have an HLA-matched donor. There is a 5% chance of finding a suitable donor in the extended family, e.g. cousins. Transplantation with 1-locus or even 2-loci mismatches from a family donor can be performed, but the risks of graft failure and GVHD increase. Haplo-identical transplants from parents to children play a role when no donor is available but are risky.
Owing to this lack of donors, and the expansion of allogeneic stem cell transplantation in malignant and non-malignant diseases, an alternative source of donors had to be found.
Matched-unrelated-donor stem cell donors
Two alternative non-family sources of stem cells are now used, namely matched unrelated donor (MUD) transplants and umbilical cord blood transplants.10
MUD registries have grown in most developed countries. Racially homogenous societies such as Scandinavia lend themselves best to such registries, as HLA genes are largely ethnically based. Most European registries have donors of Caucasian origin, making access to donors of Asian and African origin difficult to obtain. The ethnically diverse population of the USA is the best source of donors throughout the world, but high costs and strict National Marrow Donor Program (NMDP) regulations limit international access to US donors. The NMDP has developed a network of co-operative registries as an alternative form of access to donors. In August 2006 South Africa signed a co-operative agreement between the NMDP and the South African Bone Marrow Registry (SABMR).
Donor registries co-operate and their linked databases enable patients to have access to donors worldwide. At the time of writing in December 2007 there were 59 stem cell registries and 40 cord blood registries worldwide with access to 12.02 million registered donors.
Umbilical cord blood transplantation
Umbilical cord blood, the other alternative source of stem cells, is useful for children and for small adults (under 50 kg) and furthermore requires a less stringent HLA match. Stored umbilical cord blood does not rely on donor presence and current good health. Once cord blood has been shown to be HIV, hepatitis B and C virus-free, the donor is guaranteed. Living MUDs may change their minds, move town, die or seroconvert. The HIV epidemic, limited resources and lack of government support have resulted in few moves to develop umbilical cord banking in South Africa.
Bone marrow transplantation in South Africa
Bone marrow transplantation in South Africa was developed at the University of Cape Town from the mid-1970s, and the University of the Witwatersrand in the 1980s.
South African Bone Marrow Registry (SABMR)
The SABMR was started at University of Cape Town by Professor Ernette du Toit with help from Professor Peter Jacobs in early 1990s. It is a non-profit organisation (Reg. No. 004-300 NPO) that co-ordinates the provision of matched unrelated stem cell donors for South Africa, and is the contact for countries seeking unrelated donors in South Africa.
The SABMR was established in the Laboratory for Tissue Immunology (LTI) in Cape Town. This was an extension of the LTI functions, which was initially HLA typing for organ transplantation since Chris Barnard's first heart transplants in 1960s. The European Federation for Immunogenetics accredited the LTI as an HLA-typing centre for unrelated marrow transplantation in 1999.
The first donors were recruited in 1991. By May 1992 there were 210 donors on the registry, and by 1993 there were 534, of which 482 were HLA-ABDR typed. Owing to lack of funding and donor awareness, the SABMR grew more slowly for the next 7 years. Donor awareness was increased with the help of the Natal Blood Transfusion Service (NBTS) and two donor funding organisations, the Darren Serebro Foundation in Gauteng and the Sunflower Fund in Western Cape. The Darren Serebro Foundation, which started in August 1998, recruited over 20 000 donors, mainly in Gauteng. The Sunflower Fund formed in 1999 was inspired by the struggles of Chris Corlett and Darren Serebro against leukaemia. The aim of the two organisations is to rally financial support to increase the number of stem cell donors in South Africa. The Sunflower Fund now has the national responsibility for raising funds for tissue typing of unrelated donors, which had resulted in an increase in the SABMR donor database size to 63 123 by December 2007 (Fig. 1).
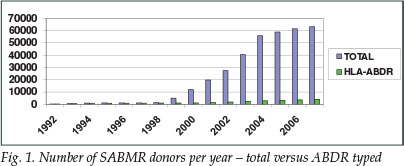
In the worldwide database of over 12 million, 70% are HLA-ABDR typed. Unfortunately only 6% of the potential SABMR donors have been HLA-DR typed (Fig. 1). This deficiency is now being addressed by the SABMR.
Lack of black donors makes MUD transplantation problematic in South Africa, with very few recipients of African origin. This problem is exacerbated by the lack of donors of African origin on European registries available to South African patients. The NMDP is a potential source of donors of African origin, although African-Americans are mainly of West African origin with different HLA typing frequencies to southern African blacks.
Following the recruitment of the first donors, the World Marrow Donor Association (WMDA) recognised the SABMR as the HUB centre for South Africa in September 1991. The WMDA is a voluntary organisation of representatives of blood stem cell donor registries, cord blood banks, other organisations and individuals with an interest in haematopoietic stem cell transplantation. It provides a forum for discussion of issues regarding the clinical use of haematopoietic stem cells from unrelated donors across international boundaries and for formulation of guidelines on logistics, quality control, ethics, finances, information technology and registry accreditation.
Bone Marrow Donors Worldwide (BMDW) situated in Leiden, The Netherlands, is a voluntary collaborative effort of stem cell donor registries. BMDW collates donor information worldwide. This database contains details of over 12 million donors, including more than 63 000 from South Africa, and is available online to all participating registries. This allows all registries to search for donors when there is no local donor available.
Matched unrelated donor transplants in South Africa
The first MUD transplant in South Africa was performed at the now University of the Witwatersrand Donald Gordon Medical Centre in Johannesburg in June 1997. Bone marrow was harvested in Belgium and flown to Johannesburg. In 1999 the first SABMR donor provided peripheral blood stem cells to a South African patient. In 2003 the first black South African donor provided stem cells for an unrelated patient and the first unrelated cord blood transplant was performed. At the time of writing, a total of 125 patients had received first MUD transplants in Gauteng and the Western Cape (Fig. 2). Of the donors 32 were from the SABMR and 93 from international registries, mainly in Europe (of the latter 6 were cord bloods). In addition 7 SABMR donors supplied stem cells to patients in Germany, Italy, Portugal, The Netherlands, the UK and the USA.

Conclusions
Allogeneic bone marrow and now peripheral blood stem cell transplantation has become an important treatment of haematological malignancies, first acute and chronic myeloid leukaemia and now myelodysplasia, lymphomas and even multiple myeloma. Its role in chronic myeloid leukaemia has diminished considerably since the advent of imatinib.11 It also plays an important role in non-malignant haematological diseases, first aplastic anaemia and now haemoglobinopathies, thalassaemias and storage diseases.
Modern tissue typing and immunosuppression, and better supportive care including newer antibiotics, antifungal and antiviral agents, have reduced mortality and morbidity.
Alternative sources of stem cells, including MUD and umbilical cord blood transplantation, have widened the availability of donors throughout the world. The growth and development of the SABMR is essential in our quest for donors, especially for patients of black African origin, and needs support from the public, donor funds, universities, private corporations and the government.
1. Osgood EE, Riddle MC, Mathews TJ. Aplastic anaemia treated with daily transfusions and intravenous marrow. Ann Intern Med 1939; 13: 357-367. [ Links ]
2. Rekers PE, Coulter M. A hematological and histological study of the bone marrow and peripheral blood in an adult dog. Am J Med Sci 1948; 216(6): 643-655. [ Links ]
3. Thomas ED, Lochte HL, Lu WC, Ferrebee JW. Intravenous infusion of bone marrow in patients receiving radiation and chemotherapy. N Engl J Med 1957; 257(11): 491-496. [ Links ]
4. Thomas ED, Lochte HL, Cannon JH, Sahler OD, Ferrebee JW. Supralethal whole body irradiation and isologous marrow transplantation in man. J Clin Invest 1959; 38: 1709-1716. [ Links ]
5. Dausset J, Contu L. MHC in general biological recognition: its theoretical implications in transplantation. Transplant Proc 1981; 13: 895-899. [ Links ]
6. Sorb R, Rudolph RH, Thomas ED. Marrow grafts between canine siblings matched by serotyping and mixed leucocyte culture. J Clin Invest 1971; 50: 1272-1275. [ Links ]
7. Ahmed T, Wuest D, Ciavarella D. Peripheral blood stem cell mobilization by cytokines. J Clin Apher 1992; 7(3): 129-131. [ Links ]
8. Hale G, Jacobs P, Wood L, et al. CD52 antibodies for prevention of graft versus host disease and graft rejection following transplantation of allogeneic peripheral blood stem cells. Bone Marrow Transplant 2000; 26(1): 69-76. [ Links ]
9. Weiden PL, Flournoy N, Thomas ED, et al. Antileukemic effect of graft versus host disease in human recipients of allogeneic marrow grafts. N Engl J Med 1979; 300(19): 1068-1073. [ Links ]
10. Hows J, McKinnon S, Brookes P, et al. Matched unrelated donor transplantation. Transplant Proc 1989; 29(1): 2923-2925. [ Links ]
11. O'Brien SG, Guilhot F, Larson RA, et al. Imatinib compared with interferon and low-dose cytarabine for newly diagnosed chronic-phase chronic myeloid leukemia. N Engl J Med 2003; 348(11): 994-1004. [ Links ]
 Correspondence:
Correspondence:
P Ruff
(paul.ruff@wits.ac.za)
Members of the Board of the SABMR: A Block, R Crookes, E du Toit, A Heyns, P Jacobs, V Jogessar, M Kganakga, C Kotzenberg, J Mahlangu, N Novitzky, P Ruff, T Schlaphoff, A Wadee.














