Services on Demand
Article
Indicators
Related links
-
 Cited by Google
Cited by Google -
 Similars in Google
Similars in Google
Share
SAMJ: South African Medical Journal
On-line version ISSN 2078-5135
Print version ISSN 0256-9574
SAMJ, S. Afr. med. j. vol.98 n.7 Pretoria Jul. 2008
IZINDABA
Beleaguered hospitals - help at last?
After 2 years of advertising, the national health department finally has the legally required Director for its Inspectorate of Standards Compliance, a multi-skilled community health specialist and former exile with no illusions about her new ambit.
Dr Carol Marshall is a UCT graduate who spent 15 years in exile in Mozambique, returning to lecture at the University of the Witwatersrand (Wits) in 1991 before directing Gauteng's Mother and Child Health programme and later running the province's district hospital and health programmes.
She comes to the complex job of ensuring quality assurance and standards compliance by managers and staff of South Africa's 400 hospitals and community health centres after 5 years of managing programmes for an international nutrition NGO.
With quality assurance and standards compliance differing widely from province to province, within provinces themselves and even from hospital department to hospital department, her new job will be painstaking and methodical - with no quick fixes. Through close collaboration with other programmes, the Department aims to systematically address the underlying causes of headline-grabbing stories about deaths due to negligence and inefficiencies in state hospitals - and to identify best practices.
Creating a single beacon to follow
Already a lack of compliance with the national department's existing guidelines has been identified in the national and provincial complaints system, technology, nosocomial neonate infections, ICUs, queues and waiting times (especially pharmacies and outpatient departments), supervision of clinic staff, lab test turnaround times and management systems and processes.
'We have two objectives: identify and celebrate best practice and identify and sort out red-flag areas. It's not as if we're going out and saying these are the worst hospitals and checking up. We know those in the news - others may be a good deal worse. We also want to benchmark best practice - the point is we just won't know until we've gone through this staged appraisal process,' she said.
Marshall began by pulling together a team and doing an audit of current strategic plans of the national health department, including responses to controversial issues like MDR/XDR TB, nosocomial infections, and checking out her legal job description.
She plays her cards close to her chest when it comes to sharing initial impressions - deeply aware how critical a role her impartiality will play in setting up a successful game plan, and turns the focus firmly back on what she's setting out to do.
The outcome she's after is a single set of core national standards against which all establishments and services can benchmark themselves. The national health act puts the responsibility for compliance in establishing norms and standards squarely on the shoulders of the national health minister.
Enhancing accountability
Says Marshall: 'In the set of Core Standards for Health Establishments (launched by the Minister in April) we intend to pool together in a horizontal, comprehensive, summarised fashion, what the expectations are of facility managers - so we can integrate the health system with health requirements.'
Seven core domains had been identified for hospital management assessment. They are safety, clinical care, governance, patient perceptions and experience of care received, access to care, infrastructure environment and facilities management, health promotion and prevention, and public health.
The first phase will begin on 17 June this year, with teams of 4 - 8 (pre-trained) people doing a rapid appraisal of 27 individual hospitals and 4 community health clinics taking '2 or 3 provinces' at a time, using questionnaires. Their travel route will be dictated by geography, not high news profiles of hospitals.
While the questionnaires will be heavily weighted towards self-appraisal, 'we do have some tools to help us get to the bottom of things'. These would include verification of documents, the local facility's complaints register, adverse event reports, legal cases, hospital board minutes and even press reports.
'I'm sure there will be some valiant attempts to portray things as they aren't,' Marshall quipped. All targeted facilities should have been fully appraised by the middle of August this year. Each appraisal would be followed by a lengthy debriefing of the facility manager.
Separately, joint national/provincial 'improvement teams' will then use the debriefing summaries to work directly with facility management, implementing recommendations and developing improvement plans focusing on the most serious issues identified.
Marshall said that in contrast to the well-known quality assurance NGO, the Council for Health Service Accreditation of Southern Africa (COHSASA), against whom criticism had been levelled for 'being both referee and coach', the approach here was different.
Her teams were made up so that no single team assessing another province would have a member originating from that particular province. Reports from these teams would be presented to facility managers by their own line managers.
Come September this year, the Office of Standards Compliance would review overall norms and standards, the pre-appraisal process and the 'support to improvement plans'. This would be followed by an up-scaling and roll-out, covering more and more facilities.
Asked why the list of 27 hospitals and clinics included at least 9 that COHSASA is currently working with, Marshall replied: 'Don't you think it's a good idea for the national department to report on its own hospitals?' She said at 7 of the 27 hospitals CEOs were currently on departmental management programmes, 8 hospitals were part of the revitalisation programme (embracing infrastructure, management, quality and technology), 1 hospital had completed revitalisation and another would soon begin.
Not reinventing the wheel
Asked how her department would avoid duplication, she said one of 'the upfront questions' was to identify every other support project each facility had worked with over the 'past 3 or 4 years'. By identifying other programmes, the department would be able to integrate them into the implementation phase of the scheme. Most of those spoken to (for example a national injection safety programme) had agreed to help out wherever needed.
Her ideas for the future included working with the universities at Wits and KwaZulu-Natal that are currently running hospital management training programmes in order to 'beef up management' and the setting up of a technical reference group.
She was aware of adverse event studies being done at hospitals in the Free State, North West Province and Gauteng and her appraisal questionnaire also asked each hospital what was in place for reporting and responding to adverse events.
Asked about the human resource crisis, Marshall responded: 'Not everything found is necessarily within the authority or capacity of facility managers to resolve. Part of the process will be looking at contributory factors outside their capacity.' While her work included questions on 'whether staffing needs benchmarks, this is not something we can go into in detail'.
'I can't tell you how we'll resolve things because that's what this is about. Neither am I promising this will solve all problems all at once with some miraculous magic wand - this is about gathering evidence and acting on it.'
Marshall described her work as 'a key component of stewardship of national government. It's incredibly exciting. I think we in SA are at the stage where we're ready for this kind of thing. I've noticed education doing the same thing. We have to be able to appraise and audit our work.'
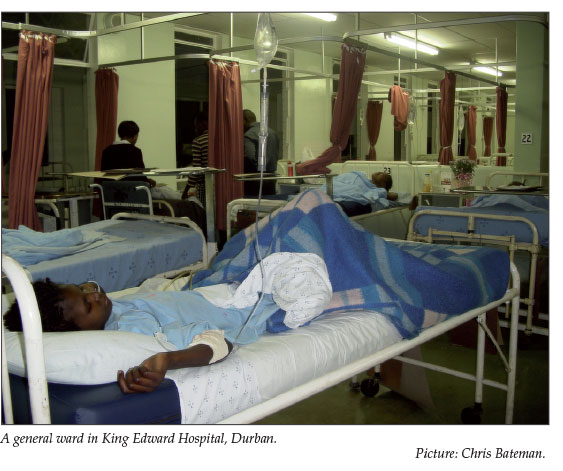
Chris Bateman














