Servicios Personalizados
Articulo
Indicadores
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares en Google
Similares en Google
Compartir
SAMJ: South African Medical Journal
versión On-line ISSN 2078-5135
versión impresa ISSN 0256-9574
SAMJ, S. Afr. med. j. vol.98 no.5 Pretoria may. 2008
ORIGINAL ARTICLES
A contrast-enhanced ultrasound study of benign and malignant breast tissue
Serita BarnardI; Timothy CookeII; Wilson AngersonIII; Edward LeenIV
IMB ChB, MRCS; Department of Surgery, Glasgow Royal Infirmary, UK
IIMB ChB, FRCS; Department of Surgery, Glasgow Royal Infirmary, UK
IIIPhD (Stats); Department of Surgery, Glasgow Royal Infirmary, UK
IVMD, FRCR; Department of Radiology, Glasgow Royal Infirmary
ABSTRACT
OBJECTIVE:. To determine the diagnostic value of haemodynamic contrast-enhanced ultrasound assessment in benign and malignant breast tissue, using histological examination as the reference standard.
METHODS: An HDI 5000 Phillips ultrasound scanner with microvascular imaging software and 2.5 ml SonoVue (Bracco spa, Milan) contrast was used to scan 50 consecutive patients (32 malignant and 18 benign, 49 with histologically confirmed breast lesions). Time-intensity curves of the regions of interest (ROI) placed over the lesional and normal breast tissues were acquired using QLAB software. The area under the curve (AUC), time to peak (TTP), in-flow gradient (IFG) and peak enhancement (PE) were determined in a standardised manner for each focal breast lesion and the control/normal breast. IFG and AUC in the periphery, and PE and AUC in the centre of the lesions, differed significantly between malignant and benign tumours. In a logistical regression model, AUC in the periphery and the ratio of PE at the tumour centre to that of normal breast were independently predictive of malignancy (p<0.001), achieving a diagnostic sensitivity of 97% and a specificity of 80% in the 41 tumours in which central vessels could be distinguished.
CONCLUSION: Haemodynamic contrast-enhanced ultrasound assessment can be used to distinguish between benign and malignant breast lesions.
The diagnostic methods currently used to distinguish between benign and malignant breast lesions are all invasive and often inconclusive. This may lead to surgery for histological assessment.1 The main objective of this study was to determine the diagnostic accuracy of SonoVue (Bracco spa, Milan) contrast-enhanced ultrasound as a diagnostic method, with histological examination as the reference standard.
Until recently SonoVue was mainly used for the assessment of liver conditions, with very few studies done on breast tissue.2,3 A secondary aim of this study was to analyse the difference in the haemodynamics between both benign and malignant focal lesions compared with normal breast parenchyma. The haemodynamic assessment represented the global average blood flow over all the vessels, neovascular and normal capillaries within a selected region of interest (ROI). This will aid the vascular characterisation of various breast abnormalities, which will be of use when microbubbles are used as a treatment modality.4
Methods
Selection and description of participants
In this prospective study, 50 consecutive patients (women aged 20 - 93 years, mean 55 years) with a breast lump were referred for clinical evaluation to the Breast Clinic of the Glasgow Royal Infirmary and Western Infirmary, UK, between July and December 2003. The lesions were diagnosed on combined clinical examination, sonography/mammography and histological examination. The histology result served as the reference standard. All the patients were aware of their confirmed diagnosis at the time of the contrast-enhanced ultrasound.
Inclusion criteria were unilateral abnormal breast lumps and a normal contralateral breast, informed consent from the patient, and ability to locate the lump by ultrasound and to identify its central area.
Exclusion criteria were bilateral breast disease, or abnormal contralateral breast tissue; any contraindication to the imaging investigations and/or histology/pathology examination; participation in another clinical study involving an investigational drug in the last 30 days; any medical condition or circumstances that would have significantly decreased the chances of obtaining reliable data or of achieving the study objectives, such as dementia, or other reasons for expected poor compliance with investigators' instructions; and pregnancy or lactation.
Technical information
Administration of SonoVue
SonoVue was supplied as a sterile, lyophilised powder contained in a septum-sealed vial. A white milky suspension of sulphur hexafluoride (SF6) microbubbles was obtained by adding 5 ml physiological saline (0.9% sodium chloride) to the powder (25 mg), using standard aseptic techniques, followed by hand agitation.
Each patient received 2 intravenous bolus injections of SonoVue (2 boluses of 2.5 ml) via a 20-gauge intravenous catheter placed in the antecubital vein for each lesion to be characterised, followed by 3 ml of saline flush.
Study design
Screening (physical examination, pregnancy test whenever applicable, medical history and concomitant medication), the triple assessment and informed written consent were obtained before the contrast-enhanced ultrasound investigation. All patients were monitored for adverse events until 2 hours after the administration of SonoVue.
Ultrasound investigations
A Phillips HDI 5000 ultrasound scanner equipped with nonlinear imaging capabilities was used in the Department of Surgery at the Glasgow Royal Infirmary. Technical settings such as mechanical index (MI) and frame rate were optimised to obtain images of the best quality (MI 0.06, frame rate 13/second). Contrast-enhanced ultrasound was performed in a standardised manner in a single plane after an IV bolus injection of 2.5 ml SonoVue and 3 ml saline flush.
To establish the location of the lesion, all patients had an unenhanced ultrasound scan using fundamental mode, followed by contrast-enhanced ultrasonography in greyscale, with non-linear imaging modes using continuous real-time imaging. The first enhanced study was over the lump and the second over a similar area of the contralateral breast. The normal breast served as the control. The enhanced sonographic examinations were recorded on CD-ROM.
QLAB (Phillips) ultrasound image analysing software transmitted the image to a computer screen. A ROI of 5 mm2 was selected over the periphery and over the centre of the focal lesion, using the accumulation image.
A time signal intensity curve was derived for both these areas. The data of these curves were automatically transferred to a Microsoft Excel file, which was used to determine the time to peak (TTP), area under the curve (AUC), in-flow gradient (IFG) and peak enhancement (PE) in a standard manner. Finally, the results were compared with the initial histological diagnosis.
Reference standard
Histological results were based on fine-needle aspirates, core biopsies and excised tumours. Ninety-eight per cent of the patients had a pathology result. One patient had a clinically evident carcinoma, without histological confirmation. This was added to 'Carcinoma not otherwise specified' (see Table II).


The final diagnosis was based on the findings of combined clinical examination, mammography/sonography and histology/pathology. Biopsies and aspirates were performed more than 2 weeks before the ultrasound study.
Definitions
Definitions are as follows: Region of interest (ROI): 5 mm square - QLAB software; Peripheral: on the edge between the normal and abnormal tissue, selected on the lesion; Central: centre of the lesion (could not be determined in scattered/small lesions); Control breast: contralateral breast without clinical or imaging evidence of breast disease; time to peak (TTP) = (time at peak) - (time at inflow), SI unit: seconds; area under the curve (AUC) = (echo2 + echo1)*(time2 - time1)/2; in-flow gradient (IFG): graph-fit-straight-line over contrast in-flow; peak-enhancement (PE) = (peak echo) - (background echo).
Statistics
Comparison between the abnormal and normal breast of each patient was performed using Wilcoxon's signed-rank test. Comparisons between malignant and benign breast lumps were performed using the Mann-Whitney test. The ability of the ultrasound-derived variables to distinguish between malignant and benign lumps was assessed using logistical regression analysis. A p-value of 0.05 or less was considered statistically significant.
Results
Subjects
A total of 50 women aged 20 - 93 years (mean age 55 years) with a breast lump were referred for clinical evaluation to the Breast Clinic of the Glasgow Royal Infirmary and Western Infirmary, UK, between July and December 2003.
All the patients were examined clinically. Seventy-four per cent had a mammogram, 32% had an unenhanced ultrasound scan, 64% had a fine-needle aspirate, 86% had a core biopsy and 98% had a pathology result.
One malignant and 8 benign tumours were excluded because the central area could not be defined.
Reference standard
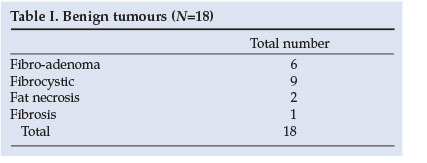
Histological examination revealed the presence of 32 breast cancers and 18 benign lesions (fibro-adenoma, fibrocystic changes, fat necrosis and fibrosis). The histopathological classification of the malignant and benign lesions is given in Tables I and II.
The mean diameter of all combined lumps was 2.5 cm (range 0.5 - 5 cm). The mean diameter of malignant lesions was 2.9 cm (0.5 - 5 cm), and of benign lesions 1.5 cm (1 - 2 cm).
Twenty-nine of the patients with malignant disease underwent breast surgery and the abnormal lesions were surgically removed. The remaining patients had a histological diagnosis made on core biopsy alone. Two patients were treated with neo-adjuvant chemotherapy before surgery and 3 patients received only hormonal treatment for their breast cancer. All the patients had unilateral breast disease. Of the 32 invasive lesions, all were primary cancers, there were no recurrences or metastatic tumours, and 1 was a Mercel cell carcinoma.
Test results and estimation
Comparison of tumour and normal tissue
The haemodynamic results for the measurements taken over the peripheral infiltrating vessels are given in Table III.
In malignant tumours, the TTP was significantly reduced and the in-flow gradient and AUC were significantly increased relative to the contralateral normal breast (all p<0.001). Peak enhancement was non-significantly increased in tumour tissue (p=0.08).
In the peripheral vessels of benign lesions, the TTP was significantly reduced (p<0.001) and the in-flow gradient significantly increased (p=0.049), but there was no significant overall difference between tumour and normal tissue in AUC (p=0.16) or peak enhancement (p=0.87).
Ultrasound measurements were performed over the central area of the tumour in 31 malignant and 10 benign tumours (Table IV). The other 1 malignant and 8 benign tumours were excluded because the central area could not be defined.
In contrast to the results in peripheral vessels, in central vessels of malignant tumours the TTP, in-flow gradient, AUC and peak enhancement were all significantly reduced (p<0.001, p=0.014, p<0.001 and p<0.001 respectively) relative to the contralateral normal breast.
In benign tumours, the TTP in central vessels was reduced (p=0.008), but there was no significant change in the other variables relative to normal breast.
Comparison of malignant and benign tumours
The in-flow gradient in peripheral vessels was significantly greater in malignant than benign tumours both in absolute terms (p=0.01) and relative to the gradient in normal breast (p=0.02). Similarly, the AUC in peripheral vessels was higher in malignant than benign tumours in both absolute and relative terms (p=0.001).
By contrast, in central vessels, the in-flow gradient tumour-to-normal ratio, the AUC (absolute and ratio), and the peak enhancement (absolute and ratio) were all significantly lower in malignant than benign tumours (p<0.05).
The variables that differed significantly between benign and malignant tumours were assessed in a multiple logistical regression analysis with forward stepwise selection, to construct a model combining independently significant predictive variables. When the analysis was restricted to measurements in peripheral vessels, so as to include all tumours, only the AUC had significant independent predictive power (p<0.001). When the analysis included measurements in both peripheral and central vessels, hence excluding those tumours in which central measurements were not available, both the AUC in peripheral vessels (p<0.001) and the tumour-to-normal ratio of peak enhancement in central vessels (p<0.001) were independently significant. The logistical regression equation relating the log of the odds of a tumour being malignant to the ultrasound variables was as follows: log odds = 6.56 PEtc /PEcon - 0.028 AUCtp - 0.51, where AUCtp = area under curve, tumour peripheral vessels, PEtc = peak enhancement, tumour central vessels, and PEcon = peak enhancement, normal breast.
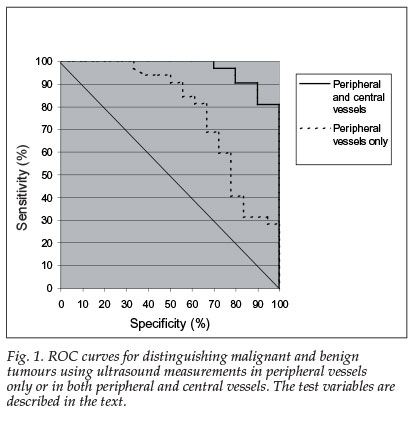
Fig. 1 shows the receiver operator characteristic (ROC) curves associated with AUCtp alone and AUCtp in combination with PEtc/PEcon. Table V shows the sensitivity and specificity achieved for each of these predictive models at thresholds that maximised the number of tumours correctly classified in this cohort. Measurements in peripheral vessels alone had poor specificity in identifying malignant tumours, and addition of the measurements in central vessels greatly improved accuracy in the subset of tumours in which these measurements were available.
Discussion
SonoVue is currently the most widely available ultrasound contrast agent in Europe for radiology applications and has replaced Levovist as the latter is no longer available or manufactured for Europe.5 The advent of the improved non-linear imaging modes combined with low mechanical index imaging has been a significant advance for the use of SonoVue clinically, as it enables continued real-time imaging with minimal microbubble destruction.4
The real-time demonstration of the contrast enhancement of the lesion relative to the control breast is the key to improving lesion characterisation, as shown in this study.
The contralateral breast was used as the control in this study; it has been proved that malignancy in a breast causes a generalised increase in flow over the entire affected breast.6 All the patients in this study had unilateral breast disease, without known metastases and there was no significant difference in the blood flow between the various groups of patients concerning the control breast. Previous studies on blood flow assessment in focal lesions have led to inconsistent results and it may well have been because the lesions were compared with the surrounding tissue, where the flow was increased because of the malignant lesion.
Two specific areas in the tumour were haemodynamically assessed, as previous studies7 have indicated that an increased vessel count and flow could be demonstrated over the periphery of the cancer and that the centre of the cancer was associated with a decrease in number of vessels and flow. This study demonstrated that this was true when both malignant and benign lumps were compared with the control breast.
Quantitative analyses on a ROI including the entire tumour volume led to inconsistent results, possibly because of the ill-defined margins in some tumours.
The majority of benign lumps assessed in this study were fibrocystic changes, which occur because of hormonal influences in the breast. The increased flow to these cysts may be a result of inflammation associated with this condition. Similarly, there was an increased flow but decreased AUC in fat necrosis.
The flow pattern of fibro-adenomas was exactly the opposite of the malignant tumours. Where malignant tumours had an increased flow and AUC over the periphery of the lump, the fibro-adenomas demonstrated an increased flow and AUC over the central aspect of the lump; this may indicate the mechanism of growth. The relative avascular state of fibrosis may explain the decrease in the AUC.
There were limitations in the design of the study. Analysis of the contrast-enhanced ultrasound scans was always done after triple assessment of the lesion and the diagnosis was available at the time of the assessment. The breast biopsies could have had an effect on the vascularity. We have not been able to demonstrate the effect. Ideally it should have been a blinded study and the analyses should have been done before breast biopsy, but the current set-up was meant to mirror clinical practice. In addition, the majority of malignant lumps were surgically removed for pathological examination and not all the benign lumps, which could potentially have led to misdiagnosis of a few benign lumps. However there is proof that once a benign lesion has been diagnosed by triple assessment, it can safely be left behind.8 Furthermore, enhancement was not always adequate to determine the central aspect of the lesion at 2.5 ml of SonoVue and pulse inversion; it may improve with 5 ml of contrast.
Nevertheless, in this study we have shown an improvement in the characterisation of focal breast lesions based on real-time assessment of the differential tumour SonoVue enhancement characteristics with regard to the normal breast. The results have shown that SonoVue-enhanced ultrasound significantly increased both the sensitivity and specificity in the characterisation of focal breast lesions. There was also a significant reduction in the number of indeterminate diagnoses following SonoVue-enhanced ultrasound.
Differentiation between the benign and malignant lesions may be difficult in some instances, e.g. fat necrosis with calcification or fibrosis post lumpectomy, more so when the lesion is small, when the characteristic features may lead to confusion and the biopsy can be difficult. In these cases contrast-enhanced ultrasound may be of benefit as it is non-invasive and can provide real-time imaging.
No adverse effects were experienced by the patients in this study. SonoVue is considered to be a safe contrast for ultrasound of the breast.4,9
Conclusion
The results suggest that SonoVue-enhanced ultrasound with non-linear imaging modes improves the characterisation of focal breast lesions and could be implemented in clinical practice to limit unnecessary referral for further invasive and/ or costly imaging scans. However further studies are needed to confirm the results and reproducibility of this study.
References
1. Bang N, Bachmann NM, Vejborg I, Mellon MA, Clinical report: contrast enhancement of tumor perfusion as a guidance for biopsy. Eur J Ultrasound 2000; 12: 159-161. [ Links ]
2. Madjar H, Prömpeler HJ, Del Favero C, Hackelöer BJ, Llull JB, A new Doppler signal enhancing agent for flow assessment in breast lesions. Eur J Ultrasound 2000; 12: 123-130. [ Links ]
3. Cosgrove D. Future prospects of SonoVue and CPS. Eur Radiol 2004; 14: 116-124. [ Links ]
4. Cosgrove D. Angiogenesis imaging-ultrasound. Br J Radiol 2003; 76: 43-49. [ Links ]
5. Leen E. The role of contrast-enhanced ultrasound in the characterisation of focal liver lesions. Eur Radiol 2001; 11: Suppl 3, E27-E3. [ Links ]
6. Mankoff DA, Dunnwald LK, Gralow JR, et al. Blood flow and metabolism in locally advanced breast cancer: Relationship to response to therapy. J Nucl Med 2002; 43: 4500-4509U. [ Links ]
7. Koukourakis MI, et al. Cancer vascularization: implications in radiotherapy? Int J Radiat Oncol Biol Phys 2000; 48: 545-553. [ Links ]
8. Houssami N, et al. Fibroadenoma of the breast. Med J Aust 2001; 174: 185-188. [ Links ]
9. Torzilli G. Adverse effects associated with SonoVue use. Expert Opinion on Drug Safety 2005; 4:399-401. [ Links ]
 Correspondence:
Correspondence:
S Barnard
(s6b7@yahoo.com)
Accepted 21 November 2006.














