Services on Demand
Article
Indicators
Related links
-
 Cited by Google
Cited by Google -
 Similars in Google
Similars in Google
Share
SAMJ: South African Medical Journal
On-line version ISSN 2078-5135
Print version ISSN 0256-9574
SAMJ, S. Afr. med. j. vol.98 n.5 Pretoria May. 2008
FORUM
CLINICAL IMAGES
An alcoholic's series of unfortunate events
S K MisserI; S R ThomsonII
IShalendra Misser was a radiology registrar at King Edward VIII Hospital, Durban, at the time of managing the patient described. Currently in private radiology practice, he has an interest in interventional radiology and is a keen athlete who has completed many Comrades and ultra-marathons
IIProfessor Thomson is a specialist surgical gastro-enterologist at Addington Hospital, Durban, who is still looking for an interventional radiologist who will stay in the academic state sector
We present a case of spontaneous decompression of a pancreatic pseudocyst into the stomach following endovascular embolisation in an alcoholic patient. To our knowledge this is the first description of this sequence of events.
A 42-year-old man, known to be an alcoholic, presented with acute severe epigastric pain and vomiting. He was moderately dehydrated, had epigastric tenderness and had an elevated serum amylase level (760 IU/l). Oral intake was restricted and nasogastric decompression applied for acute pancreatitis. He returned 7 weeks after discharge with recurrent pancreatitis and epigastric swelling. A computed tomography (CT) scan (Fig. 1) demonstrated a moderately large pancreatic pseudocyst.
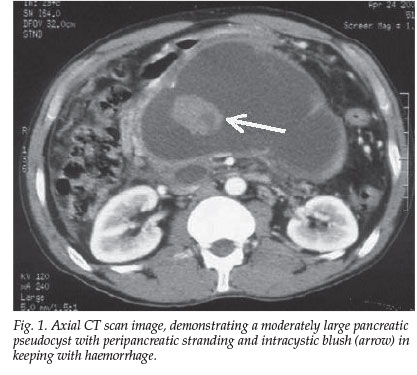
A bout of haematemesis prompted coeliac axis angiography (Fig. 2), which revealed a pseudo-aneurysm off a branch of the left gastric artery (LGA). Micro-coil embolisation (Fig. 3) was undertaken to occlude the LGA and its branch with the pseudo-aneurysm.
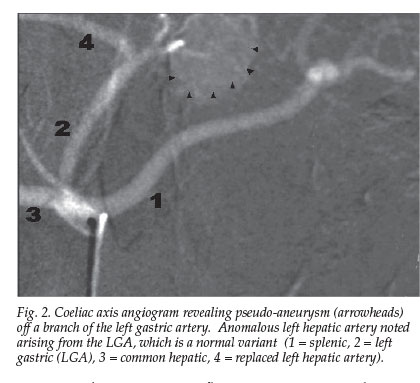
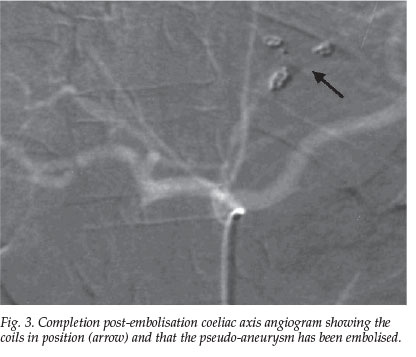
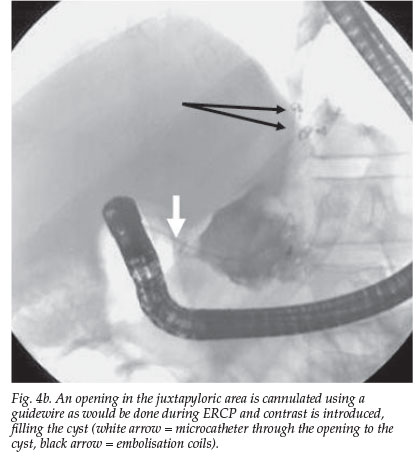
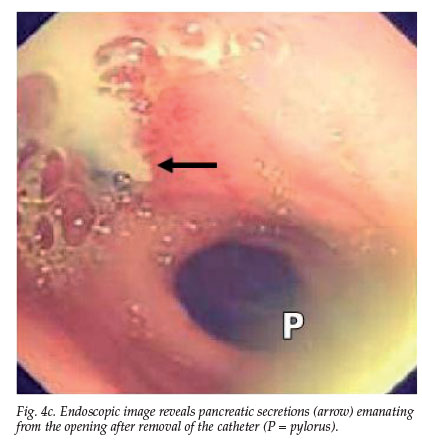
The epigastric swelling subsided but the pain persisted. At endoscopy (Fig. 4) a circular defect on the greater curve of the stomach representing a spontaneous cystgastrostomy, was noted (Figs 4a - c). This was probably due to local ischaemia from the embolisation, with resultant spontaneous decompression of the pseudocyst through a cyst-trans-gastric drainage. The epigastric pain symptoms subsided and the patient remained well after 6 months of sobriety.
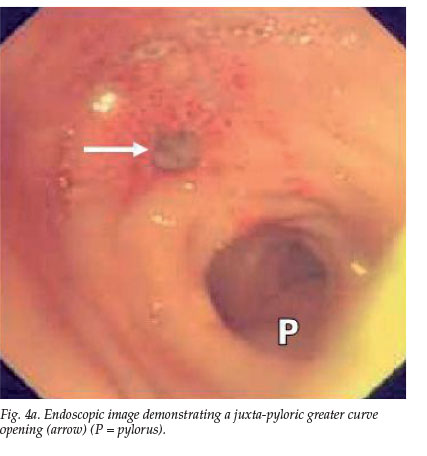
Discussion
Peripancreatic aneurysms and pseudo-aneurysms are rare but potentially devastating complications of pancreatitis, with a reported incidence between 1.3%1 and 10%.2 Severe pancreatic necrosis and peripancreatic inflammatory response in the acute phase of pancreatitis lead to leakage of proteolytic enzymes, which damage the walls of subjacent vascular structures. In the subacute or chronic phases, pancreatic abscess or pseudocyst formation may also predispose to vessel mural erosion due to compression or the elastolytic enzymatic secretions contained within these collections.3 Patients may have sudden exacerbation of abdominal pain and distension due to acute haemorrhage, which may be fatal in up to 7.5% of cases,4 or ongoing haematemesis and melaena indicating slow intermittent blood loss.5
Multidetector CT scanning of the abdomen, before and after intravenous contrast administration, is the initial investigation of choice. Contrast enhancement or a blush in relation to a peripancreatic vessel or pseudocyst, as in this patient, indicates an underlying aneurysm.1
Catheter angiography is the gold standard for identifying these aneurysms. The vessels involved are the splenic, gastroduodenal, gastro-epiploic and intrapancreatic branches.6 Visceral aneurysms have been classified in terms of their haemodynamics and management approaches devised.7 If deemed amenable to transcatheter embolisation, the vessel may be occluded. Usually only one artery is involved but synchronous false aneurysms may be successfully embolised.8 Embolisation is also the first line of treatment in pseudocyst-associated aneurysms,9 as in our patient. Other options include the use of stent-grafts and percutaneous guided intra-aneurysmal injection of thrombin.7 Initial high rebleed rates following embolisation have markedly improved over the last decade, largely owing to improved micro-catheter design and embolic agents,6 establishing embolotherapy as the first-line management in patients with haemosuccus pancreaticus due to false aneurysms.
1. Balthasar EJ, Fischer LA. Haemorrhagic complications of pancreatitis: Radiologic evaluation with emphasis on CT imaging. Pancreatology 2001; 1: 306-313. [ Links ]
2. White AF, Baum S, Buranasiri S. Aneurysms secondary to pancreatitis. AJR Am J Roentgenol 1976; 127: 393-396. [ Links ]
3. de Perrot M, Berney T, Buhler L, Delgadillo X, Mentha G, Morel P. Management of bleeding pseudoaneurysms in patients with pancreatitis. Br J Surg 1999; 86: 29-32. [ Links ]
4. Flati G, Andren-Sandberg A, La Pinta M, Porowska B, Carboni M. Potentially fatal bleeding in acute pancreatitis: Pathophysiology, prevention, and treatment. Pancreas 2003; 26: 8-14. [ Links ]
5. Huizinga WK, Kalideen JM, Bryer JV, Bell PS, Baker LW. Control of major haemorrhage associated with pancreatic pseudocysts by transcatheter arterial embolisation. Br J Surg 1984; 71: 133-136. [ Links ]
6. Mallick IH, Winslet MC. Vascular complications of pancreatitis. Journal of the Pancreas (online) 2004; 5(5): 328-337. http://www.joplink.net/prev/200409/200409_02.pdf (accessed 24 January 2007). [ Links ]
7. Nicholson AA, Patel J, McPherson S, Shaw DR, Kessel D. Endovascular treatment of visceral aneurysms associated with pancreatitis and a suggested classification with therapeutic implications. J Vasc Interv Rad 2006; 17: 1279-1285. [ Links ]
8. Pillay WR, Lalloo S, Thomson SR, Conrad MA. Embolisation of metachronous pseudoaneurysms complicating chronic pancreatitis. HPB: Official Journal of The International Hepato Pancreato Biliary Association 2003; 5(4): 251-253. [ Links ]
9. Carr JA, Cho JS, Shepard AD, Nypaver TJ, Reddy DJ. Visceral pseudoaneurysms due to pancreatic pseudocysts: Rare but lethal complications of pancreatitis. J Vasc Surg 2000; 32(4): 722-730. [ Links ]
 Correspondence:
Correspondence:
S K Misser
(shalendramisser@hotmail.com)














