Services on Demand
Article
Indicators
Related links
-
 Cited by Google
Cited by Google -
 Similars in Google
Similars in Google
Share
SAMJ: South African Medical Journal
On-line version ISSN 2078-5135
Print version ISSN 0256-9574
SAMJ, S. Afr. med. j. vol.98 n.2 Pretoria Feb. 2008
ORIGINAL ARTICLES
'Look and Lletz' - a Chris Hani Baragwanath Hospital experience
Y AdamI; C J van GelderenII; K NewellIII
IBSc, MB BCh, FCOG (SA); Department of Obstetrics and Gynaecology, Chris Hani Baragwanath Hospital and University of the Witwatersrand, Johannesburg
IIMB ChB, FCOG (SA), FRCOG; Department of Obstetrics and Gynaecology, Chris Hani Baragwanath Hospital and University of the Witwatersrand, Johannesburg
IIIBSc (Biol), MEd (Exerc Physiol), MPH (Epid & Biostats); Perinatal HIV Research Unit, Chris Hani Baragwanath Hospital and University of the Witwatersrand
ABSTRACT
OBJECTIVES: An audit was undertaken of a 'colposcopy and treatment' clinic between April 2003 and December 2006, to determine: (i) the frequency of overtreatment with Papanicolaou smear on its own, colposcopy on its own or a combination of the two methods; (ii) differences in overtreatment between patients who are HIV positive and those who are HIV negative; and (iii) the short-term complications of Lletz (large loop excision of the transformation zone) at this clinic.
DESIGN: A retrospective analysis of data from the colposcopy clinic database of patients, who were referred according to national guidelines.
SETTING: Patients who are referred to Chris Hani Baragwanath Hospital.
REULTS: Normal histology was found in 1.3% of patients, and cervical intraepithelial neoplasia (CIN) 1 or human papillomavirus (HPV) in 8.4%. The overall complication rate was 3%.
CONCLUSION: The high loss to follow-up and the low early complication rate together with an acceptable overtreatment rate make this a justifiable approach in our situation. HIV-negative women were more likely to be overtreated than HIV-positive patients (p=0.03).
Cancer of the cervix is the second most common cancer in women in South Africa, and the most common cancer in women aged 15 - 29 years and 30 - 54 years, accounting for 12.5% and 25.7% respectively.1
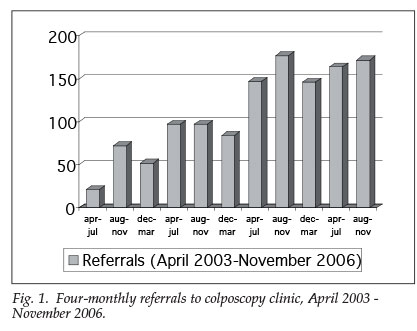
A National Screening Policy was instituted in South Africa in 2001.2 The State health system will pay for three cervical smear tests in a lifetime, commencing at the age of 30. Screening coverage has been shown to be more important than interval of screening in Scandinavian countries.3 Cytological screening for cervical cancer in Johannesburg primary health care facilities has achieved 20% coverage4 and there is a commitment to increase this. Papanicolaou smear screening and treatment of premalignant cervical abnormalities was shown to reduce the incidence of cervical cancer in Europe and North America.5 There are few dedicated clinics for the treatment of premalignant disease of the cervix in South Africa. A one-stop clinic for diagnosis and treatment is a very attractive alternative in our setting. Compliance is a concern at our clinic. Out of 231 booked patients, 80 (34.6%) did not attend in the first 6 months of 2005. Loss to follow-up was assessed at an audit done in September 2005; this showed that 9.9% of patients did not come back for their histology results and 38.5% did not come back for a 6-month Pap smear after treatment.6 The workload at the colposcopy clinic has increased over the last 2½ years because of the increase in the number of referrals to the colposcopy clinic. There was a long delay after the Pap smear in patients accessing the colposcopy clinic (Fig. 1). The range was between 14 and 706 days, with half of the patients arriving by 104 days.6
In South Africa cancer of the cervix and AIDS are both endemic. The incidence of cervical intraepithelial neoplasia (CIN) is between 50% and 70% in patients who are HIV infected in Africa.7,8 One would have anticipated an increase in the prevalence of cervical cancer but this has not yet occurred. It is possible that HIV-infected women die from other causes before they develop cancer of the cervix. With the rollout of antiretroviral drugs, cervical cancer may become more prevalent in HIV-positive patients.
Methods
The study was designed to assess the degree of overtreatment and undertreatment by correlating cytology, colposcopy and histology. The incidence of complications in the short term was also considered. The difference in overtreatment in HIV-positive as opposed to HIV-negative women was evaluated.
Information was obtained from a colposcopy database which was created for audit purposes. This was therefore a retrospective analysis of routinely collected data. The University of the Witwatersrand Ethics committee approved the study.
Patients
Between April 2003 and December 2006, 1 252 patients were referred to Chris Hani Baragwanath Hospital. Patients were excluded from the analysis if there was a lack of cytological and colposcopic evidence of CIN, pregnancy, histological evidence (e.g. punch biopsy) of CIN or if colposcopy was not possible. There were 922 patients who were included in the analysis. All of these women had a large loop excision of the transformation zone (Lletz) or cold-knife cone.
All patients with a Pap abnormality grade worse than low-grade squamous intra-epithelial lesion (LG SIL), atypical squamous cells of unknown significance which persisted for longer than 6 months, clinical suspicion of a malignancy in the presence of a normal Pap smear, and HIV-infected patients with an ASCUS or worse are referred to the clinic for colposcopy. Patients are given a written explanation of abnormalities of the Pap smear and possible treatments including outpatient Lletz and its complications. They are then counselled and given the choice of whether to have the Lletz procedure done under general or local anaesthetic. The vast majority, 892 (96.6 %) patients, have chosen to have the procedure done under local anaesthetic, while 30 (3.4%) patients (almost all by choice) had a Lletz or cold-knife cone performed under general anaesthesia.
A Lletz is performed on all patients with CIN 2 or higher on Pap smear or colposcopy, CIN 1 or higher in patients who are HIV infected, where the colposcopy is inadequate, and when there is a discrepancy between colposcopy and cytology by one grade.
The Lletz procedure
A colposcopy is performed using the saline technique. A cervical block is performed using a dental syringe with 2% lignocaine and 1 in 100 000 adrenaline. The loop size is chosen according to the size of the lesion and the transformation zone. Patients are then followed up with cervical smears at 6-monthly intervals for 3 smears and annually thereafter.
Results
Age
The patients' ages ranged from 18 to 82 with a mean of 38.7 and a median of 35.
Parity
There were 84 (9.1%) nulliparous patients, 245 (26.6%) who had had one pregnancy and 593 (64.2%) women who were multiparous.
HIV status
Two hundred and twenty (23.8%) women were HIV-negative, 464 (50.4%) had a documented HIV-positive test result and the HIV status of 238 (25.8%) women was unknown.
correlation between cytology and histology (Table I)
The correlation between Pap smear and histology was exact in 71.8%. The prediction was better with the higher grades. We considered it an undercall when Pap showed normal, ASCUS, LG SIL, or atypical squamous cells cannot exclude HG SIL (ASC-H) in the presence of histology of CIN 2 or worse. The rate of undercall with Pap smears in this group was 15.4%. The overcall for cytology was 5.6%. Of concern was the finding that the Pap smear reflected ASC-H or HG SIL in 2.1% of cases where invasive cancer was found on histology.
correlation between colposcopy and histology (Table II)
There was exact correlation between colposcopy and histology in 80.2%. The undercall (less than CIN 2 on colposcopy and more than CIN 1 on histology) with colposcopy was 5.8%. There was a 0.8% finding of invasion when the colposcopy diagnosis was CIN 2 or CIN 3.
The overcall (more than CIN 1 on colposcopy and less than CIN 2 on histology) was 7.5%.
Overtreatment
To calculate the overtreatment in this population, we used the US National Cancer Institute definition of overtreatment, in which the appropriate treatment threshold is a diagnosis of HG SIL or worse, and the numerator is the number of patients who were treated and found to have normal or LG SIL on histological diagnosis.9 Table III reflects the weighted percentages using the above definition.

A positive colposcopy was defined as reflecting an assessment of CIN 2 or worse, a positive Pap smear as HG SIL or more severe and negative histology as being normal, CIN 1 or human papillomavirus (HPV) only. Overtreatment was not significantly different whether Pap and/or colposcopy were used to decide on treatment.
HIV-negative women were more likely to be overtreated than HIV-positive women (Table IV).

Complications
Clearly only patients who returned for follow-up could be assessed in this regard. There were 79 (2.7%) patients who returned with excessive bleeding, infection or pain. There were 38 patients with haemorrhage of whom 2 were admitted for suturing in theatre. There were 34 patients with infection and 1 required a laparotomy for a pelvic abscess.
Discussion
The main criticism of the 'see-and-treat' approach is the risk of overtreatment. Quoted rates of overtreatment range between 13% and 72%.10,11 These studies differed as regards referral patterns and the definition of overtreatment.
Most of the patients who were referred to our clinic had HG SIL, and we found a better overall correlation with Pap and/or colposcopy when HG lesions were reported at histology.
The patients with equivocal smears (ASCUS, ASC-H or LG SIL) that were referred to our clinic all either had persistent abnormalities or were immunocompromised. There were 189 (20.5%) such cases, 46 (4.9%) of whom had CIN 1, HPV or normal histology, and the remainder had CIN 2 or worse. HPV testing would probably not have helped reduce the overtreatment in this group. HPV testing is less specific than Pap smear.12
The rates of overtreatment were similar for colposcopy, Pap or a combination of the two. However colposcopy did aid in assessing the transformation zone and the size of the lesion. Pap followed by Lletz without colposcopy may be considered as an option in high-prevalence areas.
There was a more liberal referral of patients who are HIV infected to the colposcopy clinic. Patients who were HIV positive were referred to the clinic with less severe cytology findings, reflecting uncertainty as regards prognosis.
It has been shown that punch biopsy does not reduce the occurrence of negative Lletz, and may be unreliable. It cannot be regarded as representing the gold standard.13 Selecting treatment on the basis of colposcopically directed punch biopsy may not be accurate.10
Failure to diagnose micro-invasive and invasive lesions was also of concern.
There were 17 out of 922 (1.8%) cases of micro-invasion or invasion not detected at colposcopy and 20 out of 922 (2.2%) cases not detected by Pap smear. These figures are similar to those reported in other series of 'see-and-treat' clinics.14,15
Conclusions
In this population with a high prevalence of both CIN and HIV, a 'see-and-treat' approach is justifiable.
The early complication rate was acceptably low, and management was appropriate in terms of over- and undertreatment, and it should be noted that overtreatment on the basis of cytology alone would have occurred in 11.1%.
References
1. Mqoqi N, Kellett P, Sitas F, Jula M. Incidence of histologically diagnosed cancer in South Africa, 1998-1999. National Cancer Registry. Johannesburg, 2004. [ Links ]
2. National guidelines for cervical cancer screening in South Africa-2000. DoH http://www.doh.gov.za/docs/facts-f.html (last accessed 14 March 2007). [ Links ]
3. Laara A, Day N, Hakama M. Trends in mortality from cervical cancer in the Nordic countries: association with organized screening programs. Lancet 1987; 8544: 1247-1249. [ Links ]
4. Report by the Public Health Unit on Cervical Cancer Screening - July 2006 to December 2006. Johannesburg: Department of Health, 2006. [ Links ]
5. Bonfiglio T. Cervical cytology: Perspectives from both sides of the Atlantic. Hum Pathol 1997; 28: 117-119. [ Links ]
6. Adam Y, van Gelderen C, Newell K. Look and LLetz. Royal College of Obstetricians and Gynaecologists, 6th International Scientific Meeting, Cairo, Egypt, 2005. [ Links ]
7. Moodley J, Hoffman M, Carrara H, et al. HIV and pre-neoplastic and neoplastic lesions of the cervix in South Africa: a case-control study. BMC Cancer 2006; 6(135). http://www.biomedcentral.com/1471-2407/6/135 (last accessed 24 May 2006). [ Links ]
8. Parham G, Sahasrabuddhe V, Mwanahamuntu M, et al. Prevalence and predictors of squamous intraepithelial lesions of the cervix in HIV-infected women in Lusaka, Zambia. Gynecol Oncol 2006; 103: 1017-1022. [ Links ]
9. Cardenas-Turanzas M, Follen M, Benedet J, Cantor S. See and treat strategy for diagnosis and management of cervical squamous intraepithelial lesions. Lancet 2005; 6: 43-50. [ Links ]
10. Ehsany N, Golbang P, Papadakis T, et al. The use of large loop excision of the transformation zone in management problems of cervical intraepithelial neoplasia. Aust NZ J Obstet Gynaecol 1998; 38(3): 251-253. [ Links ]
11. Bigrigg M, Codling B, Pearson P, Read M, Swingler G. Colposcopic diagnosis and treatment of cervical dysplasia at a single clinic visit. Experience of low-voltage diathermy loop in 1000 patients. Lancet 1990; 336: 229-231. [ Links ]
12. Walker J, Wang S, Schiffman M, Solomon D, ASCUS LSIL Triage Study Group. Predicting absolute risk of CIN3 during post-colposcopic follow-up: results from the ASCUS-LSIL Triage Study (ALTS). Am J Obstet Gynecol 2006; 195(2): 341-348. [ Links ]
13. Denny L, Soeters R, Dehaeck K, Bloch B. Does colposcopically directed punch biopsy reduce the incidence of negative LLETZ? BJOG 1995; 102: 545-548. [ Links ]
14. Das S, Elias A. Diagnosis and treatment of cervical intra-epithelial neoplasia in a single visit. Aust NZ J Obstet Gynaecol 1998; 38(3): 246-250. [ Links ]
15. Hallam N, West J, Harper C, et al. Large loop excision of the transformation zone (LLETZ) as an alternative to both local ablative and cone biopsy treatment: A series of 1000 patients. Journal of Gynecologic Surgery 1993; 9(2): 77-82. [ Links ]
Accepted 17 July 2007.














