Servicios Personalizados
Articulo
Indicadores
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares en Google
Similares en Google
Compartir
SAMJ: South African Medical Journal
versión On-line ISSN 2078-5135
versión impresa ISSN 0256-9574
SAMJ, S. Afr. med. j. vol.98 no.2 Pretoria feb. 2008
FORUM
CLINICAL IMAGES
Cutaneous cryptococcosis erroneously diagnosed as Histoplasma capsulatum infection
Geoffrey A ChipunguI; Sean J ChristiansII; Stephen P OliverIII
IG A Chipungu obtained his MB BS from University of Malawi's College of Medicine where he is employed as an assistant lecturer. He currently holds a supernumerary registrar post in Medical Microbiology at the National Health Laboratory Service (NHLS), Groote Schuur Hospital
IIS J Christians graduated from the University of Limpopo (formerly MEDUNSA) with an MB ChB and is now a registrar in the Department of Dermatology at Groote Schuur Hospital
IIIS P Oliver is a principal specialist and acting head of department in Medical Microbiology at the NHLS, Groote Schuur Hospital. All the authors are affiliated to the Faculty of Health Sciences, University of Cape Town
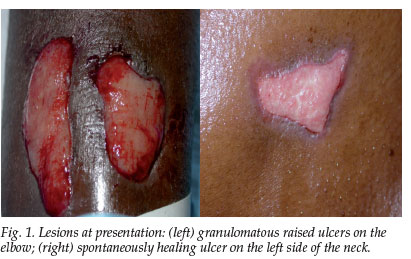
A 31-year-old patient with stage 4 HIV/AIDS presented with recurrent painful skin ulcers for more than 8 months. These would start as subcutaneous skin nodules, later becoming fluctuant and suppurating and then healing spontaneously (Fig. 1). The patient had lesions on the left wrist, left posterior thigh, right axilla, right posterior calf and right upper eyelid. He had also been diagnosed with extrapulmonary tuberculosis and had been on highly active antiretroviral therapy (HAART) for 8 months and antituberculosis medication (continuation phase). After initial poor adherence to both groups of drugs, compliance had improved. The CD4 count at baseline was 16 cells/ul and the latest result was 80 cells/ul. Histological analysis of a biopsy specimen taken from the right upper eyelid lesion showed granulation tissue with some acute inflammation. Fungal spores were seen in the exudates and stains revealed 'capsule-deficient' fungi that were first thought to be Histoplasma, and were reported as such.
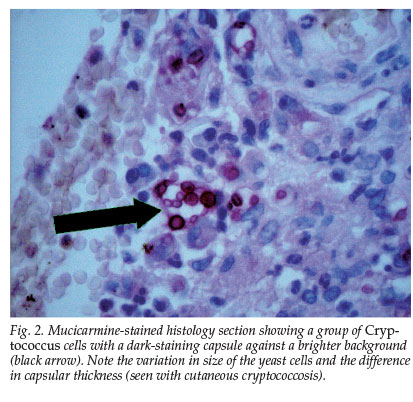
Two pus swabs were sent for bacterial, fungal and mycobacterial culture. Gram stains revealed moderate numbers of (or ++) pus cells and the presence of fungal elements. Cryptococcus neoformans, which was sensitive to fluconazole, was isolated from both pus swabs and the biopsy specimen. A mixture of Gram-negatives and Gram-positives were thought to be colonisers. Ziehl-Neelsen stain and mycobacterial culture were negative. A diagnosis of disseminated cryptococcosis was made and treatment with fluconazole was commenced. Clinicians pointed out the discrepancy between the two reports. Another section was therefore stained with mucicarmine1,2 and the diagnosis was revised to C. neoformans infection (Fig. 2). The possibility of coinfection was ruled out by means of extended fungal culture, and the lesions responded clinically to fluconazole.
Discussion
Cryptococcal infection, usually presenting as meningoencephalitis, is being diagnosed more frequently in sub-Saharan Africa because of the HIV/AIDS pandemic.3 However, presentations may vary and include skin lesions, lung infections and infections of other organs.3-5 In this patient the possibility of central nervous system involvement was ruled out by a negative lumbar puncture. Differential diagnosis included disseminated tuberculosis, carcinoma (primary or metastasis), Histoplasma capsulatum or other fungal infections, Kaposi's sarcoma and herpes simplex virus (with secondary infections).
In stage 4 HIV infection patients are so immunocompromised that opportunistic infections with multiple organisms presenting in atypical ways and at unusual sites can occur. This may present a diagnostic dilemma, and choosing empirical treatment is difficult as all these conditions merit different and sometimes potentially toxic treatment. Since histological examination can be nonspecific in the case of fungal infections, diagnosis is primarily by means of culture, with morphology, pattern of growth, biochemical reactions and automated systems used to arrive at a diagnosis. In this case a discrepancy between laboratories meant either a misdiagnosis or the rare occurrence of a mixed infection,2 which was unlikely as three specimens all cultured the same organism. The need for both histological and microbiological investigations is highlighted.
1. Vance AM. The use of the mucicarmine stain for a rapid presumptive identification of Cryptococcus from culture. Am J Med Technol 1961; 27: 125-128. [ Links ]
2. Ferry T, Ponceau B, Gaultier JB, et al. Disseminated cryptococcosis and histoplasmosis co-infection in a HIV-infected woman in France. J Infect 2005; 51: e173-e176. [ Links ]
3. Mandell GL, Bennett JE, Dolin R. Mandell, Douglas and Bennett's Principles and Practices of Infectious Diseases. 5th ed. Philadelphia: Churchill Livingstone, 2000: 2707-2718. [ Links ]
4. Murakawa GJ, Kerschmann R, Berger T. Cutaneous cryptococcus infection and AIDS. Report of 12 cases and review of the literature. Arch Dermatol 1996; 132: 545-548. [ Links ]
5. Vasanthi S, Padmavathy B. Cutaneous cryptococcosis among HIV infected patients. Indian Journal of Medical Microbiology 2002; 20: 165-166. [ Links ]
 Correspondence:
Correspondence:
G A Chipungu
(geofrey.chipungu@uct.ac.za)














