Services on Demand
Article
Indicators
Related links
-
 Cited by Google
Cited by Google -
 Similars in Google
Similars in Google
Share
SAMJ: South African Medical Journal
On-line version ISSN 2078-5135
Print version ISSN 0256-9574
SAMJ, S. Afr. med. j. vol.98 n.1 Pretoria Jan. 2008
ORIGINAL ARTICLES
Is the Western Cape at risk of an outbreak of preventable childhood diseases? Lessons from an evaluation of routine immunisation coverage
Joanne CorrigallI; David CoetzeeII; Neil CameronIII
IMB BCh, DMH (SA); School of Public Health, University of Cape Town
IIMB BCh, DTM&H, FCPHM, MS; Infectious Diseases Epidemiology Unit, University of Cape Town
IIIMB ChB, DCH, DTM&H, FCPHM (CMSA); Discipline of Community Health, Stellenbosch University, Tygerberg, W Cape
ABSTRACT
OBJECTIVE: To determine the routine immunisation coverage rates in children aged 12 - 23 months in the Western Cape.
DESIGN: Cross-sectional Household Survey using an adaptation of the '30 by 7' cluster survey technique.
SETTING: Households across the Western Cape.
SUBJECTS: A total of 3 705 caregivers of children aged 12 - 23 months who had been living in the Western Cape for at least 6 months.
OUTCOME MEASURES: Vaccination status (1 = fully vaccinated; 0 = partially vaccinated) as recorded on a Road-to-Health card or by history. Reasons for not vaccinating were established from a questionnaire.
RESULTS: The immunisation coverage was 76.8% for vaccines due by 9 months and 53.2% for those due by 18 months. The reasons given for not being immunised were clinic-related factors (47%), lack of information (27%), caregiver being unable to attend the clinic (23%), and lack of motivation (14%). Of the clinic factors cited, the two commonest ones were missed opportunities (34%) and being told by clinic staff to return another time (20%).
CONCLUSION: While the coverage indicates that a great deal of good work is being done, the coverage is insufficient to prevent outbreaks of measles and other common childhood conditions, including polio. The coverage is too low to consider not running periodic mass campaigns for measles and polio. It will need to be sustainably improved before introducing rubella vaccine as part of the Expanded Programme on Immunisations (EPI) schedule. The reasons given by caregivers for their children not being immunised are valuable pointers as to where interventions should be focused.
On the wave of the success of the smallpox vaccine achieving global eradication of smallpox, the World Health Organization (WHO) promulgated the Expanded Programme on Immunisations (EPI) in 1974.1 At that time, less than 5% of children in developing countries were receiving routine immunisations and vaccine-preventable diseases caused significant morbidity and mortality. Considerable international public health efforts have resulted in a global immunisation coverage rate of more than 80%,2 with the WHO aiming to eradicate polio by 20093 and decrease measles mortality by 90% by 2010.4 However, this coverage is not uniform, with all 699 cases of polio reported in the first half of this year occurring in developing countries.5 Polio remains endemic in Nigeria and India, and there is significant movement of people between South Africa and both these countries. Countries with inadequate immunisation coverage remain at risk, as was dramatically illustrated in May 2006 when South Africa's neighbour, Namibia, on the verge of being declared polio free, reported a large outbreak of polio with more than 90 reported cases and over 19 deaths.6
The required level of immunity in populations to prevent epidemics of infectious diseases has been estimated at about 95% and 85% for measles and polio, respectively.7 However, it should be noted that this can vary between countries and vaccines. In North America polio viruses were eliminated with a routine immunisation of less than 80% with 3 doses of oral polio vaccine, while in South America almost 100% coverage with 9 - 10 doses was required for the same result.8 Routine administration of measles vaccine was commenced in South Africa in 1975, with the current 2-dose schedule being introduced in 1995.9 After introduction of the vaccine periodic measles epidemics continued to occur, with notifications of measles in winter epidemics exceeding 20 000. Subsequent to the mass measles and polio campaigns in 1996 periodic epidemics still occur, often health-facility mediated, but only a few hundred cases are notified and the vast majority of young doctors and nurses have never seen a case of measles.
More recently, the South African Department of Health aimed 'to achieve 90% coverage for each vaccine in the routine childhood immunisation schedule in each district, by the year 2005'10 for children aged 1 year. According to routine data from the District Health Information System in November 2003, South Africa had an immunisation coverage of 79%, with the Western Cape having one of the lowest coverages of all the provinces, i.e. 69%.11 In May 2004 a comparison of vaccination rates in the Western Cape province from 2001 to 2004 showed an overall decline in fully vaccinated children from 92% in 2001 to 79% in 2004.12 The accuracy of these data was questioned and the use of different denominators (live births versus census population estimates) yielded vastly different coverage rates. Overall, these data were thought to represent an overestimation of coverage, given that the Demographic and Health Survey in 1998 measured immunisation coverage in the Western Cape at 64.2%.13
This study aimed to determine accurately the routine immunisation coverage rates of children aged 12 - 23 months in the 6 districts of the Western Cape province. In addition, the study aimed to identify factors influencing caregivers' decisions about routine childhood vaccination so that facilitating factors could be enhanced, and obstacles to vaccination might be addressed appropriately.
Methods
About 4.6 million people live in the Western Cape province, with about 3 million living in the greater Cape Town area. A cross-sectional design was used to determine immunisation coverage and to evaluate associations between vaccination status and a range of explanatory variables. The study population included all children aged 12 - 23 months who had been living in the Western Cape province for at least 6 months before the interview. The sample size calculated was 3 624 children based on 95% confidence intervals (CIs) and a 5% margin of error at the district level, presuming an equal distribution of the variable of interest in the population. The sample size was increased by 6% to allow for refusal to participate. The sampling strategy adapted the WHO's '30 by 7' technique for immunisation coverage surveys; each of the 6 health districts in the Western Cape province were divided into 90 clusters (based on Census 2001 sub-places) and 7 children in each cluster were consecutively selected from a starting household (erf number) which was selected by randomly thrown geographical darts on Arcview 3.2.
The measurement tools of this study consisted of the Road-to-Health card (RTHC) and a questionnaire. The interviewer checked the RTHC for date of birth and vaccination dates of selected children, which were entered on the questionnaire. The questionnaire collected demographic data and information on vaccination status (where the RTHC was not available). The questionnaire was compiled in English and then translated into Afrikaans and isiXhosa and translated back into English. Field workers received training in order to standardise the measurement tool, and the questionnaires were piloted before embarking on the study. Pairs of field workers conducted interviews in the first language of the respondent if they spoke English, isiXhosa or Afrikaans. Approximately 5% of interviews were conducted for quality assurance.
Definition of terms
A Road-to-Health card was given to the child caregiver by health workers who documented vaccinations on the card.
The immunisation coverage rate is the percentage of all children between 12 and 23 months during the study period that received full immunisation as per the EPI-SA norms and standards for children up to 1 year of age. Haemophilus influenzae and hepatitis vaccinations were excluded from this definition.
Data analysis
To take account of the sampling strategy, data were analysed using the survey commands on the Stata8 Statistical package, with sub-place as the primary sampling unit. In some clusters it was not possible to find 7 eligible children. In these instances the data were weighted so that a total of 7 observations from each sub-place were represented in the analysis of districts. Secondly, observations within districts were weighted to be representative of the provincial population of children aged 12 - 23 months. The primary response variable was vaccination status (1 = fully vaccinated; 0 = partially vaccinated).
Logistical regression was used to yield unadjusted odds ratios for association between the outcome and explanatory variables. Model building was performed using multiple logistical regression analysis to determine the effects of individual variables without the effects of confounding.
Results
Demographics
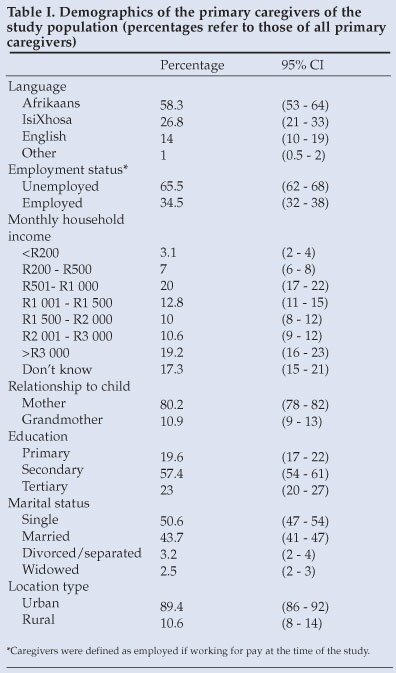
The total number of caregivers in the province who consented to be interviewed was 3 705; 154 refused consent, giving a 96% relative risk. The main reason for non-participation was lack of time to complete the interview. Ninety-six per cent of caregivers interviewed were female, with a median age of 29 years (interquartile range (IQR): 25 - 36). The median age of children was 17 months (IQR: 14 - 20). Other demographic variables are summarised in Table I. Of the socioeconomic factors, only caregiver education was shown to be a significant determinant of vaccination status. Caregivers with a secondary education were 4% (RR: 1.04; 95% CI: 1.01 - 1.06; p=0.005) more likely to have their child fully immunised compared with parents without a secondary education.
Immunisation coverage
The immunisation rates indicate the percentage of children vaccinated during the routine immunisation programme and exclude immunisation campaign vaccinations.
Immunisation coverage rates of vaccines due by 9 months
The key result, the immunisation coverage of children aged 12 - 23 months in the Western Cape province and its 6 health districts, is the immunisation coverage rate of vaccinations due at 9 months, as is the standard in such surveys. In this group fully immunised refers to children who had received 9 vaccinations due by 9 months (BCG, OPV0, OPV1, OPV2, OPV3, DPT1, DPT2, DPT3 and Measles1). Children may have received these vaccinations between birth and 23 months.
Using both card and history, the immunisation coverage for the Western Cape province was 76.8% (95% CI: 74 - 79). Of the 6 health districts in the Western Cape, only the Boland district showed a statistically significant difference with coverage at 71.7% (95% CI: 67 - 76; p=0.024). Excluding vaccinations without documentation on a RTHC ('by history' vaccines) decreased the coverage rate in the Western Cape from 76.8% to 72.1% (95% CI: 69 - 75).
Immunisation coverage rates of vaccines due by 18 months
Fully vaccinated here refers to children aged 18 months or older who had received all 12 vaccinations due by 18 months (BCG, OPV0, OPV1, OPV2, OPV3, OPV4, DPT1, DPT2, DPT3, DPT4, Measles1 and Measles2). Again, children may have received these vaccinations between birth and 23 months.
For this group, provincial coverage rates decreased to 53.2% (95% CI: 0.48 - 0.56), indicating that 24% of children fully immunised at 9 months did not receive the recommended boosters at 18 months. If only card-documented vaccinations are taken into consideration the coverage rate dropped to 49.2% (95% CI: 0.45 - 0.53).
immunisation coverage rates of specific vaccines
As illustrated in Table II, the Western Cape province has met its target of 90% immunisation coverage for 7 out of 12 (58.3%) of the routine vaccines analysed. Inadequate coverage is evident for the following 5 vaccines: OPV3 (81.3%), OPV4 (54.4%), DPT3 (85.2%), DPT4 (58.7%) and Measles2 (60%). The drop-out rate between DPT1 and DPT3 was 11.8% and between the first and second measles immunisation 32.7%. It is not clear why there is a discrepancy between the coverage of the DPT and OPV vaccines, given that they are meant to be administered at the same time.
Possession of a Road-to-Health card
Seventy-nine per cent of the sample (95% CI: 77 - 81) were in possession of a RTHC. This was the strongest predictor of immunisation coverage; children with RTHCs were 39.5 times as likely to be vaccinated compared with those without these cards (95% CI: 30 - 53).
Timeliness
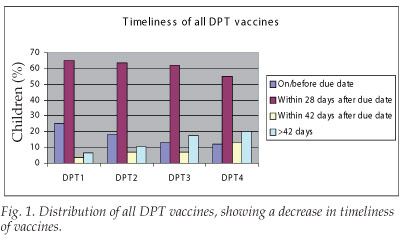
Four categories were used to analyse the timeliness of vaccines received; for each vaccine, the relative proportions of children receiving their vaccine on or before the due date, within 28 days after the due date, within 42 days of the due date, and after 42 days of the due date were calculated. This analysis allows an appraisal of the trends in timeliness of vaccines given as children get older. The results indicate that, with the exception of vaccines given at birth, the minority of children received their vaccines according to the immunisation schedule, with the majority receiving their vaccines within 28 days after the due dates. Furthermore, the results show a trend in declining rates of timely vaccinations over time (or age). This trend is best illustrated for the diphtheria-pertussis-tetanus (DPT) vaccines (Fig. 1).
Reasons given for missed vaccinations
The commonest reasons cited for having missed vaccinations were clinic factors (47.1%; 95% CI: 0.45 - 0.52), lack of information (26.9%; 95% CI: 0.19 - 0.31), caregiver being unable to attend the clinic (22.8%; 95% CI: 0.18 - 0.28), and lack of motivation (13.5%; 95% CI: 0.08 - 0.16). Of the respondents citing clinic factors 34.1% (95% CI: 0.23 - 0.48) reported missed opportunities, 19.2% (95% CI: 0.12 - 0.30) were told by clinic staff to return another time, 11% (95% CI: 0.06 - 0.19) were given incorrect vaccination dates, 9% (95% CI: 0.05 - 0.16) said the distance to the clinic was too far, 8.7% (95% CI: 0.05 - 0.16) said immunisation times were inconvenient, and 8% (95% CI: 0.03 - 0.18) experienced vaccines not being available at the clinic. The main reason cited under lack of information was the caregiver not being in their home area when the child's vaccination was due, and being unaware that they could take the child to any clinic (48.6%; 95% CI: 0.36 - 0.61). Other common reasons cited were incorrect ideas about contraindications (e.g. sick children should not be vaccinated) (24.5%; 95% CI: 0.15 - 0.37), and lack of awareness of the need for a repeat dose of a vaccine (12.1%; 95% CI: 0.06 - 0.23).
Discussion
This study is unable to identify 'pockets of low coverage' accurately, whereby certain areas or sub-districts may have significantly lower coverage than other areas. At the levels of coverage in the Western Cape, these pockets are likely to represent a high-risk group of socioeconomically disadvantaged children, the so-called 'hard-to-reach' population. Identifying these pockets through surveys or administrative data remains a challenge and would best be achieved by those working in each area.
In terms of coverage estimates, certain factors are likely to result in an underestimation of true coverage, namely exclusion of campaign vaccinations and likely underestimation of 'by history' vaccinations given (due to recall bias). Campaign vaccinations were not recorded as the explicit aim of this project was to assess the ability of routine services to achieve EPI targets. Inclusion of vaccinations as reported by caregivers (where RTHCs were unavailable) gives slightly more favourable coverage results and according to the literature is clearly more accurate than using the card alone.14 However, it is prone to recall bias, which tends to underestimate immunisation coverage.15 On the other hand, there is likely to be overestimation of true levels of immunity as vaccines are not 100% effective.16
Although the current immunisation coverage in the Western Cape is impressive, it still falls significantly short of the 90% EPI-SA target for 2005. As such, routine coverage is insufficient to prevent outbreaks of measles and other common childhood conditions, including polio, in the Western Cape. Given the relatively strong health infrastructure in this province these results raise serious concerns about immunisation coverage rates in other provinces of South Africa. Similar surveys should be considered in other provinces of South Africa to verify coverage data.
Comparing the results of the Western Cape vaccination survey with those of routinely collected data through the District Health Information System revealed both similarities and differences; it is evident that routine data have variable validity according to the denominator used and the district from which data are received. For example, routine data in 2004 indicated that immunisation coverage in the West Coast-Winelands region was 86% (using census data) or 106% (using live-birth data).12 The Provincial Department of Health recently conducted an on-site investigation of the manner in which vaccination status is recorded in order to improve the validity of routine vaccination data collection.
The evidence indicates two important explanations for the sub-optimal immunisation coverage in the Western Cape. Clinic factors, including missed opportunities and parents being sent away, are the reasons most commonly given by parents for not immunising their child. The findings give a clear indication of the problems experienced by parents at the clinic level but explanations for these experiences are lacking. Why are there so many missed opportunities? Why do nurses send caregivers away? Why are the incorrect return dates given? In the context of an overburdened health system trying to cope with dual HIV and TB epidemics, trauma and chronic disease, immunisation may be taking a back seat to more salient concerns. This is a common drawback of preventive interventions, where the success of interventions are judged precisely by what one does not see (the absence of illness). If immunisation coverage is to be improved, health workers will need to be convinced of the importance and relevance of vaccination in the era of HIV and TB. Furthermore, to enhance the complementarity of achieving immunisation targets in addition to treating disease, improving immunisation coverage should aim to strengthen health services, which will facilitate the success of both preventive and curative interventions. The key to improving service quality, well recognised by district and facility managers, is the quality of the management and supervision. Discussions with clinic staff suggest that addressing staff shortage, burn-out and patient loads will be an important component of such an intervention.
The second area in need of attention is the significant dropout between 9- and 18-month vaccines, indicating an under-utilisation of clinic services (the presumption being that those who could access a clinic at 9 months should be able to access a clinic at 18 months and thus a discrepancy is due to poor social demand for immunisations). Increasing social demand for vaccinations by ensuring that caregivers are well informed about the purpose of vaccinations, the need for repeat dosages and the availability of vaccines at any clinic is a necessary component to reduce drop-out rates.
Conclusion
The best estimate of routine immunisation coverage in the Western Cape province is 76.8%. The province has attained at least 90% coverage for 6 of the 12 individual vaccines. The overall drop-out rate of fully immunised children between 9 and 18 months was 24.5% (11.8% between DPT1 and DPT3). The results indicate that the Western Cape is at risk for an outbreak of preventable childhood diseases and it is likely that this is also the case for other provinces of South Africa. The coverage will need to be sustainably improved before introducing rubella vaccine as part of the EPI schedule.
The commonest reason given for missing a child's vaccine was clinic factors (47%), followed by a lack of information (27%). Common clinic factors were missed opportunities, being told by nurses to return another time, and being given incorrect return dates by clinic staff. These findings indicate the need to educate clinic staff and caregivers about the safety of administering vaccinations when a child is ill, provide routine checks on RTHCs at clinics, educate parents about vaccinations and where to obtain them, staff health facilities adequately, and provide channels for complaints should caregivers be sent away from clinics. Ensuring that all caregivers are given RTHCs remains an important intervention in raising immunisation coverage. Mass campaigns for measles and polio should be continued until coverage is sustained above 90%. At a higher level, provincial and regional immunisation programmes should be addressed as a unit rather than individually, taking into account the massive movement of people within South Africa and between South Africa and other countries. Lastly, identifying pockets of low coverage through routine data, further research and the knowledge of local health workers is imperative to prevent an outbreak of preventable childhood diseases.
Conflict of interest. This research was funded by the Provincial Government of the Western Cape. All the authors are in the employ of this institution.
The authors wish to acknowledge Henrietta Settler, Marilyn Braam, Mbulelo Ntlabati and all the field workers for their commitment and hard work. We would also like to thank Fawzia Desai and Stephen Titus who provided unwavering support for the project, Dr Faried Abdulla who initiated the survey, and Professor Craig Househam for granting permission to publish this work.
References
1. World Health Organization. The History of Vaccines. 2006. http://www.who.int/vaccines-diseases/history/history.shtml (accessed 12 June 2006). [ Links ]
2. World Health Organization. WHO Vaccine-Preventable Disease Monitoring System, 2004 Global Summary. Geneva: WHO, 2004. WHO publication WHO/IVB/2004. [ Links ]
3. World Health Organization. Global Polio Eradication Plan 2001-2005. Geneva: WHO, 2000. WHO publication WHO/POLIO/00.05. [ Links ]
4. WHO. Global Immunization Vision and Strategy 2006-2015. Geneva: WHO, 2005. WHO publication WHO/IVB/05.05. [ Links ]
5. World Health Organization. Geneva: WHO, 2006. http://www.polioeradication.org/casecount.asp (accessed 12 June 2006). [ Links ]
6. Department of Health, South Africa. Pretoria: Department of Health, 2006. http://www.doh.gov.za/docs/news/nz0622-f.html (accessed 12 June 2006). [ Links ]
7. Anderson RM, May RM. Vaccination and herd immunity to infectious disease. Nature 1985; 318: 323-329. [ Links ]
8. De Quadros CA, Andrus JK, Olive JM, Carrasco P. Strategies for poliomyelitis eradication in developing countries. Public Health Rev 1993/94; 21: 65-81. [ Links ]
9. Uzicanin A, Eggers R, Webb E, et al. Impact of the 1996-1997 supplementary measles vaccination campaigns in South Africa. Int J Epidemiol 2002; 31: 968-976. [ Links ]
10. National Department of Health. Immunisation That Works: the Vaccinator's Manual. Pretoria: National Department of Health, 2002: 2. [ Links ]
11. Solarsh G, Goga A. Child health. In: Ijumba P, Day C, Ntuli A, eds. South African Health Review 2003/2004. Cape Town: Health Systems Trust, 2004: 101-128. [ Links ]
12. Moodley S. Immunisation Coverage: Western Cape: Review of the Data Jan 2001. Cape Town: Provincial Government of the Western Cape, 2004. [ Links ]
13. Medical Research Council. Demographic and Health Survey 1998. Cape Town: Medical Research Council, 1998. [ Links ]
14. Delamonica E, Minujin A, Gulaid J. Monitoring equity in immunization coverage. Bull World Health Organ 2005; 83: 321-400. [ Links ]
15. Van Turrennout C, Vandelanotte J, van den Akker M, Depoorter AM. A mass campaign too often? Results of a immunisation coverage survey in the Dikgale-Soekmekaar District. S Afr Med J 2003; 93: 65-68. [ Links ]
16. Langsten R, Hill K. The accuracy of mothers' reports of child vaccination: the evidence from rural Egypt. Soc Sci Med 1998; 46: 1205-1212. [ Links ]
 Correspondence:
Correspondence:
J Corrigall
(joannecor@gmail.com)
Accepted 10 August 2007.














