Services on Demand
Article
Indicators
Related links
-
 Cited by Google
Cited by Google -
 Similars in Google
Similars in Google
Share
South African Journal of Surgery
On-line version ISSN 2078-5151
Print version ISSN 0038-2361
S. Afr. j. surg. vol.60 n.2 Cape Town Jun. 2022
http://dx.doi.org/10.17159/2078-5151/SAJS3732
TRAUMA
An audit of trauma laparotomy in children and adolescents highlights the role of damage control surgery and the need for a trauma systems approach to injury in this vulnerable population
B ReídI; V KongII; W XuI; V ThirayanV; C CheungVI; Ν RajaretnamVII; V ManchevIV; W BekkerIV; JL BruceIV; G LaingIV; DL ClarkeIV, III
IDepartment of Surgery, University of Auckland, New Zealand
IIDepartment of Surgery, Auckland City Hospital, New Zeland
IIIDepartment of Surgery, University of the Witwatersrand, South Africa
IVDepartment of Surgery, University of KwaZulu-Natal, South Africa
VDepartment of Surgery, Waikato Hospital, New Zealand
VIDepartment of Surgery, Chris Hani Baragwanath Academic Hospital, South Africa
VIIDepartment of Surgery, St James's Hospital, Ireland
ABSTRACT
BACKGROUND: This study reviews the indications and outcome of emergency laparotomy for paediatric trauma in a South African trauma centre.
METHODS: This was a retrospective study of all children less than 18 years of age who underwent an emergency laparotomy for trauma between December 2012 and October 2020 at Grey's Hospital in Pietermaritzburg.
RESULTS: During the eight-year period under review, a total of136 children of which 107 were male underwent a laparotomy for trauma. The median age was 14 years. There were 80 (57.1%) blunt mechanisms, and the rest were penetrating mechanisms. A total of 46 (33%) patients required ICU admission. Thirty-four patients developed a complication. These included nine cases of pneumonia, one case of renal failure, two patients developed abdominal collections, three wound-related complications, three neurological complications and one miscellaneous complication. There were seven (5%) deaths. The penetrating cohort were older than the blunt cohort. Solid viscera were more likely to be injured in the blunt cohort and hollow viscera more likely in the penetrating cohort. A total of 16 (11%) patients underwent damage control surgery (DCS). Of this cohort, there were three female children. Six sustained blunt trauma and ten penetrating trauma. A total of six (37%) of these children died.
CONCLUSION: Emergency laparotomy for trauma in children is not infrequent in Pietermaritzburg and there is a high incidence of penetrating trauma in this cohort. The response to increased degrees of physiological derangement is the application of DCS. Ongoing efforts to develop and strengthen a paediatric trauma service appear to be justified.
Keywords: trauma laparotomy, children, adolescents, damage control surgery, trauma systems approach, vulnerable population
Introduction
Trauma and injury contribute significantly to the burden of surgical disease in the world and are a leading cause of death and disability in young people and children. Children in the developing world are particularly at risk for sustaining trauma as injury prevention programmes are not well established, and enforcement of traffic and health and safety regulations often ineffective. In addition, poverty in itself appears to be a risk factor for sustaining trauma.1-8 In most countries, the incidence of intentional trauma in children is relatively low and this means that most of the trauma in these countries is non-intentional and blunt in nature. Blunt abdominal trauma is increasingly managed non-operatively, and this means that the need for laparotomy in children following abdominal trauma is decreasing. For all these reasons, experience with laparotomy for trauma in children may well be decreasing.9
The situation in South Africa remains somewhat of an outlier as despite being a high middle-income country (HMIC), South Africa remains plagued by an inordinate burden of trauma, despite almost three decades of relative political stability. This burden of trauma is especially egregious as a major component of it is secondary to interpersonal violence.1-8 Children in South Africa are at risk of sustaining both intentional and non-intentional trauma. Intentional trauma can be blunt in nature due to blunt assault or penetrating due to either a stab wound or a gunshot wound. This means that the spectrum of trauma in South Africa, is different to that in both the developed world and in other developing countries.
South Africa has a high rate of penetrating trauma compared to many other countries in the world.1-8 This impacts on children and there is a high incidence of penetrating injury in children and adolescents in South Africa. Subsequently, the rate of laparotomy in children in South Africa is higher than international norms. Considering the above, this project focuses on laparotomy for trauma in children < 18 years of age. It uses data from our prospectively maintained electronic registry. The project intends to quantify our experience, benchmark our outcome against the literature, and then to use this data to refine our management algorithms and to publicise this experience.
Clinical setting
Grey's Hospital is a tertiary care public hospital located in Pietermaritzburg, the capital of the KwaZulu-Natal (KZN) province, South Africa. This is one of the largest academic trauma centres in this part of the province and covers a catchment population of over three million. The Pietermaritzburg Metropolitan Trauma Service (PMTS) maintains a prospectively entered surgical registry known as the hybrid electronic medical registry (HEMR) database.
Materials and methods
Data on all children < 18 years of age who were admitted to our institution following trauma between December 2012 and October 2020 and who required a laparotomy were retrieved. Patient demographics, mechanism of injury, admission vital signs, clinical laboratory data, management strategy (operative or non-operative), number and type of blood product transfusions, duration of time from injury to admission, complications, patient residential status (urban or rural), hospital and intensive care duration of stay, and 30-day mortality rates were extracted.
Statistical analysis
All relevant data were extracted and initially summarised onto an Excel spreadsheet for review. Parametricity was assessed via the Shapiro-Wilk test. All statistical analysis was performed using R (version 4.0.2; R Foundation for Statistical Computing, Vienna, Austria). All normally distributed continuous variables were described using means with standard deviation (SD) and included heart rate (HR). Continuous variables with non-normal distribution were reported using a median with interquartile range (IQR) and included respiratory rate (RR), systolic blood pressure (SBP), lactate, length of stay (LOS) (days), temperature, pH, base excess (BE) (mEq/L) and haemoglobin (Hb) (g/dL). Independent samples t-test was used to compare normally distributed continuous variables and Mann-Whitney U test for non-normally distributed continuous variables. Chi-square test was used to compare categorical variables with the Fisher's exact test used when one group had < 5 events.
Results
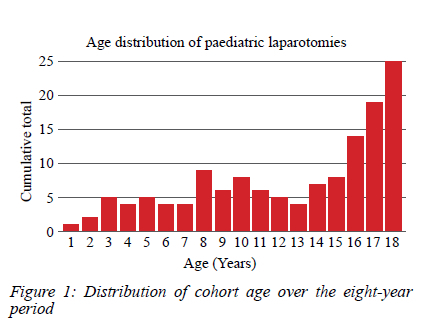
Over the eight-year period, 2 091 children and adolescents were admitted to Grey's Hospital following trauma. There were 1 479 (71%) boys and the rest were girls. The median age was 10 years (0-18). In 1 597 (76%) patients, the mechanism of injury was blunt trauma, whilst a total of 475 (23%) patients sustained penetrating trauma. These included 156 stab wounds (median age 17 years old), 141 animal bites (median age 7 years), 125 gunshot wounds (median age 16 years old), 28 impalements, and 16 assaults with miscellaneous weapons. In nine patients, the mechanism was not specified. During this time, 136 (0.6%) children, of which 107 were male, underwent a laparotomy for trauma. The median age was 14 years, and the age distribution is shown in Figure 1. There were 80 (57.1%) blunt mechanisms, and the rest were penetrating mechanisms. The frequency at which blunt trauma contributed to this data series trended upwards over the 8-year period. The inverse was observed in the case of penetrating trauma. Of the penetrating mechanisms, there were 35 stab wounds, 34 gunshot wounds, nine impalements and two animal-related injuries. Of the blunt mechanisms, there were 17 pedestrian vehicle accidents, 13 motor vehicle accidents, seven assaults, 17 falls, one structural collapse, one farming injury, one animal-related injury and one injury due to a falling missile. The number of trauma laparotomies each year remained fairly consistent, except in 2020, when there was a significant decline.
Operative findings
The mean abdominal injury score (AIS) was 2.3. There was a single AIS I, ten AIS II, 64 AIS III, 18 AIS IV, two AIS V and one AIS VI. The following organ injuries were noted: diaphragm (11), spleen (20), liver (27), kidney (21), pancreas (10), stomach (18), duodenum (7), small bowel (44), large bowel (32), rectum (7), mesentery (34), ureter (2). There were nine diaphragm repairs, nine splenectomies, five nephrectomies, 16 gastric repairs, seven duodenal repairs and eight liver packings. There were ten small bowel repairs and 14 resections and anastomoses. Of the seven rectal injuries, six had a colostomy and one a primary repair.
Outcomes
A total of 46 (33%) patients required ICU admission. Thirty-four patients developed a complication. These included nine cases of pneumonia, one case of renal failure, two cases of abdominal collections, three wound-related complications, three neurological complications and one miscellaneous complication. There were seven (5%) deaths.
Blunt versus penetrating
Table I compares the patients who sustained blunt trauma with those who sustained penetrating trauma. The presenting physiology was similar in both cohorts. The penetrating cohort was significantly older than the blunt cohort. Solid viscera were significantly more likely to be injured in the blunt cohort and hollow viscera more likely in the penetrating cohort.
Damage control
A total of 16 (11%) patients underwent damage control surgery (DCS). Six sustained blunt trauma and ten penetrating trauma. The time from injury to admission was a median of 08:34 hours with a range of (00:50:37-16:34:52). The presenting physiology of the DCS is tabulated and compared to that of the non-DCS cohort in Table II. Five patients had a concurrent head and neck injury, one a maxillo-facial injury, two a urogenital injury and five an extremity injury. Four patients underwent hepatic packing, one a splenectomy, and two a nephrectomy. In six patients, the bowel was ligated and left in the abdomen, the so-called clip and drop approach. Eleven patients required a temporary abdominal closure (TAC). Eight patients required ICU admission and three died intraoperatively. The ICU length of stay was a mean of ten days (2-50). A total of 11 patients experienced a complication. A total of six (37%) of these children died.
Of the three patients who died intraoperatively, the median time from injury to admission was 05:39:50 (03:00:0708:19:32) and the median age was eight years old (3-18). The physiology of the non-survivors is tabulated in Table III. There was a single gunshot injury and two blunt injuries in the cohort of intraoperative deaths.
Discussion
South Africa continues to experience an abnormally high burden of trauma for a country with such relative political stability.1-8 This trauma burden is unique as it is comprised of both unintentional trauma and intentional or interpersonal violence. The unintentional trauma is usually secondary to vehicle-related trauma, whilst intentional trauma is secondary to either blunt assault or assault with a penetrating weapon either secondary to knife crime or gun violence. This combination is reflected in this paper's data. There is an almost even distribution between blunt and penetrating mechanisms. This is not the norm in other countries reporting on trauma, where blunt trauma usually predominates in both adults and children. In addition, the blunt mechanisms were weighted towards vehicle-related trauma which suggests that traffic regulations are poorly enforced. The age of the penetrating trauma victims is older than that of the blunt trauma victims. This has implications for injury prevention programmes. Pre-teens are more at risk for vehicular trauma and adolescents are more at risk for penetrating trauma. This is in keeping with the experience in other cities where knife crime is endemic, such as in parts of London and Paris.9 Although strategies and policies to prevent knife crime have targeted this at-risk group, the international experience with these efforts has had mixed results.9 Ongoing efforts to improve road safety are needed for the pre-teen group. There is also a major distinction in the pattern of injury between blunt and penetrating mechanisms. Blunt trauma is largely associated with solid visceral trauma, and penetrating trauma with hollow visceral trauma.
It is now accepted that the response to increased levels of physiological derangement in a trauma patient is the application of DCS.10-13 A number of reports on the use of DCS in children have emanated from North America.14-16 An overview of the North American Trauma databank identified a total of 360 children who had undergone DCS over a period of four years and estimated that DCS is required in 12% of children with operative abdominal trauma.14-16 Another report from Pennsylvania identified 56 children who had undergone DCS over a 17-year period. These authors reported a rate of DCS of 56/371 (15%).14-16 This is similar to our series. Children who required DCS tended to have greater physiological derangements, as evidenced by a greater median ISS (25 vs 18), higher heart rate (112 vs 100), lower SBP (104 vs 113), and a lower Glasgow coma score (GCS) (12 vs 13).6 Once again, this is similar to our cohort of patients. In our series, the patients who underwent DCS all had significantly worse physiological parameters than the non-DCS cohort. These included lower SBP readings, as well as worse lactate, BE) PH and lower Hb levels. There are differences in the response to trauma between children and adults and this means that further work is required to develop appropriate guidelines for the application of DCS in children.17
The mortality rate in this series, although consistent with that reported in the literature, is not insignificant.6-9 It climbs dramatically as the degree of physiological derangement and the magnitude of injury to the central nervous system increase. This is evidenced by the significantly lower GCS on presentation in non-survivors, as well as by the significantly lower SBP and worse serum lactate levels on presentation in non-survivors.6-8,17
It is now understood that the response to trauma needs to be the establishment of a trauma system.12-18 There is increasing evidence that the development of a trauma system improves outcomes. South Africa is in the process of developing trauma systems. However, much of this initiative has been driven by adult trauma surgeons and has focused on adults. This is a major oversight as there is a considerable burden of trauma in children and adolescents. Trauma in this cohort presents unique challenges which a service focused only on adults may well struggle to meet.18-21 Despite the long distances involved in transporting injured children, it would appear that centralisation of paediatric trauma care is preferable to a more disseminated approach.22
Conclusion
Emergency laparotomy for trauma in children is not infrequent in Pietermaritzburg and there is a high incidence of penetrating trauma in this cohort. The response to increased degrees of physiological derangement is the application of DCS. Ongoing efforts to develop and strengthen a paediatric trauma service appear to be justified.
Conflict of interest
The authors declare no conflict of interest.
Funding source
No funding was required.
Ethical approval
Ethical approval for the HEMR has been granted by the Biomedical Research Ethics Committee of the University of KwaZulu-Natal (ref. no BE207/09 BCA 221/13). This approval is renewed annually and is current. The system has been functional since December 2012.
ORCID
Β Reid https://orcid.org/0000-0002-6425-2886
V Kong https://orcid.org/0000-0003-2291-2572
W Xu https://orcid.org/0000-0002-1270-2769
V Thirayan https://orcid.org/0000-0002-4528-8445
C Cheung https://orcid.org/0000-0002-4471-2822
Ν Rajaretnam https://orcid.org/0000-0001-9809-6896
V Manchev https://orcid.org/0000-0001-9152-0092
W Bekker https://orcid.org/0000-0003-0695-5994
JL Bruce https://orcid.org/0000-0001-8666-4104
G Laing https://orcid.org/0000-0001-8075-0386
DL Clarke https://orcid.org/0000-0002-8467-1455
REFERENCES
1. World Health Organization. Global Health Estimates: Life expectancy and leading causes of death and disability [Internet]. World Health Organization. Available from: https://www.who.int/data/gho/data/themes/mortality-and-global-health-estimates/ghe-leading-causes-of-death. Accessed 21 Feb 2020. [ Links ]
2. Peden M. World report on child injury prevention appeals to "Keep Kids Safe". Inj Prev. 2008;14:413-14. https://doi.org/10.1136/ip.2008.020693. [ Links ]
3. Sethi D, Hughes K, Bellis M, Mitis F, Racioppi F, editors. European report on preventing violence and knife crime among young people. 2010. p. viii + 102 pages. Available from: https://www.euro.who.int/en/publications/abstracts/european-report-on-preventing-violence-and-knife-crime-among-young-people. [ Links ]
4. Norman R, Matzopoulos R, Groenewald P, Bradshaw D. The high burden of injuries in South Africa. Bull World Health Organ. 2007;85(9):695-702. https://doi.org/10.2471/BLT.06.037184. [ Links ]
5. Brysiewicz P. Trauma in South Africa. Int J Trauma Nurs. 2001;7(4):129-32. https://doi.org/10.1067/mtn.2001.119052. [ Links ]
6. Herbert HK, Van As AB, Bachani AM, et al. Patterns of paediatric injury in South Africa: an analysis of hospital data between 1997 and 2006. J Trauma Acute Care Surg. 2012;73(1):168-74. https://doi.org/10.1097/TA.0b013e31824d67c3. [ Links ]
7. Patel N, Khofi-Phiri I, Mathiva LR, et al. Trauma related admissions to the PICU at Chris Hani Baragwanath Academic Hospital Johannesburg. Pediatr Surg Int. 2017;33(9):1013-8. https://doi.org/10.1007/s00383-017-4125-0. [ Links ]
8. Zanini A, Maistry N, Brisighelli G, et al. The burden of disease and pathology at a rapidly expanding tertiary paediatric surgical unit in South Africa. World J Surg. 2021:45(8)2378-85. https://doi.org/10.1007/s00268-021-06144-x. [ Links ]
9. Sinha CK, Rye E, Sunderland R, et al. The need for Paediatric Emergency Laparotomy Audit (PELA) in the UK. Ann R Coll Surg Engl. 2020;102(3):209-13. https://doi.org/10.1308/rcsann.2019.0141. [ Links ]
10. Rotondo M, Schwab C, McGonigal M, et al. Damage control: an approach for improved survival in exsanguinating penetrating abdominal injury. J Trauma. 1993;35(3):375-83. https://doi.org/10.1097/00005373-199309000-00008. [ Links ]
11. Lamb CM, MacGoey P, Navarro AP, Brooks AJ. Damage control surgery in the era of damage control resuscitation. Br J Anaesth. 2014;113(2):242-9. https://doi.org/10.1093/bja/aeu233. [ Links ]
12. Traynor MD Jr, Hernandez MC, Aho JM, et al. Damage control laparotomy: high-volume centres display similar mortality rates despite differences in country income level. World J Surg. 2020;44(12):3993-8. https://doi.org/10.1007/s00268-020-05718-5. [ Links ]
13. Weale R, Kong V, Buitendag J, et al. Damage control or definitive repair? A retrospective review of abdominal trauma at a major trauma centre in South Africa. Trauma Surg Acute Care Open. 2019;4(1):e000235. https://doi.org/10.1136/tsaco-2018-000235. [ Links ]
14. Polites SF, Habermann EB, Glasgow AE, Zielinski MD. Damage control laparotomy for abdominal trauma in children. Pediatr Surg Int. 2017;33(5):587-92. https://doi.org/10.1007/s00383-017-4061-z. [ Links ]
15. Villalobos MA, Hazelton JP, Choron RL, et al. Caring for critically injured children: an analysis of 56 paediatric damage control laparotomies. J Trauma Acute Care Surg. 2017;82(5):901-9. https://doi.org/10.1097/TA.0000000000001412. [ Links ]
16. Hamill J. Damage control surgery in children. Injury. 2004;35(7):708-12. https://doi.org/10.1016/j.injury.2004.03.009. [ Links ]
17. Brysiewicz P, Clarke DL, Sartorius B, Bruce JL, Laing GL. Defining predictors of mortality in paediatric trauma patients. S Afr J Surg. 2017;55(3):36-40. [ Links ]
18. Cowley RA. A total emergency medical system for the state of Maryland. Md State Med J. 1975;24:37-45. [ Links ]
19. Sampalis JS, Denis R, Lavoie A, et al. Trauma care regionalisation: a process-outcome evaluation. J Trauma Acute Care Surg. 1999;46:565-81. https://doi.org/10.1097/00005373-199904000-00004. [ Links ]
20. Nathens AB, Jurkovich GJ, Rivara FP, Maier RV. Effectiveness of state trauma systems in reducing injury-related mortality: a national evaluation. J Trauma. 2000;48(1):25-30. https://doi.org/10.1097/00005373-200001000-00005. [ Links ]
21. MacKenzie EJ, Rivara FP, Jurkovich GJ, et al. A national evaluation of the effect of trauma-centre care on mortality. N Engl J Med. 2006;354:366-78. https://doi.org/10.1056/NEJMsa052049. [ Links ]
22. Traff H, Hagander L, Salö M. Association of transport time with adverse outcome in paediatric trauma. BJS Open. 2021;5(3):zrab036. https://doi.org/10.1093/bjsopen/zrab036. [ Links ]
 Correspondence:
Correspondence:
email: victorywkong@yahoo.com














