Servicios Personalizados
Articulo
Indicadores
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares en Google
Similares en Google
Compartir
South African Journal of Surgery
versión On-line ISSN 2078-5151
versión impresa ISSN 0038-2361
S. Afr. j. surg. vol.60 no.1 Cape Town mar. 2022
http://dx.doi.org/10.17159/2078-5151/2022/v60n1a3687
COLORECTAL CANCER
Immunohistochemical determination of mismatch repair gene product in colorectal carcinomas in a young indigenous African cohort
R HollaI; A VorsterII; M LocketzIII; M de HaasII; OA OkeIV; D GovenderIII; R RamesarII; PA GoldbergIV
IDepartment of Gastroenterology, Vrije Universiteit Amsterdam, The Netherlands
IIMRC Human Genetics Research Unit, Institute of Infectious Diseases and Molecular Medicine, University of Cape Town and Affiliated Hospitals, South Africa
IIIDivision of Anatomical Pathology, National Health Laboratory Service and the University of Cape Town, South Africa
IVColorectal Surgery Unit, Groote Schuur Hospital, University of Cape Town, South Africa
ABSTRACT
BACKGROUND: Colorectal cancer (CRC) in the indigenous African population of South Africa is uncommon (age standardised incidence rates of 11.29 for males and 7.27/100 000 for females) and tends to occur at a young age. Lynch syndrome (LS), an inherited mismatch repair (MMR) gene abnormality, accounts for 3-4% of newly diagnosed CRCs in high incidence areas. There is some evidence that the contribution of an MMR abnormality to the overall CRC burden may be increased in low incidence areas. We aimed to determine the prevalence of MMR deficiency in an indigenous African population
METHODS: A cohort of 66 self-declared indigenous African patients, less than 50 years of age at diagnosis with CRC was identified from clinical and pathological records. The original histopathology was reviewed to confirm the diagnosis and features suggestive of MMR abnormality determined (pushing edge, mucinous, lymphocytic infiltration, Crohn's like reaction). Where sufficient tissue was available, samples were sectioned and stained for the four MMR proteins
RESULTS: Histopathological examination confirmed adenocarcinoma in 31 individuals. At least one feature suggestive of MMR was identified in 22 of these specimens. Twenty-seven cases were stained for all four MMR proteins using standard immunohistochemistry (IHC). MMR deficiency was found in 37% (n = 10/27) of cases. Median age of diagnosis was 35 years in the MMR-proficient group and 44 years in the MMR-deficient group, p < 0.008. No other significant differences between the groups were noted
CONCLUSION: MMR deficiency was common in colorectal carcinomas in the older patients in this cohort, but very young indigenous Africans CRCs do not appear to result from mismatch repair gene mutations
Keywords: inherited colorectal cancer, mismatch repair status
Introduction
South Africa has a low incidence of colorectal cancer (CRC), with age standardised incidence rates of 11.29/100 000 in males and 7.27/100 000 in females, according to the South African National Cancer Registry 2017. The incidence rate in the indigenous Black African population of South Africa is even lower at 4.8 in males and 3.46 /100 000 in females).1 Little is known about inherited CRCs in this population. There is some evidence that MSH2 and 6 gene mutations are relatively common2 and Lynch syndrome (LS) has been documented in Zimbabwe.3 The most common dominant inherited CRCs are familial adenomatous polyposis and LS (1% and 3-4% of cancers in the developed world). The former is easily recognised clinically by the presence of numerous colonic adenomas, while the latter has more subtle features that can be identified on histopathological examination.
LS is most commonly caused by an inactivation of one of four genes that regulates DNA mismatch repair (MMR), namely MLH1, PMS2, MSH2 and MSH6.4,5
The diagnosis of LS is made when genetic testing identifies a pathogenic germline mutation in one of the DNA MMR genes. Genetic testing is, however, expensive, time-consuming and not widely available. Therefore, a path of reflex diagnostic testing is usually followed. In this context, patients are screened using a set of clinical and histological features known as the Revised Bethesda Criteria (RBC).4 This selection is followed by tumour-based molecular testing, either by microsatellite instability determination or by immunohistochemistry (IHC) to detect the DNA MMR proteins.6,7 If microsatellite instability or loss of staining on IHC is identified, patients should undergo genetic testing.
Staining for DNA MMR protein products using IHC is a highly sensitive test for LS. It is relatively inexpensive, easily available, able to point to mutations in PMS2 and MSH6 that might be missed by MSI-testing (and has the added value of helping to reveal which MMR gene is likely defective).8
In the current investigation, we performed IHC to determine the degree to which a defective DNA MMR system is contributing to the presentation of CRC in individuals under the age of 50 years, in the understudied local indigenous African population.
Method
Informed written consent was obtained from the study participants (all patients from 1986 who had CRC and were less than 50 years of age) for molecular investigations into the genetic determinants of CRC, to access their relevant clinical information and to store tissue and information for future research.
Data collection and specimen retrieval
Between 1986 and 2015, 687 patients with colorectal carcinoma were referred to the Division of Human Genetics of the University of Cape Town (UCT) for genetic testing. For this investigation, 70 of the 687 patients were selected on the basis of self-reporting their ethnicity as indigenous African, meeting the RBC with no clinical or histological evidence of familial adenomatous polyposis. Clinical data were retrieved from the Colorectal Surgery Unit at Groote Schuur Hospital, Cape Town. Four of the 70 patients were excluded from further analysis as three did not have a histologically confirmed carcinoma and one had a carcinoma of the cervix invading the rectum, resulting in 66 patients being studied further.
Formalin-fixed paraffin-embedded tumour blocks were retrieved from archives and sectioned (3liM) using a Leica RM2125 RTS manual microtome. The sectioned tissues were fixed to the slides on a 60 °C hot plate for 5-10 minutes.
Histology
For each case, haematoxylin and eosin staining was performed on one section for the purpose of assessing histological features. Sections were dewaxed in Xylene (Merck, Kenilworth, NJ, USA) baths, three times for 30 seconds. Thereafter sections were rehydrated through three baths of absolute alcohol to water, for 30 seconds each. Sections were stained in alum haematoxylin for 5-10 minutes, rinsed with water, blued in ammonia water and again rinsed with water. Afterwards, sections were counterstained using eosin floxin for 90 seconds, rinsed with water and dehydrated through absolute alcohol to Xylene (Merck, Kenilworth, NJ, USA). Finally, the sections were covered with Entellan (Merck, Kenilworth, NJ, USA).
Tumour types were classified according to the World Health Organization "Classification of tumours of the digestive system 2010".9 Tumours were scored as Crohn's like response (CLR) present when three or more lymphoid aggregates were observed in a single low power field (4x).10 CLR is usually found in the sub-serosa and was therefore not assessed in biopsies.11 Tumours were scored as tumour-infiltrating lymphocytes (TILS) positive when there were a minimum of five intra-epithelial lymphocytes in a high power field (40x) and at least 10 high power fields had been searched.12
Immunohistochemistry
For the purpose of determining MMR status, IHC staining for all four MMR proteins was performed using the Benchmark XT (Ventana, Tucson, AZ, USA). The antibodies used for staining were MLH1 (M1) mouse monoclonal antibody, MSH2 (G219-1129) mouse monoclonal antibody, MSH6 (44) mouse monoclonal and PMS2 (EPR3947) rabbit monoclonal antibody (Ventana, Tucson, AZ, USA).
A tumour was found MMR-deficient when the neoplastic tissue showed loss of staining and the internal control tissue stained normally.8 In case normal tissue was not present on the same slide, a second slide with normal tissue was used for comparison. The evaluation of all tumour tissue sections was performed by a single pathologist (ML).
Statistics
SPSS version 23.0 (IBM) was used for all statistical analysis. To compare DNA MMR status, gender, tumour location and histological features with each other, the Pearson chi-square test was used. Alternatively, Fisher's exact test was used, if expected values were less than five. To compare age of diagnosis with other variables, an independent Kruskal-Wallis test was used. A p-value of < 0.05 was considered significant.
Results
Cohort
Tumour blocks for 31 patients could be retrieved from the archives. Twenty-six were resections and five were biopsies.
Mismatch repair
Of the 31 tumour blocks, the MMR status could not be reviewed in one case because there was no tumour. In three other cases, tissue washed off the slides. In three more cases, the PMS2 antibody did not bind to its respective protein, but these cases were included in the analysis.
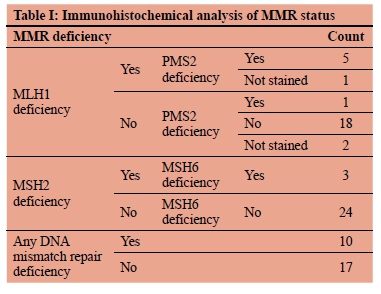
MMR deficiency was found in 10 of the remaining 27 patients (37%). Loss of staining of MLH1 (Figure 1) was found in six, of MSH2 in three and of PMS2 in one case (Table I).
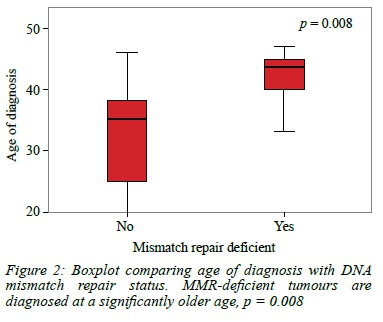
There was a significant difference in the median age of diagnosis in the MMR-proficient group (35 years) compared to the MMR-deficient group (44 years) (p = 0.008) (Figure 2).
There was no statistically significant difference between tumour location and MMR status (p = 0.667).
Histological features
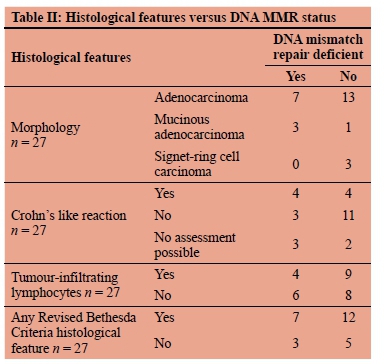
Histological assessment was available from blocks from 31 patients. Twenty-four of these were adenocarcinomas, of which four showed mucinous nnd three signet-ring cell features. A CLR was observed in 10 and TILS were seen in 14 cases. Overall, in 22 cases, at least one LS associated histological feature was identified. No statistically significant differences were found when comparing the presence of any LS histological feature to median age of diagnosis, gender or tumour location (p = 0.2, 1.0 and 1.0, respectively). Comparing histological features to MMR status showed that 70% of MMR-deficient tumours had at least one LS associated histological feature (n = 7/10). Three of the four mucinous adenocarcinomas were found to be MMR-deficient, whereas none of the signet-cell ring carcinomas showed MMR deficiency. CLR was found in four MMR-deficient tumours, as well as four MMR-proficient tumours. TILS were found in four tumours with MMR deficiency and in nine tumours with intact MMR function. No correlation between MMR status and histological features was found (p = 1.00) (Table II).
Discussion
MMR status
We set outto determine the prevalence of DNA MMR deficiencg in CRCs in young indigenous Africans from South Africa. DNA MMR deficiency was identified in 37% of cases (n = 10/27). A similar study from Morocco found 15% of colorectal tumours in patients under the age of 50 years to be MMR deficient on IHC staining.13 Three studies from western countries found percentages between 14-19%.14-16 In south-east Asia, another three studies reported percentages of 5%, 18% and 21%.17-19 An Iranian study only included CRC patients that met the strict Amsterdam II criteria and found 22.6% of cases to be MMR-deficient.20 The only similar percentage was found in a Peruvian study, reporting 38.8% MMR deficiency and/or MSI in a cohort that was not selected on the basis of age.21
This study did not assess for the possible negative staining of MLH1 due to hypermethylation of MLH1 in sporadic tumours. Because it is estimated that hypermethylation of MLH1 occurs in 15% of sporadic tumours, 80% of the MLH1 protein deficient tumours in this cohort are expected to be sporadic.22,23 This would imply that four or five of the six MLHl-deficient tumours are sporadic, reducing the prevalence of LS in this cohort to 18.5-22%.
However, Perea et al. noted that in early-onset CRC, MMR deficiency is mostly related to LS and not to somatic hypermethylation of MLH1.24 Furthermore, none of the percentages reported on the other studies were yet corrected for sporadic hypermethylation of MLH1.
In addition, one-third of mutations in MLH1 are missense mutations that may stain false-positive, a number of MMR-proficient tumours in this cohort might actually be MLHl-deficient.8
It has been hypothesised that because staining of MMR proteins can be focal, negative staining in biopsies might not be reliable.8 Kumarasinghe et al.25 provided evidence that IHC staining on biopsies had the same accuracy and was easier to interpret.
MMR-proficient tumours
The most notable difference between the MMR-deficient and MMR-proficient tumour cases is the difference in age at diagnosis (44 vs 35 years, respectively). The MMR-proficient group has a significantly lower median age at diagnosis.
Other dominantly inherited CRC syndromes could account for these DNA MMR-proficient tumours. These syndromes, however, have typical phenotypes and are suspected at endoscopic examination.26,27 A different possible cause could be MUTYH-associated polyposis (MAP). Riegert-Johnson et al.28 tested 229 cases that were referred for LS testing for MUTYH mutations and found four bi-allelic mutation carriers. This being said, MAP tumours usually present around the same age as LS, are associated with multiple polyps and are predominantly right-sided.29 The MMR-proficient group in this study presented at a younger age and showed predominance in the distal colon (73%).
It is therefore worth considering that the MMR-proficient group consists of the so-called "sporadic" subtype.27 These tumours have a strong predisposition for the distal colon, particularly for the sigmoid and rectum. They are histologically characterised by signet-ring cell tumours, perineural and venous invasion and are more likely to involve the circumferential margins of surgical resection.30 The MMR-proficient group shows the same features, with 11/15 located in the distal colon and all signet-ring cell tumours being MMR-proficient.
Perea et al.24 studied the molecular basis of early-onset CRC and reported that the majority consisted of MSS/CIMP-low tumours and were therefore most likely following the chromosomal instability pathway (CIN). Chan et al.,31 however, noted that 64% of early-onset colorectal carcinomas were microsatellite and chromosomal stable tumours (MACS).
MMR status versus histology
No correlation between histological features and MMR status was found in this study. This is in contrast with studies by Wright and Stewart32 and Bessa et al.33 who compared the histological features of tumours with MMR status. Both studies found that special subtypes of adenocarcinoma, CLR and TILS were all significantly more frequent in MMR-deficient tumours. The most likely reason for this difference is that the cohorts used in these studies consisted of ~5% of patients less than 50 years of age and are therefore not comparable to this early-onset group.
Although the results have to be interpreted with some caution due to the small size of this cohort, the comparatively high number of histological features found in the MMR-proficient tumours contributes further to the hypothesis that these tumours are a specific group of early-onset colorectal carcinoma.
Since slides tend to bleach over the years, assessing for histological features was more difficult in slides that were more than five years old. Especially determining the presence of TILS proved to be challenging. As explained in the method section, a CLR could not be assessed for in biopsies.
The MMR-proficient group of tumours occurred in patients who were younger than those who were MMR-deficient. This suggests that the proficient group represent a genetic entity that is not LS and needs to further investigation to identify the underlying genetic mechanisms.
Conclusion
This study found 37% of tumours from individuals under the age of 50 years to be MMR-deficient, which suggests that a comparatively high percentage of colorectal carcinomas in young indigenous Africans may be due to LS. In addition to this, it shows that age of diagnosis and histopathological features in this MMR-deficient group are very similar to those found in other studies on LS.
Furthermore, this study reveals an MMR-proficient subgroup of colorectal carcinoma, which bares similarity to LS when it comes to histological features but tends to be more left-sided and has a significantly younger age of onset/ diagnosis. This suggests a different and unknown genetic cause for this subgroup.
Future implications
The percentage found in this study is an indication of LS prevalence in this population. Genetic testing must be performed to determine the real prevalence and to find common variants. If a large part of the MMR-proficient group in this study does not have a germline mutation in one of the MMR genes, testing for sporadic mutations, including MLH1 promoter hypermethylation, should be considered.
Acknowledgements
The authors thank U Algar of the Colorectal Surgery Unit at The Groote Schuur Hospital Cape Town and S Govender of the Division of Anatomical Pathology at the University of Cape Town. Support for this investigation was received from the Harry Crossley Foundation.
Conflict of interest
The authors declare no conflict of interest.
Funding source
No funding was required.
Ethical approval
Ethical clearance was obtained from the Faculty of Health Human Research Ethics Committee (582/2014).
ORCID
R Holla https://orcid.org/0000-0002-8448-6217
A Vorster https://orcid.org/0000-0002-6128-0849
M Locketz https://orcid.org/0000-0002-3917-3895
M de Haas https://orcid.org/0000-0003-4173-1363
D Govender https://orcid.org/0000-0003-1487-8255
PA Goldberg https://orcid.org/0000-0003-1612-7519
REFERENCES
1. South African National Cancer Registry. Available from: https://www.nicd.ac.za/wp-content/uploads/2020/12/NCR_2017_Final_02dec2020.pdf. [ Links ]
2. McCabe M, Perner Y, Magobo R, et al. Microsatellite Instability assessment in Black South African Colorectal Cancer patients reveal an increased incidence of suspected Lynch syndrome. Sci Rep. 2019;9(1):15019. https://doi.org/10.1038/s41598-019-51316-4. [ Links ]
3. Katsidzira L, Vorster A, Gangaidzo IT, et al. Investigation on the hereditary basis of colorectal cancers in an African population with frequent early onset cases. PLoS One. 2019;14(10):e0224023. https://doi.org/10.1371/journal.pone.0224023. [ Links ]
4. Lynch HT, De la Chapelle, A. Hereditary colorectal cancer. NEJM. 2003;348(10):919-32. https://doi.org/10.1056/NEJMra012242. [ Links ]
5. Peltomaki P. Lynch syndrome genes. Fam Cancer. 2005;4(3):227-32. https://doi.org/10.1007/s10689-004-7993-0. [ Links ]
6. Umar A, Boland CR, Terdiman JP, et al. Revised Bethesda Guidelines for hereditary nonpolyposis colorectal cancer (Lynch syndrome) and microsatellite instability. J Natl Cancer Inst. 2004;96(4):261-8. https://doi.org/10.1093/jnci/djh034. [ Links ]
7. Zhang L. Immunohistochemistry versus microsatellite instability testing for screening colorectal cancer patients at risk for hereditary nonpolyposis colorectal cancer syndrome. Part II. The utility of microsatellite instability testing. J Mol Diagn. 2008;10(4):301-7. https://doi.org/10.2353/jmoldx.2008.080062. [ Links ]
8. Shia J. Immunohistochemistry versus microsatellite instability testing for screening colorectal cancer patients at risk for hereditary nonpolyposis colorectal cancer syndrome. Part I. The utility of immunohistochemistry. J Mol Diagn. 2008;10(4):293-300. https://doi.org/10.2353/jmoldx.2008.080031. [ Links ]
9. Bosman F, Carneiro F. WHO classification of tumours of the digestive system. 2010. [ Links ]
10. Alexander J, Watanabe T, Wu TT, et al. Histopathological identification of colon cancer with microsatellite instability. Am J Pathol. 2001;158(2):527-35. https://doi.org/10.1016/S0002-9440(10)63994-6. [ Links ]
11. Michael-Robinson JM, Biemer-Huttmann A, Purdie DM, et al. Tumour infiltrating lymphocytes and apoptosis are independent features in colorectal cancer stratified according to microsatellite instability status. Gut. 2001;48(3):360-6. https://doi.org/10.1136/gut.48.3.360. [ Links ]
12. Jenkins MA, Hayashi S, O'Shea AM, et al. Pathology features in Bethesda Guidelines predict colorectal cancer microsatellite instability: A population-based study. Gastroenterology. 2007;133(1):48-56. https://doi.org/10.1053/j.gastro.2007.04.044. [ Links ]
13. Benmoussa A, Badre W, Pedroni M, et al. Clinical and molecular characterisation of colorectal cancer in young Moroccan patients. Turk J Gastroenterol. 2012;23(6):686-90. https://doi.org/10.4318/tjg.2012.0474. [ Links ]
14. Steinhagen E, Shia J, Markowitz AJ, et al. Systematic immunohistochemistry screening for Lynch Syndrome in early age-of-onset colorectal cancer patients undergoing surgical resection. J Am Coll Surg. 2012;214(1):61-7. https://doi.org/10.1016/j.jamcollsurg.2011.10.004. [ Links ]
15. Wright DM, Arnold JL, Parry B, et al. Immunohistochemistry to detect hereditary nonpolyposis colorectal cancer in young patients: The 7-year Auckland experience. Dis Colon Rectum. 2011;54(5):552-8. https://doi.org/10.1007/DCR.0b013e31820e3265. [ Links ]
16. Lamberti C, Mangold E, Pagenstecher C, et al. Frequency of hereditary non-polyposis colorectal cancer among unselected patients with colorectal cancer in Germany. Digestion. 2006;74(1):58-67. https://doi.org/10.1159/000096868. [ Links ]
17. Kumamoto K, Ishida H, Suzuki O, et al. Lower prevalence of Lynch Syndrome in colorectal cancer patients in a Japanese hospital-based population. Surg Today. 2016;46(6):713-20. https://doi.org/10.1007/s00595-015-1232-1. [ Links ]
18. Ye J-X, Liu Y, Qin Y, et al. KRAS and BRAF gene mutations and DNA mismatch repair status in Chinese colorectal carcinoma patients. World J Gastroenterol. 2015;21(5):1595-605. https://doi.org/10.3748/wjg.v21.i5.1595. [ Links ]
19. Chew MH, Koh PK, Tan M, et al. Mismatch repair deficiency screening via immunohistochemical staining in young asians with colorectal cancers. World J Surg. 2013;37(10):2468-75. https://doi.org/10.1007/s00268-013-2134-2. [ Links ]
20. Zeinalian M, Emami MH, Naimi A, Salehi R, Hashemzadeh-Chaleshtori M. Immunohistochemical analysis of mismatch repair proteins in iranian colorectal cancer patients at risk for lynch syndrome. Iran J Cancer Prev. 2015;8(1):11-7. [ Links ]
21. Egoavil CM, Montenegro P, Soto JL, et al. Clinically important molecular features of Peruvian colorectal tumours: high prevalence of DNA mismatch repair deficiency and low incidence of KRAS mutations. Pathology. 2011;43(3):228-33. https://doi.org/10.1097/PAT.0b013e3283437613. [ Links ]
22. Herman JG, Umar A, Polyak K, et al. Incidence and functional consequences of hMLH1 promoter hypermethylation in colorectal carcinoma. Proc Natl Acad Sci USA. 1998;95(12):6870-5. https://doi.org/10.1073/pnas.95.12.6870. [ Links ]
23. Cunningham JM, Kim CY, Christensen ER, et al. The frequency of hereditary defective mismatch repair in a prospective series of unselected colorectal carcinomas. Am J Hum Genet. 2001;69(4):780-90. https://doi.org/10.1086/323658. [ Links ]
24. Perea J, Rueda D, Canal A, et al. Age at onset should be a major criterion for subclassification of colorectal cancer. J Mol Diagnostics. 2014;16(1):116-26. https://doi.org/10.1016/j.jmoldx.2013.07.010. [ Links ]
25. Kumarasinghe AP, De Boer B, Bateman AC, Kumarasinghe MP. DNA mismatch repair enzyme immunohistochemistry in colorectal cancer: a comparison of biopsy and resection material. Pathology. 2010;42(5):414-20. https://doi.org/10.3109/00313025.2010.493862. [ Links ]
26. Jasperson KW, Tuohy TM, Neklason DW, Burt RW. Hereditary and familial colon cancer. Gastroenterology. 2010;138(6):2044-58. https://doi.org/10.1053/j.gastro.2010.01.054. [ Links ]
27. Stigliano V, Sanchez-Mete L, Martayan A, Anti M. Early-onset colorectal cancer: a sporadic or inherited disease? World J Gastroenterol. 2014;20(35):12420-30. https://doi.org/10.3748/wjg.v20.i35.12420. [ Links ]
28. Riegert-Johnson DL, Johnson R, Rabe KG, et al. The value of MUTYH testing in patients with early onset microsatellite stable colorectal cancer referred for hereditary nonpolyposis colon cancer syndrome testing. Genet Test. 2007;11(4):361-5. https://doi.org/10.1089/gte.2007.0014. [ Links ]
29. Nielsen M, Joerink-van de Beld MC, Jones N, et al. Analysis of MUTYH genotypes and colorectal phenotypes in patients with MUTYH-associated-polyposis. Gastroenterology. 2009;136(2):471-6. https://doi.org/10.1053/j.gastro.2008.10.056. [ Links ]
30. Chang DT, Pai RK, Rybicki LA, et al. Clinicopathologic and molecular features of sporadic early-onset colorectal adenocarcinoma: an adenocarcinoma with frequent signet ring cell differentiation, rectal and sigmoid involvement, and adverse morphologic features. Mod Pathol. 2012;25(8):1128-39. https://doi.org/10.1038/modpathol.2012.61. [ Links ]
31. Chan TL, Curtis LC, Leung SY, et al. Early-onset colorectal cancer with stable microsatellite DNA and near-diploid chromosomes. Oncogene. 2001;20(35):4871-6. https://doi.org/10.1038/sj.onc.1204653. [ Links ]
32. Wright CL, Stewart ID. Histopathology and mismatch repair status of 458 consecutive colorectal carcinomas. Am J Surg Pathol. 2003;27(11):1393-406. https://doi.org/10.1097/00000478-200311000-00001. [ Links ]
33. Bessa X, Alenda C, Paya A, et al. Validation microsatellite path score in a population-based cohort of patients with colorectal cancer. J Clin Oncol. 2011;29(25):3374-80. https://doi.org/10.1200/JCO.2010.34.3947. [ Links ]
 Correspondence:
Correspondence:
PA Goldberg
Email: paulgold@iafrica.com














