Serviços Personalizados
Artigo
Indicadores
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares em Google
Similares em Google
Compartilhar
South African Journal of Surgery
versão On-line ISSN 2078-5151
versão impressa ISSN 0038-2361
S. Afr. j. surg. vol.55 no.3 Cape Town Set. 2017
NEUROSURGERY
A survey of selected key areas of management of South African neurosurgical patients
C H DanielI; M D du TrevouII
IAnaesthesiology and Critical Care, School of Clinical Medicine, University of KwaZulu-Natal
IINeurosurgery, School of Clinical Medicine, University of KwaZulu-Natal
ABSTRACT
BACKGROUND: Previous surveys of neurosurgical patient management, including a South African (SA) survey conducted in 2001, confirmed the existence of significant dissimilarities in management on national and international levels. This survey aimed to determine current SA neurosurgical patient management and to compare this with international trends.
METHODS: Questionnaires in multiple choice question (MCQ) and free text entry format covering key areas of neurosurgical practice were emailed to SA neurosurgeons following ethics approval. All responses were captured anonymously.
RESULTS: The response rate was 53%. Demographically only 5.7% respondents were younger than 40 years, 59.3% obtained a local college fellowship, 14.8% an international fellowship, 40.7% a MMed and 16.6% obtained more than one postgraduate qualification. Public sector specialists predominantly practised intracranial surgery (69%) while private specialists practised mainly spinal surgery (58%). Years in specialist practice were negatively associated with endoscopic surgery (p = 0.014) and decompressive craniectomies (p = 0.008) but not with other more recently introduced techniques including pedicle screws, neuro-navigation and cell-saver techniques. Age per se had no influence on practice. In subarachnoid haemorrhage (SAH) disease, 88% routinely administered nimodipine, 8% restricting its use to managing vasospasm. Endovascular coiling, more recently introduced for intracranial aneurysm management, was preferred to surgical clipping (54%); 69% preferred total intravenous to inhalational anaesthesia with propofol primarily replacing thiopentone for brain protection. 27% still utilised the sitting position. Only one incident of a postoperative visual defect was recorded with prone positioning.
CONCLUSION: With the exception of endoscopic and decompressive craniectomy surgery, overall management in key areas surveyed was in line with international trends.
Keywords: Endoscopic Neurosurgery, Subarachnoid haemorrhage, Spine surgery, Traumatic brain injuries and Decompressive craniectomies
Introduction
Neurosurgery in South Africa has come a long way since the pioneering days of Rowland Anthony Krynauw who in the nineteen-forties headed the first Neurosurgical unit in Africa at the Johannesburg General hospital after training in Neurosurgery in Oxford's Radcliffe Infirmary and Herman Loubcher de Villiers Hammann appointed as head of Neurosurgery at the Groote Schuur hospital in 1947 after training in Munich. Presently South Africa enjoys eight academic neurosurgical departments. The sense of differences between regions within South Africa provided the stimulus for a previous South African (SA) postal survey1 that, along with published international surveys, identified divergences in the management of neurosurgical patients. The significant developments in neurosurgery observed internationally in the last decade and the findings of Himmelseher,2 who observed significant changes between two surveys conducted in Germany in 1991 and 1997, inspired the repetition of the previous survey.
Study goals and objectives
Primary objectives
To determine whether uniformity exists in identified key areas of neurosurgical patient management in South Africa and how this relates to international trends.
Secondary objective
To determine whether demographic factors influenced practice.
Methods
The University of KwaZulu-Natal's biological research ethics committee (BREC) granted the survey ethical approval, reference number BE009/11. Informed consent for the analysis and publication of the survey data was included in the circulated electronic questionnaire with the proviso that anonymity of respondents would be protected. The Excel workbook questionnaire included semi-automated tick boxes for responses to multiple-choice questions and text boxes for free text insertion. The questionnaire comprised 69 questions covering demographics and key areas including subarachnoid haemorrhage disease (SAH), traumatic brain injury (TBI), decompressive craniotomies, brain tissue oxygen monitoring, endoscopic neurosurgery, ventricular peritoneal shunts (VPS), cervical rhizotomies, patient positioning and spinal surgery. The survey was limited to these areas because they were investigated in the initial survey (2005) and because they represent the most commonly performed neurosurgical procedures. The initial email distribution primarily utilized a database of members of the Society of Neurosurgeons of South Africa registered as specialists with the Health Professions Council of South Africa. Respondents were requested to return completed questionnaires anonymously. To ensure confidentiality, all returned questionnaires were saved as randomly numbered Excel workbooks with numbering sourced from http://www.randomizer.org. All identifying personal information was removed to prevent later identification of individuals during the analysis and subsequent publication. Initial non-responders received a second appeal to participate in the study.
International practice was broadly determined by referring to current clinical guidelines as set by international organizations such as the Brain Trauma Foundation and the North American Spine Society, while specific areas of management were individually researched in literature searches.
Statistical analyses
Data was analysed utilising IBM SPSS 21.0.0.0. 64-bit edition and Microsoft Office Excel 2011. Fisher's Exact test, Linear-by-linear association, Likelihood ratio or Pearson Chi-Square tests were employed appropriately for the analysis of all categorical data. The frequencies reflecting the degree of agreement in management strategies and the associations between demographic data and management practices were analysed.
Results
A total of 54 responses were obtained from the 102 questionnaires recorded as being successfully delivered.
Respondent demographics
There were only two female respondents. In terms of age only 5.7% were younger than 40 years. The 75.5% majority were aged between 40 and 59 years, with the remaining 18.9% being older.
Table 1 reveals the postgraduate training characteristics of respondents. The overall majority held Colleges of Medicine of South Africa fellowships.
Practice sector analysis shown in Table 2 revealed that 74.1% of respondents were in fulltime private practice, an increase over the 63.1% previously recorded.1 Private practitioners chiefly engaged in spinal surgery white state employed respondents predominantly practised intracranial surgery (p=0.001). A single respondent indicated a primarily medico-legal practice.
Subarachnoid Haemorrhage (SAH)
The 78.4% majority of respondents treated ten or fewer patients with SAH annually. There was an association between number of SAH patients seen and practice sector with greater numbers seen in fulltime hospital practice (p = 0.001). Surgeons in fulltime hospital practice constituted 81.8% of those treating more than ten SAH patients per annum.
The vast majority (88.2%) routinely used nimodipine in SAH disease; an additional 7.8% restricted its use to managing vasospasm while the 3.9% not using nimodipine all managed less than ten SAH patients a year. Oral administration of nimodipine was preferred by 38.3%, intravenous (IV) administration by 36.2% and 25.5% utilized both oral and IV administration. All public service surgeons utilized the oral route while 77.8% of those in private practice preferred IV or combinations of IV and oral administration (p = 0.016).
Triple H therapy, known as the combination of hypervolaemia, hypertension and haemodilution, was no longer routinely used (67.6%) and totally avoided by 3.9%. Triple H therapy use declined as years in practice increased (p = 0.002). In unclipped aneurysms, 54.9% were in favour and 45.1% against its use. There were no associations between demographic parameters and Triple H therapy in unclipped aneurysms.
Endovascular coiling was preferred by 54.0% for treating intracranial aneurysms as opposed to the 41.1% favouring surgcal clipping.
Total intravenous anaesthesia (TWA) was preherredto an inhalational anaesthetic technique for aneurysm surgery by 69% of respondents. Barbtturate brain protection ha0 declined considerably from the previous survey's (78.9%) to 27.3) with 75% of now preferring propoiol brain protection. 70.5% used mild hypothermia for brain protection.
Normotension for intraoperative blood pressure control was preferred by 65%. Routine intentional intraoperative hypotension was still used by 4.1%. Intraoperative blood pressure control choice was not associated with years in specialist practice, postgraduate training centre or practice sector.
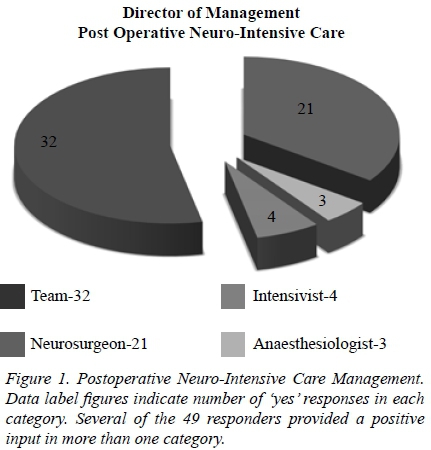
Respondents who answered the question on intraoperative monitoring all used an intra-arterial line and a central venous pressure (CVP) catheter intraoperatively during aneurysm surgery with 59.6% preferring subclavian central vein cannulation. The remainder utilized both the subclavian or internal jugular approach non-preferentially.
There was no association between the routine use of postoperative ventilation in intracranial aneurysm surgery and the age of respondent, year of qualification or the number of years in specialist practice. However, its use was associated with surgeons seeing ten or less SAH patients annually (p = 0.008).
Traumatic brain injury (TBI)
Fifty percent of respondents used prophylactic antibiotics in TBI despite 94.2% being aware that administration has no evidence base. Ceftriaxone was favoured as first choice by 59.3% and ampicillin by 22.2%. One respondent (3.7%) still favoured chloromycetin in combination with ampicillin. No associations were found between antibiotic choice, year of qualification or years in specialist practice.
Intracranial pressure (ICP) monitoring was used by 86.8% of respondents reflecting a modest increase over the 78.9% previously recorded. Over 40% of respondents utilized intra-ventricular, parenchymal or subdural ICP monitoring while 9.3% still used outmoded extradural ICP monitoring.
Brain tissue oxygen monitoring was only available to 38.5% of respondents. 53.8% considered diffuse TBI and an intracranial contusion as the major indication for brain tissue oxygen monitoring, while 23.1% specified SAH and a TBI plus an intracranial haemorrhage (ICH) as the most important indications. There was no association between practice sector and the availability of brain tissue oxygen monitoring.
Responses to the question on the utilization of decompressive craniectomies were received from 55.6% of respondents. Of these, 76.6% perform five or less procedures annually with a further 6.7% performing between six and ten procedures a year. Only 16.7% of respondents, all qualified in the last ten years, performed more than ten procedures per year. There was a negative association between the years in specialist practice and the number of decompressive craniectomies performed annually (p = 0.008).
Ninety-two percent of respondents avoided mild hypothermia usage in TBI as opposed to 71% previously recorded.
In terms of first choice for the treatment of refractory intracranial hypertension, mannitol and hyperventilation were each selected by 19.5% of respondents, cerebrospinal fluid (CSF) diversion by 8.0%, head elevation by 5.0%, sedation by 5.0%, surgery by 4.8% and steroids by 2.4%. The reasons for these choices were not determined.
Patient positioning
The number of respondents no longer utilizing the sitting position increased from 63.2% in the previous survey to 73.1%. Those using this position identified its main indications as pineal surgery 42.9%, cervical foraminotomy 28.6% and posterior fossa surgery 28.6%. For intraoperative monitoring in the sitting position, an arterial line and multiple orifice CVP was used by 85.7% of respondents, precordial doppler by 57.1% and transoesophageal echocardiography (TEE) by 50.0%.
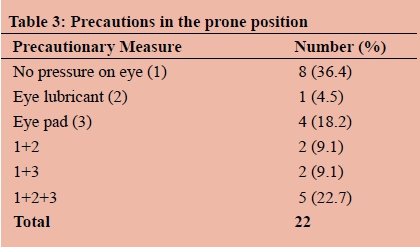
All respondents used the prone position for posterior fossa surgery and only one respondent experienced visual complications with this position. 73.1% utilized pins as a precaution to prevent ocular complications in the prone position, 7.7% the soft horseshoe and the remainder either precaution. Additional precautions are listed in Table 3 below.
Endoscopic surgery
The practice of endoscopic surgery was negatively associated with the number of years in specialist practice (p = 0.014). The characteristics of this relationship are shown in Table 4. A further association was found between practice sector and the number of endoscopic procedures performed (p = 0.002). Surgeons solely in the private sector perform relatively few endoscopic procedures with 59% not performing any. Another 33.3% performed less than five per annum and only three (7.7%) of surgeons in the private sector indicated that they performed more than five endoscopic procedures per year.
Cervical rhizotomies
24.1% of respondents performed more than 15 cervical rhizotomies each per year. The five respondents performing more than 20 procedures averaged 36.4 +/- 8.204 (range 30-50) procedures annually. 59.1% of respondents did not perform cervical rhizotomies.
Ventriculo-peritoneal shunts
With one exception, all performed Ventriculo-Peritoneal (VP) shunts. 80.3% performed more than ten VP shunts annually and there was no association between the numbers of endoscopic procedures and VP shunts performed.
Spinal Surgery
No associations were found between newer techniques in spinal surgery including neuro-navigation, pedicle screws, somatosensory evoked potentials (SSEP) and cell-saver use and years in practice. Forty-four percent of surgeons performing spinal fusions utilizing pedicle screws operated with an orthopaedic surgeon. Eighteen percent utilized neuro-navigation for the placement of pedicle screws while only 2% used SSEP. Eight percent utilized induced hypotension for spinal surgery while 50% used cell-saver technology. Sixty-six and seven tenths percent of surgeons preferred muscle relaxation maintained during spinal surgery.
Discussion
Before discussing to what extent the overall objectives of the survey were achieved we need to consider the implications of the input received and its relevance to South African Neurosurgical practice.
Demographics
UKZN, with researchers and respondents based in the same region, not unexpectedly had the highest percentage of respondents.
The apparent aging of South African neurosurgeons raises a concern. Only 5.7% of respondents were younger than 40 years while nearly a fifth were 60 years or older. Recent publications raised the issue of the implications of ageing medical practitioners on patient care. Blasier3 noted that in surgery, in addition to accompanying physical and cognitive deterioration, the rapid pace of technological developments further exacerbated the problem. Negative associations were found in relation to failure to adopt newer technology but these were unrelated to increasing age. The numbers of endoscopic procedures and decompressive craniectomies performed decreased inversely as the numbers of years in specialist practice increased. This was, however, not the case with the technologies of pedicle screws in spinal surgery, neuro-navigation, cell-saver usage and rhizotomies where no associations were found. Bhatt4 in his review of when surgeons should retire concluded that functional ability and not chronological age was the more relevant factor in determining patient mortality and postoperative complications with increased risk associated with reduced volumes of surgery. Litigation, the prime focus of several publications on this subject, was not investigated in this survey. With a response rate of 52.7% the age distribution could merely reflect unwillingness of younger neurosurgeons to participate in such surveys. The original survey distribution database did not include age, excluding comparative research in relation to response rate and age.
Gender distribution is of interest with neurosurgery emerging as a male dominated speciality. Review of successful FCS (Neurosurgery) candidates in the CMSA Transactions Journal from 2004 until 2014 identified only four female names out of 56 candidates.
Pretoria University respondents returned equal percentages for MMed and fellowship qualifications unlike the other two previously Afrikaans medium universities (Free State and Stellenbosch) that produced the highest percentages of MMeds and were least reliant on fellowships as a route to specialist qualification. In contrast, most traditional English language university respondents had fellowship qualifications with low numbers completing an MMed. The present requirement for both the CMSA fellowship single exit examination and an MMed for all specialist registrations has ended the era of specialization pathway alternatives in South Africa. The research component of the MMed has placed a further burden on specialist trainees in a specialty heavily burdened by service loads.
Practice sector emerged as a principal factor influencing spectrum of practice. The reason for the primarily spinal practice in the private sector and predominantly intracranial surgery in state or fulltime academic practice is worthy of speculation. This divergence between the private and fulltime spectrum of practice may serve to explain the distribution of patients with SAH, with two thirds of those in state practice seeing more than 20 SAH patients a year while only 3,4% of those in private seeing more than 20 patients. As this was not studied previously, no conclusion in support of a developing trend can be reached.
Subarachnoid haemorrhage disease
The management of SAH disease saw significant changes in the last decade. The main developments were related to the shift to endovascular coiling for intracranial aneurysms and intraoperative hypothermia.
The original Intraoperative Hypothermia for Aneurysm Surgery Trial (IHAST)5 published in 2005 found that moderate intraoperative hypothermia failed to improve outcome. In a recently published Cochrane database of systemic reviews Li et al. confirmed this finding.6 The fact that the majority of respondents continue with this practice is probably because many like Gupta et al7 believe that the IHAST study had limitations requiring further investigation of hypothermia.
Endovascular coiling of intracranial aneurysms has become increasingly available and is now the preferred approach for certain aneurysm in 54% of respondents. This is in line with a recent meta-analysis of coiling versus clipping demonstrating an improved clinical outcome in better grade SAH patients although accompanied by a higher incidence of rebleeding.8 Nimodipine's beneficial effect following acute aneurysmal SAH was established more than three decades ago.9 This survey confirms nimodipine as part of the national standard of care for SAH and along with intervention balloon angioplasty, is presently considered best management of cerebral vasospasm in a review by Findlay.10 The mode of administration follows practice segment profiles with public sector respondents preferring the oral route while those in private practice favoured either IV or oral and IV combinations. Recent research failed to demonstrate any benefit for either mode of administration in reducing vasospasm or delayed neurological deficits11 with the difference in choice therefore possibly related to availability or cost.
Two-thirds of respondents no longer support the routine combined use of hypervolaemia, haemodilution and hypertension (Triple H therapy). Opinions on its use remain controversial. Gupta's view is that Triple H therapy has largely been replaced by induced hypertension alone while Adamczyk, in a review of the medical management of SAH,12 declares it as the mainstay of medical management.The underlying reason for the decline is the lack of evidence of its efficacy in improving outcome and the considerable medical morbidity including dilutional hyponatremia, pulmonary oedema and myocardial ischemia and infarction associated with its use. Further intracranial complications include worsening cerebral oedema, elevation of ICP and the risk of rebleeding from an unclipped aneurysm.
A total intravenous anaesthetic (TIVA) technique was preferred to an inhalational technique by the majority. The preference of a TIVA technique may have been related to propofol's ability to significantly reduce ICP. This is crucial in early aneurysm clipping surgery where a less compliant brain is more often encountered. Thiopentone's 2:1 preference over propofol in the previous survey has been reduced to less than a third, with its decline in use possibly due to its delayed recovery compared to propofol and its prolonged clearance from the body deferring neurological assessment and brain death certification.
Patient positioning
The use of the sitting position for posterior fossa and cervical spine surgery has further declined. Reassuring was that half of those who responded to this question utilized TEE monitoring, identified as the most sensitive monitor for venous air embolism in a 600 patient sitting position series13 along with the substantial majority who routinely used a minimum of both a multi-orifice central line and an arterial line.
Traumatic brain injury
Mild hypothermia remains controversial in terms of its perceived benefit versus risk. The decreased use of hypothermia for brain protection in TBI, decreasing from 28.9% previously to 8.0% is in line with Clifton's study14 and confirmed by a recent systematic review of the role of therapeutic hypothermia in improving outcome after traumatic brain injury15 that found no benefit. Schreckinger16 still advocates a place for hypothermia in TBI in the presence of intracranial hypertension, arguing a favourable risk/benefit. He identified eleven TBI prospective randomized clinical trials in which hypothermia was compared to normothermia where data for ICP data was captured. In addition, he found six prospective cohort studies where ICP data was recorded before and during hypothermia treatment. He noted equal efficacy to barbiturates, hyperventilation and mannitol. He conceded that decompressive craniectomy, hypertonic saline and lumbar CSF drainage were superior where intracranial hypertension was present.
The indications and timing of surgery for decompressive craniectomy surgery remain controversial despite the finding of the DECRA study17,18 that it was associated with a more unfavourable outcome despite lowering elevated ICP and shorter stays in ICU. In this survey decompressive craniectomy surgery appeared confined to more recently qualified specialists with the surrounding controversy possibly dissuading surgeons trained earlier.
The reason for 50% of neurosurgeons still preferring to use prophylactic antibiotics can only be speculative.
Endoscopic surgery
Endoscopic neurosurgery is gaining popularity worldwide. This survey found that surgeons trained prior to its introduction were unlikely to embrace it. Two possible reasons exist: the time required to acquire the necessary endoscopic surgery skills and little support from medical equipment suppliers in contrast with the generous technical support by industry provided for procedures such as pedicle screws and cervical rhizotomies.
Limitations of the Study
The study depends on self-reported data on a questionnaire which was not tested for validity and reliability. The questionnaire was designed specifically for a survey of the South African context.
Conclusion
This survey has established that a degree of consensus exists in the management of South African neurosurgical patients in the key areas surveyed. In contrast with the previous survey,1 we have found that management in these areas has kept pace with international developments. There is some evidence suggesting that increasing age or years in practice is associated with continued obsolete practices. The limited update of newer techniques that require extended periods of training such as endoscopic surgery was noted among established surgeons. Our findings may influence the approach to future neurosurgical training in South Africa.
Acknowledgements
The authors wish to thank Professor Colleen Aldous, Professor Bruce Biccard, Dr Reitze Rodseth and the staff of the disciplines of Neurosurgery and Anaesthesiology and Critical Care of the University of KwaZulu-Natal for their support and assistance.
Conflict of interest
There are no conflicts of interest.
REFERENCES
1. Daniel CH, Natho N, Osborn IJ. South African Neurosurgical Patient Management Survey. South Afr J Anaesth Analg. 2005;11:615. doi: 10.1080/22201173.2005.10872399 [ Links ]
2. Himmelseher S, Pfenninger E, Werner C. Intraoperative monitoring in neuroanesthesia: a national comparison between two surveys in Germany in 1991 and 1997. Scientific Neuroanesthesia Research Group of the German Society of Anesthesia and Intensive Care Medicine. Anesth Analg. 2001;92:166-71. doi: 10.1097/00000539-200101000-00032 [ Links ]
3. Blasier RB. The problem of the aging surgeon: when surgeon age becomes a surgical risk factor. Clin Orthop Relat Res. 2009;467:402-11. doi: 10.1007/s11999-008-0587-7 [ Links ]
4. Bhatt NR, Morris M, O'Neil A, Ridgway PF. When should surgeons retire? BJS. 2016;103: 35-43. doi: 10.1002/bjs.9925 [ Links ]
5. Todd MM, Hindman BJ, Clarke WR, Torner JC. Intraoperative Hypothermia for Aneurysm Surgery Trial I. Mild intraoperative hypothermia during surgery for intracranial aneurysm. N Engl J Med. 2005;352:135-45. doi: 10.1056/NEJMoa040975 [ Links ]
6. Li LR, You C, Chaudhary B. Intraoperative mild hypothermia for postoperative neurological deficits in people with intracranial aneurysm. Cochrane Database Syst Rev. 2016. doi: 10.1002/14651858.CD008445.pub3 [ Links ]
7. Gupta N, Pandia MP, Dash HH. Research studies that have influenced practice of neuroanesthesiology in recent years: A literature review. Indian J Anaesth. 2013;57:117-26. doi: 10.4103/0019-5049.111834 [ Links ]
8. Li H, Pan R, Wang H, et al. Clipping versus coiling for ruptured intracranial aneurysms: a systematic review and meta-analysis. Stroke. 2013;44:29-37. doi: 10.1161/STROKEAHA.112.663559 [ Links ]
9. Allen GS, Ahn HS, Preziosi TJ, et al. Cerebral arterial spasm--a controlled trial of nimodipine in patients with subarachnoid hemorrhage. N Engl J Med. 1983;308:619-24. doi: 10.1056/ NEJM198303173081103 [ Links ]
10. Findlay JM, Nisar J, Darsaut T. Cerebral Vasospasm: A Review. Can J Neurol Sci. 2016;43:1532. doi: 10.1017/cjn.2015.288 [ Links ]
11. Kronvall E, Undren P, Romner B, Saveland H, Cronqvist M, Nilsson OG. Nimodipine in aneurysmal subarachnoid hemorrhage: a randomized study of intravenous or peroral administration. J Neurosurg. 2009;110:58-63. doi: 10.3171/2008.7.JNS08178 [ Links ]
12. Adamczyk P, He S, Amar AP, Mack WJ. Medical Management of Cerebral Vasospasm following Aneurysmal Subarachnoid Hemorrhage: A Review of Current and Emerging Therapeutic Interventions. Neurol Res Int. 2013;Vol 2013: [about 10 p.]. Article ID 462491. doi: 10.1155/2013/462491 [ Links ]
13. Ganslandt O, Merkel A, Schmitt H, et al. The sitting position in neurosurgery: indications, complications and results. a single institution experience of 600 cases. Acta Neurochir. 2013;155:1887-93. doi: 10.1007/s00701-013-1822-x [ Links ]
14. Clifton GL, Miller ER, Choi SC, et al. Lack of effect of induction of hypothermia after acute brain injury. N Engl J Med. 2001;344:55663. doi: 10.1056/NEJM200102223440803 [ Links ]
15. Georgiou AP, Manara AR. Role of therapeutic hypothermia in improving outcome after traumatic brain injury: a systematic review. Br. J. Anaesth. 2013;110: 357-67. doi: 10.1093/bja/aes500 [ Links ]
17. Schreckinger M, Marion DW. Contemporary management of traumatic intracranial hypertension: is there a role for therapeutic hypothermia? Neurocrit Care. 2009;11:427-36. doi: 10.1007/s12028-009-9256-2 [ Links ]
18. Cooper DJ, Rosenfeld JV, Murray L, Arabi YM, et al. Decompressive Craniectomy in Diffuse Traumatic Brain Injury. N Engl J Med. 2011;364:1493-1502. doi: 10.1056/ NEJMoa1102077 [ Links ]
19. Honeybul S, Ho KM, Lind CR. What can be learned from the DECRA study? World Neurosurg. 2013;79:159-61. doi: 10.1016/j.wneu.2012.08.012 [ Links ]
 Correspondence:
Correspondence:
Dr C. H. Daniel
daniel@ukzn.ac.za














