Serviços Personalizados
Artigo
Indicadores
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares em Google
Similares em Google
Compartilhar
South African Journal of Surgery
versão On-line ISSN 2078-5151
versão impressa ISSN 0038-2361
S. Afr. j. surg. vol.55 no.3 Cape Town Set. 2017
GENERAL SURGERY
Defining predictors of mortality in pediatric trauma patients
P BrysiewiczI; D L ClarkeII; B SartoriusI; J L BruceII; G L LaingII
ISchool of Nursing & Public Health, University of KwaZulu-Natal, South Africa
IIDepartment of Surgery, Edendale Hospital, Pietermaritzburg Metropolitan Hospital Complex, South Africa
ABSTRACT
BACKGROUND: The aim of this study was to describe our cohort of pediatric trauma patients and to analyze their physiological data. The intention was to highlight the difficulty in using systolic blood pressure (SBP) readings in this population and to investigate the role of base excess (BE) in predicting clinical outcomes in pediatric trauma patients.
METHODOLOGY: The Pietermaritzburg Metropolitan Trauma Service (PMTS) maintains a prospective digital trauma registry, and all pediatric trauma patients admitted to the service for the period January 2012 - July 2016 were included.
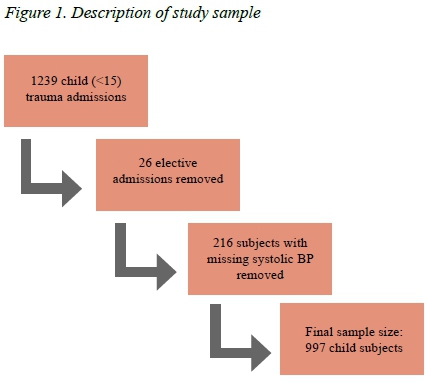
RESULTS: Out of an original dataset of 1239 pediatric trauma patients admitted to the emergency departments of the PMTS, 26 elective patients and 216 patients with missing SBP were excluded to leave a sample size of 997 patients. The majority of the sample was male accounting for 669 patients (67.2 %) with 327 females (32.8%) and 1 (0.1%) missing data. The mean age (SD) was 7.7 years (3.9) and the median age (IQR) was 8 years (5 - 11). There were 58 children < 2 years of age, 177 between the age of 2 to < 5 years of age, 402 between 5 to < 10 years of age and 360 between 10 and < 15 years of age. The predominant mechanism of injury was blunt trauma (78.4% or 782/997). Penetrating trauma accounted for 11.0% of cases (110/997). The mean systolic BP (SD) across the whole cohort was 110.1 mm Hg (16.9) and the median systolic BP (IQR) was 110 mm Hg (100-119). Mortality rate remains low and then precipitously increases below a SBP of 93 mm Hg in children older than 2 and below 89 mm Hg in children younger than 2. This suggests that a SBP of 93 mm Hg or less in children older than 2 and 89 mm Hg or less in children under 2 years is clinically significant. Similarly, as BE decreased, the mortality risk also increased prominently.
CONCLUSION: This study has used a previously described methodology based on large developed world trauma databases and confirms the current thinking that SBP is a late marker and thus not useful in the pediatric population and a better system/ approach is needed. The use of BE in conjunction with SBP may be a more useful means of identifying shock.
Keywords: pediatric trauma; trauma registry; mortality; shock
Introduction
Assessing pediatric trauma patients is difficult due to their size and the differences in the physiological response to injury between children and adults. This makes establishing the clinical diagnosis of shock in this cohort of patients difficult. The early recognition of traumatic shock in pediatric trauma victims is essential if appropriate management is to be instituted in a timely manner. It is generally taught that hypotension in children is a late sign and represents advanced shock. However, the normal range of systolic blood pressure (SBP) in children varies with age and is generally lower than in adults.1,2 This makes the use of SBP in the diagnosis of shock in children problematic. Other predictors of mortality and shock have been identified in the literature, and the most commonly available is the systemic base excess (BE).3 Our service has recently developed a hybrid electronic medical record system, which allows us to capture clinical data in real time and incorporate it into a relational database.4,5 The aim of this study was to describe our cohort of pediatric trauma patients and to analyze their physiological data. The intention was to highlight the difficulty in using SBP readings as a predictor of shock in this population as a whole and then to investigate the role of BE in predicting clinical outcomes in pediatric trauma patients.
Methodology
Ethics approval to maintain the registry has been obtained from the Biomedical Research Ethics Committee (BCA221/13 BREC) of the University of KwaZulu-Natal and from the Research Unit of the Department of Health, South Africa. This prospective digital trauma registry, which was developed and maintained by the Pietermaritzburg Metropolitan Trauma Service (PMTS), collects data from a number of institutions.4,5 All pediatric trauma patients (birth to < 15 years) admitted within the surgical service by clerking medical staff for the period January 2012-July 2016 were included in the study. The vital signs used in this study were the first recorded after arrival at the emergency department (approximately within 15 minutes), although exact time may vary from patient to patient. Analysis was performed on SBP relative to overall mortality, admission to intensive care unit (ICU), total length of hospital stay, the need for surgery, base deficit, lactate, age, and gender.
Statistical methods
Stata 13.0 and R statistical package 3.0.3 were used for data analysis.6 Several methods for selecting optimal cut-offs were implemented using receiver operating characteristic (ROC) curves. A commonly used index which minimizes the distance between the ROC plot and the point (0,1) [or upper left most corner] was used to identify the optimal breakpoint for low systolic BP for the optimal classification of mortality.7-9 The discriminatory power was evaluated by the area under the ROC curve (AUC). An AUC value of 0.5 indicates no discriminative ability while an AUC exceeding 0.8 suggests good to excellent predictive capability. Sensitivity and specificity based on the optimal cut-point were calculated along with 95% confidence intervals. Comparisons of mortality frequency and other categorical characteristics by shocked classification (systolic BP < 90 versus > 90) were performed using the Pearson chi-square (χ2) test or Fisher exact test (if expected cell count with fewer than 5 observations). Differences in mean BE and other continuous characteristics by shocked status were performed using the standard t-test. A p-value of < 0.05 was considered statistically significant. The total cohort was then broken down into four age related categories namely; < 2 years of age, 2 - < 5 years of age, 5 - < 10 years of age and 10 - < 15 years of age.
Results
A total of 1239 pediatric trauma patients were captured on our system. Figure 1 summarizes the dataset of 1239 pediatric trauma patients. The majority of the sample was male accounting for 669 patients (67.2 %) with 327 females (32.8%) and 1 (0.1%) missing data. The mean age (SD) was 7.7 years (3.9) and the median age (IQR) was 8 years (5 -11). The breakdown of ages and mean physiological variables according to age group is provided in Table 1.
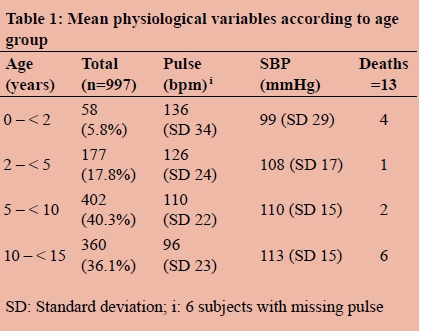
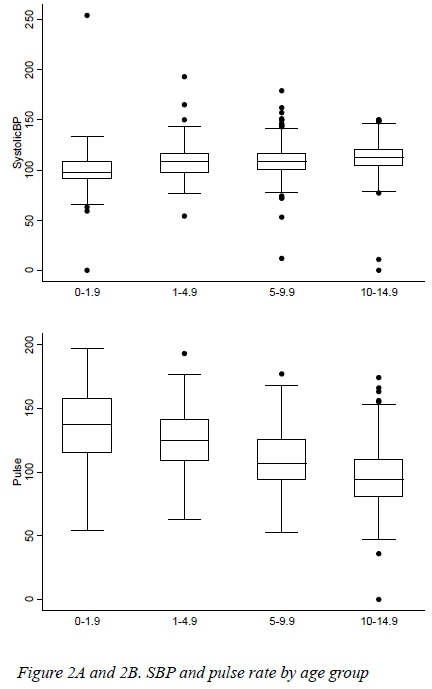
There were 58 children < 2 years of age, 177 between the age of 2 to < 5 years of age, 402 between 5 to < 10 years of age and 360 between 10 and < 15 years of age. We observed 13 (1.3 %) deaths in this cohort. Pulse rate was highest in the 0 - < 2 and 2 - < 5 age groups and lowest in the age group 10 - < 15 years. The opposite trend was observed for SBP. Figure 2A and Figure 2B represent this graphically.
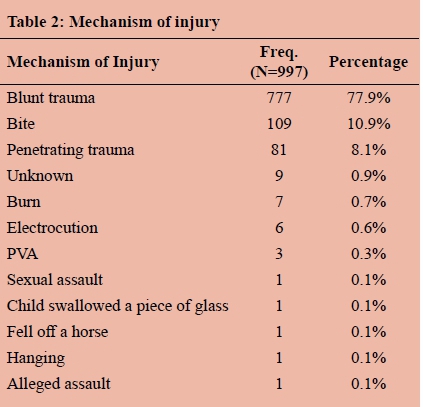
The predominant mechanism of injury was blunt trauma (78.4%) and penetrating trauma accounted for 11.0% of cases.
The breakdown of the mechanisms is provided in Table 2. The most predominant mechanims were blunt trauma (777 or 77.9%) followed by bite (109 or 10.9%), penetrating trauma (81 or 8.1%), unknown (9 or 0.9%), burn (7 or 0.7%) and electrocution (7 or 0.6%).
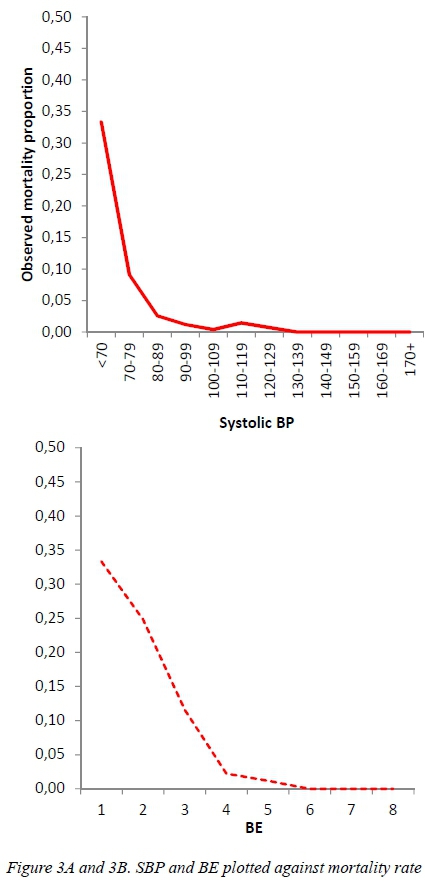
Two hundred and sixty (260), or 27%, of the sample underwent some form of surgery and 115 (11.5%) required ICU admission. The median length of total hospital stay (IQR) was 2 (1-5) days. The mean systolic BP (SD) was 110.1 mm Hg (16.9) and the median systolic BP was 110 mm Hg. Five of the 13 deaths had a SBP lower than 90 and of these 3 had a SBP lower than 70. Those who died had a significantly lower mean SBP compared to the survivors (90.6 vs 110.4, p < 0.001). Figure 3 clearly depicts this.
Predicting Mortality
The ROC analysis of all children < 15 suggests an optimal systolic BP cut-off of 93 when predicting mortality among children. This approach yields an AUC of 0.67 (95% CI: 0.49-0.85) and a high sensitivity (91.2%, 95% CI: 89.2-92.9%) and PPV (99.2%, 95% CI: 97.3-99.4%). However stratification of this analysis suggests a lower SBP cut-off in the < 2 age group of 89 [AUC of 0.72 (95% CI: 0.31-1.00) and a high sensitivity (83.3%, 95% CI: 70.1-92.8%) and PPV (97.8%, 95% CI: 78.3-99.1%).
Based on these cut-offs, 96 patients (9.6%) were classified as possibly shocked (SBP< 89 for < 2 age group and < 93 for those 2 years and older). The 95% binomial confidence interval around the shocked point estimate was 7.9-11.6%. Similarly, as BE decreased the mortality risk also increased prominently. The inflection curve (Figure 3) with fitted nonlinear curve clearly shows the upward change in observed mortality frequency at a systolic BP of ~ 93 mm Hg and lower. Similarly as BE decreased the mortality risk also increased prominently. Figure 3A and 3B shows the inflection curve of mortality risk versus systolic blood pressure and BE respectively. The possibly shocked (based on SBP < 89 and 93 respectively by age group) pediatric trauma patients from our cohort had a significantly higher mortality (6.3% vs 0.8%), significantly lower mean age (5.5 vs 8.0) and a larger median base excess (- 4.2 vs - 2.6). No significant difference was found in median lactate, ICU admission, total length of hospital stay and required surgery was observed by the shocked status. Table 3 summarizes this data.
Discussion
There is a range of normal SBP in the pediatric population, which is generally lower than in adults. This makes it confusing for staff to differentiate between categories of traumatic shock in children based on the patient's systolic blood pressure. The American Heart Association (AHA) uses the fifth-percentile systolic blood pressures for age to define hypotension.10 The ATLS provides a rule of thumb which states that the normal SBP of a child is 90 mm Hg + twice the child's age. Other authors have defined hypotension according to the respective age groups of pediatric trauma patients: SBP less than 80 mm Hg if less than 1 year old, SBP less than 90 mm Hg if 1 to 5 years old, SBP less than 100 mm Hg if 6 to 12 years old, and SBP less than 110 mm Hg if more than 12 years old. Our data confirm these differences in physiology between the three different age groups and emphasize the importance of a readily available chart of the norms for age in the resuscitation area where pediatric trauma patients are received.
All standard texts emphasize the fact that the increased physiologic reserve in children means that pediatric trauma patients may display nearly normal vital signs even in the presence of severe shock.1,2,10 Only once more than a quarter of the circulating blood volume has been lost (20 mL/kg of blood loss of an estimated total blood volume of 80 mL/kg), will the patient demonstrate the classical signs of shock such as tachycardia and hypotension. This often heralds a precipitous deterioration. For these reasons hypotension in a pediatric trauma patient is regarded as a very ominous sign. In this pediatric cohort this phenomenon is elegantly shown as mortality rates remain low and then precipitously increase below a SBP of 93 mm Hg in children older than 2 and below 89 mm Hg in children younger than 2. Our data confirms the established teaching that hypotension in children is a sign of decompensated shock. In addition, hypotension occurs suddenly and precipitously and children with hypotension are at significantly increased risk of death. This makes SBP a poor method to diagnose shock.11
The response to this has been to combine vital signs with a metabolic measurement to try and recognize the presence of a shock state at a much earlier point in the patient's management. In 1996, Davis and colleagues described four different classes of shock based on BE.11 Class I was defined by a BE of not more than 2 mmol/ L, class II (mild shock) by a BE of more than 2.0 to 6.0 mmol/L, class III (moderate shock ) by a BE of more than 6.0 to 10.0 mmol/L, and class IV (severe shock ) by a BE of more than 10 mmol/L. Work from large adult trauma databases has shown that this system is better at identifying the presence of shock than the more established ATLS classification. Our data supports this finding and goes on to show that a worsening BE correlates directly with deteriorating SBP. In our series non-survivors had a significantly worse BE than survivors. For these reasons we feel that SBP alone is inadequate to identify the presence of shock in pediatric trauma patients and the use of BE in conjunction may allow for a more accurate assessment of the presence of shock in this cohort of patients. Further work using base excess, and/or capillary refill to diagnose shock should be explored in future studies.
Conclusion
This study has shown that a SBP of < 93 mmHg and < 89 mmHg in pediatric trauma patients 2+ or < 2 years of age respectively is associated with a dramatically increased risk of mortality and confirms the current thinking that SBP is a late marker and thus not useful to use in the pediatric population. There is a relationship between deteriorating BE and SBP and this suggests that SBP should be combined with the measurement of BE in the management of pediatric trauma patients.
REFERENCES
1. Partrick DA, Bensard DD, Janik JS, Karrer, FM. Is hypotension a reliable indicator of blood loss from traumatic injury in children? Am J Surg. December 2002;184(6):555-9 discussion 559-60. [ Links ]
2. Sinniah, D. Shock in children. J S M E. 2012;6(Suppl 1):S129-S136. [ Links ]
3. Paladino L, Sinert R, Wallace D, Anderson T, Yadav K, Zehtabchi S. The utility of base deficit and arterial lactate in differentiating major from minor injury in trauma patients with normal vital signs. Resuscitation. 2008;77:363-8. [ Links ]
4. Laing GL, Bruce JL, Skinner DL, Allorto NL, Clarke DL, Aldous C. The design, construction and implementation of a computerized trauma registry in a developing South African metropolitan trauma service. Injury. January 2014 ;45(1):3-8. doi: 10.1016/j.injury.2013.05.013 [ Links ]
5. Laing GL, Bruce JL, Skinner DL, Allorto NL, Clarke DL, Aldous C. Development, implementation and evaluation of a hybrid electronic medical record system specifically designed for a developing world surgical service. World J Surg. June 2014;38(6):1388-97. doi: 10.1007/s00268-013-2438-2.2.35 [ Links ]
6. StataCorp. Stata Statistical Software: Release 13. College Station. 2013; TX: StataCorp LP. [ Links ]
7. Youden, WJ. Index for rating diagnostic tests. Cancer. 1950;3:32-5. [ Links ]
8. Metz, CE. Basic principles of ROC analysis. Seminars Nucl. Med. 1978;8:283-98. [ Links ]
9. Vermont J, Bosson JL, Francois P, Robert C, Rueff A, Demongeot J. Strategies for graphical threshold determination. Computer Methods and Programs in Biomedicine.1991;35:141-50. [ Links ]
10. American College of Surgeons on Trauma, editor. Shock. ATLS student course manual. 8th ed. Chicago: American College of Surgeons on Trauma; 2008. p. 56-61. [ Links ]
11. Davis JW, Parks SN, Kaups KL, Gladen HE, O'Donnell-Nicol S. Admission base deficit predicts transfusion requirements and risk of complications. J Trauma. 1996:41:769-74. [ Links ]
 Correspondence:
Correspondence:
Prof P Brysiewicz
brysiewiczp@ukzn.ac.za














