Serviços Personalizados
Artigo
Indicadores
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares em Google
Similares em Google
Compartilhar
South African Journal of Surgery
versão On-line ISSN 2078-5151
versão impressa ISSN 0038-2361
S. Afr. j. surg. vol.53 no.3-4 Cape Town Dez. 2015
GENERAL SURGERY
Helicobacter pylori as an occupational hazard in the endoscopy room
T du Toit; O C Buchel; S J A Smit
Department of Surgery, University of the Free State, Bloemfontein, South Africa
ABSTRACT
BACKGROUND: It remains controversial whether or not healthcare workers on upper gastrointestinal endoscopy teams are at risk of Helicobacter pylori infection. An association between occupational exposure and an increased risk of infection has been shown in a number of studies, while such a risk was not confirmed in others. None of these studies were conducted in Africa.
METHOD: We performed a cross-sectional study to determine the prevalence of H. pylori infection in endoscopy personnel versus that in a control group of other healthcare workers.
RESULTS: Ninety-two participants were included in the study. Thirty-two (55%) in the control group tested positive for H. pylori. Twenty participants (59%) in the combined endoscopy groups (34 in total) tested seropositive for H. pylori. The seropositive rate was highest in those more frequently involved with endoscopies in the endoscopy groups. None of these differences were statistically significant.
CONCLUSION: An H. pylori infection rate, similar to the national prevalence rate, estimated to be 51-71%, was displayed in both the study and control groups. We were unable to confirm that endoscopy was a risk factor for endoscopy teams with regard to contracting H. pylori.
Helicobacter pylori infection of the stomach is associated with an increased risk of peptic ulcer disease, chronic atrophic gastritis, gastric mucosa-associated lymphoid tissue lymphoma and adenocarcinoma of the stomach.12
Historically, there was an erroneous perception that the stomach was too acidic an environment for any microbial colonisation or infection. The first observation of bacteria in the stomach of dogs was made in 1893 by an Italian, Bizzozero,3 who presented his findings to the Royal Academy of Medicine of Turin. Further reports on microorganisms in the stomach followed by Gorham,4 Cowdry and Scott,5 and Freedberg and Barron.6H. pylori was identified in 1982 by an Australian physician, Marshall, and an Australian pathologist, Warren.7H. pylori was first morphologically classified as a Campylobacter spp. owing to its close resemblance to C. jejeni. In 1984, it was reclassified as a distinct new species, and named C. pyloridis, which was changed to C. pylori in 1987. In 1989, a different intracellular fatty acid composition from other Campylobacter spp. was observed, and it was reclassified as the genus, Helicobacter.1
H. pylori is a Gram-negative, spiral, motile and microaerophillic, gastric denizen.1 Its transmission is via the oral-oral or faecal-oral route.8 Several microbial factors, such as bacterial motility, adhesion mechanisms and urease production,1 enable H. pylori to colonise the stomach. The helical shape and unipolar flagella of H. pylori facilitate its movement through the viscous gastric mucous, and its escape from environmental toxins.9 The production of intracellular urease is responsible for maintaining the cytoplasmic and periplasmic pH, and is one of the most important survival mechanisms of H. pylori.1
The epidemiology of H. pylori indicates large geographical and age variations. Although it is estimated that more than half of the world's population is infected by H. pylori,10 the mainstay of the disease is in the Third World. The prevalence of H. pylori infection varies from 20-50% in developed countries, such as the USA, and from 50-90% in developing countries.4,11 The prevalence in the general population in South Africa varies from 51-71%.12
Study aim
It remains controversial whether or not healthcare workers on upper gastrointestinal endoscopy teams are at risk of H. pylori infection. An association between occupational exposure and an increased risk of infection has been shown in a number of studies,1,8,13-16 while such a risk was not confirmed in others.17,18 None of these studies were conducted in Africa.
The need for this study emanated from three variables:
- The risk of occupational transmission: Is the high prevalence of H. pylori in Africa resulting in an increased risk of the occupational transmission thereof?
- The lack of video instrumentation in developing countries: Redundant fibre-optic instruments (the old "eye scope") are still being used. This instrument brings endoscopists into close contact with patients' secretions.
- The unique composition of our local society: Societies with a very high and very low socio-economic status coexist in the same geographical area.
Method
Endoscopy personnel and healthcare workers not working in endoscopy units, with no prior history of H. pylori infection, were enrolled in this cross-sectional study (ECUFS Number 23/2014). The endoscopy group consisted of surgeons, gastroenterologists, endoscopy nurses and scope-cleaning personnel from the Universitas Tertiary Hospital, Pelonomi Tertiary Hospital and Life Rosepark Hospital, all situated in Bloemfontein. The control group consisted of doctors and nursing personnel not working in gastrointestinal endoscopy units. They were from the Universitas Tertiary Hospital and Pelonomi Tertiary Hospital, and were randomly recruited. Participants provided written informed consent to be included in the study.
One vial of whole blood was collected and submitted for serological testing for the presence of H. pylori immunoglobulin G (IgG), by means of an enzyme-linked immunosorbent assay (ELISA). The ELISA H. pylori IgG test was performed by the National Health Laboratory Service. The study was conducted over a period of four months.
Participants were divided into three groups comprising non-endoscopy users, endoscopy users performing 1-10 gastroscopies per week, and endoscopy users performing >10 gastroscopies per week for study data analysis purposes.
Data analysis was performed by the Department of Biostatistics, University of the Free State. The results were expressed as absolute frequencies and percentages. Categorical data were compared using Fisher's exact test. A 95% confidence interval (CI) was reported. A p-value of < 0.050 was considered to be significant.
Results
One hundred and two participants were enrolled in the study during the four-month period. Of these, 10 were excluded as six of the results were equivocal, and four specimens where haemolysed on arrival at the laboratory.
Data from the 92 study participants were included in the analysis. Of the 92 participants, the non-endoscopy group numbered 58 (63%), of whom 15 were male and 43 females. The endoscopy group numbered 34 (37%), of whom 21 were males and 13 females. Ages were distributed so that more endoscopy personnel than non-endoscopy personnel were > 40 years (p 0.002). The mean age of the participants in this study was 38.5 years.
A higher incidence of H. pylori was found in seropositive participants aged > 40 years (p 0.002).
The H. pylori seropositive rate was 59% in the endoscopy group and 55% in the non-endoscopy group (Table 1). The overall incidence of H. pylori (in both the study and control groups) was 57%. The difference between the endoscopy group and the total group was not significant (p 0.733).
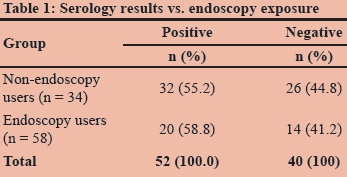

The spread of participants through the three groups was as follows:
- 58 non-endoscopy personnel (63%).
- 11 personnel performing 1-10 endoscopies per week (12%).
- 23 personnel performing > 10 endoscopies per week (25%).
The seropositive rate was highest in the group that performed > 10 endoscopies per week (Table 2).
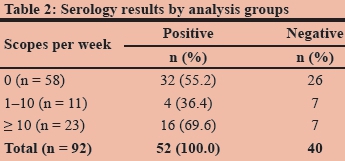
Positive antibody titres were reported in 32 (55%) participants in the control group (non-endoscopic personnel).
Four (36%) participants in the endoscopy user group performing 1-10 endoscopies per week tested seropositive. Sixteen (70%) participants in the endoscopy user group performing > 10 endoscopies per week tested seropositive (p 0.178).
Discussion
The results showed that the incidence of H. pylori infection between the two main groups was not significantly different, with an incidence of 59% in the endoscopy group, and an incidence of 55% in the control group (p 0.733). This correlates with the results obtained by Tanih et al.,12 who measured the national prevalence of H. pylori in South Africa to be 51-71%.
The outcome of this study was in keeping with the findings of Noone et al.,2 who reported no difference between the studied groups.
There was an increased incidence of H. pylori infection in participants with higher exposure to endoscopies, i.e. 55% in the control (non-exposure) group, compared to 70% in the group who performed > 10 endoscopies per week, but the difference was not statistically significant (p 0.178).
This was a negative study as we were unable to confirm that being part of an upper gastrointestinal endoscopy team was a risk factor for the acquisition of H. pylori.
However, this negative finding does not necessarily prove that it was not a risk factor. The reasons for this are as follows. This was not conducted as a cohort study, so there may have been a higher baseline prevalence of H. pylori infection in the control group. Also, statistical significance might be demonstrated in a larger study.
Conclusion
A significantly higher rate of H. pylori seropositivity in endoscopists could not be confirmed in this study, which may have been under-powered. A further study is needed to corroborate these findings.
REFERENCES
1. Stabile BE, Smith BR, Weeks DL. Helicobacter pylori infection and surgical disease: part 1. Curr Probl Surg. 2005;42(11):756-789. [ Links ]
2. Noone PA, Waclawski ER, Watt AD. Are endoscopy nurses at risk of infection with Helicobacter pylori from their work? Occ Med (Lond). 2006;56(2):122-126. [ Links ]
3. Bizzozero G. Ueber die Schlauchförmigen Drüsen des Magendarmkanals und die Beziehungen ihres Epithels zu dem Oberflächenepithel der Schleimhaut. Archiv fur mikroskopische. Anatomie. 1893;42:82-152. [ Links ]
4. Gorham FD. In discussion of the presence of spirochetes in human gastric mucosa. Am J Dig Dis. 1940;7:443-145. [ Links ]
5. Cowdry EV, Scott GH. Effect on monkeys of small doses of concentrated preparation of viosterol. Arch Pathol. 1936;22:1-23. [ Links ]
6. Freedberg AS, Barron LE. The presence of spirochaetes in human gastric mucosa. Am J Dig Dis. 1940;7:443-145. [ Links ]
7. Marshall BJ, Warren JR. Unidentified curved bacilli in the stomach of patients with gastritis and peptic ulceration. Lancet. 1984;1(8390):1311-1315. [ Links ]
8. Mastromarino P, Cattaruzza MS, Orsi GB. Helicobacter pylori infection among healthcare workers: further investigation is needed. J Hosp Infect. 2007;66(3):297-298. [ Links ]
9. Yoshiyama H, Nakazawa T. Unique mechanism of Helicobacter pylori for colonizing the gastric mucus. Microbes Infect. 2000;2(1):55-60. [ Links ]
10. Knigge KL. The role of H pylori in gastrointestinal disease. A guide to identification and eradication. Postgrad Med. 2001;110(3):71-82. [ Links ]
11. Torres J, Perez-Perez G, Goodman KJ, et al. A comprehensive review of the natural history of Helicobacter pylori infection in children. Arch Med Res. 2000;31(5):431-469. [ Links ]
12. Tanih NF, Okeleye BI, Ndip LM, et al. Helicobacter pylori prevalence in dyspeptic patients in the Eastern Cape Province - race and disease status. S Afr Med J. 2010;100(11):734-737. [ Links ]
13. De Schryver AA, van Hooste WL, van Winckel MA, van Sprundel MP. Helicobacter pylori infection: a global occupational risk for healthcare workers? Int J Occup Environ Health. 2004;10(4):428-432. [ Links ]
14. Birkenfeld S, Keter D, Dikman R, et al. Prevalence of Helicobacter pylori infection in health-care personnel of primary care and gastroenterology clinics. J Clin Gastroenterol. 2004;38(1):19-23. [ Links ]
15. Nishikawa J, Kawai H, Takahashi A, et al. Seroprevalence of immunoglobulin G antibodies against Helicobacter pylori among endoscopy personnel in Japan. Gastrointest Endosc. 1998;48(3):237-243. [ Links ]
16. Peters C, Schablon A, Harling M, et al. The occupational risk of Helicobacter pylori infection among gastroenterologists and their assistants. BMC Infect Dis. 2011;11:154. [ Links ]
17. Shelley KH, Haddadin AS. Is Helicobacter pylori infection an occupational hazard for anesthesiologists? Anesth Analg. 1998;87(4):973-974. [ Links ]
18. Braden B, Duan L, Caspary WF, Lembcke B. Endoscopy in not a risk factor for Helicobacter pylori infection - but medical practice is. Gastrointest Endosc. 1997;46(4):305-310. [ Links ]
 Correspondence:
Correspondence:
Theunis du Toit
theunis.du.toit@gmail.com














