Services on Demand
Article
Indicators
Related links
-
 Cited by Google
Cited by Google -
 Similars in Google
Similars in Google
Share
South African Journal of Surgery
On-line version ISSN 2078-5151
Print version ISSN 0038-2361
S. Afr. j. surg. vol.52 n.1 Cape Town Jan. 2014
VASCULAR SURGERY
The intramyocardial left anterior descending artery: Prevalence and surgical considerations in coronary artery bypass grafting
E A VankerI; N O AjayiII; L LazarusIII; K S SatyapalIV
IMB ChB, FRCS (Edin); St Augustine’s Hospital, Chelmsford Medical Centre, Durban, South Africa
IIMBBS, MMedSci; Department of Clinical Anatomy, School of Laboratory Medicine and Medical Sciences, College of Health Sciences, University of KwaZulu-Natal, Durban, South Africa
IIIBMedSci, MMedSci; Department of Clinical Anatomy, School of Laboratory Medicine and Medical Sciences, College of Health Sciences, University of KwaZulu-Natal, Durban, South Africa
IVLRCP, LRCS, LM, MD, FICA (USA), FRCP (Irel), LLM (Medical Law); Department of Clinical Anatomy, School of Laboratory Medicine and Medical Sciences, College of Health Sciences, University of KwaZulu-Natal, Durban, South Africa
ABSTRACT
BACKGROUND: Major coronary arteries usually have a subepicardial course and only dip into the myocardium near or at their termination. However, occasionally a segment of the epicardial artery may have an intramural course, and it is often referred to as a myocardial bridge. The left anterior descending (LAD) artery is the most commonly bridged vessel. Its prevalence has been evaluated at both autopsy and angiography. However, in the literature reviewed it is apparent that there are no reports of the prevalence of the intramyocardial LAD (IMLAD) artery in coronary artery bypass graft (CABG) series.
OBJECTIVES: To document the prevalence of the IMLAD artery in a series of CABGs and to describe the surgical techniques used in these cases.
METHODS: A retrospective analysis of 1 349 surgical reports of consecutive CABGs performed over a period of 23 years was conducted.
RESULTS: An IMLAD artery was present in 293 patients (21.7%). The prevalence was 20.2% (51/253) in females and 22.1% (242/1 096) in males. The IMLAD arteries extended into the interventricular septum in 3.8% (11/293) of the patients.
CONCLUSION: An intramyocardial course of the LAD artery is relatively common in patients undergoing CABG and poses a challenge in bypass grafting. Techniques are described to address this anatomical variation when it is encountered at surgery.
Major coronary arteries have a subepicardial course through subepicardial fat and only dip into the myocardium at or near their termination.[1-2] However, sometimes a variable segment of the epicardial artery can have a long intramural course or lie under a short band of cardiac muscle.[3-6] This anatomical arrangement has been variously described as an intramural coronary artery,[7] a submerged coronary artery,[8] a mural coronary artery,[3] a tunnelled artery[9] and, more commonly in anatomical descriptions, a coronary artery with a 'myocardial bridge' (MB).[8]
MBs were first recognised by Rayman in 1737, then by Black in 1805 (both cited by Ferreira et al.[10]) and were first described angiographically by Portman and Iwig in 1960 (cited by Loukas et al.[11]). The MB is considered to be a congenital anomaly by some authors, while others refer to it as an anatomical variant of a coronary artery.[12-16] The first in-depth autopsy analysis of MBs was done by Geiringer.[3] Clinically, the diagnosis is made by systolic 'milking' of the involved epicardial artery during coronary angiography,[4] due to transient compression of the vessel during systole. However, the present report excluded the short-bridged left anterior descending (LAD) artery where no occlusive lesion was demonstrated angiographically, and patients with symptoms resulting from systolic constriction of the vessel.
Myocardial infarction (MI) of the anterior cardiac wall is usually the consequence of disease in the LAD artery.[17] The LAD artery is most commonly situated intramuscularly, although other vessels may be involved.[10,11,18-20] Clinically, the LAD artery is the most important affected vessel,[10] and in view of the routine use of the left internal mammary artery (LIMA) to graft it, it presents specific challenges to the operating surgeon.
In their autopsy study, Ferreira et al.[10] distinguished two types of MBs, viz. superficial and deep. The superficial variation was situated in the interventricular groove and was crossed perpendicularly by muscle fibres. The deep variation had larger muscle bundles than the superficial one and was situated deep within the inter-ventricular septum. Geiringer[3] and Polacek[21] reported fewer atheromatous changes in the intramuscular arterial segment than in the subepicardial arterial segment. Ishii et al.[18] also observed that the intramuscular location influences the atherosclerotic disease process in the coronary artery. The MB is therefore regarded by some researchers as an uncommon cause of cardiac disease and considered as benign.[22,23] Conversely, there are reports suggesting that the myocardial bridging increases coronary artery spasm.[24] Furthermore, MBs may be a contributory factor in the development of MI,[7] cardiogenic shock after acute inferior MI,[25] unstable angina,[12] life-threatening cardiac arrhythmias[26] and sudden cardiac death.[14]
The intramyocardial LAD (IMLAD) artery poses difficulty in the localisation of the coronary artery at CABG for revasculari-sation,[27] and may complicate the procedure.[28] A review of the literature revealed no reports of the prevalence of IMLAD in a surgical series, which was the impetus for this study.
Objectives
The study aimed to record the prevalence and location of IMLAD arteries identified during CABG and to discuss the surgical techniques adopted to address this anatomical variation.
Methods
A retrospective analysis of 1 349 surgical reports of consecutive CABGs in a single surgical series performed over a period of 23 years was conducted. All the operations had been done by a single surgeon. Of the patients 1 096 (81.3%) were male and 253 (18.7%) female, and the age range was 23 - 82 years. The racial distribution was 17 black African (1.3%), 414 white (30.7%) and 918 Indian (68.7%). Clinical reports were accessed from databanks in the private sector in the Durban metropolitan region of KwaZulu-Natal, South Africa. Surgical notes were analysed for details of the prevalence and location (based on the classification of Ferreira et al.[10]) of MBs of the LAD artery and the surgical techniques used. All the cases had been reported by the single surgeon who had done the CABGs. The IMLAD artery was identified at surgery by not being visualised on the surface of the heart in almost its entire course. Short-segment bridged vessels with systolic constriction on angiograms were excluded from the study. Only cases in which more than 50% of the proximal length of the LAD was found to be intramuscular were included.
Results
Prevalence
An IMLAD artery was present in 293 patients (21.7%), with an age range of 23 - 78 years. The prevalence according to gender and race was as follows: 21.6% (51/253) in females and 22.9% (242/1 096) in males; and 29.4% (5/17) in black Africans, 24.1% (221/918) in Indians and 16.2% (67/414) in whites.
Location
The IMLAD arteries did not extend deep into the interventricular septum in 96.2% (282/293) of the cases reviewed (on the basis of the criteria described above), and were classified as superficial. The remaining 3.8% (11/293) were found to be deep in the interventricular septum. Of the patients in the latter group, two presented with poor ventricular function (ejection fraction 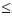 20%).
20%).
Surgical solutions employed
The IMLAD artery was located and grafted within the myocardium in 145 of the 293 cases. In the remaining 148, it was grafted distally where it was superficial and visible
Discussion
Myocardial bridging is generally an incidental finding during coronary angiographic studies, with a prevalence ranging from
0.5% to 36%,[4,5,12,24,27] although the prevalence can be as high as 90% - in autopsy series.[2,6,11] We recorded a prevalence of 21.7%, which is lower than the weighted mean of 50.7% for the prevalence of MBs at autopsy but higher than the weighted mean of 14.3% observed in the angiographic series (Table 1). The higher weighted mean prevalence of MB (50.7%) reported in the autopsy series is not surprising, since many patients with MBs are asymptomatic and therefore do not present for coronary angiography. Furthermore, superficial MBs were encountered more frequently than deep MBs, with prevalences of 96.2% and 3.8% recorded for superficial and deep MBs, respectively. This is comparable to the figures reported by Ferreira et al.[10] of 75% and 25% for superficial and deep MBs, respectively.
Hauser[29] suggested that congenital anomalies of the heart may be a factor predisposing to the early development of coronary artery disease (CAD), and as noted earlier, MBs may also be regarded as a congenital anomaly. In one patient with an MB, aged 23 years, the right coronary artery originated from the left coronary sinus. The combination of an MB and the congenital anomaly may in our view have been a factor predisposing to the early development of CAD in this patient.
When the LAD artery is buried in the myocardium for most of its course, locating the vessel can be very challenging and can translate into extended bypass time and a prolonged ischaemic interval during surgery.[30] In our series various surgical techniques were used to address this anatomical entity. The surgical strategy evolved over the period of this retrospective review. These techniques fall into two broad categories and are discussed as practised chronologically.
Locating the IMLAD artery and grafting it within the myocardium
In the early part of this series, the LAD artery was targeted by direct dissection into the overlying fat and myocardium. The incision was guided by the expected course of the vessel using three criteria:
- Using reference points distally (the visible terminal portion of the LAD artery) and proximally (the lateral edge of the main pulmonary artery), and appreciating that the bridged artery takes a straight course and lacks tortuosity.[31]
- Using the 'groove sign'. This refers to an epicardial groove that is said to lie directly over the LAD artery. It is anecdotally referred to as the ‘address’ for the vessel. This sign was found to be unreliable, as there are frequently several grooves in this epicardial territory. The validity of this sign forms part of an ongoing study.
- Using the 'vein sign'. Some surgeons believe that the IMLAD artery is directly below the anterior cardiac vein. This was used in eight cases, and was found to be useful in locating the artery. The validity of the relationship observed between vein and artery also forms part of an ongoing investigation.
The above technique using any of the reference points described has distinct disadvantages. Firstly, the right ventricular cavity may inadvertently be entered. In our series this occurred in three cases, all of which were safely repaired. Secondly, the myocardial incision is often accompanied by troublesome venous bleeding not always apparent in the arrested heart and difficult to control later. In the early part of the series, the epicardial edges around the LIMA pedicle were approximated to control venous bleeding. It was suspected that this method of controlling venous bleeding caused three cases of narrowing of the LIMA graft above the point of insertion found at re-study of these patients, who had recurrent symptoms.
Later in the series, the position of the intramuscular vessel was located with pinpoint accuracy. An incision was made over the terminal part of the LAD artery, close to the apex. A tiny 0.5 mm puncture of the vessel was made, and a malleable vascular probe inserted and directed proximally. The fat and myocardium overlying the vessel were incised directly onto the tip of the probe. The distal opening in the vessel was closed with a suture through the adventitia only. This took the guesswork out of locating the artery, but did pose the problem of venous oozing from the incised muscle, and involve the need to make an additional arterial incision.
Grafting the IMLAD artery distally, where it is superficial and visible
The problem here is that of adequate length of the LIMA pedicle. This is especially the case when the left lung is voluminous and crosses the midline. The problem of inadequate length was resolved in two ways:
- Earlier in the series, the LIMA pedicle was augmented by attaching a short length (usually 2 - 3 cm) of vein end-to-end to the artery, to create a variant of a composite arteriovenous graft. This experience is being separately documented, and longer-term follow-up data are being collected. A remarkable feature of cases that have been re-studied is the inability to differentiate the vein from the artery in terms of calibre.
- The currently preferred technique involves re-routing of the LIMA pedicle. In this method a shortened route for the LIMA pedicle is created, so that it can easily reach the distal point of insertion without tension. The parietal pericardium and parietal pleura, and the intervening thymus gland and mediastinal fat, are incised to a point 1 cm from the left phrenic nerve. The LIMA pedicle lies in this groove, medial to the lung, and is not stretched by the inflated lung, irrespective of its volume. This technique has made it unnecessary to dissect out the LAD from its deep position within the myocardium. Many re-studies of distal LIMA attachments to the LAD artery have been performed and the grafts were shown to be functioning well by providing prograde and retrograde blood flow.
During the 30-day follow-up period, which was complete in this series, the prevalences of postoperative bleeding and mortality were similar for the two surgical solutions employed.
Conclusion
An intramyocardial course of the LAD artery is not infrequent, as it was found in at least one in five surgical patients in the CABG series presented. The IMLAD artery may present the surgeon with technical challenges. Various surgical techniques used over the study period are described, and a simpler currently preferred technique is described, which is safer, more reproducible and quicker to execute than earlier methods.
REFERENCES
1. Standring S, Ellis H, Healy JC, et al. Gray's Anatomy. 39th ed. London: Churchill Livingstone, 2005:1014. [ Links ]
2. Edwards JC, Burnsides C, Swarm RL, Lansing AI. Arteriosclerosis in the intramural and extramural portions of coronary arteries in the human heart. Circulation 1956;13(2):235-241. [http://dx.doi.org/10.1161/01.CR.13.2.2.235] [ Links ]
3. Geiringer E. The mural coronary. Am Heart J 1951;41(3):359-368. [http://dx.doi.org/10.1016/0002-8703(51)90036-1] [ Links ]
4. Noble J, Bourassa MG, Petitclerc R, Dyrda R. Myocardial bridging and milking effect of the left anterior descending coronary artery: Normal variant or obstruction? Am J Cardiol 1976;37(7):993-999. [http://dx.doi.org/10.1016/0002-9149(76)90414-8] [ Links ]
5. Ge J, Erbel R, Rupprecht HJ, et al. Comparison of intravascular ultrasound and angiography in the assessment of myocardial bridging. Circulation 1994;89(4):1725-1732. [http://dx.doi.org/10.1161/01.CIR.89.4.1725] [ Links ]
6. Bandyopadhyay M, Das P, Baral K, Ckakroborty P. Morphlogical study of myocardial bridge on the coronary arteries. Indian J Thorac Cardivasc Surg 2010;26(3):193-197. [http://dx.doi.org/10.1007/s12055-010-0044-6] [ Links ]
7. Bourassa MG, Butnaru A, Lespérance J, Tardif J-C. Symptomatic myocardial bridges: Overview of ischemic mechanisms and current diagnostic and treatment strategies. J Am Coll Cardiol 2003;41(3):351-359. [http://dx.doi.org/10.1016/s0735-1097(02)02768-7] [ Links ]
8. Soran O, Pamir G, Erol C, et al. The incidence and significance of myocardial bridge in a prospectively defined population of patients undergoing coronary angiography for chest pain. Tokai J Exp Clin Med 2000;25(2):57-60. [ Links ]
9. Verma AK, Kumar S, Kumar N, et al. Myocardial bridge: Findings of postmortem heart. Indian Journal of Forensic Medicine and Pathology 2009;2(4):153-159. [ Links ]
10. Ferreira AG Jr, Trotter SE, König B, et al. Myocardial bridges: Morphological and functional aspects. Br Heart J 1991;66(5):364-367. [http://dx.doi.org/10.1136/Grt.66.5.364]. [ Links ]
11. Loukas M, Curry B, Bowers M, et al. The relationship of myocardial bridges to coronary artery dominance in the adult human heart. J Anat 2006;209(1):43-50. [http://dx.doi.org/10.1111/j.1469-7580.2006.00590.x] [ Links ]
12. Mookadam F, Green J, Holmes D, Moustafa S, Rihal C. Clinical relevance of myocardial bridging severity: Single center experience. Eur J Clin Invest 2009;39(2):110-115. [http://dx.doi.org/1111/5.1365-2362.2008.02073.x. [ Links ]]
13. Alegria JR, Herrmann J, Holmes DR Jr, Lerman A, Rihal CS. Myocardial bridging. Eur Heart J 2005;26(12):1159-1168. [http://dx.doi.org/10.193/eurheartj/ehi203] [ Links ]
14. Morales A, Romanelli R, Boucek R. The mural left anterior descending coronary artery, strenuous exercise and sudden death. Circulation 1980;62(2):230-237. [http://dx.doi.org/10.1161/01.CIR.62.2.230] [ Links ]
15. Akdemir R, Gunduz H, Emiroglu Y, Uyan C. Myocardial bridging as a cause of acute myocardial infarction: A case report. BMC Cardiovasc Disord 2002;2(15):1-5. [http://dx.doi.org/10.1186/1471-2261-2-15] [ Links ]
16. Loukas M, Groat C, Khangura R, Owens DG, Anderson RH. The normal and abnormal anatomy of the coronary arteries. Clin Anat 2009;22(1):114-128. [http://dx.doi.org/ 10.1002/ca.20761] [ Links ]
17. Hori M, Inoue M, Ohgitani N, et al. Site and severity of coronary narrowing and infarct size in man. Br Heart J 1980;44(3):271-279. [http://dx.doi.org/10.1136/hrt.44.3.271] [ Links ]
18. Ishii T, Hosoda Y, Osaka T, et al. The significance of myocardial bridge upon atherosclerosis in the left anterior descending coronary artery. J Pathol 1986;148(4):279-291. [http://dx.doi.org/10.1002/path.1711480404] [ Links ]
19. Kosi´ński A, Grzybiak M. Myocardial bridges in the human heart: Morphological aspects. Folia Morphol (Warsz) 2001;60(1):65-68. [ Links ]
20. Saidi H, Ongeti WK, Ogeng'o J. Morphology of human myocardial bridges and association with coronary artery disease. Afr Health Sci 2010;10(3):242-247. [ Links ]
21. Polacek P. Relation of myocardial bridges and loops on the coronary arteries to coronary occlusions. Am Heart J 1961;61(1):44-52. [http://dx.doi.org/10.1016/0002-8703(61)90515-4] [ Links ]
22. Tauth J, Sullebarger JT. Myocardial infarction associated with myocardial bridging: Case history and review of the literature. Cathet Cardiovasc Diagn 1997;40(4):364-367. [http://dx.doi.org/10.1002/(SICI)1097-0304(199704)40:4<364::AID-CCD9>3.0.CO;2-7] [ Links ]
23. Kramer JR, Kitazume H, Proudfit WL, Sones FM Jr. Clinical significance of isolated coronary bridges: Benign and frequent condition involving the left anterior descending artery. Am Heart J 1982;103(2):283-288. [http://dx.doi.org/10.1016/0002-9149(78)90890] [ Links ]
24. Teragawa H, Fukuda Y, Matsuda K et al. Myocardial bridging increases the risk of coronary spasm. Clin Cardiol 2003;26(8):377-383. [http://dx.doi.org/10.1002/clc.4950260806] [ Links ]
25. Yano K, Yoshino H, Taniuchi M, et al. Myocardial bridging of the LAD in acute inferior wall myocardial infarction. Clin Cardiol 2001;24(3):202-208. [http://dx.doi.org/10.1002/clc.4960240307] [ Links ]
26. Faruqui A, Maloy WC, Felner JM, et al. Symptomatic myocardial bridging of coronary artery. Am J Cardiol 1978;41(7):1305-1310. [http://dx.doi.org/10.1016/0002-9149(78)90890-1] [ Links ]
27. Irvin RG. The angiographic prevalence of myocardial bridging in man. Chest 1982;81(2):198-202. [http://dx.doi.org/10.1378/chest.81.2.198] [ Links ]
28. Trivellato M, Angelini P, Leachman RD. Variations in coronary anatomy: Normal versus abnormal. Cardiovascular Diseases, Bulletin of the Texas Heart Institute [ Links ]
29. Hauser M. Congenital anomalies of the coronary arteries. Heart 2005;91(9):1240- 1245. [http://dx.doi.org/10.1136/hrt.2004.057299] [ Links ]
30. Topol EJ, Califf RM, Isner J, et al. Textbook of Cardiovascular Medicine. Philadelphia: Lippincott Williams & Wilkins, 2002. [ Links ]
31. Lachman N. A clinically applied anatomical study of the coronary arteries in the South African population. PhD dissertation in Anatomy, University of KwaZulu-Natal, 2003. [ Links ]
32. Lee SS, Wu TL. The role of the mural coronary artery in prervention of coronary arteriosclerosis. Arch Pathol 1972;93(1):32-35. [ Links ]
33. Wymore P, Yedlicka JW, Garcia-Medina V, et al. The incidence of myocardial bridge in heart transplants. Cardiovasc Intervent Radiol 1989;12(4):202-206. [http://dx.doi.org/10.1007/BF02577154] [ Links ]
 Corresponding author:
Corresponding author:
K S Satyapal
(satyapalk@ukzn.ac.za)














