Services on Demand
Article
Indicators
Related links
-
 Cited by Google
Cited by Google -
 Similars in Google
Similars in Google
Share
South African Journal of Surgery
On-line version ISSN 2078-5151
Print version ISSN 0038-2361
S. Afr. j. surg. vol.52 n.1 Cape Town Jan. 2014
PAEDIATRIC SURGERY
The role of limb perfusion studies in the paediatric ischaemic limb
A BrinkI; S CoxII; M D MannIII; H RodeIV
IMB ChB, MMed (Nucl Med); Department of Paediatrics and Child Health (Nuclear Medicine), Faculty of Health Sciences, University of Cape Town and Red Cross War Memorial Children's Hospital, Cape Town, South Africa
IIMB ChB, FCS (SA), Cert Paed Surg (SA); Department of Paediatric Surgery, Faculty of Health Sciences, University of Cape Town and Red Cross War Memorial Children's Hospital, Cape Town, South Africa
IIIMB ChB, MMed (Paed), MMed (Nucl Med), PhD; Department of Paediatrics and Child Health (Nuclear Medicine), Faculty of Health Sciences, University of Cape Town and Red Cross War Memorial Children's Hospital, Cape Town, South Africa
IVMB ChB, MMed (Surg), FRCS, FCS (SA); Department of Paediatric Surgery, Faculty of Health Sciences, University of Cape Town and Red Cross War Memorial Children's Hospital, Cape Town, South Africa
ABSTRACT
OBJECTIVES: To study the use of limb perfusion scans in children with limb-threatening ischaemia and determine whether such scans are helpful in making clinical decisions.
METHODS: This retrospective study compared the clinical, scan and surgical findings in children who had limb perfusion scans for critical limb ischaemia at Red Cross War Memorial Children's Hospital, Cape Town, South Africa, from July 2001 to December 2010. Records were reviewed and the data analysed for aetiology, clinical findings, limb perfusion results, operative findings and outcome.
RESULTS: There were complete clinical and scan records for 20/22 patients, aged 1 month to 12 years. The causes of limb ischaemia were meningococcal septicaemia (n=9), septic shock (n=6), hypovolaemic shock due to gastroenteritis (n=4), and electrical burns (n=1). The clinical, scan and surgical findings correlated in 40/48 imaged limbs. In one leg the findings did not correlate, but the perfusion scan results predicted the outcome. In the remaining seven cases the exact correlation was uncertain owing to technical difficulties or absent operative notes.
CONCLUSION: This study describes a method for performing limb perfusion studies in children. Limb perfusion studies correlated well with surgical findings. These studies were useful in treatment decisions, parent and patient counselling and surgical planning. They supplemented clinical examination in assessment of the children.
In the child with a strong indication of progressive ischaemic changes in a limb such as the disappearance of arterial pulses and severe limb pain on passive extension, limb perfusion scans have been used as a supplement to clinical judgement to determine the area of demarcation between the viable and non-viable tissue. Clinical assessment cannot always determine the extent of the skin, subcutaneous tissue, muscle or bone necrosis accurately. Limb perfusion studies are valuable in delineating the level of impaired tissue perfusion.
Limb perfusion studies at our institution were born out of necessity more than 20 years ago to supplement clinical assessment of tissue viability and aid surgical planning and decision making in extremely ill children with critical impairment to the distal limb areas. The children had severe meningococcal, staphylococcal or streptococcal sepsis, gastroenteritis or injury from electrical burns.
Patients and methods
Since 2001 the raw data of all studies performed at Red Cross War Memorial Children's Hospital, Cape Town, South Africa, have been stored in an electronic archive and are available for review. The Nuclear Medicine database, which contains details of all investigations performed and reports issued, was searched for patients who had limb perfusion studies between July 2001 and December 2010.
In all patients referred for limb perfusion studies, critical ischaemia was deemed clinically present but the combination of clinical and Doppler signs did not correlate or the exact Rutherford classification of ischaemia was difficult to determine, often as a result of the cutaneous manifestations of the underlying condition. None of the patients included underwent angiography, as the ischaemia was thought to be related to small-vessel disease, and in many of the smaller patients with multiple limb involvement arterial puncture could have worsened the condition.
One patient was imaged using 99mTc sodium pertechnetate. All the other patients were scanned using 99mTc methylene diphosphonate (99mTc MDP). The dose of pertechnetate was calculated according to the recommended cardiac first-pass dose on the 1990 EANM dose card[1] until mid-2008, after which the new EANM dose card (version 1.5.2008)[2] was used. The minimum dose was 50 MBq and the maximum 400 MBq.
All the studies were recorded on a Philips Axis Dual Head camera, previously known as Picker and then Marconi (Koninklijke Philips Electronics NV, Milipitas, Calif., USA), using a low-energy high-resolution collimator.
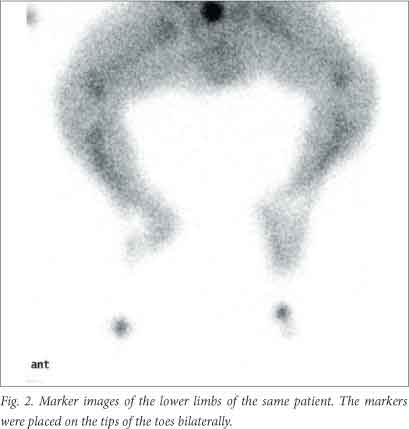
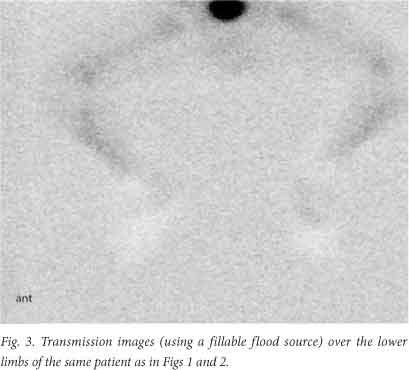
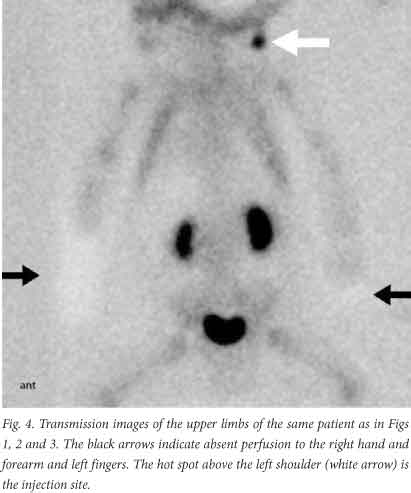
Before imaging was started, the radiographer verified with a marker that the areas of concern were in the field of view. Anterior and posterior perfusion images of the area of interest were recorded simultaneously at 2 seconds a frame for 2 minutes. Immediately after the perfusion study, blood pool images of the areas of interest were obtained for 300 seconds per image with an appropriate zoom (Fig. 1). Once the initial blood pool images were recorded, they were followed by marker (Fig. 2) and transmission images (Figs 3 and 4). A fillable flood source, containing 150 MBq 99mTc sodium pertechnetate in water, was used for the transmission images. The transmission images helped delineate areas of non-perfusion. If indicated by the initial findings and clinical question, and if the patient was stable enough to be moved for a second set of images, a delayed whole-body bone scan was recorded 2 hours after the 99mTc MDP injection.
All the patients were severely ill and most were sedated and on ventilator support at the time of the study.
Scans were reported by visual inspection. In addition, measurements of the demarcations between perfused and non-perfused areas were made using fixed landmarks such as the closest intact growth plate as the proximal reference point and the line of demarcation in uptake as the distal point. In most cases, images and scan findings were discussed with the operating surgeon during the scan.
We reviewed the clinical notes, raw data and reports of all patients and correlated clinical, scan and surgical findings.
Ethics approval was obtained from the Human Research Ethics Committee, Faculty of Health Sciences, University of Cape Town.
Results
A total of 22 children were referred for limb perfusion studies between July 2001 and December 2010. The clinical notes on two patients were not available, leaving 20 in whom the clinical, scan and surgical findings could be reviewed.
The causes of the limb ischaemia were meningococcal septicaemia in nine cases, septic shock in six, hypovolaemic shock due to gastroenteritis in four and electrical burns in one. The ages of the patients ranged from 1 month to 12 years, with the median age at scan being 7 months. The interval between admission and scintigraphy ranged from 0 to 29 days with a median of 9 days.
Fig. 5 summarises the results. Ischaemia was suspected clinically in 48 of the limbs imaged and confirmed on imaging in 47. In one patient, a 12-year-old girl with septic shock due to missed appendicitis, the scan showed decreased but present perfusion despite severe ischaemia on clinical examination including absent pulses and absent flow on Doppler ultrasound (Fig. 6).
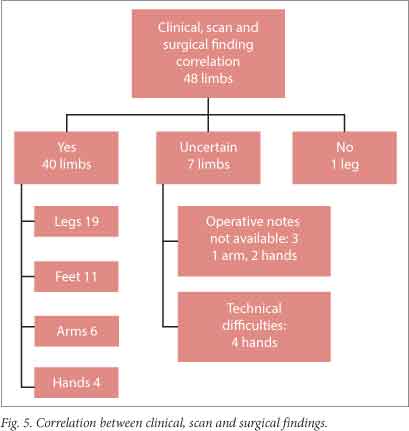
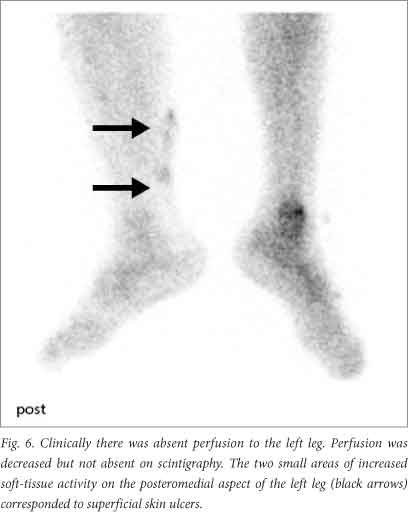
In two of the patients surgery was not performed. The scan findings influenced the decision to opt for conservative management in both. They aided the decision to withdraw active treatment in a 7-month-old baby with meningococcal septicaemia, extensive four-limb involvement and neurological damage. In the other, discussed above, conservative treatment was continued and amputation of a leg avoided based on the perfusion findings alone (Fig. 6). The remaining 18 patients proceeded to surgery.
In all cases discussed below, tissue showing no perfusion on the scan was found to be clinically necrotic, while areas showing reduced but present perfusion were found at surgery to be viable. Sixteen patients had surgical intervention in one or both lower limbs. In two cases (three legs) the scanned level of perfusion correlated with the extent of necrosis found at surgery, but the level of amputation had to be higher for anatomical and functional reasons. In the remaining 14 patients (28 lower limbs) the scan findings correlated with the eventual clinical outcome. In 22 of the legs with ischaemia, the scan identified the exact level of necrosis found at surgery. In another three, the scan abnormalities coincided with the clinical presence of dry gangrene of toes and the digits were allowed to auto-amputate. There was no clinical suspicion of ischaemia in three legs, and on scintigraphy perfusion of these limbs was normal.
Five of the patients requiring surgery had ischaemia of one or more arms. In four patients (six imaged arms) the clinical, scan and surgical findings correlated very well, but in one the level of amputation needed to be higher than the level of perfusion because of damage to the neurovascular bundle in the arm. In the fifth patient, the clinical and scan findings correlated but the subsequent surgical procedures were performed at another hospital and the surgical notes were not available for correlation.
In seven patients there was ischaemic involvement of ten hands. In four hands the scan, clinical and surgical findings correlated. In two hands the clinical outcome and scan findings correlated, but there was not enough information in the local operative notes to correlate the surgical findings as orthopaedic procedures were performed elsewhere. In four hands, technical difficulties decreased the quality of the scan. One hand was heavily bandaged and the fingers could not be extended from the hand. In one patient there was an interstitial injection in one of the hands and the image could not be interpreted owing to the extravasation of activity in that hand. In one patient both hands had developed flexion deformities of the fingers by the time the scan was performed.
Discussion
Limb perfusion studies using pertechnetate have been described in the literature since the 1980s.[3] Limb perfusion studies using 99mTc hydroxymethylene diphosphonate (HMDP) to give prognostic information, establish the time limits for amputation and help determine the level of amputation were well described by Cauchy et al.[4] in a large adult group of patients suffering from frostbite. Frostbite lesions with no uptake on bone scan require amputation, areas with normal or increased uptake recover, and most areas of low uptake ultimately recover. Overall absent uptake on bone scanning has a strong correlation with later amputation, with a specificity of 99%, sensitivity of 96% and positive predictive value of 92%. Normal or increased uptake is an indicator of later healing with a negative predictive value of 99%.
In contrast, a prospective study by Bhatnagar et al.[5] on 20 adults with mild to moderate frostbite found that patients with chronic stable ischaemia and fibrotic digits had absent perfusion to these digits on a perfusion study using 99mTc sodium pertechnetate. In this study population, patients with severe ischaemia were not included as they had immediate amputation. The authors concluded that doing the same study using a bone agent would probably have yielded different results, as tissue with no blood flow or blood pool activity but uptake on the delayed bone scan images would represent viable tissue.
The use of 99mTc MDP in adult patients with high-voltage electrical burns has also been described.[6] Electrical burns are known to cause deep-seated damage to muscle and underlying tissue with limited burns in the corresponding skin. The lack of clinical evidence of the deeper burn wounds makes identification of the site and estimation of the exact extent of the subcutaneous damage difficult, but blood flow, blood pool and delayed images correlate well with the level of amputation required.
In a recent study,[7] limb perfusion studies using 99mTc pyrophosphate (99mTc PYP) were performed on 11 adult patients, eight with high-voltage injuries, one with frostbite and two with soft-tissue infections. In the patients who underwent amputation, the amputation margins were correlated pathologically with the scintigraphic findings and the authors found a very good correlation. In this small study sample, the accuracy of 99mTc PYP was 96%, the sensitivity 94% and specificity 100%.
Previously our institution described a case where a limb perfusion study altered the decision regarding surgery on a child with meningococcal septicaemia.[8] The child had extensive necrosis involving 85% of her total body surface area, including both legs up to the knees. Initially amputations of the lower limbs were contemplated, but the limb perfusion scan demonstrated perfusion to the affected limbs. Limb preservation surgery was performed and the patient recovered with reasonable locomotive activity.
Harley et al.[9] describe the case of a 3-year-old girl with meningo-coccal septicaemia who had a bone scan prior to amputation. Both forearms were fashioned beyond the level of viability shown on the bone scan, and these amputations needed to be revised proximally.
The pathophysiology leading to limb ischaemia involves bacterial toxins activating the complement cascade, resulting in disseminated intravascular coagulation, microvascular thrombosis and resulting poor tissue perfusion. This is compounded by low cardiac output from septicaemic shock[10] and dehydration in patients with gastroenteritis. Progressive peripheral ischaemia sets in, often progressing more proximally when inotropes are used. While the intensive care management priorities are to optimise the metabolic parameters, the musculoskeletal priorities, which are not a primary concern,[10] are to preserve any viable tissue and prevent soft-tissue infection.[11]
The combination of small-vessel thrombosis, vasculitis and generalised coagulopathy results in a clinical picture of ischaemia, and on clinical examination it is extremely difficult to discriminate between definitely necrotic tissue and tissue that may potentially survive.[11] All patients referred for limb perfusion studies were those in whom the combination of clinical and Doppler signs did not correlate or the exact Rutherford classification of ischaemia was difficult to determine. With the median age being 7 months, and the majority of patients being intubated, ventilated and paralysed, muscular and sensory levels are difficult to determine. In addition, while critical ischaemia was deemed clinically present in all cases, the exact level of viable tissue was difficult to determine, often owing to the cutaneous manifestations of the underlying condition.
While the role of fasciotomy in such patients remains a topic in the recent literature,[12,13] there are few papers focusing on clinical findings and investigations helpful in determining the level of necrotic tissue. Many papers and protocols rely on clear demarcation of necrotic, mummified tissue prior to amputation,[11,14,15] stating that early amputation does not appear to be an option.[12] Demarcation may take several weeks, and while it is true that as the tissue involved is not perfused reperfusion injury and secondary infection may not often be a clinical problem,[11] the time spent waiting for such demarcation delays the healing and rehabilitation process and commits the child to a longer period of hospitalisation.
Performing early amputation has its own pitfalls, however, the most important being the potential to excise tissue that may eventually recover. Preservation of all functional tissue is of paramount importance for functional, reconstructive and aesthetic outcomes. A carefully planned and expertly carried out amputation is preferable to an unplanned operation. For these reasons, the use of perfusion scans was considered in our institution. They were performed on haemodynamically stable patients after the initial period of intensive treatment, at a median of 9 days after admission. The concept was to evaluate perfusion in the limbs and determine the levels relative to various landmarks. This study aimed to evaluate these scans to determine the degree of correlation of the scan with clinical and intra-operative findings to assess whether perfusion scans are indeed an investigation that could aid in clinical decision making. Patients scanned included those who had undergone prior facsciotomies and those who had not.
Several radiopharmaceuticals can be used to assess perfusion scintigraphically. The perfusion and early blood pool images recorded after the injection of 99mTc sodium pertechnetate and 99mTc MDP provide the same information. Initially we used 99mTc sodium pertechnetate for imaging limb perfusion studies. Later it was found that using 99mTc MDP gave more imaging options, as one could proceed to record 2- to 3-hour images that gave additional information such as the extent of tissue with decreased uptake and sites of possible osteomyelitis. Delayed images were recorded in only six patients. The decision to perform delayed images was made on a case-to-case basis depending on the exact clinical question and the findings of the initial perfusion images as well as the clinical condition of each patient. Most patients were gravely ill, and moving them from the intensive care unit to the nuclear medicine department was limited to the absolute minimum.
It was useful to use fixed landmarks such as growth plates to measure the length of viable tissue. We strongly advocate that studies are reviewed jointly by the nuclear physician and the surgeon who will perform the surgery while planning the surgery.
The scans correlated very well with clinical and surgical findings in the larger body parts, legs, arms, hands and feet in identifying ischaemic tissue (Fig. 4). There were no instances of the scan showing perfusion in tissue shown to be necrotic at surgery. In most cases the surgical outcome correlated with the scan findings. In four cases the nature of the soft-tissue damage, while correlating with the scan results, required a higher level of amputation to achieve a functional outcome or wound closure. There were no cases in which repeat amputation was required because of inadequate initial amputation through residual necrotic tissue, as is described in other papers on meningococcal septicaemia.[15,16]
Although limb perfusion studies, including imaging of digits, are well described in adults with frostbite,[4] we had difficulty in imaging digits and in interpreting perfusion defects in the digits. There were numerous reasons for this. In one case there was a technical problem with an interstitial injection in the hand. In another, the patient had developed flexion deformities of the hands and the fingers could not be imaged. In a third case the hand was extensively bandaged and the fingers could not be extended.
It should be kept in mind that the primary focus of the scintigraphy was to aid in planning surgery, and no dedicated images were recorded of digits that had already developed dry gangrene. It must also be noted that the average digit of a small child is at the limits of resolution for a gamma camera.
Conclusion
We found that limb perfusion studies in children presenting with limb-threatening ischaemia correlated well with surgical findings. These studies were useful in treatment decisions, parent and patient counselling and surgical planning. We believe that limb perfusion scans are sufficiently sensitive to allow early amputation with the assurance that potentially viable tissue is not being sacrificed. In addition to clinical, Doppler and angiography studies, limb perfusion scans should be considered as a further method of assessment of ischaemic limbs.
REFERENCES
1. Piepsz A, Hahn K, Roca I, et al. A radiopharmaceuticals schedule for imaging in paediatrics. Paediatric Task Group European Association of Nuclear Medicine. Eur J Nucl Med 1990;17(3-4):127-129. [http://dx.doi.org/10.1007/bf00811439] [ Links ]
2. Jacobs F, Thierens H, Piepsz A, et al. Optimized tracer-dependant dosage cards to weight-independent effective doses. Eur J Nucl Med Mol Imaging 2005;32(5):581-588. [http://dx.doi.org/10.1007/s00259-004-1708-5] [ Links ]
3. Salimi Z, Vas W, Tang-Barton P, Eachenpati RG, Morris L, Carron M. Assessment of tissue viability in frostbite by 99mTc pertechnetate scintigraphy. AJR Am J Roentgenol 1984;142(2):415-419. [http://dx.doi.org/10.2214/ajr.142.2.415] [ Links ]
4. Cauchy E, Chetaille E, Lefevre M, Kerelou E, Marsigny B. The role of bone scanning in severe frostbite of the extremities: A retrospective study of 88 cases. Eur J Nucl Med 2000;27(5):497-502. [http://dx.doi.org/10.1007/s002590050534] [ Links ]
5. Bhatnagar A, Sarker BB, Sawoop K, Chopra MK, Sinha N, Kashyap R. Diagnosis, characterisation and evaluation of treatment response of frostbite using pertechnetate scintigraphy: A prospective study. Eur J Nucl Med Mol Imaging 2002;29(2):170-175. [http://dx.doi.org/10.1007/s00259-001-0658-4] [ Links ]
6. Kao PF, Tzen KY, Chang LY, You DL, Yang YI. 99Tcm-MDP scintigraphy in high-voltage electrical burn patients. Nucl Med Commun 1997;18(9):846-852. [http://dx.doi.org/10.1097/00006231-199709000-00008] [ Links ]
7. Affleck DG, Edelman L, Morris S, Saffle JR. Assessment of tissue viability in complex extremity injuries: Utility of the pyrophosphate nuclear scan. J Trauma 2001;50(2):263-269. [http://dx.doi.org/10.1097/00005357-200102000-00011] [ Links ]
8. Numanoglu A, Bickler SW, Rode H, Bosenberg AT. Meningococcal septicaemia complications involving skin and underlying deeper tissues - management considerations and outcome. S Afr J Surg 2007;45(4):142-146. [ Links ]
9. Harley OJ, Ahmed OA, Ng RL. Imaging to guide amputation of necrotic limbs in paediatric patients with meningococcal septicaemia. Br J Plast Surg 2004;57(2):174-175. [http://dx.doi.org/10.1016/j.bjps.2003.11.016] [ Links ]
10. Boeckx WD, Nanhekhan L, Vos GD, Leroy P, Van den Kerckhove E. Minimizing limb amputations in meningococcal sepsis by early microsurgical arteriolysis. J Pediatr Surg 2009;44(8):1625-1630. [http://dx.doi.org/10.1016/j.jpedsurg.s007.12.060] [ Links ]
11. Monsell F. The skeletal consequences of meningococcal septicaemia. Arch Dis Child 2012;97(6):539-544. [http://dx.doi.org/10.1136/archdischild-2011-30/284] [ Links ]
12. Davies MS, Nadel S, Habibi P, Levin M, Hunt DM. The orthopaedic management of peripheral ischaemia in meningococcal septicaemia in children. J Bone Joint Surg Br 2000;82(3):383-386. [http://dx.doi.org/10.1302/0301-620x82b3.9887] [ Links ]
13. Potokar TS, Oliver DM, Ross Russell R, Hall PN. Meningococcal septicaemia and plastic surgery - a strategy for management. Br J Plast Surg 2000;53(2):142-148. [http://dx.doi.org/10.1054/bjps.1999.3249] [ Links ]
14. Huang DB, Price M, Pokorny J, Gabriel KR, Lynch R, Paletta CE. Reconstructive surgery in children after meningococcal purpura fulminans. J Pediatr Surg 1999;34(4):595-601. [http://dx.doi.org/10.1016/s0022-3468(99)90082-9] [ Links ]
15. Wheeler JS, Anderson BJ, de Chalain TM. Surgical interventions in children with meningococcal purpura fulminans - a review of 117 procedures in 21 children. J Pediatr Surg 2003;38(4):597-603. [http://dx.doi.org/10.1053/jpsu.2003.50130] [ Links ]
16. Genoff MC, Hoffer MM, Achauer B, et al. Extremity amputations in meningococcemia-induced purpura fulminans. Plast Reconstr Surg 1992;89(5):878-881. [http://dx.doi.org/10.1097/00006534-199205000-00015] [ Links ]
 Corresponding author:
Corresponding author:
A Brink
(anita.brink@uct.ac.za)














