Servicios Personalizados
Articulo
Indicadores
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares en Google
Similares en Google
Compartir
South African Journal of Surgery
versión On-line ISSN 2078-5151
versión impresa ISSN 0038-2361
S. Afr. j. surg. vol.52 no.1 Cape Town ene. 2014
GENERAL SURGERY
Lessons from emergency laparotomy for abdominal tuberculosis in the HIV/AIDS era
J IslamI; D L ClarkeII; S R ThomsonIII
IMB BS, FCS (SA), Cert Vasc Surg (SA), MMedSci; Department of Surgery, Edendale Hospital and Faculty of Health Sciences, Nelson R Mandela School of Medicine, University of KwaZulu-Natal, Pietermaritzburg, South Africa
IIMB ChB, FCS (SA), MMedSci; Department of Surgery, Edendale Hospital and Faculty of Health Sciences, Nelson R Mandela School of Medicine, University of KwaZulu-Natal, Pietermaritzburg, South Africa
IIIChM, FRCS (Eng & Edin); Department of Surgery, Edendale Hospital and Faculty of Health Sciences, Nelson R Mandela School of Medicine, University of KwaZulu-Natal, Pietermaritzburg, South Africa
ABSTRACT
BACKGROUND: The rising incidence of HIV/AIDS has resulted in a resurgence of abdominal tuberculosis (TB) in HIV-positive patients in South Africa. These often debilitated patients frequently present with acute complications requiring surgery.
METHODS: A prospective audit of all patients with abdominal TB undergoing emergency laparotomy was conducted. From January 2008 to June 2010, 49 patients had emergency laparotomy and specimens obtained from them were diagnostic of TB. Twenty-five were males and 24 females, with a median age of 32 years (range 2 - 62). Thirty-nine patients were HIV-positive (79.6%).
RESULTS: Intra-operative findings were bowel perforations in 13 cases, small-bowel obstruction in seven, a frozen abdomen in ten, and enlarged lymph nodes and an ileocaecal mass in 19. Eleven patients (22.4%) underwent small-bowel resection and eight (16.3%) right hemicolectomy. Eighteen patients (36.7%) ended up with stomas, 14 (28.6%) had re-laparotomies, and 18 (36.7%) were admitted to the intensive care unit. Twenty-three patients (46.9%) required blood transfusion and 15 (30.6%) total parenteral nutrition. Three patients (6.1%) developed an enterocutaneous fistula and 19 (38.8%) died. Pre-operative illness severity indices of acidosis, anaemia and hypo-albuminaemia were significant predictors of death, but mode of presentation and surgical interventions were not.
CONCLUSION: Laparotomy as currently practised for the 'acute abdomen' in patients with suspected HIV and abdominal TB is associated with very high morbidity and mortality, which is related to pre-operative severity indices. More liberal use of imaging may define cases in which a more conservative approach could improve outcome.
South Africa (SA) has a quarter of the HIV/AIDS disease burden in sub-Saharan Africa and a sixth of the global burden.[1] Approximately 80% of patients with tuberculosis (TB) in SA are HIV-positive, and - these co-infected individuals are more likely than HIV-negative TB patients to have smear-negative pulmonary or extrapulmonary TB.[2] Abdominal TB is the sixth most common site of extrapulmonary TB, in the range of 11 - 16%,[3,4] and is difficult to diagnose clinically. It has been reported that the hospital prevalence of HIV infection in the adult surgical population in SA is as high as 39%.[5] These statistics attest to the increasing burden of the disease in our institutions. Patients frequently present with features of an acute abdomen on the background of chronic illness. In this heterogeneous group of patients laparotomy is performed primarily to treat the acute abdomen and secondarily to establish the diagnosis. We decided to carry out an institutional analysis of the outcome of emergency laparotomy for abdominal TB in a population with a high prevalence of HIV/AIDS.
Methods
A prospective database was maintained of all patients with suspected and confirmed abdominal TB from January 2008 to June 2010. Those who underwent an emergency laparotomy and had - histopathologically or microbiologically proven TB were analysed and followed up during the study period and their outcomes were evaluated. The study was conducted at Edendale Hospital (EH), Pietermaritzburg, an 860-bed district and regional hospital in a semi-urban area in the province of KwaZulu-Natal, SA, which serves a mainly black African population of 1.6 million people. EH is also a referral centre for TB patients from local clinics and district hospitals. The study was approved by the EH Ethics Committee and the Biomedical Research Ethics Committee of the University of KwaZulu-Natal.
Statistical analysis
Descriptive statistics were used. Demographic data were expressed as means with 95% confidence intervals (CIs). In the case of quantitative data, means and 95% CIs were reported around sample estimates. Fisher's exact test (two-tailed) was used for differences in proportions. A p-value of  0.05 was considered significant.
0.05 was considered significant.
Results
From January 2008 to June 2010, 190 patients with suspected abdominal TB were identified. In 49 cases the diagnosis was confirmed histologically from specimens obtained at emergency laparotomy: there were 25 males and 24 females, median age 32 - years (range 2 - 62). There were four children, aged 2, 2, 9 and 11 years. Thirty-nine patients were HIV-positive (79.6%), two were HIV-negative, and the rest refused testing. CD4+ counts were known in seven patients (mean 91 cells/ìl; range 17 - 200), eight patients were on antiretroviral therapy, and four patients were already on empirical TB therapy. The median hospital stay was 14 days (range 8 - 28).
Thirty-seven patients (75.5%) presented with abdominal pain, distension, vomiting and signs of peritonism. Twelve patients (24.5%) presented predominantly with features of bowel obstruction, i.e. abdominal pain, distension and constipation.
All the patients had a chest radiograph. Free air under the diaphragm was present in nine, and four had pulmonary infiltrates suggestive of TB. Abdominal radiographs showed dilated loops of bowel suggestive of bowel obstruction in 12 cases. Six patients had a computed tomography (CT) scan: three showed features of bowel perforation, and the rest showed mesenteric lymphadenopathy, free fluid and evidence of bowel wall thickening. The mean haemoglobin level was 8.8 g/dl (range 6 -11.8); 23 patients had a haemoglobin level of <8 g/dl and received blood transfusions. Arterial blood gas measurement identified 22 patients with metabolic acidosis. The mean serum albumin level was 13 g/l (range 8 - 32). Fifteen patients required total parenteral nutrition (TPN).
The operative findings, procedures and outcomes are detailed in Table 1. Bowel perforations occurred in 26.5%, most commonly of the ileum. Of the 73.5% with obstructive symptoms, the majority had enlarged mesenteric lymph nodes, seven had a clear-cut level of obstruction, and the remainder had a'frozen' abdomen. Eleven small-bowel resections and eight right hemicolectomies were performed. The rest of the patients had only lymph node or omental biopsies. Eighteen patients (36.7%) ended up with stomas, but only two had a primary bowel anastomosis.
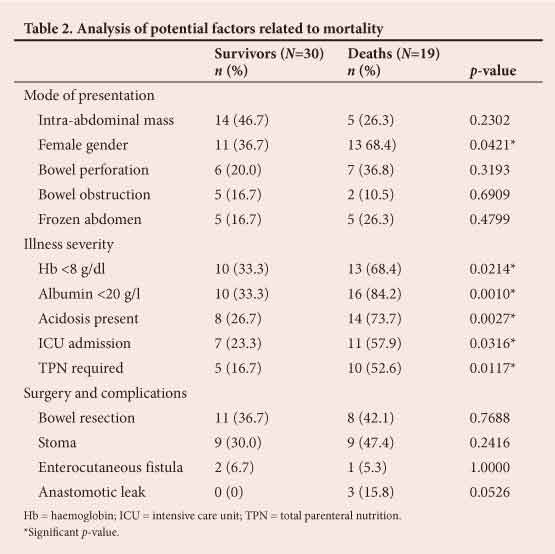
Of the 18 patients (36.7%) who were admitted to the intensive care unit (ICU), 14 required re-laparotomy, with ten patients returning to theatre on two or more occasions. Ten patients were discharged - with a stoma and five with ventral hernias. Septic morbidity was associated with three enterocutaneous fistulas and three anastomotic leaks. Seventeen of the 19 patients who died were HIV-positive and included two children. Table 2 analyses the factors potentially associated with death. Female gender and the pre-operative severity indices acidosis, anaemia, hypo-albuminaemia, TPN requirement and ICU admission were significant predictors of death. Mode of presentation, surgical interventions and complications did not predict mortality. Follow-up was very poor. Only 12 of the survivors could be contacted telephonically after their initial postoperative surgical review. They were well and receiving their TB medications. Two underwent uncomplicated closure of their stomas.
Discussion
The number of patients with abdominal TB appears to be increasing. This is evidenced by an earlier publication from a sister institution in the same province documenting a series of 67 patients with abdominal TB.[6] In this series 34% of the patients were HIV-positive, and in the remainder their HIV status was unknown. Most of the patients (79.6%) in our series were HIV-positive. Several series have failed to report on HIV status,[7-91 but reports from Zambia,[10] Nigeria[11] and India[12] indicate abdominal TB and HIV co-infection rates of 16%, 14% and 50%, respectively. However, none of these series included any patients who underwent laparotomy. Similar to other series,[7,13] our patients were generally in their 4th decade with only 10% aged <20 years. Only four patients (8.2%) in our series had radiological features of pulmonary TB, which is half that reported by others.[6,14]
Small-bowel stricturing was the most common finding (50%) reported by Baloch et al.[8] and Akbar et al.,[9] but only 14% of our patients presented with a bowel obstruction secondary to a discrete stricture. Baloch et al.[8] and Akbar et al.[9] performed stricturoplasty in 48% and 36% of cases, respectively. Stricturoplasty was not performed at all in our series as oedematous bowel and systemic hypo-albuminaemia in our patients made it clinically unsafe. For similar reasons we were reluctant to perform primary anastomosis (4.1%) which is in stark contrast to the 36% rate in Khan et al.'s[15] series. Anastomotic leak and the development of an enteric fistula are associated with enteroclysis and enterostomy, which should be avoided if at all possible.[16]
Twenty-nine patients (59.2%) in our series were found to have either a surgically inaccessible 'frozen' abdomen or mesenteric lymphadenopathy, whereas this occurred in less than 10% of the series reported by Akbar et al.[91 Nafeh et al.[17] did not have any patients with mesenteric lymphadenopathy, whereas Clarke et al.[61] and Baloch et al.[8] found mesenteric lymphadenopathy in 23% and 27% of their patients, respectively. Mesenteric lymphadenopathy was the most common operative finding in our series. Among our patients with 'frozen' abdomens and lymphadenopathy there were four stomas (13.5%), seven ICU admissions (24.1%) and ten deaths (34.4%). Laparotomy was associated with significant morbidity in our cohort. In addition, the mortality rate was significantly higher in our series (38.8%) than in the published literature.[7,8,14]
Factors significantly associated with death in our setting were pre-operative severity indices that attest to both acute and sustained inflammatory responses. When these are evident on presentation, it is prudent to consider further investigation prior to surgery. This may avoid a non-therapeutic laparotomy, particularly in patients presenting without signs of peritonitis. Ultrasound and CT scans and gastrointestinal contrast studies were used infrequently in our series because our patients presented as acute surgical emergencies. More liberal use of CT scanning may provide supportive evidence of abdominal TB. Peripheral rim enhancement with central necrosis is very characteristic of tuberculous lymphadenopathy.[18,19] CT can - also provide valuable information regarding the level of obstruction, localised perforation, or intra-abdominal collections that may be amenable to percutaneous drainage, and may allow re-assessment of the need for laparotomy and enable a more conservative approach to diagnosis and management, the use of laparoscopy and endoscopy to obtain tissue samples.[20]
Conclusions
Laparotomy is currently an option employed for the 'acute abdomen' in patients with suspected HIV and abdominal TB. In view of the high mortality and morbidity rates associated with laparotomy for abdominal TB, emergency surgery should be reserved for patients with convincing radiological or clinical evidence of perforation. However, in those who present with acidosis and significant anaemia or hypo-albuminaemia, and an unresolving sub-acute small bowel obstruction is the most likely diagnosis, more detailed investigations and minimally invasive sampling should be carried out if feasible. This will help in deciding whether to opt for a conservative trial of anti-TB therapy with intravenous nutritional support or proceed to a laparotomy with its attendant risks.
REFERENCES
1. Karim SSA, Churchyard GJ, Karim QA, Lawn SD. HIV infection and tuberculosis in South Africa: An urgent need to escalate the public health response. Lancet 2009;374 (9693):921-933. [http://dx.doi.org/10.1016/S0140-6736(09)60916-8] [ Links ]
2. Cohen T, Wilson D, Murray M, et al. The prevalence and drug sensitivity of tuberculosis among patients dying in hospital in KwaZulu-Natal, South Africa: A postmortem study. PLoS Med 2010;7(6):e1000296. [http://dx.doi.org/10.1371/journal.pmed.1000296] [ Links ]
3. Riquelme A, Calvo M, Salech F, et al. Value of adenosine deaminase (ADA) in ascitic fluid for the diagnosis of tuberculous peritonitis. J Clin Gastroenterol 2006;40(8):705-710. [http://dx.doi.org/10.1097/00004836-200609000-00009] [ Links ]
4. Khan R, Abid S, Jafri W, Abbas Z, Hameed K, Ahmad Z. Diagnostic dilemma of abdominal tuberculosis in non-HIV patients: An ongoing challenge for physicians. World J Gastroenterol 2006;12(39):6371-6375. [ Links ]
5. Cacala SR, Mafana E, Thomson SR, Smith A. Prevalence of HIV status and CD4 counts in a surgical cohort: Their relationship to clinical outcome. Ann R Coll Surg Engl 2006;88 (1):46-51. [http://dx.doi.org/10.1308/003588406X83050] [ Links ]
6. Clarke DL, Thomson SR, Bissety T, Madiba TE, Buccimazza I, Anderson F. A single surgical unit's experience with abdominal tuberculosis in the HIV/AIDS era. World J Surg 2007;31(5):1088-1097. [http://dx.doi.org/10.1007/s00268-007-0402-8] [ Links ]
7. Abro A, Siddiqui FG, Akhtar S, Memon AS. Spectrum of clinical presentation and surgical management of intestinal tuberculosis at tertiary care hospital. J Ayub Med Coll Abbottabad 2010;22(3):96-99. [ Links ]
8. Baloch NA, Baloch MA, Baloch FA. A study of 86 cases of abdominal tuberculosis. Journal of Surgery Pakistan (International) 2008;13(1):30-32. [ Links ]
9. Akbar M, Islam F, Haider IZ, et al. Surgical management of tuberculous small bowel obstruction. J Ayub Med Coll Abbottabad 2010;22(2):171-175. [ Links ]
10. Sinkala E, Gray S, Zulu I, et al. Clinical and ultrasonographic features of abdominal tuberculosis in HIV positive adults in Zambia. BMC Infect Dis 2009;9:44. [http://dx.doi. org/10.1186/1471-2334-9-44] [ Links ]
11. Iliyasu Z, Babashani M. Prevalence and predictors of tuberculosis coinfection among HIV-seropositive patients attending the Aminu Kano Teaching Hospital, Northern Nigeria. J Epidemiol 2009;19(2):81-87. [http://dx.doi.org/10.2188/jea.JE20080026] [ Links ]
12. Ghiya R, Naik E, Casanas B, Izurieta R, Marfatia Y. Clinico-epidemiological profile of HIV/TB coinfected patients in Vadodara, Gujarat. Indian J Sex Transm Dis 2009;30:10-15. [http://dx.doi.org/10.4103/0253-7184.55472] [ Links ]
13. Khan I, Khan F, Khan M. Surgical management of abdominal tuberculosis. Journal of Postgraduate Medical Institute 2003;17:32-41. [ Links ]
14. Arif AU, Shah LA, Sadiq M. The frequency and management of intestinal tuberculosis: A hospital based study. Journal of Postgraduate Medical Institute 2008;22(2):152-156. [ Links ]
15. Khan IA, Khattak IU, Asif S, Nasir M, Rehman Z. Abdominal tuberculosis: An experience at Ayub Teaching Hospital Abbottabad. J Ayub Med Coll Abbottabad 2008;20(4):115-118. [ Links ]
16. Abbasi A, Javaherzadeh M, Arab M, Keshoofy M, Pojhan S, Daneshvar G. Surgical treatment for complications of abdominal tuberculosis. Arch Iran Med 2004;7(1):57-60. [ Links ]
17. Nafeh MA, Madhat A, Abdul-Hameed AG, et al. Tuberculous peritonitis in Egypt: The value of laparoscopy in diagnosis. Am J Trop Med Hyg 1992;47(4):470-477. [ Links ]
18. Ko CY, Schmit PJ, Petrie B, Thompson JE. Abdominal tuberculosis: The surgical perspective. Am Surg 1996;62(10):865-868. [ Links ]
19. Pereira JM, Madureira AJ, Vieira A, Ramos I. Abdominal tuberculosis: Imaging features. Eur J Radiol 2005;55(2):173-180. [http://dx.doi.org/10.1016/j.ejrad.2005.04.015] [ Links ]
20. Akgun Y. Intestinal and peritoneal tuberculosis: Changing trends over 10 years and a review of 80 patients. Can J Surg 2005;48(2):131-136. [ Links ]
 Corresponding author:
Corresponding author:
J Islam
(islam@telkomsa.net)














