Serviços Personalizados
Artigo
Indicadores
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares em Google
Similares em Google
Compartilhar
South African Journal of Surgery
versão On-line ISSN 2078-5151
versão impressa ISSN 0038-2361
S. Afr. j. surg. vol.52 no.1 Cape Town Jan. 2014
GENERAL SURGERY
Understanding the reasons for delay to definitive surgical care of patients with acute appendicitis in rural South Africa
V Y KongI; C AldousII; D L ClarkeIII
IMB ChB; Department of Surgery, Nelson R Mandela School of Medicine, University of KwaZulu-Natal, Durban, South Africa
IIPhD; Research Facilitator, Postgraduate Committee, Nelson R Mandela School of Medicine, University of KwaZulu-Natal, Durban, South Africa
IIIFCS (SA); Department of Surgery, Nelson R Mandela School of Medicine, University of KwaZulu-Natal, Durban, South Africa
ABSTRACT
BACKGROUND: Acute appendicitis in rural South Africa is associated with significant morbidity due to prolonged delays before definitive surgical care.
OBJECTIVE: This audit aimed to quantify the delay in our healthcare system.
METHODS: From September 2010 to September 2012, all patients with confirmed acute appendicitis were interviewed and asked about the onset of symptoms and subsequent events in the disease process. Events before and after contact with the healthcare system were referred to as the pre-hospital or behavioural domain and the in-hospital or assessment domain, respectively.
RESULTS: Of the 500 patients, 350 (70.0%) experienced a delay of >48 hours from onset of symptoms to definitive surgical care. The mean time before treatment for this group was 5 days (range 3 - 7), while the mean for the group without delay was 1.6 days (range 1 - 2) (p<0.0001). Of 463 delays, 291 were in the behavioural domain and 172 in the assessment domain; 178 patients (50.9%) experienced delay in the behavioural domain only, 59 (16.9%) in the assessment domain only, and 113 (32.2%) in both domains. The mean ambulance transport time from the district hospital to the regional hospital was 4.9 hours.
CONCLUSION: There are barriers that prevent patients with acute appendicitis from accessing care. There are also prolonged delays within the system once care has been accessed. Both these sources of delay need to be addressed by quality improvement programmes.
Acute appendicitis in South Africa is associated with prolonged delays to definitive surgical care and significant morbidity due to intra-abdominal sepsis.[1-3] This is a directly causal relationship, as delayed source control has repeatedly been shown to be the variable most closely associated with poor outcomes from intra-abdominal sepsis.[4,5] Strategies and quality improvement interventions designed to reduce the morbidity associated with acute appendicitis must attempt to reduce delays to definitive care.[2] However, there is a paucity of research on the reasons for these delays. If the treatment of appendicitis is thought of as a process of care, there are a number of distinct areas or domains within the process where delay can be experienced.[6] There may be a significant delay between the onset of symptoms and the patient making contact with the healthcare system. Once the patient has made contact with the system, further delays can be experienced. These include delayed recognition of the need for surgical care and subsequent logistical delays in transferring the patient to the regional hospital. This audit quantifies the delay to definitive surgical care of acute appendicitis in our system and attempts to increase our understanding of where in the process of care the delay was experienced and the factors that contributed to delay in each area or domain. It is hoped that this information may allow for the development of targeted quality improvement programmes.
Methods
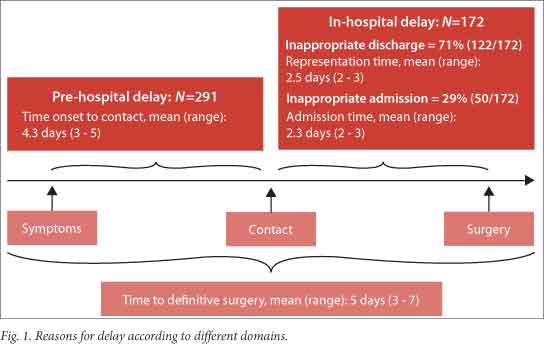
Ethics approval for the study was obtained from the Biomedical Research Ethics Committee of the University of KwaZulu-Natal, and the Umgungundlovu Health Review Board. It was conducted from September 2010 to September 2012 at Edendale Hospital in Pietermaritzburg, South Africa. Edendale Hospital receives patients from the city of Pietermaritzburg and surrounding peri-urban settlements and is the regional hospital for the four rural hospitals in Sisonke district. None of the rural hospitals performs appendectomy. All patients with acute appendicitis confirmed at operation were eligible for inclusion. Basic demographic data were collected, and each patient was interviewed by the principal author and specifically asked about the onset of symptoms and subsequent events in their disease process. All events before the patient made contact with the healthcare system were referred to as the pre-hospital or behavioural domain, while events from making contact up to recognition of the need for definitive surgical care were referred to as the in-hospital or assessment domain. We asked the patients whether they had been sent home after making initial contact with the healthcare system. All such cases were classified as inappropriate discharges. Fig. 1 schematically demonstrates the timeline of the disease process. Detailed questioning was used to classify the reasons for any delay in the assessment domain, e.g. whether patients were discharged home, or admitted to hospital for inappropriate management. A significant delay was defined as >48 h from the onset of symptoms to definitive surgery.
Statistical analysis
Pearson's x2 test was used when the sample size assumption was adhered to, Fisher's exact test was used in cases where the x2 assumption was not fulfilled, and the Mann-Whitney U test was performed to identify any significant difference between the two groups after data distributions were proven to be asymmetrical. Non-parametric (asymmetrical) data were described in terms of a median and interquartile range (IQR Q1 - Q3). Statistical significance was set at p<0.05. All statistical analysis was performed using SPSS version 19.
Results
A total of 500 patients presented to our unit with acute appendicitis during the 2 years of the study. The mean age was 22 years (standard deviation (SD) ±6.1), and 316 (63.2%) were male and 184 (36.8%) female. Of all patients, 70% (350/500) experienced a delay of >48 h from onset of symptoms to definitive surgical care.
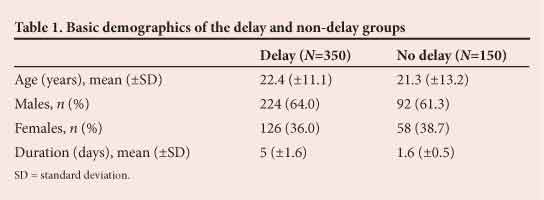
In the delay group, 64% were males (224/350) and 36% females (126/350), and the mean age was 22.4 years (range 12 - 29). The mean time from onset of symptoms to definitive surgical care for this group was 5 days (SD ±1.6), while the mean for the group without delay was 1.6 days (SD ±0.5) (p<0.0001). Table 1 summarises the demographics of these patients.
There were 463 delays in total, of which 291 were in the behavioural domain and 172 in the assessment domain; 178/350 patients (50.9%) experienced delay in the behavioural domain only, 59 (16.9%) in the assessment domain only, and 113 (32.2%) in both domains. The mean duration of illness from the onset of symptoms to first contact with the healthcare system in the behavioural domain group was 4.4 days (SD ±1.5). Tables 2 and 3 provide a summary of the above. Fig. 1 provides a narrative of the reasons for delay from onset of symptoms to definitive surgery.

Of the 172 patients with delay in the assessment domain, 71% (122/172) were inappropriately discharged from the hospital, and 29% (50/172) were admitted prior to referral for definitive surgical care. For the 122 who were inappropriately discharged, a mean of 2.5 days (SD ±1.0) elapsed between discharge and re-presentation at the hospital. For the 50 who were admitted to hospital for observation, the mean duration of stay prior to referral was 2.3 days (SD ±1.0). The mean ambulance transport time from the district hospital to the regional hospital was 4.9 h (SD ±2.1). Of the total of 500 patients, 49 (9.8%) had taken traditional medicine at some point during the course of the illness; of the 172 patients who experienced delay in the assessment domain, 20.4% (n=35) used traditional medicines, while the figure for the 328 without a delay in assessment was 4.3% (n=14) (p<0.0001).
Discussion
Acute appendicitis in South Africa is associated with significant morbidity due - to intra-abdominal sepsis.[1] Intra-abdominal sepsis is a time-dependent condition, and delayed surgical source control is directly associated with adverse outcomes.[4,7] We demonstrated a significant delay from onset of symptoms to definitive care in our cohort. The reasons for this delay are almost certainly multifactorial. We broke down the process of care of acute appendicitis into two broad domains where delay may be experienced, and showed that each domain contributes to the overall delay to definitive care. This is a significant finding, because strategies and avenues of research to address deficits differ according to the domain in which the deficits occur.
The majority of patients in our series did not make contact with the healthcare system until long after the onset of abdominal symptoms. Making contact with the healthcare system is referred to as health-seeking behaviour and is influenced by a multitude of factors, such as gender inequalities, educational levels, awareness, inadequate infrastructure, endemic poverty and cultural factors.[8-10] Factors that deter health-seeking behaviour are collectively referred to as barriers to care and have been divided into cultural (acceptability), financial (affordability) and structural (accessibility) issues.[11] Dissecting out and understanding the barriers to care requires a nuanced methodology incorporating culturally appropriate qualitative techniques. It is doubtful that our methodology would be able to do this complex problem justice. We have, however, illustrated the point that there is a long delay between the onset of symptoms and seeking medical opinion. Further public health and sociological research is required to improve understanding of the reasons for late presentation following the onset of symptoms in our environment, and the barriers to care.
A significant number of the patients in our series sought advice from traditional healers, and this was directly associated with subsequent assessment failure. Developing a programme that integrates traditional healers into the healthcare system may be a potential intervention.[12] In Pietermaritzburg we run a course with local traditional healers, attempting to educate them on the warning signs of acute appendicitis and encouraging them to refer specific groups of patients to the healthcare system earlier.
Our findings indicate that patients with acute appendicitis are at risk for delayed diagnosis after they have made contact with the healthcare system. A significant number were discharged home inappropriately, and a further sub-group were admitted for excessive periods of observation. Acute appendicitis, although - common, is a difficult clinical diagnosis, and the classic clinical features may only be present in a third of patients.[13] This is especially true among black Africans, many of whom present with nonspecific abdominal pain.[1,14] Female patients have a wider differential diagnosis, and gynaecological causes of abdominal pain and symptoms associated with pregnancy need to be excluded.[15] The situation is made still more complex by the high prevalence of infectious diseases, such as abdominal tuberculosis associated with HIV disease.[16] The relatively junior level of the staff at the rural hospitals in our drainage area exacerbates the clinical dilemma.[17] Addressing this deficit is complex and requires a multifaceted strategy that may include the use of educational initiatives, 'tick box'-type clerking sheets, and possible telemedicine support.
Conclusions
Patients with acute appendicitis experience significant delays between the onset of symptoms and definitive surgical treatment, resulting in major morbidity. The reasons for this situation are multifactorial and include barriers to healthcare, delays in assessment, and logistical problems with patient transfer. Understanding these reasons may help in developing targeted quality improvement interventions. There are delays associated with health-seeking behaviour and delays associated with failure of healthcare workers to recognise the need for surgery. Delay related to health-seeking behaviour is difficult to modify, and improvement initiatives must focus on improving access to care. Improving the diagnostic capability of healthcare workers in rural district hospitals must be addressed as a matter of urgency.
REFERENCES
1. Kong VY, Bulajic B, Allorto NL, et al. Acute appendicitis in a developing country. World J Surg 2012;36(9):2068-2073. [http://dx.doi.org/10.1007/s00268-012-1626-9] [ Links ]
2. Kong VY, Aldous C, Handley JJ, Clarke DL. The cost effectiveness of the early management of acute appendicitis underlies the importance of curative surgical services to a primary health care program. Ann R Coll Surg Engl 2013;95(4):280-284. [http://dx.doi.org/10.1308/003588413X13511609958415] [ Links ]
3. Fulton J, Lazarus C. Acute appendicitis among black South Africans. S Afr J Surg 1995;33(4):165-166. [ Links ]
4. Bickell NA, Aufses AH Jr, Rojas M, et al. How time affects the risk of rupture in appendicitis. J Am Coll Surg 2006;202(3):401-406. [http://dx.doi.org/10.1016/j.jamcollsurg.2005.11.016] [ Links ]
5. Sartelli M, Viale P, Catena F, et al. 2013 WSES guidelines for management of intra-abdominal infections. World J Emerg Surg 2013;8(1):3. [http://dx.doi.org/10.1186/1749-7922-8-3] [ Links ]
6. Jablonski KA, Guagliardo MF. Pediatric appendicitis rupture rate: A national indicator of disparities in healthcare access. Popul Health Metr 2005;3(1):4. [ Links ]
7. Papaziogas B, Tsiaousis P, Koutelidakis I, et al. Effect of time on risk of perforation in acute appendicitis. Acta Chir Belg 2009;109(1):75-80. [ Links ]
8. Ahmed SM, Adams AM, Chowdhury M, et al. Gender, socioeconomic development and health-seeking behaviour in Bangladesh. Soc Sci Med 2000;51(3):361-371. [http://dx.doi.org/10.1016/S0277-9536(99)00461-X] [ Links ]
9. Akande TM, Owoyemi JO. Healthcare-seeking behaviour in Anyigba, North-Central, Nigeria. Research Journal of Medical Sciences 2009;3(2):47-51. [ Links ]
10. Titchener JL, Zwerling I, Gottschalk L, et al. Problem of delay in seeking surgical care. JAMA 1956;160(14):1187-1193. [ Links ]
11. Grimes CE, Law RS, Borgstein ES, et al. Systematic review of met and unmet need of surgical disease in rural sub-Saharan Africa. World J Surg 2012;36(1):8-23. [http://dx.doi.org/10.1007/s00268-011-1330-1] [ Links ]
12. Nxumalo N, Alaba O, Harris B, et al. Utilization of traditional healers in South Africa and costs to patients: Findings from a national household survey. J Public Health Policy 2011;32(Suppl 1):S124-S136. [http://dx.doi.org/10.1057/jphp.2011.26] [ Links ]
13. Paulson EK, Kalady MF, Pappas TN. Clinical practice. Suspected appendicitis. N Engl J Med 2003;348(3):236-242. [http://dx.doi.org/10.1056/NEJMcp013351] [ Links ]
14. Chamisa I. A clinicopathological review of 324 appendices removed for acute appendicitis in Durban, South Africa: A retrospective analysis. Ann R Coll Surg Engl 2009;91(8):688-692. [http://dx.doi.org/10.1308/003588409X12486167521677] [ Links ]
15. Dunn EL, Moore EE, Elerding SC, et al. The unnecessary laparotomy for appendicitis - can it be decreased? Am Surg 1982;48(7):320-323. [ Links ]
16. Clarke DL, Thomson SR, Bissetty T, et al. A single surgical unit's experience with abdominal tuberculosis in the HIV/AIDS era. World J Surg 2007;31(5):1087-1096; discussion 1097-1098. [ Links ]
17. De Villiers MR. The knowledge and skills gap of medical practitioners delivering district hospital services in the Western Cape, South Africa. S Afr Fam Pract 2006;48(2):16a-c. [ Links ]
 Corresponding author:
Corresponding author:
D L Clarke
(damianclar@gmail.com)














