Serviços Personalizados
Artigo
Indicadores
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares em Google
Similares em Google
Compartilhar
South African Journal of Surgery
versão On-line ISSN 2078-5151
versão impressa ISSN 0038-2361
S. Afr. j. surg. vol.51 no.4 Cape Town Jan. 2013
CASE REPORT
Use of a circular stapler for Billroth I anastomosis after distal gastrectomy
S Hasukic; O Muratovic; I Hasukic
Department of Surgery, University Clinical Center Tuzla, Faculty of Medicine, University of Tuzla, Tuzla, Bosnia and Herzegovina
ABSTRACT
Staplers are widely used in gastrointestinal surgery. We used a circular stapler to establish gastroduodenal anastomosis after distal gastrectomy in a recent case. After separating the stomach from the duodenum, we anastomosed the posterior wall of the stomach to the duodenum by introducing the circular stapler through the part of the stomach that was to be resected. Then we separated the distal part of the stomach with a linear stapler, and so completed the distal gastric resection. The advantages of this technique are that it is simple and safe.
A gastroduodenostomy creates a new connection between the stomach and the duodenum. It is the preferred type of reconstruction after surgery for benign diseases because it restores normal gastrointestinal physiology. Although mechanical stapling is now an established alternative to conventional hand suturing for construction of a gastrointestinal anastomosis, its role in gastroduodenostomy remains to be defined.[1] Several techniques have been described for performing Billroth I anastomosis after distal gastrectomy using a circular stapler.[1-3] Some surgeons make an incision on the anterior wall of the residual stomach, insert the circular stapler, and perform side-to-end gastroduodenostomy. The place where the stapler has been introduced is closed manually.[1] Others create the anastomosis before distal gastrectomy, introducing the circular stapler through the part of the stomach to be resected.[2] A modification of this technique has been described by Takeuchi et al.,[3] but is not often used.
We describe a Billroth I gastrectomy and Billroth I anastomosis in which we introduced a CDH stapler (Ethicon Endo-Surgery, Cincinnati, Ohio, USA) through the part of the stomach to be resected.
Case report
A 55-year-old woman with benign pyloric stenosis was scheduled for Billroth I gastrectomy. Pre-operative preparation and anaesthesia were similar to those used for the traditional open operation.
Surgical technique
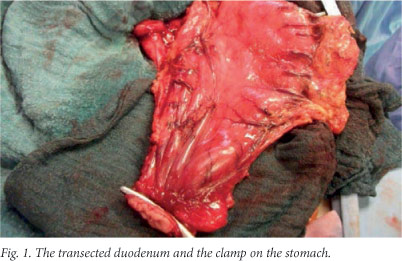
After making an upper midline incision and ligating and dividing the stomach vessels, the greater and lesser curvatures of the stomach are freed. The first portion of the duodenum is freed to enable a purse-string instrument to be placed distal to the resection line. The purse-string suture is introduced, an intestinal clamp is applied proximal to the purse string, and the duodenum is transected between the purse-string instrument and the clamp (Fig. 1).
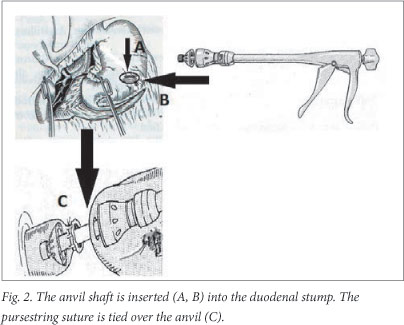
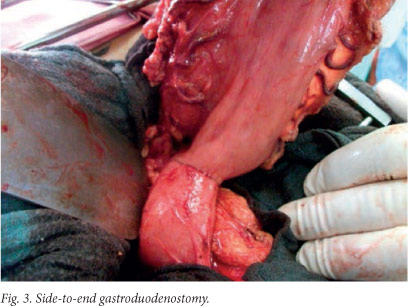
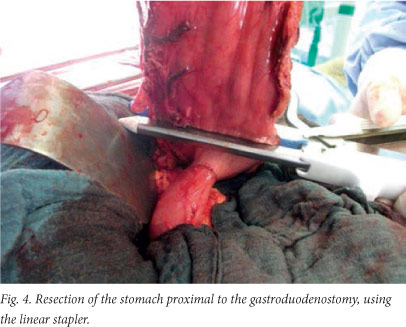
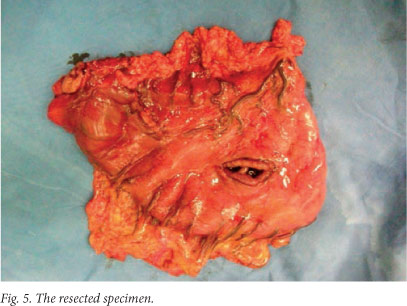
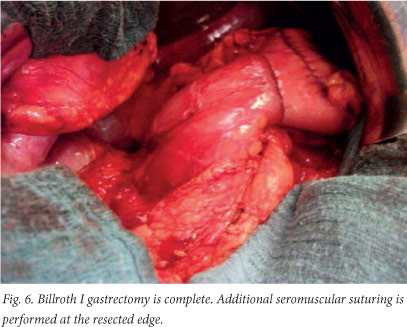
An anvil (CDH 29) is now inserted into the duodenal stump (Fig. 2), and the purse-string suture is tied over the anvil. The circular stapler is introduced into the body of the stomach through a 3 cm vertical incision in its anterior wall. A side-to-end gastroduodenostomy (Fig. 3) is performed on the rear wall of the stomach along its greater curvature, 2 cm above the gastric resection line. The cartridge and anvil are brought together and fired. The instrument is then removed through the open edge of the stomach. After visual examination of the anastomosis following resection of the stomach proximal to the side-to-end gastroduodenostomy, gastric resection is done using the linear stapler ILA 100 (Figs 4 - 6). The specimen is removed together with the stapler. Additional seromuscular suturing at the resected edge is usually performed.
Discussion
Use of staplers in gastrointestinal surgery has many advantages compared with hand suturing - for example, clinical studies have shown that it decreases operation time. However, use of a circular stapler for gastroduodenal anastomosis after resection of the distal stomach has rarely been reported. Nakane et al.[2] were the first to report a technique similar to that described above but using two linear staplers. Takeuchi et al.[3] then reported the first gastroduodenal anastomosis using one circular and one linear stapler. This technique has also been effectively used for Billroth II anastomosis.[4] We established gastroduodenal anastomosis using the circular stapler before resection of the stomach with the linear stapler, which also meant that we needed to use only one linear stapler. This technique reduces the time needed to create the Billroth I anastomosis, is reliable and safe, and should be used more often in everyday work.
Conclusion
Application of the circular stapler in creating a Billroth I anastomosis after distal resection of the stomach has been described, but it is not widely used. We report successful use of the circular stapler technique in establishing gastroduodenal anastomosis after distal gastrectomy. The advantages of this technique are that it is simple and safe.
REFERENCES
1. Hori S, Ochiai T, Gunji Y, Hayashi H, Suzuki T. A prospective randomized trial of hand-sutured versus mechanically stapled anastomoses for gastroduodenostomy after distal gastrectomy. Gastric Cancer 2004;7(1):24-30. [http://dx.doi.org/10.1007/s10120-003-0263-2] [ Links ]
2. Nakane Y, Kanbara T, Michiura T, et al. Billroth I gastrectomy using a circular stapler to treat gastric cancer. Surg Today 2001;31(1):90-92. [http://dx.doi.org/10.1007/s005950170 229] [ Links ]
3. Takeuchi K, Tsuzuki Y, Ando T, et al. A modified stapling technique for performing Billroth I anastomosis after distal gastrectomy. World J Surg 2005;29(1):113-115. [http://dx.doi.org/10.1007/s00268-004-7356-x] [ Links ]
4. Oh SJ, Hong JJ, Oh CA, et al. Stapling technique for performing Billroth II anastomosis after distal gastrectomy. J Gastrointest Surg 2011;15(7):1244-1246. [http://dx.doi.org/10.1007/s11605-010-1403-8. [ Links ]]
 Correspondence:
Correspondence:
Š Hasukić
(shasukic@bih.net.ba)














