Services on Demand
Article
Indicators
Related links
-
 Cited by Google
Cited by Google -
 Similars in Google
Similars in Google
Share
South African Journal of Surgery
On-line version ISSN 2078-5151
Print version ISSN 0038-2361
S. Afr. j. surg. vol.51 n.4 Cape Town Jan. 2013
CASE REPORT
Tubercular biliary stricture - a malignant masquerade
K Vijay; S Naidu; R Godara; V Vijayvergia
Department of Gastrointestinal Surgery and Liver Transplantation, Army Hospital R&R, New Delhi, India
ABSTRACT
Hilar cholangiocarcinoma is the most common cause of a stricture in the hilar region, and hilar stricture in the absence of any previous surgical intervention should be considered to indicate malignant disease until proven otherwise. We present a rare case of isolated hilar tubercular stricture, all the features of which were suggestive of malignancy.
Abdominal tuberculosis is the most common form of extrapulmonary tuberculosis, but very rarely involves the biliary tree.[1] Either the primary biliary tuberculosis or external compression by adjacent organs can lead to formation of strictures that may be single or multiple[2,3] and are difficult to diagnose accurately pre-operatively. We present a rare case of hilar tubercular stricture that mimicked hilar cholangiocarcinoma.
Case report
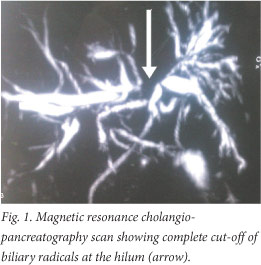
A 40-year-old man presented with complaints of painless progressive jaundice, pruritus, clay-coloured stools and weight loss of 3 months' duration. Clinical examination revealed icterus, scratch marks all over the body and hepatomegaly. A chest radiograph and the results of blood tests were essentially normal except for an erythrocyte sedimentation rate of 40 mm/1sth. The results of liver function tests were as follows: total bilirubin level 268 |imol/l (direct 166 µmol/l), serum glutamic oxaloacetic transaminase 32 IU/l, serum glutamic pyruvate transaminase 40 IU/l, serum alkaline phosphatase 1 270 IU/l and gamma-glutamyl transpeptidase 760 IU/l. Ultrasonography revealed an indistinct mass in the area of the hilum with backpressure biliary changes that suggested a neoplastic cause. Magnetic resonance cholangiopancreatography showed a lesion measuring 2x2 cm at the hilum with complete separation of the biliary radicals at the confluence with periportal lymphadenopathy (Fig. 1). Levels of the serum tumour markers carbohydrate antigen 19-9, carcino-embryonic antigen and alpha-fetoprotein were within normal limits. Resective surgery was planned on the basis of the imaging findings. Diagnostic laparoscopy showed greyish-white nodular deposits on the inferior surface of segment V Frozen-section biopsy confirmed a diagnosis of tuberculosis. Biliary decompression was achieved postoperatively with endoscopic retrograde cholangiopancreaticography and stenting followed by standard antituberculosis therapy. The patient made an uneventful recovery and was doing well when seen 5 months after treatment.
Discussion
Involvement of small to large ducts in primary biliary tuberculosis can result in stricture formation.[4] In this situation, comprehensive investigations usually fail to provide an accurate pre-operative diagnosis. If the lesion appears to be resectable on imaging, surgery should be considered rather than relying on minimally invasive investigations such as brush cytology, percutaneous fine-needle aspiration biospy (FNA) or endoscopic ultrasound-guided FNA, as these investigations are helpful only if positive for adenocarcinoma and have a very low negative predictive value. Management includes endoscopic, percutaneous or surgical biliary drainage and standard antituberculosis therapy.[2] Sequential placement of multiple plastic stents has been shown to be effective, as the stents both enable biliary drainage and act as dilators. The management of multiple or complex strictures is more challenging and requires a combination of endoscopic, percutaneous and surgical therapies.
The authors are of the opinion that in a country such as India, where tuberculosis is relatively common, tubercular biliary stricture should be kept in mind in the differential diagnosis of hilar stricture when a patient presents with a short history and in relatively good health. These lesions should not be allowed to masquerade in the guise of a malignant tumour, but it is equally important that bile duct malignancies are not mistaken for benign lesions.
REFERENCES
1. Acharya SK, Tandon BN. Abdominal tuberculosis. In: Watters D, Kiire C, eds. Gastroenterology in the Tropics and Subtropics: A Practical Approach. 10th ed. London and Basingstoke: Macmillan Education, 2005:85-102. [ Links ]
2. Chong VH, Lim KS. Hepatobiliary tuberculosis. Singapore Med J 2010;51(9):744-751. [ Links ]
3. Alvarez SZ. Hepatobiliary tuberculosis. J Gastroenterol Hepatol 1998;13(8):833-839. [http://dx.doi.org/10.1111/j.1440-1746.1998.tb00743.x] [ Links ]
4. Inal M, Aksungur E, Akgul E, et al. Biliary tuberculosis mimicking cholangiocarcinoma: Treatment with metallic biliary endoprothesis. Am J Gastroenterol 2000;95(4):1069-1071. [http://dx.doi.org/10.1016/S0002-9270(00)00736-X] [ Links ]
 Correspondence:
Correspondence:
K Vijay
(drkapileshwer@gmail.com)














