Services on Demand
Article
Indicators
Related links
-
 Cited by Google
Cited by Google -
 Similars in Google
Similars in Google
Share
South African Journal of Surgery
On-line version ISSN 2078-5151
Print version ISSN 0038-2361
S. Afr. j. surg. vol.51 n.4 Cape Town Jan. 2013
TRAUMA
Patterns of injury seen in road crash victims in a South African trauma centre
F ParkinsonI, III; S KentII; C AldousIII; G OosthuizenIV; D L ClarkeIV
IDepartment of Surgery, Edendale Hospital, Pietermaritzburg, KwaZulu-Natal, South Africa
IINgwelezane Hospital, Ngwelezane, KwaZulu-Natal, South Africa
IIIPostgraduate Committee, Nelson R Mandela School of Medicine, University of KwaZulu-Natal, Durban, South Africa
IVDepartment of Surgery, Edendale Hospital, Pietermaritzburg, and Nelson R Mandela School of Medicine, University of KwaZulu-Natal, Durban, South Africa
ABSTRACT
BACKGROUND: Road traffic crashes (RTCs) account for a significant burden of disease in South Africa. This prospective study reviews basic demographic and outcome data of patients who sustained an RTC-related injury and analyses the common patterns of injury associated with specific mechanisms of injury.
METHOD: We reviewed all patients seen at a single regional hospital (Edendale Hospital, Pietermaritzburg) with injuries sustained in RTCs over a 10-week period. State mortuary data were gathered on all RTC-related fatalities over the same period.
RESULTS: Three hundred and five RTC patients were seen at the hospital over the 10-week period. The average transfer time to hospital was 9.2 hours (range 1 - 17 hours). One hundred patients were admitted and the rest were discharged home from the emergency department. Of the admitted cohort, 59 were motor vehicle occupants (MVC group) and 41 were pedestrians (PVC group). PVC patients commonly had lower limb, head, radio-ulnar and clavicular injuries, while MVC patients commonly had neck and intraabdominal injuries. Thirty-seven patients had multiple injuries. The in-hospital mortality rate was 5.6%, but the overall mortality rate was 10.0%, as 15 patients died at the scene.
CONCLUSIONS: Patterns of injury differ according to the mechanism of injury. Pedestrians impact against various parts of the vehicle and the ground and so sustain injuries to their arms and legs. Occupants of vehicles impact against the dashboard and steering wheel and are more likely to sustain torso injuries. The low number of severe injuries and multiple injuries and the relatively low inpatient mortality rate are a consequence of the triage effect of long delays in transfer. More severely injured patients are more likely to die at the scene.
South Africa has a major burden of injury related to road traffic crashes (RTCs). The widespread use of flat-bed trucks and overcrowded minibuses to transport passengers and a pervasive culture of disregard for the rules of the road result in a very high rate of RTCs. This situation is not confined to South Africa but appears to be widespread throughout the developing world, and RTCs are a significant cause of morbidity and mortality globally. It is estimated that over 1.2 million people die and up to 50 million are injured each year worldwide as a result of RTCs. However, the burden of these injuries is disproportionally distributed, with 90% of these deaths and morbidities occurring in middle- and low-income countries, where less than half of the world's motor vehicles are owned.[1] As a result of urbanisation and increased vehicle ownership in developing countries, the magnitude of the problem is likely to rise. The World Health Organization estimates that by the end of the current decade RTCs will have risen from the 9th to the 5th leading cause of death worldwide.[1] The situation in South Africa supports this prediction, as South African traffic statistics have demonstrated a steadily increasing number of registered vehicles and drivers and there were 13 802 deaths from RTCs in South Africa during 2011.[2]
This prospective study reviewed all trauma admissions subsequent to an RTC at a single busy regional hospital and attempted to determine the common mechanisms of injury and associated patterns of injury.
Methods
The Metropolitan Trauma Service in Pietermaritzburg, KwaZulu-Natal, has class approval from the relevant ethics review boards to maintain a prospective database on all trauma patients under its care. This study was undertaken at Edendale Hospital, a busy regional hospital in Pietermaritzburg. It is the regional referral hospital for approximately 3 million people in Pietermaritzburg, as well as the deep rural areas of Sinsonke Health District. The load of referrals is shared with the tertiary hospital based in the same city. Data were taken from a 10-week period from late 2011 to early 2012. Details for those discharged from the emergency department (ED) were taken from the outpatient records. The clinical notes for all admitted patients were reviewed, and structured interviews were carried out with all patients who had a Glasgow Coma Score (GCS) of 15/15 during admission. All patients who were interviewed gave informed consent to be interviewed. Patients whose GCS did not reach 15 during admission were not interviewed. Information sought included the estimated speed at which the vehicle was travelling, use of seatbelts, abuse of substances and general information about the nature of the crash. Each of the admitted patients was reviewed clinically by the primary author (FP) and followed up every 48 hours until discharge. An Injury Severity Score (ISS) was calculated for all the admitted patients. The time between the crash and arrival at the hospital was taken from ambulance sheets where possible, and data from the patient and ED records elsewhere. State mortuary data were gathered on the number of corpses taken to the police mortuary following an RTC over the same period.
Results
A total of 305 patients were seen at our hospital following an RTC over the 10-week study period. One hundred of these patients were admitted. A total of 45 deaths from RTCs were recorded at the police mortuary over the same time period. These included 15 from the scene of the crash, 17 from Edendale Hospital (of which 13 occurred during initial resuscitation and 4 after admission), and 13 from the other hospitals in the metropolitan complex. These 13 fatalities were excluded from the study. This makes a total of 320 RTC victims over a 10-week period, with an on-scene mortality rate of 4.7% (15/320) and an overall mortality rate of 10.0% (32/320), translating into 5 RTC victims every day and a fatality every second day.
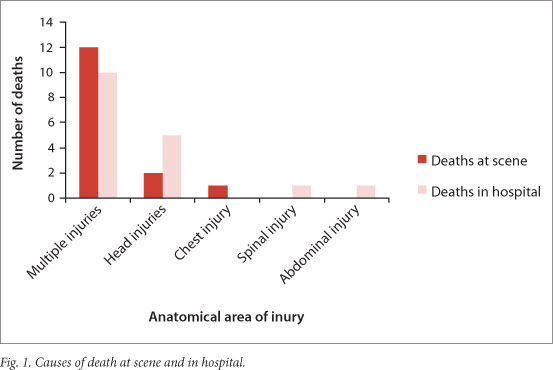
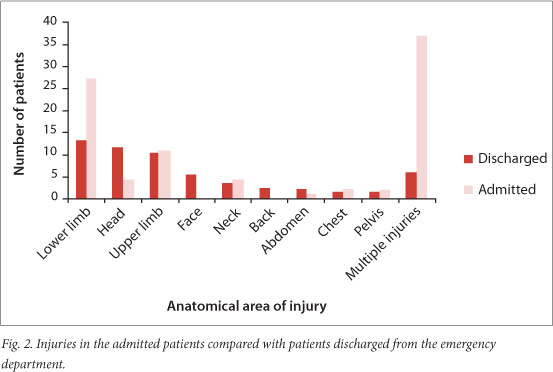
The causes of death at the scene and in hospital are compared in Fig. 1. The most common cause of death in both environments was multiple injuries, followed by head injury. The time delay between the crash and arrival at hospital was recorded in one-third of the patients and was 9.2 hours on average (range 1 - 17 hours). The majority of these patients were brought to hospital by ambulance. Of the 100 patients who were admitted, 13 were aged less than 15 years and 68 between 15 and 44 years. Table 1 summarises the demographics of the admitted group. Fifty-nine patients were involved in crashes as motor vehicle occupants (MVCs) and 41 as pedestrians (PVCs). The PVC patients were on average younger than the MVC patients (p=0.02). In the group of patients not admitted to hospital, 39 had been involved in PVCs and 166 in MVCs. Multiple injuries, defined as any injury to more than one anatomical area noted during the primary survey, were more common in the admitted patients than the discharged patients (Fig. 2): 34% of those admitted after MVCs and 44% of those admitted after PVCs (p=0.32). While a greater proportion of the PVC group was admitted (41/80 of PVCs v. 59/225 of MVCs (pp=0.45)).
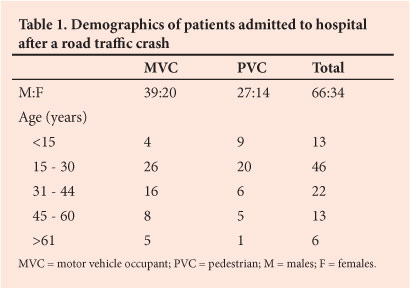
However, the pattern of injury differed markedly between the two groups (Figs 3 -5). More PVC patients than MVC patients had lower limb (tibia-fibula), clavicle and radio-ulnar fractures, head, facial and thoracic injuries. More MVC patients had humeral, neck and intra-abdominal injuries.
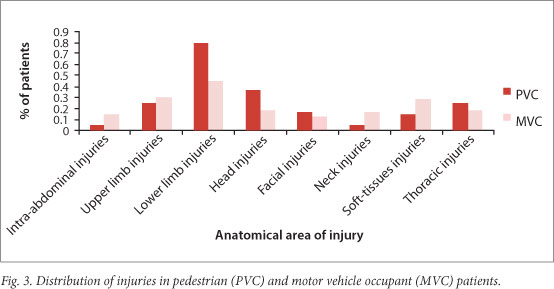
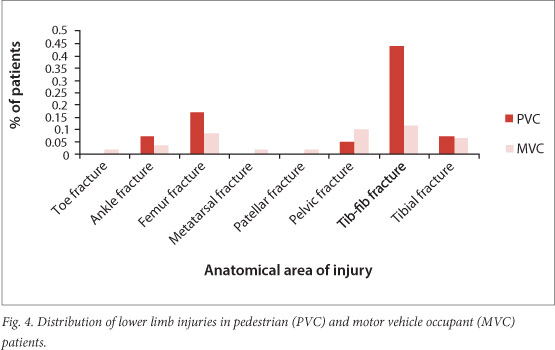
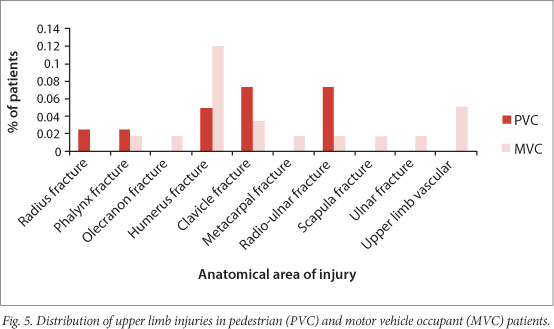
The incidence of head injuries decreased with age in both MVC and PVC patients.
Discussion
RTCs cause significant morbidity and mortality in the developing world. Ninety per cent of the 1.2 million deaths a year from RTCs occur in low- and middle-income countries,[1] where 81% of the world's population live and own about 20% of the world's vehicles.[3] Rapid urbanisation with inadequate city planning results in large numbers of vulnerable road users such as cyclists and pedestrians sharing the same space as vehicles. There are a number of differences between trauma in a developing country such as South Africa and the developed world. The significant delay between the time of the crash and arrival at hospital (average of 9.2 hours, range 1 - 17 hours) reflects an immature trauma system, translating into much poorer outcomes for major trauma than in developed countries. The patients in this cohort had a much lower rate of multiple injuries compared with patients in international series (37% v. 80 -82%).[4,5] The overall mortality rate was 10%; however, the mortality rate for patients who reached hospital was lower than that reported in series from developed countries,[4,6] and the majority (76%) of the deaths in hospital occurred during initial resuscitation. The most plausible explanation for this is that more severely injured patients do not survive the prolonged transfer times documented in this study. In effect, the long transfer times act as a ruthless triage mechanism, which eliminates a certain spectrum of patients.
Causes of death differ according to geographical location. The major causes of death at the scene are multiple injuries and head injuries. This is in keeping with the well-described triphasic pattern of death seen in trauma. Deaths from abdominal injuries, spinal injuries and chest injuries tend to occur at a later phase in hospital. Head injuries in themselves are a significant cause of mortality. ISS scores did not differ significantly between MVCs and PVCs, but there was a trend for the PVC group to sustain more multiple injuries and to have a higher rate of admission.
Different patterns of injury were associated with different mechanisms of injury in our cohort. PVC patients were admitted more often than the MVC group, reflecting the seriousness of their injuries, although ISS scores for the two admitted groups were not significantly different. The admitted group were more likely to have multiple injuries and lower limb injuries than the patients who were primarily discharged from the ED. Of the admitted group, pedestrians predominantly sustained lower extremity injuries, upper limb fractures and head and torso injuries. These victims sustain three impacts: (i) the impact of the vehicle bumper; (ii) impact with the bonnet and windscreen; and (iii) impact with the ground. This translates into: (i) lower limb injuries; (ii) head and torso injuries; and (iii) head and 'outstretched' upper limb injuries. Motor vehicle occupants more commonly sustained neck, abdominal and upper arm injuries. The mechanism of rapid deceleration results in neck injuries, and impact against the steering wheel or dashboard or caving in of the side of the car results in intraabdominal and upper arm injuries.
The study was conducted over December and January, months that have been shown to have the highest and lowest number of fatal crashes, respectively,[2] so the data should reflect the general incidence of crashes throughout the year.
Conclusion
This study demonstrates problems with access to healthcare and logistics in KwaZulu-Natal, and the significant effect this has on mortality from RTCs. It also shows common patterns of injury depending on patient age and mechanism of injury. Pedestrians are more likely to sustain upper and lower limb fractures, paediatric pedestrians are more likely to sustain head injuries, and motor vehicle occupants tend to sustain blunt torso trauma.
REFERENCES
1. World Health Organization. Violence and Injury Prevention. 2009. www.who.int/violence_injury_prevention/road_safety_status/2009 (accessed 3 August 2012). [ Links ]
2. Road Traffic Management Corporation. Arrive Alive - Road Traffic Report 2011. 31 March 2011. http://www.arrivealive.co.za/pages.aspx?i=2826 (accessed 3 August 2012). [ Links ]
3. Lehohla P. Road Traffic Accident Deaths in South Africa, 2001-2006. Evidence from death notifications. Statistician-General, Statistics South Africa. Report No 03-0907 (2001-2006), 2009. http://www.statssa.gov.za/publications/Report-03-09-07/Report-03-09-07.pdf (accessed 11 September 2013). [ Links ]
4. Peng RY, Bongard FS. Pedestrian versus motor vehicle accidents: An analysis of5000 patients. J Am Coll Surg 1999;189(4):343-348. [http://dx.doi.org/10.1016/S1072-7515(99)00166-0] [ Links ]
5. Brainard BJ, Slauterbeck J, Benhamin JB, Hagaman RM, Higie S. Injury profiles in pedestrian motor vehicle trauma. Ann Emerg Med 1989;18(8):881-883. [http://dx.doi.org/10.1016/S0196-0644(89)80218-5] [ Links ]
6. Small TJ, Sheedy JM, Grabs AJ. Cost, demographics and injury profile of adult pedestrian trauma in inner Sydney. ANZ J Surg 2006;76(1-2):43-47. [http://dx.doi.org/10.1111/j.1445-2197.2006.03646.x] [ Links ]
 Correspondence:
Correspondence:
D L Clarke
(damianclar@gmail.com)














