Services on Demand
Article
Indicators
Related links
-
 Cited by Google
Cited by Google -
 Similars in Google
Similars in Google
Share
South African Journal of Science
On-line version ISSN 1996-7489
Print version ISSN 0038-2353
S. Afr. j. sci. vol.111 n.11-12 Pretoria Nov./Dec. 2015
http://dx.doi.org/10.17159/sajs.2015/20140427
REVIEW ARTICLE
A review of the control of schistosomiasis in South Africa
Kundai MagaisaI; Myra TaylorII; Eyrun F. KjetlandII, III; Panjasaram J. NaidooI
IPharmaceutical Sciences, University of KwaZulu-Natal, Durban, South Africa
IIPublic Health Medicine, Howard College Campus, University of KwaZulu-Natal, Durban, South Africa
IIINorwegian Centre for Imported and Tropical Diseases, Department of Infectious Diseases, Oslo University Hospital, Oslo, Norway
ABSTRACT
Schistosomiasis is the second most important tropical disease in the world in terms of public health impact. In South Africa, more than 4 million people are estimated to be infected with schistosomiasis. School-age children usually have the highest prevalence and intensity of infection. Schistosoma haematobium may result in female genital schistosomiasis which presents as inflammation and ulceration of the genital mucosa and pathological blood vessels. These effects may increase the susceptibility of women with female genital schistosomiasis to HIV. Praziquantel is the drug used to treat schistosomiasis and it is best to treat people during the early stages of infection, before female genital schistosomiasis presents as lesions and sandy patches, as there currently is no treatment for these symptoms. Schistosomiasis is not regarded as a serious public health issue in South Africa despite evidence revealing the seriousness of the disease. In areas endemic for schistosomiasis, the World Health Organization recommends regular mass treatment of all school-age children. In 2001, South Africa became a signatory to the World Health Assembly resolution 54.19 which urged all member states to achieve the minimum goal of 75% treatment coverage in school-age children at risk by 2010. This goal was not achieved in South Africa, despite efforts made by the Department of Health, such as the first statutory school-based geohelminth control programme in the province of KwaZulu-Natal. However, this programme has not been continued. Therefore, there is still much work to be done in order to control and decrease the prevalence of schistosomiasis in endemic areas.
Keywords: neglected tropical disease; praziquantel; Schistosoma haematobium; female genital schistosomiasis; schoolchildren
Introduction
Epidemiology
Schistosomiasis (also known as bilharzia) is the second most important tropical disease after malaria, in terms of public health impact.1 Over 800 million people are at the risk of acquiring schistosomiasis in 76 endemic countries, with 46 of these countries in Africa.2,3 Approximately 207 million people worldwide are infected with schistosomiasis4 and 85% of the estimated number of infections are in the less developed areas of sub-Saharan Africa. Worldwide, Schistosoma haematobium causes more than half of the schistosomiasis infections, that is, approximately 112 million infections.4 S. haematobium and S. mansoni are responsible for about 280 000 deaths annually.4 In South Africa, more than 4 million people are estimated to be infected with schistosomiasis.4 The endemic areas in South Africa are in the north and the east, covering about a quarter of the country.5 The most common species in South Africa is S. haematobium . School-aged children usually present the highest prevalence and intensity of infection.5
Morbidity caused by schistosomiasis
Schistosomiasis is a systemic helminth infection caused by the Schistosoma blood fluke and is a disease of major public health concern.1,6 Morbidity is determined by the type of schistosome species involved; for example, S. haematobium infection may cause haematuria, dysuria, nutritional deficiencies, lesions in the bladder, kidney failure, an elevated risk of bladder cancer, reproductive tract morbidity, and growth retardation in children.7 Schistosomiasis is found in areas with poor sanitation where humans are in contact with water contaminated by human waste (urine, genital tract excretions and faeces) either as part of their daily lives or during recreational or professional activities.4,8 Schistosomiasis is transmitted to humans via cercariae released from the Bulinus snail.8 Upon contact with contaminated water, the parasite enters the human body by penetrating the skin. The parasite is then transported via the lymphatic system and the lungs to the liver. Final maturation into dimorphic worms takes place in the liver, with male and female adult worms growing to about 12-20 mm in size.8 The adult worm pair migrates to the different organs in the body. S. haematobium affects the pelvic organs, whereas S. mansoni affects the intestines.8
Female genital schistosomiasis
According to community based studies in S. haematobium endemic areas, 33-75% of female individuals have genital schistosomiasis.8 Female genital schistosomiasis is the presence of schistosome eggs and/or worms in the female genital organs, in the epithelium of the urinary bladder or genital mucosa where erosions, so-called sandy patches, contact bleeding and oedema may be found.9-11
Adult S. haematobium worms can be found in the venules surrounding any organ of the upper and lower genital tract.9 These adult S. haematobium worms lay between 20 and 200 eggs per day.4 A large number of the eggs penetrate the vessel wall of the urogenital tract and become sequestered in the tissues of the urinary bladder, cervix, vagina and fallopian tubes.4,8 The S. haematobium eggs may induce blood vessel proliferation in the tissues surrounding the eggs.8 The eggs, whether viable or calcified, may also induce an influx of immune cells, such as lymphocytes, macrophages, eosinophils, neutrophils, foreign body giant cells, Langerhans cells and fibroblasts.11,12 This influx may result in chronic inflammation in the affected organs.10,11
The symptoms of female genital schistosomiasis include pelvic pain, postcoital bleeding, inter-menstrual bleeding, genital itch and abnormal vaginal discharge.4,10 Female genital schistosomiasis may therefore easily be mistaken for a sexually transmitted infection like chlamydia and women may be reluctant to seek medical attention. Case reports and community based studies have further indicated decreased fertility and abortions in some women.8 Female genital schistosomiasis is also associated with increased frequency of urination and stress incontinence.8
Female genital schistosomiasis and HIV infection
It has been hypothesised that other sexually transmitted infections increase the susceptibility of women to HIV infection.8,13 Increased susceptibility may be because of an influx of immune cells but could also be because of breaches in the integrity of the mucosal barrier of the vagina and the cervix. Similarly, female genital schistosomiasis has been hypothesised to increase HIV susceptibility of women. HIV in semen may have easier access to the systemic circulation of women because of these entry points on the disrupted genital tract epithelium. Contact bleeding during sexual intercourse and other genital mucosal bleeding tendencies associated with female genital schistosomiasis might increase HIV susceptibility in infected women.14
Cross-sectional studies conducted in Zimbabwe and Tanzania indicated that women with female genital schistosomiasis had a higher HIV prevalence than women without female genital schistosomiasis.4 Female genital schistosomiasis was associated with a 2.9-4-fold higher risk of HIV seropositivity. S. haematobium infection typically occurs during childhood, preceding HIV exposure, and may pose a risk for HIV in young girls when they become sexually active4 because the vaginal epithelium would be disrupted before first sexual intercourse in S. haematobium infected girls. HIV prevalence seems to peak at a younger age in women in rural areas compared to women in urban areas. It is well known that there is often poor sanitation and a lack of piped water in rural areas and these conditions may increase a woman's risk of contracting schistosomiasis.
Immune cells in the genital lesions caused by S. haematobium infection may provide easy points of entry for HIV to attach to susceptible cells.12 The eggs trapped in the genital mucosa, whether viable or calcified, may both induce an influx of immune cells. CD4 cells are the receptors used by HIV to enter the host cells and a high concentration of CD4 cells is contained in the egg granulomas and the adjacent areas.13
It has further been hypothesised that women co-infected with HIV and S. haematobium infection may transmit HIV to their partners more easily than HIV-infected women without S. haematobium infection.4 Leukocytes may harbour HIV and conditions that result in recruitment of leukocytes to the genital tract, for example genital ulcer disease or S. haematobium infection, may result in an increase in viral shedding of HIV into the female genital tract.13
Young people and HIV in South Africa
According to the Joint United Nations Programme on HIV/AIDS (UNAIDS) 2012 fact sheet on adolescents, young people and HIV, there are about 1.6 billion people between the ages of 12 and 24 in the world today.15 In 2010, 42% of new HIV infections were among youths between the ages of 15 and 24.15 Among young people living with HIV, approximately 4 of the 5 million live in sub-Saharan Africa.15 Statistics also show that, globally, women aged 15-24 have HIV infection rates twice as high as young men in the same age group. In South Africa, the National Antenatal Sentinel HIV and Syphilis Prevalence Survey, conducted in 2011 among pregnant women attending public sector clinics and hospitals, reported KwaZulu-Natal as the province with the highest HIV prevalence in the world.16 KwaZulu-Natal had an HIV prevalence of 37.4% in 2011. Of the women aged between 15 and 24 years tested at antenatal care facilities, 25.5% were HIV positive.16 The Ugu district in KwaZulu-Natal had the highest HIV prevalence - 41.7%.
Method
Information in this article was obtained from peer-reviewed articles, published World Health Organization (WHO) reports and WHO statements, exclusively.17,18 All articles were accessed online on PubMed. Of 106 studies reviewed, similar information was reported in several sources and hence only the references which were significantly relevant to this paper were selected and are quoted.
A brief history of schistosomiasis in South Africa
The first record of urogenital schistosomiasis in South Africa was in 1863. Dr J Harley, a general practitioner in Port Elizabeth, diagnosed boys from Uitenhage in the Eastern Cape with schistosomiasis.19 This diagnosis was only 12 years after Schistosoma haematobium had been discovered by the German physician Bilharz in Egypt in 1 851.20 Case reports between 1864 and 1899 revealed how children, mostly boys between the ages of 3 and 16, were infected with schistosomiasis in the Eastern Cape.19 Transmission among the boys was as a result of recreational swimming, contact with infested water in open pools, farm dams and furrows. The most common symptom was haematuria. In the 1920s and 1930s, Leipoldt and colleagues reported the wide spread of schistosomiasis in South Africa and negative consequences of the disease, particularly in children.19
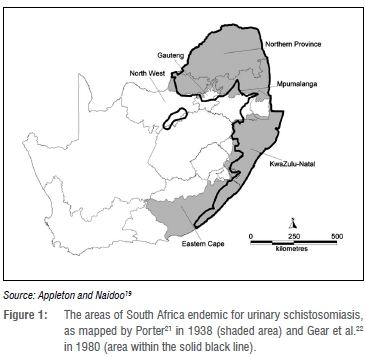
By 1934, sufficient information had been gathered on urinary schisto-somiasis to produce the first map of the geographical distribution of the disease in South Africa.21 The map was drawn from data collected between the 1860s and 1932 and was published in 1938.21 Further research and surveys on schistosomiasis were carried out in South Africa after the first map was published and using disease prevalence data collected between the early 1950s through to the late 1970s, the Atlas of Bilharzia in South Africa was published by Gear et al.22 This map was quite similar to the first map published by Porter in 1938.21
Efforts to get schistosomiasis recognised as a serious public health issue and to persuade health authorities to take measures to control the disease started as early as the 1960s.23 After noticing in other surveys how serious the effects of the disease were, Bhagwandeen24 carried out an investigation of the clinical pathology of urogenital schistosomiasis in Durban. High prevalence as well as high intensity infections were noted for both urinary and intestinal schistosomiasis among Africans.25 The study also showed severe hepatic damage among the patients. However, despite this study by Bhagwandeen and several other studies, schistosomiasis was still not regarded as a serious health problem by the public health authorities. Therefore, no government-run control programme was carried out in the 1960s, 1970s or 1980s.25 To justify this omission, the authorities often asked the question, 'How many people die of urogenital schistosomiasis?'24 By 1989, Utroska estimated the average prevalence of schistosomiasis in the country to be 17.5% with 1 575 000 infected children under 15 years.25
Unique cases of schistosomiasis recorded
A study by Pitchford in 1966 reported evidence that Schistosoma mattheei, a form of intestinal schistosomiasis found mainly in sheep, had been found in people in Humansdorp, South Africa. However, in 1986, Pitchford reported that the human infection rates caused by S.mattheei were not as high as those caused by S. haematobium and S. mansoni.26
There were 14 cases of spinal cord schistosomiasis recorded between August 1985 and March 1987 in KwaZulu-Natal. Twelve patients were of Zulu origin and two patients were Caucasians.27 Of these, two patients required surgery and three patients were treated with praziquantel only and recovered.27 The other nine patients were treated with praziquantel and corticosteroids; six patients responded well to treatment (although one patient relapsed) and three patients showed a reduction in conus size.27 The reported prevalence of spinal schistosomiasis is low and is believed to be an under-reported condition.27
In 2006, an 11-year-old girl in Port St Johns (Eastern Cape Province) presented with an itchy genital rash; she had no history of sexual abuse and was in good health.28 She was later diagnosed with vulval schistosomiasis. This case occurred after a study carried out in the district from 1987 to 1989 revealed a prevalence of 42% of S. haematobium infection among schoolchildren in the area.28 Vulval schistosomiasis is classified under female genital schistosomiasis and is not a common diagnosis in the endemic areas of South Africa. At the Department of Anatomical Pathology at Walter Sisulu University in the Eastern Cape, only 20 cases of this condition were recorded from 1986 to 2000.28 At the Department of Anatomical Pathology at Nelson R Mandela School of Medicine (also in the Eastern Cape), 27 cases of vulval schistosomiasis were recorded from 1994 to 1998.28
Control programme efforts in South Africa
Plans made by South Africa to control schistosomiasis
The success of any schistosomiasis control programme requires long-term commitment. Three important aspects have contributed to the success of control programmes in other countries over the years.29 These aspects are (1) recognising the public health importance of schistosomiasis, (2) the political will and commitment to utilising local resources for control and (3) readily available public health facilities for the delivery and maintenance of control interventions.30-32 In line with these control programmes, the Department of Health in South Africa put together a document titled 'The Primary Health Care Package for South Africa - A set of norms and standards', in an attempt to incorporate schistosomiasis management into the primary healthcare system.33 The norms and standards were intended to be used as planning guidelines by district and provincial health planners to help assess the unmet needs of their population and to draw up plans to bring services up to national standards. The document includes guidelines on the management of schistosomiasis, i.e. treatment, prevention and active surveillance of the disease in primary healthcare facilities in endemic areas in South Africa.33
These guidelines33 on treatment and control strategies require every clinic in endemic areas to have the latest copy of Bilharzia in South Africa by Gear et al.22 Each clinic is required to be well stocked with anthelminthic drugs and must have posters and information leaflets to educate the public on the disease.33 Any dam, river or pond near a clinic in a schistosomiasis endemic area must have a notice board about the danger of children swimming there if the Environmental Health Officer has identified it as a habitat for host snails.33 The staff are expected to know whether or not the clinic is in an area endemic for schistosomiasis. The staff should know basic information about schistosomiasis and be able to give correct information to patients on the life cycle of the schistosomiasis host snail and how to prevent future infections.33 The staff are expected to help with mass prevention or treatment projects initiated by the district, e.g. treating schoolchildren in areas endemic for schistosomiasis.33 The staff are also expected to educate schoolteachers, pupils and parents on the district advocated control.33
This strategy provides an integrated approach involving treatment, prevention and active surveillance, but unfortunately, it has not been implemented in primary healthcare facilities. Schistosomiasis control continues to be a low priority among health authorities in South Africa34,35 despite the fact that schistosomiasis is endemic in South Africa and remains a public health concern among high risk groups, i.e. pre-schoolers, school-age children, women of childbearing age and adolescents.22,34 South Africa harbours over 25.7 million people at risk of schistosomiasis, with an estimated 4.5 million infections annually.35 In order for South Africa to show that schistosomiasis has been successfully controlled, no new infections should be observed over a given period of time, or the prevalence should significantly be reduced.36 These outcomes can only be assured if a surveillance system such as the one described above is properly implemented in primary healthcare facilities in endemic areas.
WHO recommendations
Globally, schistosomiasis is regarded as an important health issue which requires attention because of the significant negative consequences it has both on the economy and on public health.32,37 Interest in schistosomiasis control was revived during the 54th World Health Assembly held in 2001.38 Although WHO recommended large-scale distribution of praziquantel to at-risk populations living in endemic areas in the 1970s and 1980s, it was only at the 54th World Health Assembly that chemotherapy was endorsed officially as the key public-health strategy to fight schistosomiasis. South Africa endorsed resolution WHA54.19, which calls on member states to take effective steps to control schistosomiasis and soil transmitted helminths.38 The following is an excerpt from the resolution WHA54.19.38 All member states were urged to38:
1. sustain successful control activities in low-transmission areas in order to eliminate schistosomiasis and soil-transmitted helminth infections as a public-health problem
2. give high priority to implementing or intensifying control of schistosomiasis and soil-transmitted helminth infections in areas of high transmission while monitoring drug quality and efficacy
3. ensure access to essential drugs against schistosomiasis and soil-transmitted helminth infections in all health services in endemic areas for the treatment of clinical cases and groups at high risk of morbidity such as women and children, with the goal of attaining a minimum target of regular administration of chemotherapy to at least 75% and up to 100% of all school-age children at risk of morbidity by 2010
4. promote access to safe water, sanitation and health education
5. ensure that any development activity likely to favour the emergence or spread of parasitic diseases is accompanied by preventive measures to limit its impact
In 2009, urinary schistosomiasis was renamed 'urogenital schistosomiasis' because in 75% of infected people, the disease affects both the urinary and genital tracts.4
What South Africa has achieved
In October 1997, South Africa set up its first helminth control programme in KwaZulu-Natal. This programme was funded and run entirely by the government.23 The programme targeted both geohelminths (Ascaris lumbricoides, Necator americanus, Trichuris trichiura) and schistosomaiasis.23 This was a primary school based programme and about 1.5 million primary school children were to be treated with praziquantel on a regular basis in high intensity areas.31,36 The programme was in line with WHO guidelines. Children are likely to benefit from treatment because of the early stage of their chronic lesions and because schoolgoing children present with the highest prevalence and infection intensities of schistosomiasis.2,36,37 The increasing number of children attending school in KwaZulu-Natal provided a good opportunity for a cost-effective programme.39
The overall aim of the first helminth control programme in KwaZulu-Natal was to significantly reduce prevalence and morbidity resulting from schistosomiasis and soil-transmitted helminths by the end of 2010.23 The goals of the programme were to23:
1. permanently reduce morbidity caused by helminth infections in children living in endemic areas
2. improve sanitation (e.g. build school toilets, build latrines in the community, identify cheap building materials)
3. create links between parents, teachers and health personnel in the area in order to fight poor health amongst children
4. improve the children's learning potential by improving their health status
Children are especially vulnerable to schistosomiasis and may become physically and intellectually compromised because infection may result in anaemia, attention deficit disorder, learning disabilities, school absenteeism and high school dropout rates.3,5,34,40 The effects on child development may result in a generation of adults disadvantaged by the irreversible consequences of this infection.42 Endemic areas were identified using the Atlas of Bilharzia in Southern Africa23which helped to provide estimates of the population at risk of the disease and to adequately plan for the control programme.
A high total prevalence and a large proportion of high intensity infections of S. haematobium were observed.24,40 This observation indicated that, according to the WHO guidelines, it is necessary to regularly treat schoolchildren in KwaZulu-Natal with praziquantel.24,40 According to Appleton and Kvalsvig23, a decline in infection was recorded during this intervention. A significant reduction (95.3%) in egg excretion 3 weeks after treatment and a 94.1% cure rate for heavy infections were recorded.3 It was proposed that one treatment per year, at the end of summer, was sufficient to keep infection and intensities low.23 Unfortunately, this programme did not gain the necessary support and there is currently no treatment strategy of any kind in any area of the country.3
Praziquantel
Praziquantel is the drug of choice for the treatment of all forms of schistosomiasis.3 It is highly effective in killing adult worms.3 With praziquantel, the cure rates for S. haematobium are 75-85% and 63-85% for S. mansoni.3In studies conducted in North, West and East Africa, South America and Asia, mass treatment with praziquantel in endemic areas has been shown to reduce the burden of urogenital schistosomiasis.1,3,41 Studies have shown that a single treatment given in childhood seems to prevent half the cases of genital schistosomiasis in women.8 Therefore, it is vital to do an early intervention through mass treatment programmes in endemic communities in South Africa, to prevent the serious impact of schistosomiasis.
Currently, praziquantel is given as a single oral dose of 40 mg/kg, with food and drink, in order to minimise gastrointestinal side effects.3,42 In South Africa, only Bayer's Biltricide® (praziquantel) is available for the treatment of schistosomiasis.3 The Department of Health purchases praziquantel for schistosomiasis at a cost of USD4.49 per tablet making mass treatment programmes unaffordable and almost impossible to run in South Africa.3 Praziquantel is not even fully stocked in local clinics at the moment as it is too expensive.3
Contrary to the current practice in South Africa, other countries accept WHO-accredited generic praziquantel.3 These simple, effective, cheap and commercially available generics are of excellent quality, have been on the market for more than 20 years3 and have been used widely in schistosomiasis control programmes. Countries with successfully established schistosomiasis national control programmes using generic praziquantel supplied free of charge include Zambia, Nigeria, Mozambique and Uganda.43 There has been no evidence of development of resistance to praziquantel. These generics are not available in South Africa because only one brand of praziquantel is registered for the treatment of schistosomiasis.3 Therefore, for South Africa to be able to successfully control schistosomiasis and its debilitating consequences, donated or inexpensive and affordable generic medication must be made available for mass treatment programmes in endemic areas.
WHO strategic plan to eliminate schistosomiasis by 2025
Over the years, several countries have implemented schistosomiasis control programmes successfully. These countries include Brazil, Burkina Faso, China, Egypt and Uganda.44 Significant reduction in urogenital schistosomiasis infection and morbidity has been achieved by mass treatment. In countries that have not been able to successfully control schistosomiasis, the major obstacle has been limited access to praziquantel as well as unavailability of water, sanitation, environmental health infrastructure or the necessary resources to implement schistosomiasis control.
The WHO came up with a strategic plan to eliminate schistosomiasis in endemic countries by 2025.44 This plan can be used as a guide by the South African government. One of the goals is to successfully control schistosomiasis morbidity by 2020. This goal has been defined as 75% national coverage for schistosomiasis control and less than 5% prevalence of heavy infections recorded in endemic countries.44 If this goal is achieved by 2020, it may be possible to eliminate schistosomiasis as a public-health problem in South Africa by 2025. By increasing schistosomiasis control activities in endemic areas and ensuring an adequate supply of praziquantel and the other resources required, this goal is attainable. The monitoring and evaluation of schistosomiasis control can be undertaken by local health facilities. Primary health facilities and school health teams across the country should be supplied with praziquantel for treating infected patients. The communities should also be provided with potable water in order to avoid contact with contaminated water as well as adequate sanitation to decrease contamination of water bodies.44 Educational programmes are needed to encourage less recreational water contact, and bridges or stepping stones across rivers need to be provided.
Conclusion and recommendations
South Africa still has much to achieve in order to successfully control and decrease the prevalence of schistosomiasis in endemic areas. South Africa was unable to achieve the minimum goal of 75% treatment coverage in school-aged children at risk by 2010 as stated by resolution WHA54.19 of the World Health Assembly. Several factors contributed to this failure: the lack of support from public health authorities as the government still underestimates the seriousness of schistosomiasis, the price of praziquantel in South Africa and the lack of availability of praziquantel in public health facilities as well as the lack of blanket permission to use WHO-accredited generic drugs. Failure to incorporate schistosomiasis control into the general healthcare system, e.g. failure of primary healthcare systems to perform specific control tasks, is another contributing factor. Successful schistosomiasis control can only be achieved by taking into account other factors such as health education, improvements in sanitation (including preventing urination and defecation in or near the water body by building latrines and educating people on the importance of using them) and lastly, mass-treating the population in endemic areas. The latter method has been found to have a dual effect, by also reducing short- and even longer-term morbidity.1
To improve the control of schistosomiasis, a comprehensive primary healthcare district based schistosomiasis control programme needs to be established within the primary healthcare system. This programme could be led by school health teams at district level. It is important that there is increased awareness of the deleterious effects of schistosomiasis and the school health teams should provide health education to ensure health literacy about schistosomiasis amongst educators and learners and increase such awareness in the community. This programme could contribute to strengthening the health system as it offers the opportunity for linking mobile teams undertaking preventive work with schools, thus enabling the health service to reach many South African children before they need to access a primary healthcare clinic. The current initiative to re-engineer primary healthcare provides an opportunity for such efforts.
As a Schedule 4 drug, praziquantel currently must be dispensed by a professional nurse and the rescheduling of this drug, which does not have serious side effects, should be considered. Urgent action is also required to register the less expensive generic forms of praziquantel tablets in South Africa as many of these generics have been, and are currently used in other countries throughout the world. The negative effects of female genital schistosomiasis on the genital system is now recognised, as is the association with HIV infection. A well-structured schistosomiasis control programme therefore has the potential to contribute to a reduction in the prevalence of HIV amongst young women.
Acknowledgements
We acknowledge those who are working to ensure that South African children are treated timeously for schistosomiasis.
Authors' contributions
K.M. drafted the article; PJ.N. was the project leader; M.T., PJ.N. and E.F.K. made conceptual contributions, added to the content and approved the final manuscript.
References
1. Fenwick A, Webster JP Blair L, Fleming FM, Zhang Y Garba A. The schistosomiasis control initiative (SCI): Rationale, development and implementation from 2002-2008. Parasitology. 2002;136(13):1719-1730. http://dx.doi.org/10.1017/S0031182009990400 [ Links ]
2. Steinmann P Keiser J, Bos R, Tanner M, Utzinger J. Schistosomiasis and water resources development: Systematic review, meta-analysis, and estimates of people at risk. Lancet Infect Dis. 2009;6(7):411-425. http://dx.doi.org/10.1016/S1473-3099(06)70521-7 [ Links ]
3. Berge S, Kabatereine N, Gundersen SG, Taylor M, Kvalsvig JD, Mkhize-Kwitshana Z, et al. Generic praziquantel in South Africa: The necessity for policy change to provide cheap, safe and efficacious schistosomiasis drugs for the poor, rural population: Review. South Afr J Epidemiol Infect. 2011;26(1):22-25. [ Links ]
4. Mbabazi P Andan O, Fitzgerald DW, Chitsulo L, Engels D, Downs JA. Examining the relationship between urogenital schistosomiasis and HIV infection. PLoS Negl Trop Dis. 2011;5(12):e1396. http://dx.doi.org/10.1371/journal.pntd.0001396 [ Links ]
5. Saathoff E, Olsen A, Magnussen P, Kvalsvig JD, Becker W, Appleton CC. Patterns of Schistosoma haematobium infection, impact of praziquantel treatment and re-infection after treatment in a cohort of schoolchildren from rural KwaZulu-Natal/South Africa. BMC Infect Dis. 2004;4(1):40. http://dx.doi.org/10.1186/1471-2334-4-40 [ Links ]
6. World Health Organization. Schistosomiasis fact sheet no. 115 [document on the Internet]. c2012 [cited 2014 Apr 04]. Available from: http://www.who.int/mediacentre/factsheets/fs115/en/index.html [ Links ]
7. King CH, Dangerfield-Cha M. The unacknowledged impact of chronic schistosomiasis. Chronic Illn. 2008;4(1):65-79. http://dx.doi.org/10.1177/1742395307084407 [ Links ]
8. Kjetland EF, Leutscher P, Ndhlovu P. A review of female genital schistosomiasis. Trends Parasitol. 2012;28(2):58-65. http://dx.doi.org/10.1016/j.pt.2011.10.008 [ Links ]
9. Poggensee G, Kiwelu I, Weger V Göppner D, Diedrich T, Krantz I, et al. Female genital schistosomiasis of the lower genital tract: Prevalence and disease-associated morbidity in northern Tanzania. J Infect Dis. 2000;181(3):1210-1213. http://dx.doi.org/10.1086/315345 [ Links ]
10. Kjetland EF, Kurewa EN, Ndhlovu PD, Midzi N, Gwanzura L, Mason PR, et al. Female genital schistosomiasis - A differential diagnosis to sexually transmitted disease: Genital itch and vaginal discharge as indicators of genital Schistosoma haematobium morbidity in a cross-sectional study in endemic rural Zimbabwe. Trop Med Int Health. 2008;13(12):1509-1517. http://dx.doi.org/10.1111/j.1365-3156.2008.02161.x [ Links ]
11. World Health Organization (WHO). Report of an informal working group on urogenital schistosomiasis and HIV transmission. Geneva: WHO; 2009. Available from: http://whqlibdoc.who.int/hq/2010/WHO_HTM_NTD_PCT_2010.5_eng.pdf [ Links ]
12. Harms G, Feldmeier H. Review: HIV infection and tropical parasitic diseases - Deleterious interactions in both directions? Trop Med Int Health. 2002;7(6):479-488. http://dx.doi.org/10.1046/j.1365-3156.2002.00893.x [ Links ]
13. Johnson LF, Lewis DA. The effect of genital tract infections on HIV-1 shedding in the genital tract: A systematic review and meta-analysis. Sex Transm Dis. 2008;35(11):946-959. http://dx.doi.org/10.1097/OLQ.0b013e3181812d15 [ Links ]
14. Jourdan PM, Roald B, Poggensee G, Gunderson SG, Kjetland EF. Increased vascularity in cervicovaginal mucosa with Schistosoma haematobium infection. PLoS Negl Trop Dis. 2011;5(6):e1170. http://dx.doi.org/10.1371/journal.pntd.0001170 [ Links ]
15. UNAIDS. Fact sheet: Adolescents, young people and HIV [document on the Internet]. c2012 [cited 2014 Apr 04]. Available from: http://www.unaids.org/en/media/unaids/contentassets/documents/factsheet/2012/20120417_FS_ adolescentsyoungpeoplehiv_en.pdf [ Links ]
16. Department of Health. 2011 National Antenatal Sentinel HIV and Syphilis Prevalence Survey, South Africa. Pretoria: Department of Health; 2012. Available from: http://www.health-e.org.za/2012/12/11/2011-national-antenatal-hiv-syphilis-prevalence-survey-released/ [ Links ]
17. World Health Organization (WHO). Making health services adolescent friendly. Geneva: Department of Maternal, Child and Adolescent Health, WHO; 2012. Available from: http://apps.who.int/iris/bitstream/10665/75217/V9789241503594_eng.pdf [ Links ]
18. World Health Organization (WHO). Adolescent friendly health services: An agenda for change. Geneva: WHO; 2002. Available from: http://whqlibdoc.who.int/hq/2003/WHO_FCH_CAH_02.14.pdf [ Links ]
19. Appleton CC, Naidoo I. Why did schistosomiasis disappear from the southern part of the Eastern Cape? S Afr J Sci. 2012;108(1/2), Art. #411, 11 pages. http://dx.doi.org/10.4102/sajs.v108i1/2.411 [ Links ]
20. Rabello A. Diagnosing schistosomiasis. Mem Inst Oswaldo Cruz. 1997;92(5):669-676. [ Links ]
21. Porter A. The larval trematodes found in certain South African Mollusca with special reference to schistosomiasis (bilharziasis). Johannesburg: South African Institute of Medical Research; 1938. [ Links ]
22. Gear JHS, Pitchford RJ, Van Eede JA. Atlas of bilharzia in South Africa. Johannesburg: South African Institute for Medical Research; 1980. [ Links ]
23. Appleton CC, Kvalsvig JD. A school-based helminth control programme successfully implemented in KwaZulu-Natal. South Afr J Epidemiol Infect. 2006;21(2):55-67. [ Links ]
24. Bhagwandeen SB. The clinico-pathological manifestations of schistosomiasis in the African and the Indian in Durban. Pietermaritzburg: University of Natal Press; 1968. [ Links ]
25. Utroska JA, Chen MG, Dixon H, Yoon S, Helling-Borda M, Hogerzeil HV et al. An estimate of global needs for praziquantel within schistosomiasis control programmes. Geneva: WHO; 1989. [ Links ]
26. Pitchford RJ. Some aspects of bilharzia in southern Africa. S Afr Med J. 1986;70(suppl):80-82. [ Links ]
27. Haribhai HC, Bhigjee AI, Bill PLA, Pammenter MD, Modi G, Hoffmann M, et al. Spinal cord schistosomiasis: A clinical, laboratory and radiological study, with a note on herapeutic aspects. Brain. 1991;114(2):709-726. http://dx.doi.org/10.1093/brain/114.2.709 [ Links ]
28. O'Mahony D, Banach L, La Grange LL. A case of vulval schistosomiasis. S Afr Fam Pract. 2007;49(9):42-43. http://dx.doi.org/10.1080/20786204.2007.10873640 [ Links ]
29. Utzinger J, Bergquist R, Shu-Hua X, Singer BH, Tanner M. Sustainable schistosomiasis control - The way forward. Lancet. 2003;362(9399):1932-1934. http://dx.doi.org/10.1016/S0140-6736(03)14968-9 [ Links ]
30. Chitsulo L, Engels D, Montresor A, Savioli, L. The global status of schistosomiasis and its control. Actatropica. 2000;77(1):41-51. http://dx.doi.org/10.1016/s0001-706x(00)00122-4 [ Links ]
31. Engels D, Chitsulo L, Montresor A, Savioli L. The global epidemiological situation of schistosomiasis and new approaches to control and research. Actatropica. 2002;82(2):139-146. http://dx.doi.org/10.1016/s0001-706x(02)00045-1 [ Links ]
32. World Health Organization (WHO). Prevention and control of schistosomiasis and soil-transmitted helminthiasis. A report of the WHO Expert Committee. Technical report series 912. Geneva: WHO; 2002. [ Links ]
33. Department of Health. The primary health care package for South Africa -A set of norms and standards. Pretoria: Department of Health; 2000. Available from: http://www.hsph.harvard.edu/population/vaccination/southafrica2.doc [ Links ]
34. Johnson CL, Appleton CC. Urban schistosomiasis transmission in Pietermaritzburg, South Africa. South Afr J Epidemiol Infect. 2005;20(3):103-107. [ Links ]
35. Wolmarans CT, De Kock KN. The influence of health education on the prevalence, intensity and morbidity of Schistosoma haematobium infections in children over a two-year period in the Limpopo Province, South Africa. South Afr J Epidemiol Infect. 2009;24(1):13-17. [ Links ]
36. Moodley I, Kleinschmidt I, Sharp B, Craig M, Appleton CC. Temperature-suitability maps for schistosomiasis in South Africa. Ann Trop Med Parasitol. 2003;97(6):617-627. http://dx.doi.org/10.1179/000349803225001445 [ Links ]
37. Taylor M. Global trends in schistosomiasis control. Bull World Health Organ. 2008;86(10):738. http://dx.doi.org/10.2471/BLT.08.058669 [ Links ]
38. World Health Organization (WHO). WHA54.19 Schistosomiasis and soil-transmitted helminth infections. Resolutions and decisions 1 [document on the Internet]. No date [cited 2014 Apr 04]. Available from: http://www.who.int/neglected_diseases/mediacentre/WHA_54.19_Eng.pdf [ Links ]
39. Taylor M, Jinabhai CC, Couper I, Kleinschmidt I, Jogessar VB. The effect of different anthelmintic treatment regimens combined with iron supplementation on the nutritional status of schoolchildren in KwaZulu-Natal, South Africa: A randomized controlled trial. Trans R Soc Trop Med Hyg. 2001;95(2):211-216. http://dx.doi.org/10.1016/S0035-9203(01)90171-3 [ Links ]
40. Guyatt HL, Brooker S, Kihamia CM, Hall A, Bundy DA. Evaluation of efficacy of school-based anthelmintic treatments against anaemia in children in the United Republic of Tanzania. Bull World Health Organ. 2001;79(8):695-703. [ Links ]
41. King CH. Parasites and poverty: The case of schistosomiasis. Actatropica. 2010;113(2):95-104. http://dx.doi.org/10.1016/j.actatropica.2009.11.012 [ Links ]
42. King CH. Lifting the burden of schistosomiasis - Defining elements of infection-associated disease and the benefits of antiparasite treatment. J Infect Dis. 2007;196(5):653-655. http://dx.doi.org/10.1086/520522 [ Links ]
43. World Health Organization (WHO). Report of the WHO informal consultation on the use of praziquantel during pregnancy/lactation and albendazole/ mebendazole in children under 24 months. Geneva: WHO; 2002. p. 1-34. [ Links ]
44. World Health Organization (WHO). Schistosomiasis: Progress report 20012011 and strategic plan 2012-2020. Geneva: WHO; 2013. Available from: www.who.int/iris/bitstream/10665/78074/1/9789241503174_eng.pdf [ Links ]
 Correspondence:
Correspondence:
Myra Taylor
Public Health Medicine, 2nd floor, George Campbell Building, Science Drive
Howard College Campus, University of KwaZulu-Natal
Durban 4001, South Africa
Email: Taylor@ukzn.ac.za
Received: 02 Feb. 2015
Revised: 19 May 2015
Accepted: 21 May 2015














