Services on Demand
Article
Indicators
Related links
-
 Cited by Google
Cited by Google -
 Similars in Google
Similars in Google
Share
South African Journal of Science
On-line version ISSN 1996-7489
Print version ISSN 0038-2353
S. Afr. j. sci. vol.108 n.7-8 Pretoria Jan. 2012
NEWS AND VIEWS
The limits of observational epidemiology: hormonal contraception and women's risk of HIV infection
Landon Myer
Centre for Infectious Diseases Epidemiology & Research, School of Public Health & Family Medicine, University of Cape Town, Cape Town, South Africa
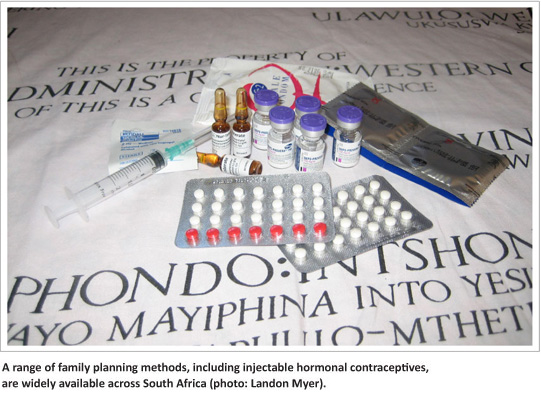
For almost two decades, scientists around the world have grappled with the question of whether women's use of hormonal contraception increases their risk of becoming infected with the human immunodeficiency virus (HIV). For the health of women across South Africa, the stakes are incredibly high. There are over 5 million HIV-infected women and men living in the country, and the vast majority are of reproductive age.1 At the same time, millions of women use hormonal contraception: injectable hormones and oral contraceptive pills are used by approximately 28% and 10% of South African women of reproductive age, respectively.2 Providing hormonal contraception is a critical part of promoting women's health in South Africa and globally; if hormonal contraceptives were to increase women's risk of acquiring HIV, it could be a tragedy of modern public health.
This question re-emerged recently with the publication by Heffron et al.3 in Lancet Infectious Diseases of an international study suggesting that HIV acquisition is more common in women who use hormonal contraception (both oral and injectable) compared to women who did not. The study was conducted in 1314 couples in which the male partner was HIV-positive and the female partner was HIV-negative. In observing these couples over 1-2 years of follow-up, the researchers found that the occurrence of new HIV infections was about twice as high in the women that used hormonal contraception than in the women who did not.
This finding has rekindled the debate on the putative association between hormonal contraception and HIV,4,5 and is certainly cause for public health concern. At the same time, this work forces to the surface a broader, ongoing discussion regarding the limits of scientific knowledge that can be generated through observational epidemiological studies.6 Several observational studies have suggested a similar association between different forms of hormonal contraception and HIV, complementing the results of Heffron et al.3 However, there are as many published studies on this question that have shown no such association.7,8,9,10 (By way of disclosure, the author has led a local study showing no association.7)
Observational epidemiological research faces several basic challenges in trying to identify the causes of specific diseases by observing patterns of 'risk factors' (any exposure, behaviour or condition that may be a cause of disease) within individuals and populations. Foremost among the concerns facing observational epidemiology is the ubiquitous phenomenon of confounding, in which the correlations of potential risk factors create a biased result, making it difficult to discern true causality. In the case of hormonal contraception and HIV, the likely sources of confounding include sexual behaviours, such as condom use, that are associated both with the use of hormonal contraception and with women's acquisition of HIV infection. For example, women who use hormonal contraception are less likely to use condoms than those who do not (since the contraceptive effect of condoms is a principle reason for their use in many settings), and thus are at a higher risk of sexually transmitted HIV infection for reasons other than their hormonal contraceptive use.
Confounding is a fundamental concern that snakes throughout epidemiological research. In observational studies, the most that scientists can hope for is to anticipate, measure and attempt to adjust for confounding effects using various statistical tools.11 (This approach is in contrast to experimental epidemiological studies, in which investigators use tools such as randomisation to help minimise confounding effects and other biases.12) When we find large associations between risk factors and disease outcomes, confounding effects are unlikely to be responsible for the entire association. But it is impossible to remove the effects of confounding definitively. This fact leads most investigators conducting epidemiological research towards highly tentative conclusions, and, occasionally, significant reversals. For example, use of hormone replacement therapy (HRT) in postmenopausal women was widely thought to reduce women's risk of cardiovascular disease based on observational epidemiological studies from the USA. Only more recently has the confounding effect of socio-economic status in these studies come to be fully appreciated -women who use HRT are typically wealthier and less likely to experience cardiovascular disease (at least in the USA) than women who do not use HRT.13
Epidemiologists have an arsenal of statistical tools to confront confounding and related phenomena. New analytical refinements to deal with confounding effects emerge every few years and promise new hope to the discipline, but the challenge that confounding presents to observational epidemiological research is more fundamental. As we study patterns of disease in populations, and search for smaller and smaller associations, the ability to discern spurious, confounded effects from true, causal effects is increasingly fraught with uncertainty.14 As in the case of the association between hormonal contraception and women's HIV acquisition, the results produced by any single observational study should be interpreted with tremendous caution; inferences about causality in epidemiological research emerge only over time after repeated investigations of a particular question in different populations.
In this instance, the World Health Organization convened a panel to review the body of evidence on this question, including the study by Heffron et al.3 The panel's conclusion was that the results were too mixed overall, and individual studies too flawed, to draw any conclusions.15 Yet, observational epidemiological research still faces the ubiquitous challenge of confounding.
References
1. Joint United Nations Programme on HIV/AIDS. Report on the Global AIDS Epidemic, 2010. Geneva: UNAIDS; 2010. [ Links ]
2. United Nations Population Division. World contraceptive use, 2011. New York: Department of Economic and Social Affairs, United Nations; 2011. [ Links ]
3. Heffron R, Donnell D, Rees H, et al. Use of hormonal contraceptives and risk of HIV-1 transmission: A prospective cohort study. Lancet Infect Dis. 2012;12(1):19-26. http://dx.doi.org/10.1016/S1473-3099(11)70247-X [ Links ]
4. Daly CC, Helling-Giese GE, Mati JK, et al. Contraceptive methods and the transmission of HIV: Implications for family planning. Genitourin Med. 1994;70:110-117. [ Links ]
5. Bulterys M, Chao A, Habimana P, et al. Incident HIV-1 infection in a cohort of young women in Butare, Rwanda. AIDS. 1994;8:1585-1591. http://dx.doi.org/10.1097/00002030-199411000-00010 [ Links ]
6. Taubes G, Mann C. Epidemiology faces its limits. Science. 1995;269(5221):164-169. http://dx.doi.org/10.1126/science.7618077 [ Links ]
7. Myer L, Denny L, Wright TC, Kuhn L. Prospective study of hormonal contraception and women's risk of HIV infection in South Africa. Int J Epidemiol. 2007;36(1):166-174. http://dx.doi.org/10.1093/ije/dyl251 [ Links ]
8. Klienschmidt I, Rees H, Delany S, et al. Injectable progestin contraceptive use and risk of HIV infection in a South African family planning cohort. Contraception. 2007;75(6):461-467. http://dx.doi.org/10.1016/j.contraception.2007.02.002 [ Links ]
9. Kiddugavu M, Makumbi F, Wawer MJ, et al. Hormonal contraceptive use and HIV-1 infection in a population-based cohort in Rakai, Uganda. AIDS. 2003;17:233-240. http://dx.doi.org/10.1097/00002030-200301240-00014 [ Links ]
10. De Vincenzi I. A longitudinal study of human immunodeficiency virus transmission by heterosexual partners. European Study Group on Heterosexual Transmission of HIV. N Engl J Med. 1994;331:341-346. http://dx.doi.org/10.1056/NEJM199408113310601 [ Links ]
11. Shapiro S. Causation, bias and confounding: A hitchhiker's guide to the epidemiological galaxy part 2. Principles of causality in epidemiological research: Confounding, effect modification and strength of association. J Fam Plann Reprod Health Care. 2008;34(3):185-190. http://dx.doi.org/10.1783/147118908784734873 [ Links ]
12. Pocock SJ, Elbourne DR. Randomised trials or observational tribulations? New Engl J Med. 2000;342:1907-1909. http://dx.doi.org/10.1056/NEJM200006223422511 [ Links ]
13. Grodstein F, Clarkson TB, Manson JE. Understanding the divergent data on postmenopausal hormone therapy. N Engl J Med. 2003;348(7):645-650. http://dx.doi.org/10.1056/NEJMsb022365 [ Links ]
14. Davey Smith G. Reflections on the limitations of epidemiology. J Clin Epidemiol. 2001;54:325-331. http://dx.doi.org/10.1016/S0895-4356(00)00334-6 [ Links ]
15. World Health Organization. Hormonal contraception and HIV: Technical statement. WHO/RHR/12.08. Geneva: WHO; 2012. [ Links ]
 Correspondence to:
Correspondence to:
Landon Myer
School of Public Health and Family Medicine,
Falmouth Building, Faculty of Health Sciences,
University of Cape Town,
Observatory 7925, South Africa
Email: Landon.myer@uct.ac.za
© 2012. The Authors. Licensee: AOSIS OpenJournals. This work is licensed under the Creative Commons Attribution License.














