Services on Demand
Article
Indicators
Related links
-
 Cited by Google
Cited by Google -
 Similars in Google
Similars in Google
Share
South African Dental Journal
On-line version ISSN 0375-1562
Print version ISSN 0011-8516
S. Afr. dent. j. vol.73 n.4 Johannesburg May. 2018
OBSERVATIONAL STUDY
Diabetic status of patients presenting for dental treatment
M NegiI; H HolmesII; LXG StephenIII
IBChD, MSc. Division of Oral Medicine and Periodontics, Faculty of Dentistry, University of the Western Cape
IIBChD, MSc, MChD. Division of Oral Medicine and Periodontics, Faculty of Dentistry, University of the Western Cape
IIIBChD, MChD, PhD. Division of Oral Medicine and Periodontics, Faculty of Dentistry, University of the Western Cape
ABSTRACT
INTRODUCTION: Untreated Diabetes mellitus (DM) has severe long-term complications. In 2008, DM affected 4.6% of the South African population.1 Glycemic status is an indicator of the blood glucose levels.
AIM AND OBJECTIVES: To assess the glycemic status and presence of intra-oral soft tissue lesions in a sample of patients presenting at UWC Maxillofacial outpatient clinic.
Design and Methods
A cross-sectional observational study was carried out on 400 adult patients, 18 years or older. Pregnant patients were excluded. Random blood glucose levels (RBG) were measured In mmol/L on samples of peripheral blood (finger prick) using a glucometer.
RESULTS: Of the 400 patients, 51 (12,7%) were either known diabetic patients or newly diagnosed (prediabetic and diabetic) and 15 (29.4%) of these 51 patients were unaware of their status (undiagnosed). Of the diabetic patients (n=40), 17 (42.5%) had soft tissue lesions, which occurred in 137 of the 349 patients having normal blood glucose levels (39.2%). Oral candidiasis was seen in 25% (n=10) of diabetic patients, compared with the prevalence of 18.3% amongst those with normal blood glucose levels (n=64 out of 349).
CONCLUSION: The study supports the need for general screening of all patients to facilitate early diagnosis of this disease.
INTRODUCTION AND LITERATURE REVIEW
Diabetes Mellitus (DM) is the most prevalent endocrine disorder, affecting approximately 6% of the population worldwide.2 In 2010, the global prevalence amongst adults aged 20-79 years was 6.4%, and is projected to be 7.7% by 2030.
In developed countries, the increase between 2010 and 2030 is expected to be approximately 20% and may be as high as 69% in developing countries.3 Similarly, the prevalence of type 2 DM In children and adolescents is on the increase and appears to be related to obesity. DM, commonly referred to as diabetes.
Is becoming more common in younger persons, highlighting the need for prevention and early diagnostic strategies, to reduce treatment demand and morbidity of diabetic related complications.4
A substantial proportion of any population remains undiagnosed (UDM)5 because diabetes has an asymptomatic, latent period during which the disease is not clinically detected. Diabetes Is referred to as a "silent killer" because, if not diagnosed early, it results in acute and/or chronic complications. Acute complications include hyperglycemia, hypoglycemia and ketoacidosis. Chronic complications comprise retinopathy, neuropathy, nephropathy, cardiovascular complications, delayed wound healing6 and death, especially in poorly controlled and pregnant diabetics.7
Diabetes is a metabolic disorder caused by an absolute or relative deficiency of insulin. This can be due to low insulin production by the pancreatic beta cells, or insulin resistance in the peripheral tissues.8 When insulin is lacking or its action is stopped, glucose cannot enter cells and this results in loss of energy and weakness. In addition, glucose accumulates in the blood (hyperglycemia) and overflows into the urine (glycosuria) with subsequent increased urine volume (polyuria).
Prediabetes (intermediate hyperglycemia) is defined by a blood sugar level that is higher than normal but not high enough to be diabetic. The glycemic variables are higher than normal, but lower than diabetes thresholds. Without lifestyle changes, prediabetics are at risk of progressing to type 2 diabetes.9
Haemoglobin A1C test (HbA1c) is the gold standard confirmatory test for diabetes and captures chronic glucose exposure for a period of three months. It is more likely to be confirmatory in establishing a diagnosis of diabetes than any single measure of glucose.1 All other investigations (fasting plasma glucose FPG, 75-g oral glucose tolerance test OGTT, random plasma glucose RPG) require a repeat test (either FPG or 75-g OGTT) to confirm a diagnosis of diabetes.11
The diagnosis of diabetes (Table 1) is established by a fasting plasma glucose level of >126mg/dL (7.0mmol/L) on two separate occasions; a plasma glucose s 200mg/dL (11.1 mmol/L) after 2-h OGTT, HbA1c 2 6.5% (48mmol/L) or random plasma glucose > 200 mg/dL (11.1 mmol/L), along with symptoms of hyperglycemia.11
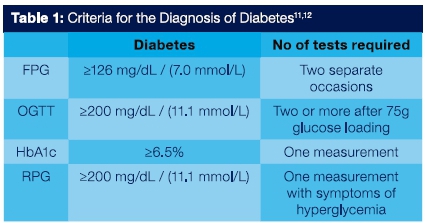
The disadvantage of the fasting plasma glucose test includes the need to abstain from food and drink for 8 hours prior to phlebotomy procedure and that there is a 12-15% day-to-day variance in fasting blood glucose values.13
The OGTT is considered a first-line diagnostic test. Limitations of this test include poor reproducibility and the need for patient compliance as an eight-hour fast is needed before the 75-g glucose load, followed by drawing blood two hours later.1 The total prevalence of pathologic glucose metabolism was substantially higher based on HbA1c values than from OGTT.1
RBG levels of 200 mg I dl_ (11.1 mmol I L) or higher associated with classic symptoms of diabetes such as polyuria, polydipsia, weight loss, blurred vision and fatigue, are diagnostic. Lower RBG values as 140 - 180 mg I dL (7.8 - 10.0 mmol I L) have a fairly high specificity of 92-98%; thus patients with such values should undergo more definitive testing. A low sensitivity of 3955% limits the use of RBG testing.1
HbA1C values have currently been permitted by the American Diabetes Association ADA as a screening and diagnostic measurement for DM. One advantage of using this test is that it does not require fasting. However, it must be performed in a clinical laboratory because of the lack of standardization of point-of-care testing. Limitations of HbA1C test includes low sensitivity and possible racial disparities. Interferences are also possible by medications such as high-dose salicylates; vitamins C, Ε and conditions such as severe iron deficiency anemia.1,13
There is a strong relationship between oral health and diabetic status. Poorly controlled diabetics are susceptible to dental problems such as gingivitis, periodontitis, recurrent periodontal abscess, delayed healing after extraction, dry socket, oral Infections like candidiasis, xerostomia, neurosensory disorders which result in glossodynia, stomatopyrosis or burning mouth syndrome, hypogeusia and other oral dysesthesias.16
The rising prevalence of Type 2 DM, especially in the younger population, the delay in diagnosis and the morbidity associated with complications of undiagnosed diabetes emphasize the need for screening, prevention and early diagnostic strategies. The purpose of this study was to investigate the utility of random blood glucose collection as a screening tool to facilitate early referral and definitive diagnosis of diabetes mellitus amongst outpatients attending the Maxillofacial Clinic at the UWC dental faculty. The term diabetes will be used for patients with a RBG value > 11.1 mmol/L or fasting blood glucose FBG value >7.0 mmol/L.
AIM AND OBJECTIVES
To assess the glycemic status, as an indicator for diabetes, of patients presenting for dental treatment at the Maxillofacial Outpatient Department at Tygerberg Hospital. To assess the Incidence of undiagnosed diabetes mellitus. To determine the prevalence of diabetes mellitus in patients presenting for dental treatment and to describe associated intraoral soft tissue lesions.
DESIGN AND METHODS
A cross-sectional observational study was done on n=400 patients who presented for treatment at the Maxillofacial Outpatient's Department at Tygerberg Hospital. They were adults > 18 years of age. Children and adolescents <18 years of age, patients who are unable to open their mouth for any reason, those with sepsis and pregnant women were excluded.
A blood drop was collected from consenting patients who met the inclusion criteria. Participants were advised to rinse their hands with water and antiseptic solution whereafter the side of a fingertip was lanced, a blood drop applied to the (Accu-Chek®) test strip which was inserted into the Accu-Chek® blood glucose monitor, to measure the glycemic status.
The data collected was recorded on a collection form, transferred to an Excel® spread sheet and analyzed by a statistician using the same program.
THE RESULTS
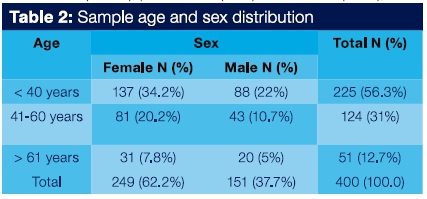
Of the 400 study participants, 38.5% were male and 61.5% were female. Their age range was 18 to 81 years with a mean of 39.8 years. The respondents below the age of 40 comprised 56.2%, 31% were between 41 and 60 years and 12.7% were above the age of 60 years.
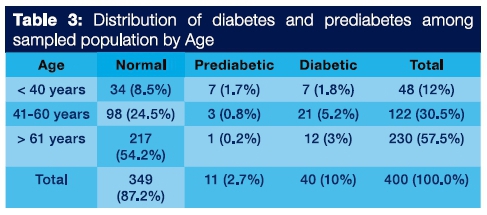
Patients were categorized into three groups based on blood glucose level: normal (n=349), pre-diabetic (n=11) and diabetic (n=40).
Of the subjects aged below 40 years, 7 (1.8%) were pre-diabetic and 7 (1.7%) were diabetic. Among participants aged between 41-60 years, 3 (0.8%) were pre-diabetic and 21 (5.2%) were diabetic, whereas only one (0.2%) pre-diabetic and 12 (3%) diabetic subjects were above 60 years of age.
Blood glucose measurements were obtained from 309 and 91 patients using the Random blood glucose method and fasting blood glucose method respectively, summarized in Table 4. Of the 400 patients included in the study.
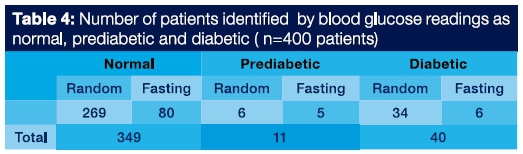
-
The prevalence of diabetes was 10% (n= 40).
-
The incidence was 1% (n=4).
-
Prediabetic patients accounted for 2.7% (n= 11).
In total 51 (12.7%) out of 400 were either known diabetic patients or newly diagnosed (prediabetic and diabetic) and 15 (29.4%) out of these 51 patients are unaware of their status (undiagnosed).
Table 5 shows the blood glucose levels (normal, prediabetic and diabetic) for the fasting group. Seven (7.6%) out of 91 patients were referred for diabetes testing.
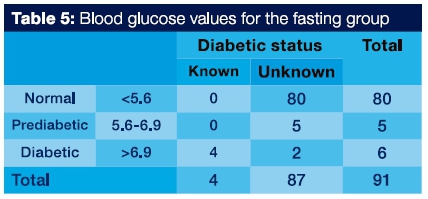
In these patients the time between food intake and blood glucose measurement was a minimum of 8 hours and their blood glucose measurements were categorized as FPG. Five patients (5.4%) had FBG measurements between 5.6 and 6.9 mmol/dl and 6 (6.5%) had FPG measurements of > 6.9 mmol/L. Four (4.3%) of known diabetic patients had a FBG of > 6.9 mmol/L.
Table 6 shows the blood glucose levels (normal, pre diabetic and diabetic) obtained from the RBG group. Eight (2.5%) patients were referred for diabetes testing.
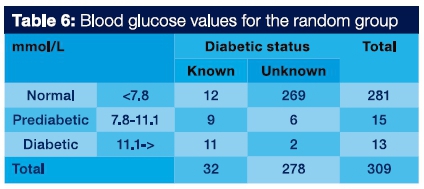
In the RBG group, 15 (4.8%) patients had blood glucose measurements between 7.8 and 11.1 mmol/L and 13 (4.2%) had blood glucose readings of >11.1 mmol/L.
Thirty-two (10.3%) patients were known diabetics and 8 (2.5%) out of 309 patients were referred for confirmation of their diabetes status (6 prediabetic, 2 diabetic).
SOFT TISSUE LESIONS, CANDIDA AND SMOKING
Soft tissue lesions (candidiasis, fissured tongue, geographic tongue, irritation fibroma and traumatic ulcer) were recorded in 160 patients, 23(18%) of whom had above normal blood glucose levels. The prevalence of soft tissue lesions seen is summarized in Table 7. Clinically evident oral candidiasis was seen in 64/137 patients with normal blood glucose levels and in 14/23 patients with elevated blood glucose levels. Forty-five participants with blood glucose levels above normal (prediabetic and diabetic) had soft tissue lesions, 27.4% of which were oral candidiasis. In comparison, of the participants whose blood glucose readings were within the normal range, 39% had soft tissue lesions, 18% of which was oral candidiasis.

In the FBG group, clinically evident soft tissue lesions were recorded in n=30/91 (32.9%) patients, 50% of whom had blood glucose levels > 7 mmol/L (40% were in the prediabetic range and 31 % had normal blood glucose levels). Oral candidiasis accounted for 33.3%, 40% and 17.5% of these soft tissue lesions in the diabetic, prediabetic and normal group respectively.
In the RBG group, clinically evident soft tissue lesions were recorded in n=140/309 (45%) patients, of whom 41% had blood glucose levels > 11 mmol/L (66.6% were in the prediabetic range and 41.6% had normal blood glucose levels). Oral candidiasis accounted for 23.5%, 33% and 18% of these soft tissue lesions in the diabetic, prediabetic and normal group respectively.
Soft tissue lesions were recorded in 42.5% (n=17) of all diabetic patients (n=40), compared with non-diabetic individuals 39.2% (n=137 out of 349). Of the 17 patients who had soft tissue lesions, 13 (76%) had blood glucose levels >15 mmol/L. Oral candidiasis was recorded in 25% (n=10) of diabetic compared with non-diabetic participants 18.3% (n=64 out of 349).
Of the 51 hyperglycemic patients, 45% (n=23) had soft tissue lesions; 23.5% (n=12) had oral candidiasis, compared with the 18.3% of patients with normal blood glucose levels.
Data analysis showed that 103 (25.7%) of 400 patients wore dentures. Oral candidiasis was evident in 12.5% of diabetics who wore dentures.
Other soft tissue lesions recorded included fissured tongue (17.5%), geographic tongue (4%), irritation fibroma (4%) and traumatic ulcers (4%).
DISCUSSION
The purpose of the study was to evaluate the glycemic status (as an indicator) of undiagnosed diabetes mellitus, to determine the prevalence of diabetes mellitus in patients presenting for dental treatment and to describe associated intraoral soft tissue lesions.
The sample comprised n=400 participants, whose ages ranged between 18-81 years, with a mean of 39.8 years. Most respondents were female aged between 18-40 years. The age range and gender profile of this study was comparable to one in rural North India,17 in which 59.2% of participants were below the age of 40 years, 32.2% were between 41 - 60 years and 8.6% above 60 years of age.
Previous studies have mainly only screened people 40 years and older, but recent studies4,17-19 have included and subsequently diagnosed patients below 40 years with Type II diabetes mellitus. In the present study, the percentage of prediabetic patients was highest in the age group below 40 years of age. Prediabetic states have been shown to progress to diabetes mellitus in 2-10 years when no intervention is put in place.20 This supports the Inclusion of screening a broader age range for investigation in the current study. This would facilitate early diagnosis and thereby Intercept undiagnosed chronic exposure to hyperglycemia and Its long-term cumulative effects.
In the present study, the greatest proportion of diabetic patients was seen in participants older than 40 years of age. This was expected and comparable to other studies,3,17 which revealed a higher rate of diabetes between ages 40 to 60 years.
This study revealed that the incidence of undiagnosed DM was 1.0%. This is comparable to other studies in which incidence estimates of 1.2% and 1% were reported in the Western Cape and in Zambia respectively,19 despite the study's smaller sample size. A study in rural India17 reported an incidence of diabetes of 2.9%. This higher percentage of newly diagnosed patients could be related to the previous exclusion of patients younger than 40 years of age from diabetes screening programs. It is known that persons of Indian decent reportedly have the highest proportion of diabetes,18 and the exclusion of possible prediabetic patients therefore precluded them from early intervention strategies. Notably, the proportion of prediabetic participants in the Indian study17 was very high (10.6%) compared with our study findings. In the present study, ethnicity was not taken into account.
The prevalence of DM in this study was 10%. This is higher than prevalence values in a previous Western Cape and Zambian study,19 which were 7.2 % and 3.5% respectively. That study was large and included eight communities within the Western Cape and 16 communities in Zambia. In our study, the sample size was considerably smaller and the geographical area was limited, thus the high prevalence values may be reflective of the lack of awareness of high blood glucose levels in general.
In healthy individuals, blood glucose levels do not vary widely throughout the day21 because the relevant hormones (insulin and glucagon) work synergistically to prevent plasma glucose levels from shifting too high or low. Blood glucose levels higher than 11 mmol/L may indicate a problem when measuring RBG. In this study two different tests were used to measure glycemic status namely, FBG and RBG. Both measured a single episode of glucose exposure and can be used for screening purposes. These findings were used to facilitate the referral of at-risk patients for the measurement of HbA1C levels or to provide dietary counseling. (The HbA1C level provides information for the average of three months plasma glucose exposure.)
In total 51 (12.7%) of the 400 patients were either known diabetic patients or newly diagnosed (prediabetic and diabetic) and 15 (29.4%) of these 51 patients had been unaware of their status (undiagnosed). All the screened patients whose blood glucose readings were above normal were referred for confirmatory tests to measure their HbA1C. Previously known diabetic patients with elevated above normal glycemic readings were also refereed to their doctors for further evaluation.
The range of soft tissue lesions seen in prediabetic and diabetic patients were candida 27.4%, fissured tongue 17.5%, geographic tongue 4%, irritation fibroma 4%, traumatic ulcer 4%. Other soft tissue lesions were too few for any inferences to be made with regard to their presence and diabetic status. The study revealed that 42.5% (n=17) of diabetic patients (n= 40) had a soft tissue lesion, which was higher than in those with normal blood glucose levels 39.2% (n=137 out of 349) and 25% (n=10) of patients who were diabetic had oral candidiasis, compared with those with normal blood glucose levels 18.3% (n=64 out of 349).
In total, 45% of prediabetic and diabetic patients (n=23 of 51 patients) had soft tissue lesions, 27.4% (n=14 of 51 patients) of whom had candidiasis. This was greater than in participants with normal blood glucose measurements. Denture wearing, smoking and inadequate oral hygiene could be additional predisposing factors. Similarly, a Malaysian study22 found the prevalence of oral mucosal lesions to be higher in diabetic patients (45.5%). It has been reported that poor glycemic control predispose to oral candida infection oral, which occurs with increased frequency in patients with DM.23
Early diagnosis would allow management to prevent or delay development of diabetes and its complications and thereby reduce associated diabetic related costs. Chatterjee et al. in 2010 revealed that screening seems to be cost saving compared with not screening from a health system perspective, and potentially cost-neutral from a social assessment.24 Our study findings recommend that attention should be paid to early screening for DM.
CONCLUSION
In conclusion, diabetes is one of the most widespread diseases and its prevalence is increasing significantly. Furthermore, it has a definite relationship with oral health.
Screening enables early diagnosis of individuals who are unaware of their glycemic status and also identifies persons at risk for possible future development of the condition. Screening thereby facilitates early management for both at risk and diabetic persons and is likely to be less than the cost of the subsequent treatment. RBG testing method is easier, more rapid, is cost-effective and less invasive than laboratory measurement of plasma glucose concentration.
RECOMMENDATION
This study co-incidentally demonstrates the potential of public health facilities, such as dental clinics, for the screening of various conditions of public health concern such as Diabetes Mellitus, HIV and Tuberculosis.
RBG is a useful method to screen for prediabetes and diabetes to facilitate referral of patients to measure HbAIC.
ACRONYMS
DM : Diabetes Mellitus
RBG : Random Blood Glucose
References
1. Pretorius M. 2014. Knowledge and Practices of Occupational Health Nurse Practitioners in the Management of Diabetes Mellitus in South Africa (Doctoral dissertation, Cape Peninsula University of Technology). [ Links ]
2. Adeghate E, Schattner P, Dunn E.. An update on the etiology and epidemiology of Diabetes Mellitus. Annals of the New York Academy of Sciences 2006;1084: 1-29. [ Links ]
3. Shaw JE, Sicree RA, Zimmet, PZ. Global estimates of the prevalence of diabetes for 2010 and 2030. Diabetes Research and Clinical Practice 2010; 87(1):4-14. [ Links ]
4. Reinehr T. Type 2 diabetes mellitus in children and adolescents. World J Diabetes 2013;4(6) :70-81. [ Links ]
5. Sosale A, Kumar KP, Sadikot SM, Nigam A, Bajaj S, Zargar AH, Singh SK. Chronic complications in newly diagnosed patients with Type 2 diabetes mellitus in India. Indian Journal of Endocrinology and Metabolism 2014:18(3):355. [ Links ]
6. Huang ES, Laiteerapong N, Liu JY, John PM, Mottet HH, Karter AJ. Rates of complications and mortality in older patients with diabetes mellitus: the diabetes and aging study. JAMA Internal Medicine, 2014;174(2) :51-8. [ Links ]
7. Global report on diabetes (WHO), 2016. Available from: <http://apps.who.int/iris/bitstream/10665/204871/1/9789241565257_eng.pdf> [ Links ]
8. Sousa MGDM, Costa ADLL, Roncalli AG. Clinical study of the oral manifestations and related factors in type 2 diabetics patients. Brazilian Journal of Otorhinolaryngology, 2011;77(2):145-52. [ Links ]
9. Tabák AG, Herder C, Rathmann W, Brunner EJ, Kivimäki Μ. Prediabetes: a high-risk state for diabetes development. The Lancet 2012;379(9833):79-90. [ Links ]
10. American Diabetes Association. Diagnosis and Classification of Diabetes Mellitus. Diabetes Care, 33(Supplement 1), 2010 :pp. S62-S69. [ Links ]
11. Kharroubi AT, Darwish HM Diabetes mellitus: The epidemic of the century. World Journal of Diabete 2015; 6(6: 850. [ Links ]
12. American Diabetes Association. Diagnosis and Classification of Diabetes Mellitus. Diabetes Care, 32 (Suppl 1), 2009 : pp.S62-S67. [PMC free article] [PubMed] [ Links ]
13. Patel Ρ, Macerollo A. Diabetes mellitus: diagnosis and screening diabetes, 2010.100, p.13. [ Links ]
14. Hjellestad ID, Astor MC, Nilsen RM, Softeland E, Jonung T. HbA 1c versus oral glucose tolerance test as a method to diagnose diabetes mellitus in vascular surgery patients. Cardiovascular Diabetology 2013;12(1):79. [ Links ]
15. Saudek CD, Herman WH, Sacks DB, Bergenstal RM, Edelman, Davidson MB. A new look at screening and diagnosing diabetes mellitus. The Journal of Clinical Endocrinology & Metabolism 2008; 93(7) :2447-53. [ Links ]
16. Jha R, Kalyani P, Bavishi R.. Oral manifestations of diabetes. Journal of Research in Medical and Dental Science 2014 ; 2(3) :6-8. [ Links ]
17. Thomas T, Prabhata S, Valsangkar S. Diabetes screening and the distribution of blood glucose levels in rural areas of North India. Journal of Family and Community Medicine 2015 ;22(3) :140. [ Links ]
18. Ramachandran A. Epidemiology of type 2 diabetes in Indians. Journal of the Indian Medical Association 200;100(7): 425-7. [ Links ]
19. Bailey SL, Ayles H, Beyers N, Godfrey-Faussett P, Muyoyeta M, du Toi, Ε, Yudkin, JS, Floyd S. Diabetes mellitus in Zambia and the Western Cape province of South Africa: Prevalence, risk factors, diagnosis and management. Diabetes Research and Clinical Practice 2016;118 :1-11. [ Links ]
20. Fonseca VA. Identification and treatment of pre-diabetes to prevent progression to type 2 diabetes. Clinical Cornerstone 2008; 9(2) :51-61. [ Links ]
21. Bloodglucose, WebMD, 2015. Available from: http://www.webmd.com/diabetes/guide/blood-glucose#1> [ Links ]
22. AI-MAweri SAA, Ismail NM, Ismail A R I, Al-Ghashm A. Prevalence of oral mucosal lesions in patients with type 2 diabetes attending Hospital Universiti Sains Malaysia. The Malaysian Journal of Medical Sciences 2013 ; 20(4): 39. [ Links ]
23. Soysa NS, Samaranayake LP, Ellepola ANB.. Diabetes mellitus as a contributory factor in oral candidosis. Diabetic Medicine 2006; 23(5) :455-9. [ Links ]
24. Chatterjee R, Naraya KV, Lipscomb J, Phillips LS. Screening adults for pre-diabetes and diabetes may be cost-saving. Diabetes Care 2010;33(7) :1484-90. [ Links ]














