Serviços Personalizados
Artigo
Indicadores
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares em Google
Similares em Google
Compartilhar
South African Dental Journal
versão On-line ISSN 0375-1562
versão impressa ISSN 0011-8516
S. Afr. dent. j. vol.73 no.3 Johannesburg Abr. 2018
CASE REPORT
A foreign object found in the ostiomeatal complex during dental implant planning: A case report
Smit DAI; Swart LII; Morkel; JAIII
IDirk Smit:, BChiD (Stellenbosch/Western Cape), MChiD (Comm Dent), Dentist; Department of Maxillo-Facial and Oral Surgery, University of the Western Cape, South Africa
IIL Swart:, BChD(Stellenbosch) Part time Consultant; Department of Maxillo-Facial and Oral Surgery, University of the Western Cape, South Africa
IIIJA Morkel:, BChD, MBChB, MChD (Stellenbosch), FCMFOS (SA) Head (Academic); Department of Maxillo-Facial and Oral Surgery, University of the Western Cape, South Africa
INTRODUCTION.
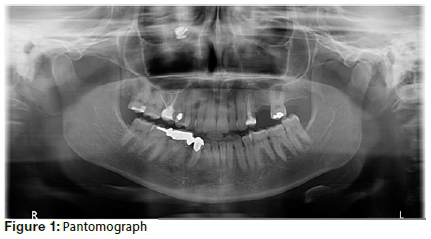
A general dental practitioner referred a 40-year-old Caucasian female to a maxillofacial and oral (MFOS) surgeon for the placement of an implant in the area of tooth number 25 (under the ISO System) and the evaluation of a neighbouring tooth (24) which had a poor prognosis. The patient's medical history indicated pulmonary stenosis, mild hypothyroidism and endometriosis. Previous surgery had involved three Caesarean sections. Her medication included Oratane, vitamins and homeopathic thyroid medications. She was allergic to codeine. During the extra-oral examination, no abnormalities were detected. The intra-oral examination revealed that teeth 14, 35 and 45 were missing (removed previously as part of orthodontic treatment) and that teeth 25, 26, 28 and 44 had been lost. The patient was radiographically examined by pantomograph and a cone-beam computerized tomography (CBCT) scan with the pantomograph revealing restored teeth at 18, 16, 15, 24, 27 and a bridge extending from 43-46. Teeth 16 and 24 had been treated endodontically, and notable alveolar bone loss was evident across the 24-28 area. The maxillary sinuses were pneumatized. A radio-opaque structure was detected in the right ostiomeatal complex (OMC). No opacification of the right maxillary sinus was detected. The CBCT scan confirmed the radio-opaque area in the right OMC, bulging into the ethmoid infundibulum. The differential diagnosis of this radio-opaque area in the OMC was that of either a fungus ball or a foreign object.
TREATMENT PLAN
The proposed treatment plan was to replace the missing and unsaveable premolars in the second quadrant with dental implants and to load immediately. The final restoration was to be carried out by the referring dentist. The patient was also referred to an ear, nose and throat (ENT) specialist with the request that the radio-opaque area be examined and assessed. The report from the ENT specialist proposed the removal of the foreign object under general anaesthetic, which would provide the opportunity to proceed simultaneously with the implant surgery.
TREATMENT
The root rest of 24 was removed atraumatically. Two 4.3-mm Nobel Active® implants were placed in the 24 and 25 areas (with immediate loading). Suturing was done with 3.0 Vicryl® rapide stitches. An endoscopic evaluation of the right OMC was performed and the foreign body was subsequently carefully removed transnasally via an endoscopic sinus approach to avoid injury to the orbital floor. A biopsy specimen was then sent for histological evaluation. There were no complications during surgery and the patient recovered well.
HISTOLOGICAL INVESTIGATION
Macroscopic investigation of the biopsy specimen revealed three grey-yellowish fragments which were each 3-5 mm in cross section and reminiscent of calculus. Microscopic investigation revealed oral tissue with the presence of scattered fibrovascular connective tissue containing a chronic inflammatory cell infiltrate that was partially covered by respiratory epithelium. The sub-mucus layer contained mucus glands and a chronic inflammatory infiltrate. The presence of a black pigmented foreign body was noted, having the appearance of dental amalgam restorative material. No further pathological analysis was done to confirm whether the particles were indeed amalgam.
DISCUSSION
A 1965 description of the ostiomeatal complex considered it as a conjunct of anatomic structures which is primarily responsible for drainage of the anterior paranasal sinus.1 It forms the functional part of the anterior ethmoid complex which provides the final common pathway for drainage and ventilation of the frontal, maxillary and anterior ethmoid cells.2 A generalized theory is that obstruction of the OMC may lead to the formation of a fungus ball which is a diseased condition in the anterior ethmoids and frontal sinuses which then produces symptoms similar to those of chronic unilateral rhinosinusitis. However, a study conducted by Tsai et al. did not support this hypothesis and their findings suggested that even with the presence of a fungal ball, the OMC can still function normally in terms of draining and ventilation.3
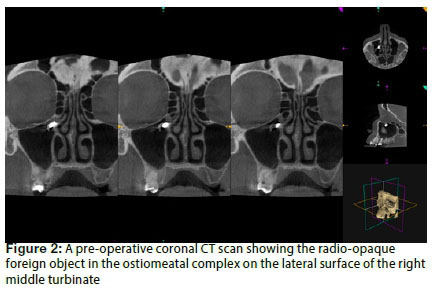
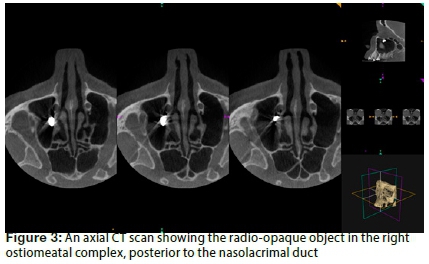
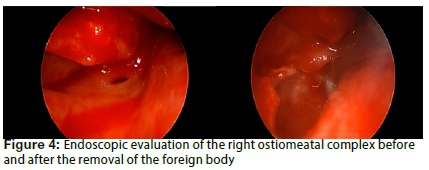
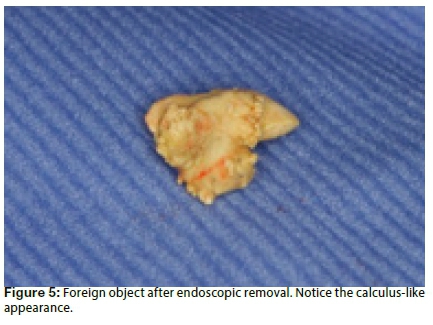
It is very rare to find a foreign object in the paranasal sinuses obstructing the OMC and causing maxillary disease such as is evident in the present case.4 The fact that microscopic histology revealed material similar to amalgam, makes this case even more intriguing. Whilst no chemical analysis was performed on the material, it may be reasonable to assume that it was amalgam, based on the microscopic description.
Only a few case studies report dental restorative material located near the maxillary sinus.5-8 Of these, only one involved obstruction of the OMC and most of these cases were associated with maxillary disease.9
The case report published by Raman and Padgham in 2007 provides a possible explanation of how the dental amalgam migrated to the OMC: "It could have entered the maxillary sinus during a restorative procedure" and in their case, the patient began experiencing symptoms shortly after the dental procedure. In the current case it is uncertain whether the patient had a history of maxillary symptoms as she was asymptomatic on presentation and had given no indication of maxillary disease during the assessment for the planned dental implants.
Considering the endodontic treatment of the 16 and the extensive restoration performed on the patient several years ago, it can only be assumed that, during this procedure, amalgam particles had entered the maxillary sinus. Over time, the particles could have been migrated to the OMC under the influence of the mucocilliary clearance mechanism found in the mucosal lining of the maxillary antrum. However, this is only a postulation, given the limited number of similar cases previously reported.
It may be relevant to note the difference between the present case and that reported by Raman and Padgham in that this patient had no acute sinusitis, which may indicate that the foreign object could have been present for several years.4 Also, despite the obstruction, the patient provided no history of chronic sinusitis. It was a coincidence that the radio-opaque object was discovered during the radiographic examination.
CONCLUSION
Cone Beam Computed Tomography has become indispensable in the surgical planning of dental implantology since it describes details of the anatomical structures in the vicinity of the surgical site and is superior to the limited view provided by two-dimensional radiographs. The present case highlights the importance of such full radiological evaluation as an adjunct to clinical assessment of the dental patient before any implant surgery is contemplated.
ACRONYMS
CBCT : cone-beam computerized tomography
OMC : ostiomeatal complex
Reference
1. Lloyd GAS, Lund VJ, Scadding GK. CT of the paranasal sinuses and functional endoscopic surgery: a critical analysis of 100 symptomatic patients. The Journal of Laryngology & Otology 1991; 105:181-5. [ Links ]
2. Stammberger, HR, Kennedy DW. Paranasal sinuses: terminology and nomenclature. The Anatomic Terminology Group. Ann Otol Rhinol Laryngol Suppl 1995; 167:7-16. [ Links ]
3. Tsai TL, Guo YC, Ho CY, Lin CZ. The role of ostiomeatal complex obstruction in maxillary fungus ball. Journal of American Academy of Otolaryngology-Head and Neck Surgery 2006; 134:494-8. [ Links ]
4. Raman V, Padgham N. A case of tooth-filling antral rhinolithiasis presenting with blockage of the ostiomeatal complex. The British Journal of Radiology 2007; 80 (960): 299-300. Available at: http://www.ncbi.nlm.nih.gov/pubmed/18065637. [ Links ]
5. George MK, Rashid N, Pahor AL. Dental filling in maxillary sinus. Br Med J 1991; 3112: 976. [ Links ]
6. Manjaly G, Pahor AL. Antral rhinolithiasis and tooth filling. ENT J 1994; 73: 676-9. [ Links ]
7. Bodner L, Ferit T, Bar-Ziv J. Teeth in the maxillary sinus - imaging and management. J Laryngol Otol 1997; 111:820-4. [ Links ]
8. Connor SEJ, Chavda SV, Pahor AL. Computed tomography evidence of dental restoration as aetiological factor of maxillary sinusitis. J Laryngol Otol London 2000; 114:510-4. [ Links ]
9. Hasbini AS, Hadi U, Ghafari J. Endoscopic removal of third molar obstructing the ostiomeatal complex. ENT J 2001; 80:667. [ Links ]
 Correspondence:
Correspondence:
Dr Dirk Smit
Tel 021 937 3085
Email dirkiesmit@gmail.com














