Serviços Personalizados
Artigo
Indicadores
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares em Google
Similares em Google
Compartilhar
South African Dental Journal
versão On-line ISSN 0375-1562
versão impressa ISSN 0011-8516
S. Afr. dent. j. vol.72 no.6 Johannesburg Jul. 2017
http://dx.doi.org/10.17159/2519-0105/2017/v72no6a4
CLINICAL COMMUNICATION
Localised "vertical relapse" following orthodontic correction in young growing patients with cleft lip/ palate: Case studies potentially leading to a revision of the retention protocol
S Singh
BSc (Unisa) BDS (Wits), MSc (Dent) UWC, MChD (Orthodontics) UWC. Private Practice in Orthodontics, Durban North, Kwa-Zulu Natal. Tel: 031 564 6501 / 5949, Fax: 031 564 8061. E-mail: sikki@orthodent.co.za
ABSTRACT
Vertical dental relapse following orthodontic treatment has been observed in growing cleft lip and palate patients who had been treated at a Cleft Centre in Kwa-Zulu Natal. It appears that such relapse may occur in those who had had alveolar bone grafts in the cleft area and that it takes place at a time coinciding with the eruption of the maxillary canines. This communication is based on case studies of patients who presented three different types of clefts. All the grafts had been taken from the iliac crest. The observations may indicate a need for an in-depth study to investigate whether teeth erupt normally through iliac crest bone grafts in cleft patients. Confirmation of an altered eruption pattern may indicate a need for a change in retention protocol.
INTRODUCTION
Most cleft lip/ palate (CLP) patients are treated from birth to adulthood, undergoing various phases of treatment delivered by a coordinated team of many care givers. One of the most important aspects of treatment is the objective to achieve orthodontic alignment of the dentition, which has been greatly facilitated by secondary alveolar bone grafting for patients with clefts involving the maxillary alveolus. This has transformed the dental management of these patients, with bone grafting of the cleft area being effected in late childhood (i.e. during late mixed dentition, early permanent dentition). Over the years there has been a steady improvement in the bone grafting procedures leading to enhanced success of the grafts.1-7
However, a major complication of bone grafting techniques is the resorption of the grafted bone in the cleft area, especially if there are no teeth to secure the graft.8 Whilst the scheduling of bone grafts is quite variable and controversial, grafting in the cleft areas is normally done around the ages of 9 years to 11 years, timed to coincide with the eruption of the canine into the graft area. Various studies have indicated that the erupted canine with good periodontal support helps maintain the grafted bone.8,9 It is commonly believed that this supported bone allows for orthodontic tooth movement in the cleft area.9
Today most grafts are harvested from the iliac crest. Other donor sites include the mandibular symphyseal bone and the retromolar pad area, and allografts. A study in Netherlands showed a positive outcome with mandibular symphyseal bone grafted into the cleft area, but, notably, the authors also advocated life-time fixed upper and lower retention for cleft lip/ palate patients.10
Although most cleft lip/ palate patients are missing the maxillary lateral incisors in the cleft area, those that do in fact have these teeth can be considered for an earlier bone graft at age 6-7years. The lateral incisor should preferably be on the mesial side of the cleft. Hence, the recommended age of grafting is variable and is still very controversial.11
A search of the literature has shown no studies or research which have been undertaken of the stability of the dentition in and adjacent to the bone grafted cleft area following orthodontic treatment in young pre-pubertal and pubertal cleft lip/ palate patients. Since grafting is intended to provide bone for the successful stabilization of the dentition in the grafted area, it is warranted to evaluate cases who have received grafts to assess the degree of post treatment stability.
A series of case studies was therefore carried out on cleft lip and palate patients who had received bone grafts. These case presentations show vertical relapse or movement of the dentition adjacent to clefts which had been grafted with iliac crest bone. The type of relapse is localised to teeth adjacent to the cleft area. This appears to not have been previously reported.
OBJECTIVE
To investigate the post-orthodontic stability of well aligned upper teeth in young cleft lip/ palate patients who had had bone grafts placed in the cleft area.
To describe and to evaluate the extent and character of any relapse and to propose suitable retention protocols, amended if necessary.
MATERIALS AND METHODS
The study involved an investigation of four cases which included two patients with unilateral cleft lip/ alveolus, one with a unilateral cleft lip/ palate and one with a bilateral cleft lip/ palate. These are patients from a joint private practice / public service Cleft lip/ palate Clinic in the province of Kwa Zulu Natal in South Africa. The public sector clinic is run under the auspices of the Wentworth Foundation* for Cleft lip/ palate Service, a non-Governmental Organisation (NGO). Most patients at that facility are treated from birth.
All ethical considerations have been taken into account. The necessary permission for publication of patient information has been obtained.
This is a photographic evaluation which depicts and records dental changes in the post orthodontic treatment phase (i.e. retention phase). It is confined to those cleft lip/ palate patients who received bone grafts during the growing phase of life, timed to coincide with the eruption of the maxillary canine. All grafts were from the iliac crest. An outline of the active treatment phase and the passive post treatment phase (retention) is given, showing the changes in the dentition. "Debanding" of patients refers to removal of fixed braces. The patients comprised three young females and one male. All are based in Kwa Zulu Natal, South Africa.
CASE 1: UNILATERAL CLEFT LIP ALVEOLUS
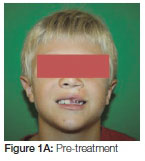
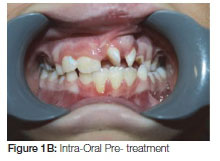
This patient is a young male. He presented with a unilateral cleft lip and alveolus. The primary operation for the lip was performed at about four months of age. A first phase orthodontic treatment was commenced at the age of nine years with a removable expansion device. At that stage the patient had a supernumerary tooth in the cleft area, on the mesial side of the cleft. The lateral incisor (22) was on the distal side of the cleft (Figure 1 A, B).
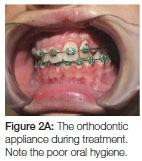
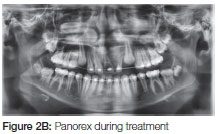
The second phase of fixed orthodontic appliances commenced when the patient was 12 years of age. A bone graft, taken from the iliac crest, was placed within three months of commencement of fixed orthodontic treatment, when the supernumerary was also extracted. Space closure began about six months after placement of the graft, the delay allowing for complete postoperative healing (Figure 2 A, B).
On completion of fixed orthodontics at age 14 years, the patient was debanded and placed on a removable upper retainer and a lower fixed retainer (Figures 3 A, B, C). The discrepancies in the gingival heights of teeth adjacent to the cleft was of immediate concern.
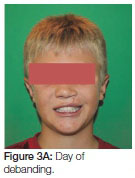
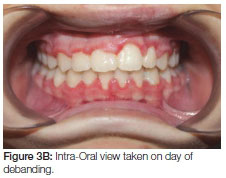
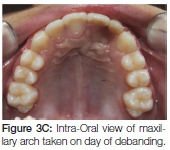
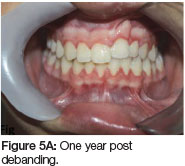
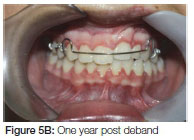
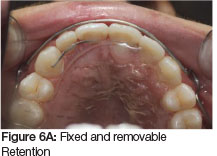
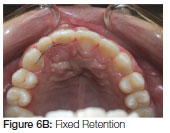
Six months into the retention phase the failure of the eruption of the teeth adjacent to the cleft became apparent (Figure 4). The vertical relapse continued the situation deteriorated further one year into retention (Figure 5 A, B). To prevent further relapse a fixed retainer was placed on the teeth adjacent to the cleft. This will remain in place until re-treatment at the age of 18 years to correct overbite (Figure 6 A, B).
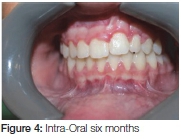
CASE 2: UNILATERAL CLEFT LIP ALVEOLUS
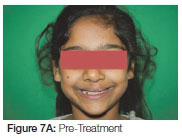
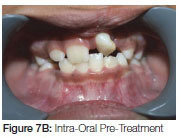
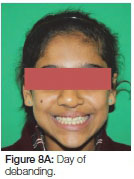
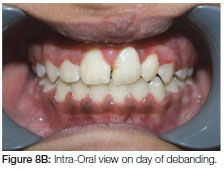
This patient presented, as a young female, with a unilateral cleft lip alveolus (Figure 7 A, B). Her cleft was on the left side with the lateral incisor on the distal aspect of the cleft. Fixed orthodontic treatment was commenced at age nine and a half years. The bone graft, harvested from the iliac crest, was inserted about 12 months after initiation of the fixed appliance orthodontic treatment. No movement of the teeth into the cleft area was undertaken for some six months post-surgery to allow for the consolidation of the graft. The patient was debanded at the age of 11½ years (Figure 8 A, B) and upper removable and lower fixed retention appliances were fitted.
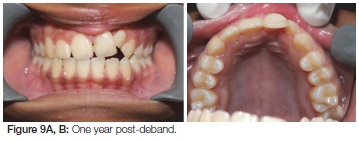
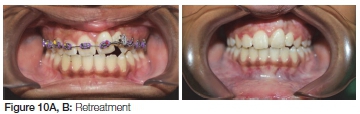
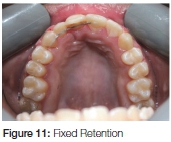
One year post retention, the patient presented with vertical relapse of the teeth adjacent to the cleft (Figure 9 A, B). The patient was retreated with fixed appliances to align the upper teeth (Figure 10 A, B). A fixed "bond-a-braid" retainer was placed on the upper teeth across the cleft area to adjacent teeth (Figure 11). The patient was advised that a third phase of orthodontic treatment could be necessary at 18 years of age.
CASE 3: UNI-LATERAL CLEFT LIP/ PALATE
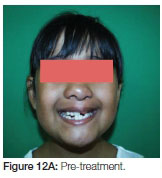
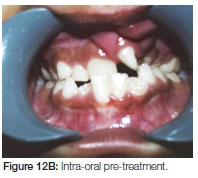
This young female patient presented with a unilateral cleft lip/ palate. The cleft was on the left side. The panorex radiograph showed the presence of a supernumerary tooth on the distal aspect of the cleft and a lateral incisor on the mesial side of cleft. A preliminary phase of orthodontic treatment was started at the age of eight years with a removable expansion device (Figure 12 A, B).
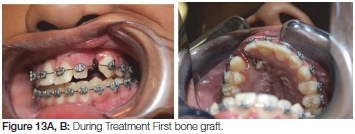
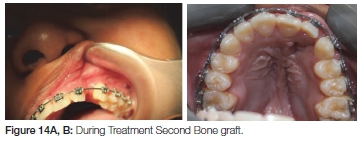
The second phase fixed orthodontics was started at the age of approximately nine years. A bone graft taken from the iliac crest was placed in the cleft area when the patient was one year into the fixed appliance orthodontic treatment (Figure 13 A, B). The supernumerary was actively erupted through the graft in an effort to consolidate the graft. This was un-successful and a second bone graft with extraction of the supernumerary was done a year later (Figure 14 A, B).
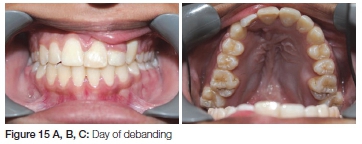
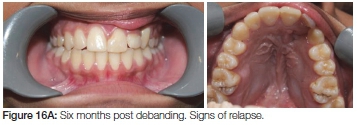
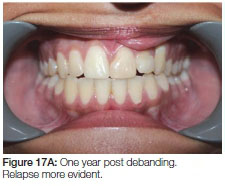
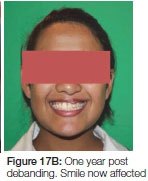
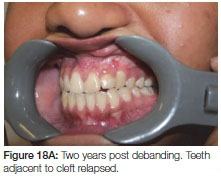
Spaces were closed and the patient was debanded a year later (after almost 40 months of fixed orthodontic treatment). (Figure 15 A, B, C). A removable upper retainer and a lower fixed retainer were placed. Six months into retention a failure of eruption of the teeth adjacent to the cleft could be observed (Figure 16 A, B). Twelve months into retention the teeth adjacent to the cleft showed no signs of erupting any further, with a gradual decrease in the anterior overbite (Figure 17 A, B). Two years post-treatment the trend continued in the cleft area (Figure 18 A, B). A fixed retainer was placed to prevent further relapse. It was decided to retreat the patient at 18 years of age to re-establish a good overbite.
CASE 4: BILATERAL CLEFT LIP/ PALATE
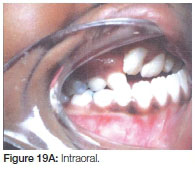
This patient presented in the early mixed dentition as having a bilateral cleft lip/ palate with a Class 3 occlusion. She was missing her lateral incisors. Initial treatment was started with a removable expansion screw and progressed to fixed appliance with continued expansion (Figure 19 A,B,C,).
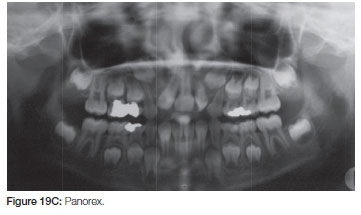
A "Hyrax" expansion appliance was placed in (early permanent dentition stage) to facilitate bone grafting as the canines were erupting. An iliac crest bone graft was placed during fixed orthodontic treatment. On completion of the orthodontic treatment the patient was debanded and a removable upper retainer incorporating the missing laterals was inserted (Figure 20 A, B, C, D).

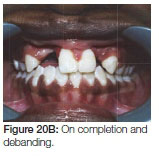
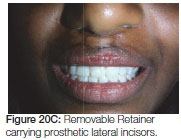
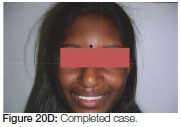
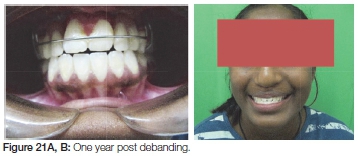
One year post treatment there was a noticeable amount of vertical relapse (Figure 21A, B).
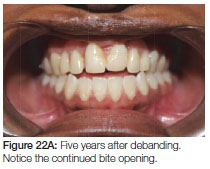
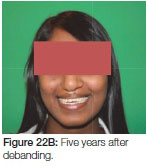
Five years later there was an increase in the anterior open bite (Figure 22A, B).
RESULTS
It is evident in all cases that there was a gradual dental relapse over a period of time which was confined to the area of the cleft, affecting the teeth adjacent to the cleft. In all these cases successful iliac crest bone grafts had been performed. The observed relapse appeared to continue to deteriorate until the late stages of facial growth.
DISCUSSION
This study is a review of cases from a cleft lip/ palate centre and is focused on localised vertical relapse (or failure of eruption?) of the teeth in the cleft area following orthodontic treatment and bone grafting. Although orthodontic relapse is a major problem in cleft lip/ palate patients, few studies have been undertaken to determine the causes of the vertical relapse. The etiology can be varied, for example, a loss or shrinkage of grafted bone, the type of bone or scar tissue. Much has been written about surgical relapse and collapse of the maxillary arch following orthodontics and orthognathic surgery.12-14 Timing of bone grafting should ideally coincide with the eruption of the maxillary canine to ensure stability. No studies have been conducted on understanding the physiology of the eruption of teeth through the bone grafts (autogenic/alloplastic).
Further longitudinal and cross sectional studies is required, using appropriate yardsticks (eg. Goslon Yardstick), and this research should include cleft centres.
CONCLUSION
The vertical relapse, in spite of good retention appliance wear, is possibly due to the failure of eruption of the teeth in the cleft area and may point to the need for an extensive revision in the retention appliance protocol to prevent an open bite vertical relapse. One or two re-treatment phases with fixed appliances are possibly required and patients should be so informed.
The failure of eruption of teeth in the grafted cleft area of the maxilla in the growing patients is a common observation in our cleft clinic. In view of this we have added a new retention protocol. In addition to the post orthodontic removable retainer a fixed bonded retainer is placed on all teeth adjacent to the cleft (the bonded retainer should be placed from one non-cleft area across the cleft to the other non- cleft area, incorporating two or three teeth on either side of the cleft). This precaution, whilst achieving some control, has not been observed to completely control vertical relapse. Further research is required to overcome the vexing question of achieving and maintaining vertical stability.
ACRONYM
CLP: Cleft lip and palate
References
1. Boyne PJ, Sands NR. Secondary bone grafting of residual alveolar and palatal defect. J Oral Maxillofacial Surgery 1972; 30:87-92. [ Links ]
2. Boyne PJ, Sands NR. Combined orthodontic surgical management of residual palate - alveolar defect. American Journal of Orthodontics 1976 70:20-37. [ Links ]
3. Bergland O, Semb G,Abyholm FE. Elimination of the residual alveolar cleft by secondary bone grafting and subsequent orthodontic treatment. Cleft Palate Journal 1986a; 23:175-205. [ Links ]
4. Kalaaji A, Lilja J, Friede H, Elander A. Bone grafting in the mixed and permanent dentition in cleft lip and palate patients: Long term results of the surgeon's experience. J Craniomaxillofacial Surgery 1996; 24:29-35. [ Links ]
5. Enemark H, Krantz Simonsen E, Schahram JE. Mandibular bone graft material for reconstruction of alveolar cleft defects: Long term results. Cleft Palate Craniofacial Journal 2001; 38:155-63. [ Links ]
6. McIntyre GT, Delvin MF. Secondary alveolar bone grafting (CLEFTSiS) 2000-2004. Cleft Palate Craniofacial Journal 2010; 47:66-72. [ Links ]
7. Paterson M, Rae J, Paterson P, Gillgrass T, Devlin Mark, McIntyre G. Secondary alveolar bone grafting (CLEFTSiS) 2007-2010. Cleft Palate Craniofacial Journal 2016; 53:141-6. [ Links ] '
8. Feichtinger M, Mossbock R, Karcher H. Assessment of bone resorption after secondary alveolar bone grafting using three dimensional computed tomography: A three year study. Cleft Palate Craniofacial Journal 2007; 44:142-8. [ Links ]
9. DeWinter G, Quirynen M, Heidbuchel K, Verdonck A, Willems G, Carels C. Dental abnormalities, bone graft quality and periodontal condition in patients with unilateral cleft lip/ palate at different phases of orthodontic treatment. Cleft Palate-Craniofacial Journal 2003; 40:343-50. [ Links ]
10. de Ruiter AD, van der Bilt A, Meijer G, Koole R. Orthodontic treatment results following grafting autologous mandibular bone to the alveolar cleft in patients with complete unilateral cleft. The Cleft Palate-Craniofacial Journal 2010;47:35-43. [ Links ]
11. Shashua D,Omnell ML. Radiographic determination of the position of the maxillary lateral incisor in the cleft alveolus and parameters for assessing its rehabilitation prospects. The Cleft Palate-Craniofacial Journal 2000; 37(1):21-5. [ Links ]
12. Watts G, Antonarakis GS, Forrest CR, Thompson BD, Phillips JH. Is linear advancement related to relapse in unilateral cleft palate orthognathic surgery? The Cleft Palate- Craniofacial Journal 2015; 52:717-24. [ Links ]
13. Saltaji H, Major P, Alfakir H, Al-Saleh MA, Flores-Mir C. Maxillary advancement with conventional orthognathic surgery in patients with cleft lip/ palate: Is it a stable technique? J Oral Maxillofacial Surgery 2012; 70:2859-66. [ Links ]
14. A-Gunaid T, Asahito T, Yamaki M, Hanada K, Takagi R, Ono K, Saito I. Relapse tendency in maxillary arch width in unilateral cleft lip/ palate patients with different maxillary arch forms. The Cleft Palate-Craniofacial Journal 2008; 24:278- 83. [ Links ]
* The Wentworth Foundation, founded by Dr Surandar Singh, renders a free service to indigent cleft lip/ palate patients in the province of KZN. The Wentworth Foundation has been registered as an NGO and a Public Benefit Organisation. Website: www.wentworthfoundation.org.za














