Services on Demand
Article
Indicators
Related links
-
 Cited by Google
Cited by Google -
 Similars in Google
Similars in Google
Share
South African Dental Journal
On-line version ISSN 0375-1562
Print version ISSN 0011-8516
S. Afr. dent. j. vol.71 n.10 Johannesburg Nov. 2016
COMMUNICATION
Lower facial and cervical lymphadenopathy in the context of clinical dentistry
NH WoodI; S MeerII; RAG KhammissaIII; J LemmerIV; L FellerV
IBChD, DipOdont (MFP), MDent (OMP). Department of Periodontology and Oral Medicine, Sefako Makgatho Health Sciences University, Pretoria, South Africa
IIBChD, MDent, FC Path (SA), Department of Oral Pathology, Faculty of Health Sciences, University of the Witwatersrand, Johannesburg, South Africa
IIIBChD, PDD, MSc(Dent), MDent (OMP). Department of Periodontology and Oral Medicine, Sefako Makgatho Health Sciences University, Pretoria, South Africa
IVBDS, HDipDent, FCD(SA)OMP, FCMSAae, Hon. FCMSA, Department of Periodontology and Oral Medicine, Sefako Makgatho Health Sciences University, Pretoria, South Africa
VDMD, MDent (OMP). Department of Periodontology and Oral Medicine, Sefako Makgatho Health Sciences University, Pretoria, South Africa
ABSTRACT
The dental practitioner is in a good position to detect lower facial and cervical lymphadenopathy. A medical history and a physical examination of a patient with lower facial and cervical lymphadenopathy might provide important clues as to the underlying cause. Lower facial or cervical lymphadenopathy is usually a manifestation of reactive hyperplasia to local infections of mouth, teeth, jaws or oropharynx; less commonly of malignant metastases. Discrimination between benignly and malignantly enlarged lymph nodes is crucial for appropriate treatment. If the lymphadenopathy does not improve after treatment of a clinically apparent infective cause, then special investigations become necessary for definitive diagnosis and treatment planning.
The purpose of this article is to provide the dental practitioner with some guidelines for evaluating patients with lower facial and cervical lymphadenopathy.
Key words: lymphadenopathy; function and structure of lymph nodes; reactive hyperplasia.
INTRODUCTION
The principle components of the lymphatic system are the lymph nodes, the lymphatic vessels and the circulating immune cells which together have the primary function of protecting the host against infections.
Lymphadenopathy refers to any enlargement of lymph nodes. It may be a manifestation of various infectious, neoplastic or lipid-storage conditions, but in many cases, lymphadenopathy is non-specific, without any identifiable cause.1,2
Lymphadenopathy may be associated with the patients' main complaint or be an incidental finding,2 in which case the clinician must decide whether to regard the enlarged lymph nodes as merely the legacy of some infection in the past or as a current reaction to disease.2,3
The term regional lymphadenopathy refers to enlargement of lymph nodes within a single defined anatomical region (Figure 1) closely related to the site of the causative condition, whether it be infective or malignant. Generalised lymphadenopathy refers to the enlargement of lymph nodes at several non-contiguous anatomical regions related to a systemic condition. Generalised lymphadenopathy is usually associated with Epstein Barr virus (EBV)-induced infectious mononucleosis, an infectious mononucleosis-like condition caused by cytomegalovirus (CMV), HIV infection (Figure 2), immunological diseases or with haematological malignancies (leukaemia, lymphoma).2
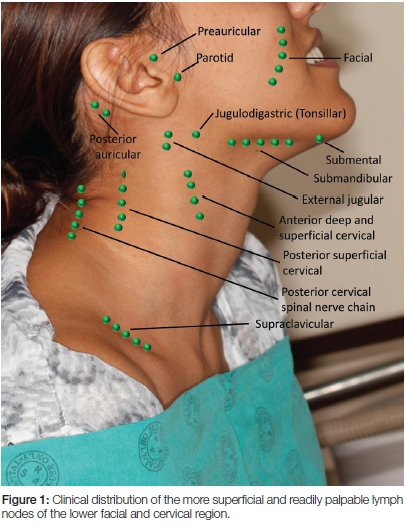

The most common causes of regional lower facial or cervical lymphadenopathy are upper respiratory infections, dental infections, periodontal infections, oral soft tissue infections and metastases from head, neck and mouth cancers.2,4,5
THE NORMAL LYMPH NODE
Lymph nodes are peripheral lymphoid organs linked to the blood vascular circulation by afferent and efferent lymphatics. These dense discrete accumulations of lymphoid tissue are ovoid, round or bean-shaped nodules that vary from 2 to 20mm in size. The major functions of lymph nodes are lymphopoiesis, filtration, and recognition and processing of antigens.6
The capsule, the fibrous trabeculae, and a reticulin network constitute the framework of the lymph node. The lymph node consists of three functionally and morphologically distinct zones: cortical, paracortical and medullary (Figure 3). Lymphoid cells comprise populations of B cells, T cells and plasma cells together with follicular dendritic cells and interspersed reticulum cells that have a role in antigen processing and presentation. The resident histiocytes, which are primarily phagocytic cells, remove microorganisms and other foreign particles from the lymph.6
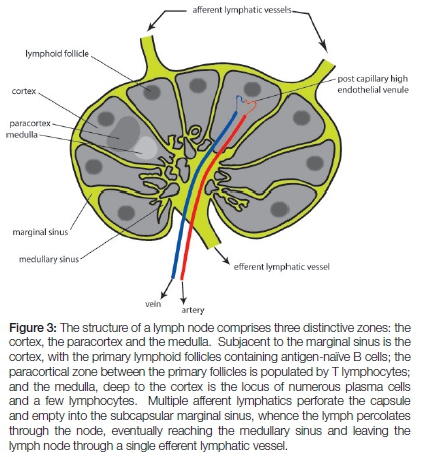
Physiologically, upon activation by antigens, the 'resting' lymphoid follicles enlarge and become dynamic cellular complexes comprising pale-staining germinal centres with large B lymphocytes surrounded by dark-staining mantle zones with small antigen-naïve B lymphocytes. The lymphoid follicles are engaged in humoral immunity, and undergo hyperplasia when humoral immune responses are generated. The densely cellular paracortical zone beneath the cortical zone extending between the lymphoid follicles, comprises mainly T lymphocytes and is the site of generation of cellular immunity.7
The medulla comprises cords of lymphocytes, plasma cell precursors and plasma cells and is the main site of antibody production. The role of plasma cells is to convey antibodies into the general circulation. The lymphatic sinuses are endothelium-lined passages between reticulin fibres in the cortical, paracortical and medullary zones. The phagocytes within the sinuses clear the lymph of foreign particles and play an important role in antigen processing.6
CLINICAL EVALUATION OF A DENTAL PATIENT WITH LOWER FACIAL AND CERVICAL LYMPHADENOPATHY
Medical history
Age, gender, occupation, exposure to pets, promiscuity of sexual behaviour, drug usage, dental and oral history, and symptoms such as sore throat, cough, fever, night sweats, and fatigue or weight loss may provide clues for determining possible causes of the lymphadenopathy. Lymphadenopathy in children and young adults is usually owing to infections, but with increasing age, the possibility of malignancy increases. Some drugs such as diphenylhydantoin and isoniazid are well known to cause lymphadenopathy.4
Physical examination
The size, consistency, mobility or fixation of the lymph node and whether or not it is tender to palpation are all important signs in determining the nature of the lymph node enlargement. In terms of size, abnormal lymph nodes smaller than 1cm in diameter are usually reactive and may persist after resolution of the cause owing to post-inflammatory fibrosis. On the other hand, lymph nodes bigger than 2cm in diameter are usually associated with malignant or infectious granulomatous diseases.
Lymph node tenderness is the result of rapid enlargement with stretching of the capsule, with hyperaesthesia of the associated sensory nerve endings caused by an acute or subacute inflammatory process.2
Abnormal lymph nodes can be described as being soft, firm, rubbery, hard, discrete or matted, mobile or fixed, tender or non-tender. Acute infection is characterised by regional lymphadenopathy in which the lymph nodes are discrete, tender, mobile and soft, but with chronicity of the infection, the lymph nodes become firmer and less tender.2,7 Acute submandibular or submental lymphadenitis is usually caused by dental, oral mucosal and maxillary sinus infections,2 while acute bilateral cervical lymphadenitis is most commonly caused by upper respiratory viral infection or by bacterial pharyngitis. Subacute and chronic cervical lymphadenitis are typically caused by mycobacterial infection and toxoplasmosis.4
In lymphadenopathy from metastatic cancer, the nodes are usually non-tender, hard and fixed to the surrounding tissues; but in the case of lymphoma, they are usually non-tender, large, discrete, rubbery, and mobile.2,5
LABORATORY STUDIES AND IMAGING TECHNIQUES
In the process of evaluation of lymphadenopathy, if the medical history and a clinical examination are not suggestive of a malignant origin, a causative infection must be sought and if found treated. Laboratory investigations are not usually required. Follow-up at about four weeks is advisable to determine if the lymphadenopathy has resolved.
If at this time the lymphadenopathy has not resolved, or has become worse, a complete blood count may provide information about possible leukaemia, lymphoma, EBV or CMV infection.1,2 Serological tests may show antibodies against specific viruses; and a culture of a throat swab may demonstrate persistent infection.1,2
Several imaging techniques including computed tomography (CT), magnetic resonance imaging (MRI), positron emission tomography (PET), ultrasound and colour Doppler ultrasonography can facilitate the differentiation of benign from malignant enlarged lymph nodes.2,8-11 If anything in the medical history, in the physical examination or in the imaging investigations is suggestive of malignancy, then biopsy of an accessible enlarged lymph node should be done.2 In general, lower facial and cervical lymphadenopathy should never be treated as being trivial.2
REACTIVE CHANGES AND MALIGNANT CELL INVASION OF LYMPH NODES
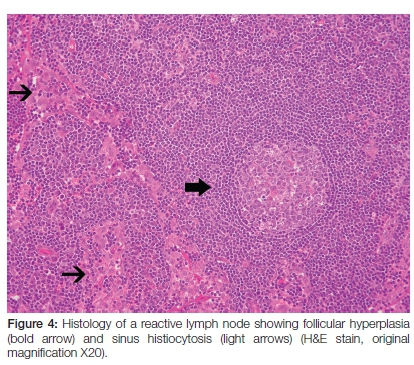
In response to infections, malignancy or other causes of tissue damage, lymph nodes in the drainage region will undergo reactive hyperplasia. Follicular hyperplasia (hyperplasia of the cortical follicles) with the development of enlarged B cell germinal centres (Figure 4) and the production of B lymphocytes will generate a humoral immune response; parafollicular (paracortical) hyperplasia will result in increased production of T lymphocytes, generating a cell-mediated immune response; and sinus hyperplasia (sinus histiocytosis) with the dilatation of the subcapsular and the medullary sinuses will result in increased numbers and upregulation of functional activity of macrophages and phagocytic sinus-lining cells. In addition, specific chronic granulomatous inflammatory processes in lymph nodes are observed in sarcoidosis, tuberculosis (Figure 5), syphilis and in Crohn's disease.12

In general, warm lymph nodes with erythematous overlying skin are suggestive of an acute pyogenic process, and fluctuance of a lymph node suggests that an abscess has formed within it. In long-standing chronic granulomatous diseases, notably tuberculosis, enlarged lymph nodes with abscess formation may not be warm at all, giving rise to the classical description of 'cold abscess'.
Whereas reactive lymph nodes are enlarged owing to the inflammatory changes of vasodilation, with B cell, T cell and plasma cell proliferation and oedema, lymph nodes affected by cancer metastases are enlarged chiefly because of proliferation of the malignant metastatic cells within the lymph node, and only to a lesser extent because of reactive hyperplasia and inflammation.13
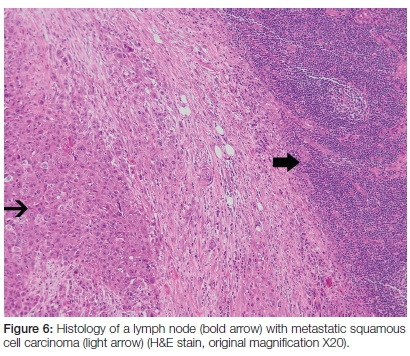
When metastatic malignant cells reach regional lymph nodes via afferent lymphatic vessels, they proliferate in the subcapsular sinus, and then infiltrate the medullary sinuses with progression to from solid malignant masses in the parenchyma of the lymph node (Figure 6).12
CONCLUSION
Lower facial or cervical lymphadenopathy is usually a manifestation of reactive hyperplasia to local infective processes such as dento-alveolar abscesses, acute periodontal diseases, oral soft tissue and salivary glandular infective conditions, systemic conditions, or to malignant metastasis.
Many cases of lower facial and cervical lymphadenopathy related to self-limiting oropharyngeal infections are self-limiting so that most cases resolve and do not per se necessitate any active treatment; but if the lymphadenopathy does not improve, special investigations as outlined above should be done.
Self-evidently, when lymphadenopathy is malignant in origin, radical treatment whether excisional, radio-or chemotherapeutic is mandatory, as may be decided by an oncologist.
Conflict of interest: None declared.
Acknowledgments: We are grateful to Dr R Ballyram for the illustrations of Figure 1 and Figure 3.
ACRONYMS
CMV: cytomegalovirus
CT: computed tomography
EBV: Epstein Barr virus
MRI: magnetic resonance imaging
PET: positron emission tomography
References
1. Bozlak S, Varkal MA, Yildiz I, Toprak S, Karaman S, Erol OB, et al. Cervical lymphadenopathies in children: A prospective clinical cohort study. Int J Pediatr Otorhinolaryngol 2016;82:81-7. [ Links ]
2. Henry PH, Longo DL. Enlargement of lymph nodes and spleen. In: Kasper DL, Hauser J, Jameson JL, Fauci AS, Longo DL, Loscalzo J, editors. Harrison's principles of internal medicine. United States of America: Mc-Graw Hill; 2015. 407-13. [ Links ]
3. Niedzielska G, Kotowski M, Niedzielski A, Dybiec E, Wieczorek P. Cervical lymphadenopathy in children--incidence and diagnostic management. Int J Pediatr Otorhinolaryngol 2007;71:51-6. [ Links ]
4. Leung AK, Robson WL. Childhood cervical lymphadenopathy. J Pediatr Health Care 2004;18:3-7. [ Links ]
5. Scully C. Haematology. In: Scully C, editor. Scully's medical problems in dentistry. Seventh Edition ed. London: Churchill Livingstone Elsevier; 2014. 212-22. [ Links ]
6. Ioachim HL. Lymph node pathology. Philadelphia: Lippincott 2008. [ Links ]
7. Aster JC. Diseases of white blood cells, lymph nodes, spleen and thymus. In: Gruliow R, editor. Robbins and Cotran Pathologic basis of disease: Elsevier Saunders; 2005. 661-3. [ Links ]
8. Tsuji T, Satoh K, Nakano H, Nishide Y, Uemura Y, Tanaka S, et al. Predictors of the necessity for lymph node biopsy of cervical lymphadenopathy. J Craniomaxillofac Surg 2015;43:2200-4. [ Links ]
9. Som PM. Detection of metastasis in cervical lymph nodes: CT and MR criteria and differential diagnosis. AJR Am J Roentgenol 1992;158:961-9. [ Links ]
10. Na DG, Lim HK, Byun HS, Kim HD, Ko YH, Baek JH. Differential diagnosis of cervical lymphadenopathy: usefulness of color Doppler sonography. AJR Am J Roentgenol 1997;168:1311-6. [ Links ]
11. Luciani A, Itti E, Rahmouni A, Meignan M, Clement O. Lymph node imaging: basic principles. Eur J Radiol 2006;58:338-44. [ Links ]
12. Stevens A, Lowe JS, Young B. Lymphoid and haemopoietic systems. In: Horne T, editor. Wheater's basic histopathology: Churchill Livingston; 2002. 185-97. [ Links ]
13. Choi MY, Lee JW, Jang KJ. Distinction between benign and malignant causes of cervical, axillary, and inguinal lymphadenopathy: value of Doppler spectral waveform analysis. AJR Am J Roentgenol 1995;165:981-4. [ Links ]
 Correspondence:
Correspondence:
Liviu Feller
Head: Department of Periodontology and Oral Medicine,
Sefako Makgatho Health Sciences University,
Pretoria, South Africa, 0204.
Tel: 012 521 4834;
Fax: 012 521 4833.
E-mail: liviu.feller@smu.ac.za













