Serviços Personalizados
Artigo
Indicadores
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares em Google
Similares em Google
Compartilhar
South African Dental Journal
versão On-line ISSN 0375-1562
versão impressa ISSN 0011-8516
S. Afr. dent. j. vol.71 no.10 Johannesburg Nov. 2016
COMMUNICATION
Immune-mediated response of bone in osteomyelitis - fundamental concepts
HD MiniggioI; EJ RaubenheimerII
IBDS, MScMed(Bioethics and Health Law). Unit 5: Oral Biology, Faculty of Health Sciences- Sefako Makgatho Health Sciences University, Pretoria, South Africa
IIPhD, DSc, Unit 2: Oral Pathology, Faculty of Health Sciences- Sefako Makgatho Health Sciences University, Pretoria, South Africa
ABSTRACT
Advancement of knowledge on the role of the immune system in bone metabolism has uncovered a dynamic interdisciplinary research field labelled "osteoimmunology". The immune system provides stem cells for bone remodelling and elaborates cytokines under both physiological- and pathological circumstances which map the local response of bone cells and alter the phenotypic expression of bone. This manuscript provides an overview of the interaction between the immune system and bone in the different stages of osteomyelitis and correlates the inductive patterns with the radiologic appearances.
Keywords: osteoimmunology, immune regulatory mediators, bone remodelling, osteomyelitis
INTRODUCTION
Bone formation is a complex and precisely regulated process initiated with the differentiation of mesenchymal cells into osteoblasts that are responsible for secretion of the organic bone matrix and the mineralization thereof. Upon completion of bone formation, a continuous process of bone remodelling is responsible for preserving bone mass, repair of fractures and maintaining calcium and phosphorous homeostasis. The seemingly inert skeleton displays an impressive restructuring capacity, with approximately 10% of the mass of the adult skeleton being replaced every year.1 In the jaws, the flexibility of the remodelling process renders alveolar bone highly adaptable and make possible several clinical interventions such as orthodontic tooth movement, the integration of dental implants and the replacement of resorbed bone. Remodelling of mature bone is initiated by osteoclast-mediated resorption coupled with osteoblast-mediated bone formation.2 The successive sequence of bone resorption and bone formation and the observation that under physiological circumstances the bone mass remains constant, is proof of a delicate regulatory balance between these two opposing processes.2 This balance is mediated in a supportive metabolic environment by a delicately controlled release of chemical mediators, also known as cytokines, by the bone cells involved in the remodelling process (Figure 1).
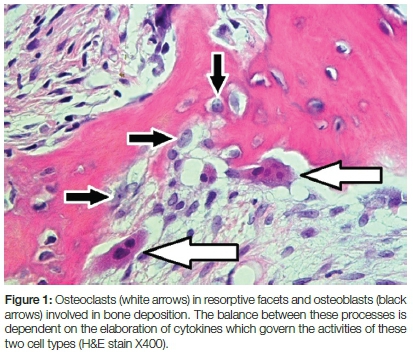
The importance of the immune system in bone metabolism is illustrated by the rapidly expanding interdisciplinary field of osteoimmunology. During physiological bone remodelling the immune system not only provides stem cells, but also elaborate cytokines that regulate the activities of osteoclasts and osteoblasts through binding to specific receptors on the cell surfaces.3 However, the release of inflammatory cytokines and an influx of immune cells during the course of osteomyelitis overwhelms the physiological cell signalling patterns and results in the induction of bone changes. These changes manifest on radiographs and signify the different clinical patterns of osteomyelitis. This manuscript aims to provide an overview of the interaction between the immune system and bone during the course of osteomyelitis and provides insight into the bone changes seen on radiographs in the different patterns of the disease.
BONE REACTION IN ACUTE OSTEOMYELITIS
Acute osteomyelitis is characterised radiographically as an area of poorly demarcated bone loss at the site of inflammation. The resorptive process is initiated by the attraction of neutrophils and monocytes, the mainstay of the innate immune response, to the site of inflammation. Osteoclasts which are responsible for bone resorption differentiate from a pool of predestined osteoclast precursors which circulate in the blood as monocytes and are attracted to bone by a complex interaction of cytokines, the details of which fall outside the scope of this paper.11
Osteoclasts are retained within bone by a chemokine known as stromal-derived factor-1 (SDF-1).4 Depending on the cytokines elaborated in bone, monocytes may also differentiate into macrophages (the cells responsible for phagocytosis of necrotic bacteria and tissue debris at the site of inflammation).5 The common ancestry of osteoclasts and macrophages illustrates the close relationship between the immune system and bone.
During normal bone remodelling, macrophage-colony-stimulating factor (M-CSF) promotes the expression of receptor activator of nuclear factor κ β (RANK) receptors on dedicated monocytes6 which are important receptor sites for the activation of the pre-osteoclasts. Osteoblasts release RANKL (RANK ligand) which activates osteoclasts through binding to the RANK receptors on their cell surfaces. The action of RANKL is antagonised by osteoprotegerin (OPG), a cytokine produced by osteoblasts which acts as a decoy receptor for RANKL.7-9 This finely tuned control of bone resorption by osteoblasts is important for calcium and phosphate homeostasis whilst maintaining the integrity of the skeleton.
The attraction of leukocytes and macrophages to a site of osteomyelitis and subsequent elaboration of several osteoclastogenic cytokines by the inflammatory cells, amongst others RANKL produced by activated macrophages, several interleukins (IL's) released by leukocytes10 and tumour necrosis factor α (TNF α)11 have a profound stimulatory influence on osteoclasts, resulting in accelerated bone resorption. Microscopically this catabolic shift manifests as an increase in the number of active osteoclasts which are large, multinucleated cells that attach to the bone surface via an integrin vitronectin receptor, αVβ3.12 The active osteoclasts display specialised ruffled cytoplasmic borders which enlarge their contact area with bone. H+ -and Cl- ions are secreted across the ruffled borders in the contact zones with bone and the hydrochloric acid formed creates an acidic environment which is responsible for demineralization of the inorganic fraction of bone. Proteolytic enzymes such as tartrate resistant acid phosphatase (TRAP) and cathepsin K are released which degrade the organic matrix.13 The result is rapid bone resorption which manifests as a poorly demarcated radiolucency (Figures 2a and 2b).
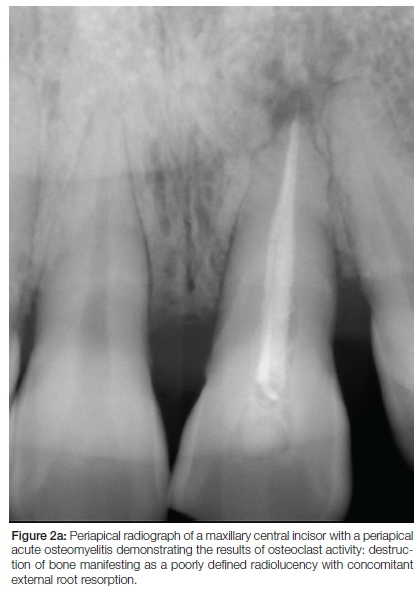

BONE REACTION IN CHRONIC OSTEOMYELITIS
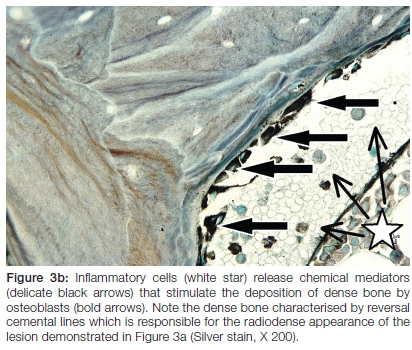
After neutralization of most of the antigens by the innate immune response and the short life span of neutrophils, the nature of the inflammatory reaction in osteomyelitis changes and cells of the adaptive immune response (lymphocytes and plasma cells) appear. Osteoclasts are active for approximately three weeks14 and thereafter progressively undergo apoptosis and become less abundant. The ingrowth of granulation tissue rich in blood vessels, which is mediated by the release VEGF (vascular endothelial growth factor),15 provides a source of undifferentiated mesenchymal cells which are predestined to differentiate into osteoblasts.16 Several transcription factors together with bone morphogenic proteins (BMP) belonging to the transforming growth factor beta (TGFβ) superfamily are essential in the differentiation of mesenchymal cells to the osteoblast lineage.17 Of particular interest in the context of bone formation stimulated by immune cells is the elaboration of prostaglandin E2 which binds to receptors on the cell surfaces of osteoblasts and stimulate their activity.18 The changes in the cell composition at a site of persistent inflammation and the subsequent changes in the cytokines released contribute to the creation of an environment favourable for bone formation. It therefore comes as no surprise that the sites of chronic osteomyelitis in the jaw bone manifest as radiopacities (Figures 3a and 3b). In children, the elaboration of bone inductive cytokines at a site of chronic inflammation and in the presence of anabolic hormones such as human growth hormone (HGH) and insulin-like-growth-factor-1 (IGF-1)19 stimulates a periosteal bone reaction (Figure 4). This reactive process manifests with an "onion-skin appearance" radiologically and is designated as chronic osteitis with proliferative periostitis.


CONCLUSION
Mapping of the cytokines released during the course of osteomyelitis provides an explanation for the reaction of bone and the subsequent radiologic changes of the disease. The characterization of cell receptors governing the inflammatory induced bone changes provide lucrative commercial opportunities for the manufacturing of patented drugs and auto antibodies which can either limit bone resorption or stimulate bone formation, thereby facilitating an enhanced clinical outcome for patients with osteomyelitis. Injectable biodegradable microspheres coated by osteoinductive cytokines have already been shown to decrease post infection healing time of bone.20,21 Further advances in this rapidly developing field of manipulating bone health is certain to impact in the near future on the management of osteomyelitis of the jaw bones.
References
1. Murthy MB. Osteoimmunology- Unleasing the concepts. J Indian Soc Periodontol 2011; 15:190-8. [ Links ]
2. Corral DA, Amling M, Priemel M, et al. Dissociation between bone resorption and bone formation in osteopenic transgenic mice. Proc Natl Acad Sci USA. 1998; 95 (23):12835-13840. [ Links ]
3. Lorenzo J, Horowitz M, Choi Y. Osteoimmunology: interactions of the bone and immune system. Endocr Rev, 2008: 29(4): 403-40. [ Links ]
4. Boyce BF. Advances in the regulation of osteoclasts and osteoclast functions. J Dent Res 2013: 92(10): 860-7. [ Links ]
5. Tetti A, Rucci N. The unexpected links between bone and the immune system. Medicograph 2010 (32)4:341-8. [ Links ]
6. Boyce BF, Zuscik MJ, Xing L. Biology of bone and cartilage. In: Genetics of Bone Biology and Skeletal Disease. London, UK: Elsevier, pp3-24. [ Links ]
7. Abu-Amer Y: NFKB signalling and bone resorption. Osteoporos Int 2013;24: DOI:10.1007/s00198-013-2313-x. [ Links ]
8. Glass DA, Bialek P, Ahn JD. Cananonical Wnt signalling in differentiated osteoblasts controls osteoclast differentiation. Dev Cell 2005;8:751-64. [ Links ]
9. Lacey DL, Timms E, Tan HL. Osteoprotegerin ligand is a cytokine that regulates osteoclast differentiation and activation. Cell 1998;93:165-76. [ Links ]
10. Walsh MC, Kim N, Kadono Y. Osteoimmunology: interplay between the immune system and bone metabolism Ann Rev Immunol 2006;24:33-63. [ Links ]
11. Jurisic V, Colic S, Jurisic M. The inflammatory radicular cysts have a higher concentration of TNF alpha in comparison to odontogenic keratocysts (odontogenic tumour). Acta Medica (Hradec Kralove) 2007;50:233-8. [ Links ]
12. Boyce BF. Advances in the regulation of osteoclasts and osteoclast functions. J Dent Res 2013; 92(10): 860-7. [ Links ]
13. Hayman AR. Tartrate-resistant acid phosphatase (TRAP) and the osteoclast/immune cell dichotomy. Autoimmun 2008;41:218-23. [ Links ]
14. Sims NA, Martin TJ. Coupling the activities of bone formation and resorption: a multitude of signals within the basic multicellular unit. BoneKey Rep 2014; doi:10.1038/bonekey.2013.215. [ Links ]
15. Street J, Bao M, deGusman L. Vascular endothelial growth factor stimulated bone repair by promoting angiogenesis and bone turnover. Proc Natl Acad Sci USA 2002;99:9656-9661. [ Links ]
16. Sacchetti B, Funari A, Michienzi S. Self-renewing osteoprogenitors in bone marrow sinusoids can organize a hematopoietic microenvironment. Cell 2007;131:324-6. [ Links ]
17. Komori T. Regulation of osteoblast differentiation by transforming factors. J Cell Biochem 2006;99:1233-9. [ Links ]
18. Graham S, Gamie Z, Polyzois I. Prostaglandin EP2 and EP4 receptor agonists in bone formation and bone healing: In vivo and in vitro evidence. Expert Opin Investig Drugs 2009;18:746-66. [ Links ]
19. Olney RC. Regulation of bone mass by growth hormone. Med Pediatr Oncol 2003;41:228-34. [ Links ]
20. Jennisen HP. Accelerated and improved osseointegration of implants biocoated with bone morphogenetic protein 2 (BMP-2). Ann NY Acad Sci 2002;961:139-42. [ Links ]
21. Tiffany NV, Kasper FK, Mikos AG. Strategies for controlled delivery of growth factors and cells for bone regeneration. Adv Drug Deliv Rev 2012;64:1292-1309. [ Links ]
 Correspondence:
Correspondence:
Hilde D Miniggio
P.O. Medunsa 0204, Pretoria
Tel: 012 521 4882
Fax: 012 521 4274
Cell: 072 869 4045
E-mail: hilde.hendrik@smu.ac.za













