Serviços Personalizados
Artigo
Indicadores
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares em Google
Similares em Google
Compartilhar
South African Dental Journal
versão On-line ISSN 0375-1562
versão impressa ISSN 0011-8516
S. Afr. dent. j. vol.71 no.10 Johannesburg Nov. 2016
RESEARCH
The use of temporary skeletal anchorage devices amongst South African orthodontists
TF MothobelaI; MPS SethusaII; MI KhanIII
IBDT, BDS (Medunsa), M Dent Orthodontics (Sefako Makgatho Health Sciences University). Registrar 2015 (Sefako Makgatho Health Sciences University)
IIB (Diag) Rad and BDS (Medunsa), PDD (Stellenbosch), M Dent Orthodontics (University of Limpopo), P G Dip (UCT), Head of Department of Orthodontics. Sefako Makgatho Health Sciences University
IIIBDS cum laude (Medunsa), M Dent Orthodontics (University of Limpopo). Senior part-time specialist in the Department of Orthodontics. Sefako Makgatho Health Sciences University
SUMMARY
BACKGROUND: Temporary Skeletal Anchorage Devices (TSADs) are small titanium screws that are inserted through the gingival or palatal mucosa into supporting bone to form an independent rigid anchor unit or may be tied to adjacent teeth to enhance their anchorage capability. On completion of orthodontic treatment the orthodontist is easily able to unscrew and remove the screws.
OBJECTIVE: To conduct a survey on the clinical use of TSADs amongst South African orthodontists.
MATERIALS AND METHOD: The method consisted of a structured survey questionnaire which was sent to 110 South African orthodontists registered on the South African Society of Orthodontists database in 2013.
RESULTS: Forty six orthodontists completed the survey, a response rate of 41.81%. Of these respondents, 63.04% used TSADs, and of those, 58.62% placed TSADs themselves while the remainder referred to maxillo-facial surgeons, and to a lesser extent, to periodontists, for placement. The majority (72.41%) loaded TSADs immediately. TSADs were used mostly to provide anchorage when teeth were moved mesially (52%) or distally along the arch.
CONCLUSIONS: South African orthodontists have adopted a cautious approach to the use of TSADs. Training in the placement and the clinical application of TSADs should be incorporated in the curriculae of postgraduate orthodontics.
INTRODUCTION AND LITERATURE REVIEW
The term "orthodontic anchorage" was defined by Ottofy as "the base against which orthodontic force or reaction of orthodontic force is applied".1 This definition was later expanded upon by Daskalogiannakis2 who explained it more simply as "resistance to unwanted tooth movement". In essence, anchorage means the prevention of undesired forward movement of posterior teeth, which are often used as "anchors" when crowded or proclined anterior teeth are being retracted into space created by premolar extraction.3 Every effort should be made during retraction to prevent the anchor teeth from moving forward.3-5
Orthodontists have traditionally used extra-oral appliances such as headgears and face masks to control anchorage. Headgear obtains anchorage from the back of the head and face masks from the chin and forehead. In more recent times these appliances have lost popularity, with many patients regarding the devices as unappealing to wear, and consequently are not compliant, leading to poor treatment outcomes.5,6
In an effort to overcome these problems, tooth anchorage devices which are not reliant on patient cooperation were designed, such as the Nance holding arch, the transpalatal arch (TPA) and the lingual arch.7-9 Unfortunately, untoward mesial movement of posterior teeth anchored with these appliances still occurs.3,8
Recently, temporary anchorage devices (TADs) have been introduced to clinical orthodontics. These are small screws inserted into bone for the purpose of enhancing orthodontic anchorage and are removed following completion of treatment.10-14 The first clinical case report on the successful use of an intra-osseous mini-screw was published in 1983.4 In that case a patient with a deep impinging overbite was treated using a vitallium bone screw inserted below the nasal spine. An elastic chain was then used to intrude the maxillary incisors. It was only in the early 21st century, however, after the introduction of the more biocompatible titanium screws, that these devices became common.10-13 Approval by the FDA for their clinical use was granted in 2003.15 Since then various terminologies have been used to describe a screw inserted into bone and used for orthodontic anchorage, including: mini-screw, micro-screw, mini-implant, micro-implant, pin-plant, ortho-implant and temporary anchorage device (TAD). A panel of orthodontists meeting at the 2004 conference of the American Association of Orthodontists16 was mandated to resolve the confusion. It was suggested that the terms micro and screw be avoided as the former implies a metric measurement of 1016 requiring for visualisation the aid of a microscope, while the latter may have a negative connotation. The terms miniscrews and TAD were adopted, although the term TAD is actually applicable to other appliances such as the headgear and mandibular holding arch. The term Temporary Skeletal Anchorage Device (TSAD) is today preferred with the pronunciation remaining "tad" with a silent "s". They are easy to place, even by orthodontists with the patient in the dental chair. Minimal local or topical anaesthesia is required and the tad can be loaded immediately.17-19
Mini-plates were introduced at about the same time that miniscrews were taken into use.18, 20-23 Mini-plates are Y, T or L-shaped flat bars of titanium plate surgically inserted and fixated to bone using two to three monocortical screws. The technique has a high success rate. It is claimed that the plates provide reliable stability and can withstand heavy forces. They are therefore reserved for cases where heavy forces such as those used for retraction of teeth en-masse, for distal movement of molars and for skeletal correction are applied. The disadvantages associated with these devices are added cost of the TSADs and their placement as well as the need for a second surgical procedure for the removal of plates and screws on completion of treatment.
Orthodontists have since introduced several uses for TSADs including: retraction of anterior teeth, retraction of whole dentition, distal repositioning of molars, protraction of molars or the whole dentition, orthopaedic correction of maxillary deficient cases, intrusion of teeth and arch expansion. Other minor uses include: improved tooth anchorage in periodontally compromised individuals, uprighting and dis-impacting molars as well as correcting a canted occlusal plane.24-34
The aim of this study was to report on the uses of TSADs by South African orthodontists and to compare the findings with those of similar surveys elsewhere. Information obtained from such a survey could be useful in informing the training of orthodontists.
MATERIALS AND METHODS
A structured self-administered questionnaire, used previously in a survey in the USA,35 was modified and directed at 110 South African orthodontists registered on the South African Society of Orthodontists database in 2013. Questions were aimed at obtaining information regarding how frequently TADs were used, and sought reaction on how orthodontists viewed the experience. Orthodontists attending the annual SASO Congress in 2013 were invited to complete the questionnaire. A follow-up web-based survey was sent to those who had not attended the Congress and to those who had attended but had not returned their questionnaires.
Descriptive statistical analyses were performed using SAS® (SAS Institute Inc, Carey, NC), Release 9.3, run under Microsoft® Windows® from a personal computer.
RESULTS
A response rate of 41.8% (46 out of 110) was achieved in this study.
The responses to the questions posed in the questionnaire are as follows:
I. Orthodontists using TSADs in their practices
i) How long have you been using TSADs?
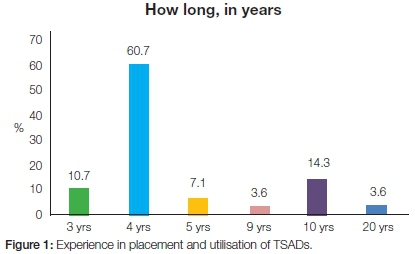
Twenty eight (60.9%) of the responding orthodontists had been using TSADs in their clinical practices for periods varying from three to twenty years (see Figure 1), the majority ( 60.7%) reporting experience in their use for at least four years (Figure 1).
ii) Who places TSADs and to whom do you refer to if you don't place them yourself?
The majority of orthodontists who use TSADs (57.2%) place the screws themselves (Table 1). Of the remaining orthodontists who referred their patients for placement, most (28.6%) referred to maxillofacial and oral surgeons, and 7.1% to periodontists.

iii) When do you load TSADs?
Seventy-five percent of orthodontists responded that they loaded TSADs immediately after placement, while 21.4% impose a waiting period before loading (Table 2).

iv) What do you use TSADs for?
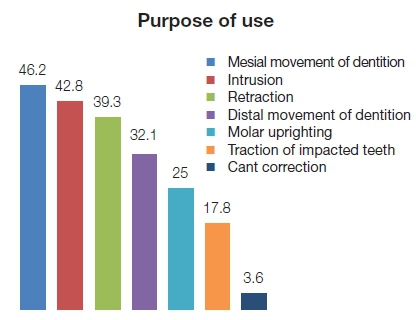
An analysis of the responses of the participating orthodontists revealed that TSADs were most commonly used for anchorage when the dentition was being moved mesially (46.2%), for intrusion (42.8%) and for retraction (39.3%). Applications reported less frequently included: distal movement of dentition (32.1%), molar uprighting (25%) and traction of impacted teeth (17.8%). They were used least for correction of an occlusal cant (3.6%) (Figure 2).
Reports in the literature indicate that 54% to 57% of orthodontists place TSADs themselves.39
v) How many TSADs do you place per month?
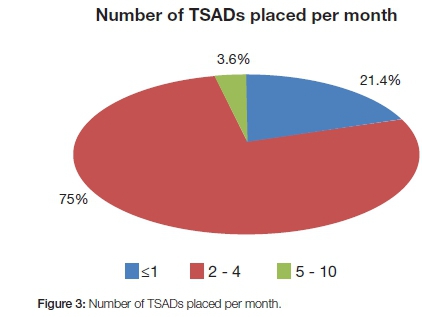
In this study a large number of orthodontists (75%) placed an average of two to four TSADs per month. Fewer than one was placed per month by 21.4% of the sample while 3.6% placed an average of between five and 10 TSADs per month (Figure 3).
vi) What complications have you experienced in the use of TSADs?
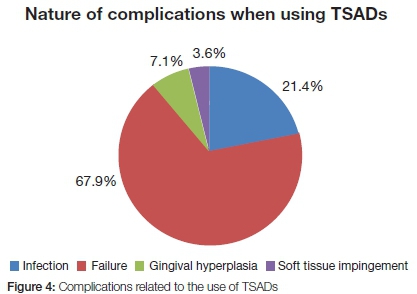
The most commonly reported complication experienced with the use of TSADs was failure (67.9%) (Figure 4).
vii) How many failures do you experience per month? (Failure rate)
No failures were reported by 32.1% of orthodontists in their use of TSADs, while 50% had experienced the failure of one to five TSADs during treatment (Figure 5).

viii) In your experience, would you say that these devices have added value to your clinical practice in terms of clinical/treatment results?
Most respondents who used TSADs (50%) were satisfied, believing that the devices added value to their clinical practice in terms of clinical/treatment results. Only two respondents (7.1%) reported not being completely satisfied with the application of TSADs.
II Orthodontists not using TSADs in their practices
i) Why are you not using TSADs?
Among the 18 orthodontists who were not making use of TSADs in their practices, the most commonly cited reason was that they were not skilled in placing the screws (22.2%). Other reasons provided were that orthodontists were apprehensive of complications that might arise (22.2%), the high cost of TSADs, and patients' inability to accept TSADs (Table 3).
ii) What alternative methods of anchorage are you using?
When questioned about the method/s of anchorage that they were using other than TSADs, orthodontists mentioned the following: headgear, transpalatal arch, Nance holding arch, figure eight ligatures, wire stops, pushing springs, bonding second molar teeth, elastics, face mask and the Begg technique.
iii) If lack of skill is your reason for not using TSADs, do you believe a hands-on course would benefit you?
Of the nine orthodontists who cited lack of skill as their reason for not using TSADs, five (55.5%) reported that they believed that a hands-on course would benefit them, and that they would use TADs if another professional was to place them on their behalf. Four (44.4%) of the nine answered "maybe" to the two questions.
DISCUSSION
This study sought to establish the use of TSADS amongst South African orthodontists through the use of a validated, structured self-administered questionnaire.35 Questions were separated into two categories, namely for orthodontists using TSADS to find out how frequent and for what purpose was their use and a second category for those not using the technique, to explore their reasons and to discover what alternative form of anchorage they are using.
The response rate from participants was modest and rather lower than that achieved in a USA36 study where the reported response rate was 82%. The 2008 survey of AAO members37 and the Swiss study,38 however had much lower response rates at 6% and 24.4% respectively. (Surveys using questionnaires generally have low response rates.)
The highest percentage of orthodontists using TSADs was in the USA,35 reported as 91%, closely followed by the Swiss at 80%.38 In this South African study, the percentage of orthodontists using TSADs was lower (60.9%). This might be due to delayed arrival of new technology and innovation and a longer lag period in becoming established. Also, when technology finally arrives, it comes at a much higher and possibly prohibitive cost.
The experience levels of orthodontists using TSADs in this study were comparable to those of orthodontists in the USA study in that none of the clinicians reported having used TSADs for longer than 10 years. The majority of respondents (89.2%) had been using the devices for only the past five years or less.36 This finding was to be expected since the technique was still relatively new at the time when this study was conducted.
The number of SA orthodontists who place TSADS on their own is comparable to the figures reported in the literature (54% to 57%) and so is the pattern of referral for placement, with the majority of orthodontists involving maxillofacial surgeons and very few referring to periodontists.37,39 The reasons for these preferences are not clear. Even though there is agreement that placement of TSADs is relatively easy,40 some orthodontists are still not comfortable to manage insertion of the screw, an indication that placement and clinical use of these devices should be taught at training centres.
A high number of orthodontists are comfortable in loading TSADS immediately.33,36,37 Other researchers agree that immediate loading is not only possible but may also positively affect the osseous density around the screw.41
South African orthodontists use TSADs mostly for mesial movement of the dentition and the least frequent application is for correction of canted occlusal planes. The findings are similar to what has been found elsewhere.35,36
The frequency in the use of TSADS could of course be linked to the prevalence of the specific malocclusion traits with cases requiring mesial movement of the dentition being more common than those requiring correction of the canted occlusal plane.29,33,35-37
A high number of orthodontists (75) using TSADS place an average of four per month. This means that they are fairly comfortable with the clinical application of these devices. In the USA study36 only six of 46 clinicians reported having placed more than 20 TSADs in their clinical lives. TSADs were placed in only 6% of the patients reported in the study by Shirck et al,35 whereas Keim et al42 reported an average of only three patients per orthodontist. These findings suggest that orthodontists are very careful and selective in their use of TSADs.
Failure was the commonest complication when using TSADs, although the rate is low and comparable to that found in the literature.43,44 Most studies have shown failure rates of around 10%.43
Most respondents in this study agree that the use of these devices has added value to their practices and only two reported that they are not completely satisfied with TSADs. This indicates how clinically valuable the devices are and perhaps also emphasises the need to offer registrars instruction in their application . It is evident from the literature that the use of TSADs does enhance orthodontic treatment results. In this study, a greater proportion of SA orthodontists (85.7%) was found to consider that TSADs had added value to their treatment outcomes than was shown amongst USA orthodontists (78.7%).37
Most orthodontists not using TSADs seem to still rely on conventional methods of anchorage control. They cite lack of skills to place and use TSADs and concerns about possible complications in their use as reasons for not practising the technique. Perhaps these are normal reactions to new technology. Venkatesh and Parveen included lack of training by 67% of their respondents, fear of risk factors (54%), and patients' refusal to accept TSADs (29%) as factors hampering the acceptance of TSADs in most practices.33 Most orthodontists not using TSADS confirmed that they would consider using them if they can receive adequate training.
Another factor in South Africa is the high cost of new technology as most of these items are imported at great expense.
LIMITATIONS OF THE STUDY
As a result of the low response rate from a relatively small population, sample size was the greatest limitation of this study.
CONCLUSIONS
The following conclusions can be drawn from the findings, while recognising the limitations of the study:
The majority of South African orthodontists use TSADs in their clinical practices but are selective and cautious in their application. Lack of training and a lack of confidence, fear of performing surgical procedures and the high costs involved contribute to a reluctance for greater usage. We recommend that placement techniques and the clinical use of these devices should be incorporated in the orthodontic postgraduate training programme.
Conflict of interest: None declared.
ACRONYMS
TSADs: Temporary Skeletal Anchorage Devices
TPA: Transpalatal Arch
References
1. Ottofy L. Chicago: Standard Dental Dictionary, Laird and Lee, Inc; 1923. [ Links ]
2. Daskalogiannakis J. Glossary of Orthodontic Terms, Leipzig: Quintessence Publishing Co; 2000. [ Links ]
3. Cope JB. Temporary anchorage devices in orthodontics: A paradigm shift. Sem Orthod. 2005; 11: 3-9. [ Links ]
4. Creekmore TD, Eklund MK. The possibility of skeletal anchorage. J Clin Orthod. 1983; 17: 266-9. [ Links ]
5. Brandão M, Pinho HS, Uriasb D. Clinical and quantitative assessment of headgear compliance: A pilot study. Am J Orthod and Dentofac Orthop. 2006; 129: 239-44. [ Links ]
6. Bos A, Kleverlaan CJ, Hoogstraten J, Andersen B, Kuitert R. Comparing subjective and objective measures of headgear compliance. Am J Orthod and Dentofac Orthop. 2007; 132: 801-5. [ Links ]
7. Nance HN. The limitations of orthodontic treatment. I and II. Am J Orthod. 1947; 33: 253-301. [ Links ]
8. Zablockia HL, McNamara JA, Franchi L, Baccetti T. Effect of the transpalatal arch during extraction treatment. Am J Orthod and Dentofac Orthop. 2008; 133: 852-60. [ Links ]
9. Wein SL. The lingual arch as a source of anchorage in Class II treatment. Am J Orthod and Dentofac Orthop. 1959; 45: 32-49. [ Links ]
10. Graber TM. Have we finally found the Holy Grail of Orthodontics? World J Orthod. 2002;3:107. [ Links ]
11. Kanomi R. Mini-implants for orthodontic anchorage. J Clin Orthod. 1997; 31: 763-7. [ Links ]
12. Freudenthaler JW. Bantleon HP. Haas R. Biocortical titanium screws for critical anchorage in the mandible: a preliminary report on clinical applications. Clin Oral Implants Res. 2001; 12: 358-63. [ Links ]
13. Woo SS, Jeong ST, Huh YS, Hwang KG. A clinical study of the skeletal anchorage system using mini screws. J Korean Assoc Oral Maxillofac Surg. 2003; 29:102-7. [ Links ]
14. Mah J, Bergstrand F, Graham JW. Temporary anchorage devices: a status report. J Clin Orthod. 2005; 39: 132-6. [ Links ]
16. Choo H, Kim SH, Huang JC. TAD, a misnomer? Am J Orthod and Dentofac Orthop. 2009; 136: 145-6. [ Links ]
17. Miyawaki S, Koyama I, Inoue M, Mishima K, Sugawara T, Yamamoto TT. Factors associated with the stability of titanium screws placed in the posterior region for orthodontic anchorage. Am J Orthod and Dentofac Orthop. 2003; 124: 373-8. [ Links ]
18. Chen YJ, Chang HH, Lin HY, Lai EH, Hung HC, Yao CC. Stability of miniplates and miniscrews used for orthodontic anchorage: experience with 492 temporary anchorage devices. Clin Oral Implants Res. 2008; 19: 1188-96. [ Links ]
19. Chen Y, Kyung HM, Zhao WT, Yu WJ. Critical factors for the success of orthodontic mini-implants: a systematic review. Am J Orthod and Dentofac Orthop. 2009; 135: 284-91. [ Links ]
20. Sugawara J, Nishimura M. Minibone plates: the skeletal anchorage system. Sem Orthod. 2005; 11: 47-56. [ Links ]
21. Sugawara J. Temporary skeletal anchorage devices: The case for miniplates. Am J Orthod and Dentofac Orthop. 2014; 145: 558-65. [ Links ]
22. De Clerck HJ, Geerinckx V, Siciliano SJ. The zygoma anchorage system. J Clin Orthod. 2002; 36: 455-9. [ Links ]
23. Cornelis M, De Clerck H J. Biomechanics of skeletal anchorage. Part 1. Class II extraction treatment. J Clin Orthod. 2006; 40: 261-9. [ Links ]
24. Giancotti A, Greco M, Docimo R., Arcuri C. Extraction treatment using palatal implant for anchorage. Aust Orthod J. 2003; 19: 87-90. [ Links ]
25. Ohnishi H, Yagi T, Yasuda Y, Takada K. Mini-implants for orthodontic anchorage in a deep overbite case. Angle Orthod. 2005; 75: 444-52. [ Links ]
26. Park H, Lee S, Kwon O. Group distal movement of teeth using microscrew implant anchorage. Angle Orthod 2005; 75: 602-8. [ Links ]
27. Lee KJ, Park,YC, Hwang WS, Seong EH. Uprighting mandibular second molars with direct miniscrew anchorage. J Clin Orthod. 2007; 10: 627-35. [ Links ]
28. Papadopoulos MA, Tarawneh F. The use of miniscrew implants for temporary skeletal anchorage in orthodontics: A comprehensive review. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2007; 103: e6-e15. [ Links ]
29. Takano-Yamamoto T, Kuroda S. Titanium screw anchorage for correction of canted occlusal plane in patients with facial asymmetry. Am J Orthod and Dentofac Orthop. 2007; 132: 237-42. [ Links ]
30. Yamada K, Kuroda S, Deguchi T, Takano-Tamamoto T, Yamashiro T. Distal movement of maxillary molars using miniscrew anchorage in the buccal inter-radicular region. Angle Orthod. 2009; 79:78-84. [ Links ]
31. Giancotti A, Greco M, Mampieri G, Arcuri C. Palatal-implant anchorage in an adult Class II patient. J Clin Orthod. 2011; 45:627-34. [ Links ]
32. Lee M, Shuman J. Maxillary molar intrusion with a single miniscrew and a transpalatal arch. J Clin Orthod. 2012; 46:48-51. [ Links ]
33. Venkatesh, M.K.G., Parveen, J.M.F. Current trends in miniscrew utilisation among Indian orthodontists. J Orthod Sci. 2012; 1:46-50. [ Links ]
34. Nienkemper M, Willmes B, Lubberink G, Ludwig B, Drescher D. Extrusion of impacted teeth using mini-implant mechanics. J Clin Orthod. 2012; 46:150-5. [ Links ]
35. Shirck JM, Firestone AR, Beck FM, Vig KW, Huja SS. Temporary anchorage device utilization: comparison of usage in orthodontic programmes and private practice. Orthodontics (Chic). 2011; 12:222-31. [ Links ]
36. Hyde JD, King GJ, Greenlee GM, Spiekerman C, Huang GJ. Survey of orthodontists' attitudes and experiences regarding miniscrew implants. J Clin Orthod. 2010; 44:481-6. [ Links ]
37. Buschang PH, Carrillo R, Ozenbaugh B, Rossouw PE. 2008 Survey of AAO members on miniscrew usage. J Clin Orthod. 2008; 42:513-8. [ Links ]
38. Markic G, Katsaros C, Pandis N, Eliades T. Temporary anchorage device usage: a survey among Swiss orthodontists. Progress in Orthod. 2014; 15:29-39. [ Links ]
39. Osterman WL. Who places miniscrews? An informal JCO survey. J Clin Orthod. 2008; 45:519-27. [ Links ]
40. Melsen B, Costa A. Immediate loading of implants used for orthodontic anchorage. Clinical Orthodontic Research. 2000; 3:23-8. [ Links ]
41. Melsen B, Verna C. Miniscrew implants: the Aarhus system. Sem Orthod. 2005; 11:24-31. [ Links ]
42. Keim RG, Gottlieb EL, Nelson AH, Vogels DS. 2008 JCO study of orthodontic diagnosis and treatment procedures. Part 1 results and trends. J Clin Orthod. 2008; 42:625-40. [ Links ]
43. Kravitz ND, Kusnoto B. Risks and complications of orthodontic miniscrews. Am J Orthod and Dentofac Orthop. 2007; 131:S43- [ Links ]
44. Park H, Jeong S, Kwon O. Factors affecting the clinical success of screw implants used as orthodontic anchorage. Am J Orthod and Dentofac Orthop. 2006; 130:18-25. [ Links ]
 Correspondence:
Correspondence:
Mosimane Peter Silas Sethusa
P.O.Box 16, Medunsa, 0204
Tel: 012 521 4854
E-mail: Peter.Sethusa@smu.ac.za / orthosethusa@gmail.com













