Serviços Personalizados
Artigo
Indicadores
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares em Google
Similares em Google
Compartilhar
South African Dental Journal
versão On-line ISSN 0375-1562
versão impressa ISSN 0011-8516
S. Afr. dent. j. vol.71 no.7 Johannesburg Ago. 2016
RADIOLOGY CASE
Maxillo-facial radiology case 143
CJ Nortjé
BChD, PhD, ABOMR, DSc. Faculty of Dentistry, University of the Western Cape. E-mail: cnortje@uwc.ac.za
This 30 year old female presented with slight pain and discomfort and intermittent attacks of severe, itching pain in the third quadrant. The affected jaw is enlarged (Figures. 1 & 2). What is your diagnosis?
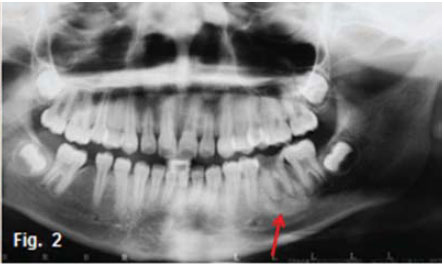
INTERPRETATION
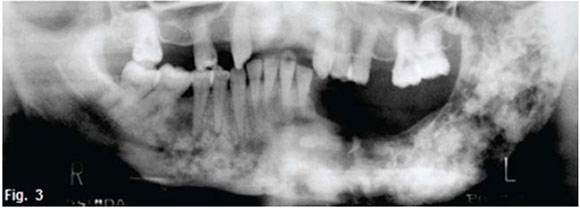
The cropped pantomograph demonstrates a tooth presenting an extensive carious lesion with widening of the periodontal ligament space, and a well circumscribed diffuse radiopaque mass of sclerotic bone surrounding the root apices (red arrow). This is suggestive of focal sclerosing osteomyelitis, also known as condensing osteitis. The condition can be described as a predominantly proliferative reaction occurring in the periapical region as a result of pulpal necrosis. It is rather common, and is usually found in young individuals, especially before the age of 20 years. The mandibular molar teeth seem to be the most frequently involved. Focal sclerosing osteomyelitis is usually asymptomatic, but some patients have mild symptoms. The only classical sign may be a large carious tooth or a large restoration with marginal deficiencies. The second type of sclerosing osteomyelitis is known as diffuse sclerosing osteomyelitis (Figure 3) which is similar to the focal form except that the proliferative reaction is more generalized and commonly results from generalized periodontal disease instead of pulpal degeneration. Diffuse sclerosing osteomyelitis is not a very common condition. It can occur at any age but, in contrast to focal sclerosing osteomyelitis, is more common in older patients, especially black females. It is also more common in the mandible; especially in the edentulous regions. It is usually symptomatic. The patient complains of tenderness and pain in the affected part of the jaw. These exacerbations are usually accompanied by suppuration, elevated temperature and an increased erythrocyte sedimentation rate. In young patients facial asymmetry is a common feature, resulting from swelling along the lower border of the mandible. In summary, sclerosing osteomyelitis can be described as a predominantly proliferative reaction of bone to infection occurring in patients with high host resistance or a low grade infection. The infection acts as a stimulus rather than irritant, producing proliferation instead of destruction. Bone is deposited along existing trabeculae, resulting in thickening of the trabeculae and reduction or obliteration of the marrow spaces. The success of operative treatment is often questionable, and since in many cases there is a tendency to a spontaneous regression, conservative treatment and observation is often recommended.
Reference
1. Farman AG, Nortje CJ & Wood R E: Oral and Maxillofacial Imaging, 1st Ed, Mosby. St. Louis, Missouri 1993 pp. 195-9. [ Links ]













