Serviços Personalizados
Artigo
Indicadores
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares em Google
Similares em Google
Compartilhar
South African Dental Journal
versão On-line ISSN 0375-1562
versão impressa ISSN 0011-8516
S. Afr. dent. j. vol.71 no.5 Johannesburg Jun. 2016
SEDATION
Continuous education in sedation 2: Protecting the airway during sedation
James A RoelofseI; Cherese LapereII; Will BothaIII
IUniversity of the Western Cape, Stellenbosch University, and University College London, London
IISedation Practitioner
IIISedation Solutions, London
Keywords: Airway protection, sedation monitoring, preoperative assessment
INTRODUCTION
Protecting the airway is a critical aspect of safe sedation practice. Sedation practitioners must be able to identify the patient at risk for airway obstruction. We will discuss key aspects of airway evaluation, sedation monitoring, and practical points to prevent compromising the airway during sedation.
DISCUSSION
According to the 2015 SASA Sedation Guidelines for surgical procedures, no patient should be considered for sedation without having undergone a focused airway assessment.1 Becker and Haas state that the most important aspect of patient care is airway management.2
Features that are commonly linked with difficult intubation are also associated with upper airway obstruction during sleep.3 Various evaluation tools are available to assess patency of the airway, e.g. Mallampati classification, LEMON law, Upper Lip Bite Test, and the simplified airway risk index. All factors that can compromise the airway leading to possible difficult bag-valve ventilation (rescue) or difficult intubation should be carefully evaluated. Risk identification for factors that may compromise the airway is essential.4 These include: obesity, maxillary hypoplasia, mandibular abnormalities, beards, edentulous patients, a short thyro-mental distance, restricted mouth opening, large neck circumference and specific obstructive lesions such as nasal obstruction or adeno-tonsillar hypertrophy.
There are particular conditions which preclude surgery-based sedation: for instance patients with severe obstructive sleep apnoea(OSA), poorly controlled respiratory disease (asthma or COPD) or patients with active respiratory tract infections. They may not be ASA 1 or 11 patients who would qualify for sedation outside the operating theatre. Tonsillar hypertrophy and excessive lymphoid tissue in the pharynx are predisposing factors to OSA in children.4
Pre-operative fasting remains a controversial issue. In a sedation technique where dissociative and non-dissociative intravenous techniques are used we suggest that sedation practitioners follow the SASA Guidelines.1 The patient needs to be fasted from solid foods for six hours and from clear fluids (defined as a non-particulate fluid) for two hours before sedation.
Standards of monitoring differ slightly according to the level of sedation provided. Minimal sedation can be monitored with clinical monitoring, deep sedation with the same electronic and clinical monitoring as with general anaesthesia. However, it is important for the sedation practitioner to understand that sedation is a continuum. The more drugs we give the deeper the level of sedation may be. The sedation practitioner must be prepared to rescue any patient that inadvertently slips into a deeper level of sedation.
Moderate sedation levels require continuous monitoring that includes pulse oximetry, heart rate, respiratory rate and breathing pattern, and blood pressure recording. Capnography is said to be the gold standard for monitoring of effective breathing as it is more sensitive than pulse oximetry. It is not mandatory for moderate sedation but highly recommended in patients with respiratory disease, the obese, and where deep sedation is utilized.1
Patients with a tendency to upper airway obstruction during sleep are more vulnerable for airway problems during sedation.4 This is especially so if we are not careful with the doses of sedative drugs used. During the sedation, the practitioner needs to be vigilant to monitor the possible reversible causes of airway obstruction, e.g. amount of pressure from the surgeon on the lower mandible, patient position, pushing the tongue backwards towards the soft palate, and over-extension of the neck, especially in the paediatric population. When a patient is supine, airway obstruction could be worsened due to gravitational effects on the tongue and soft palate. Neck flexion, mouth opening and the "head-down" position often used in dentistry can lead to airway compromise.4 Most patients will also find it difficult to swallow when their mouths are held open wide with a mouth prop or other devices in frequent use in dentistry. Good and effective suctioning, especially focused to the back of the mouth, is therefore vital.
Certain drugs are known to decrease the muscle tone in the upper airway. Propofol and Midazolam are commonly used in sedation practice and are well known for their effects in inhibiting upper airway activity, resulting in airway compromise. Ketamine is probably a better drug if we want to prevent airway compromise. Titration still remains the best option when we administer drugs for sedation.
Opioids and sedation drugs are synergistic and may enhance the respiratory depression caused by opioids. Ketamine seems to protect against hypoventilation when combined with Propofol (Ketofol). Similarly, during the post-operative period, the depression on breathing may be further exacerbated by residual effects of sedative pre-medications as well as any sedation drugs used.5 Protecting the airway means monitoring a patient in recovery until he/she is fully awake and able to maintain breathing.
When administering opioids, according to the SASA sedation guidelines, the specific antagonist, Naloxone, must always be immediately available.1 Pharmacological reversal should be considered as part of the treatment regime when unintentional apnoea occurs during procedural sedation, especially if breathing becomes difficult.2
Various maneuvers can be used when the airway is threatened: Firstly, placing the head in the "sniffing the morning air" (extension of the neck) position decreases the upper airway collapsibility.
Secondly, when displacing the mandible forwards, the tongue will be pulled forwards too and increase the diameter of the retro-lingual and retro-palatal airway. Simply lifting the chin with mouth closure can also assist in increasing pharyngeal dimensions.4
The sedation practitioner and the whole team are responsible to check the presence and working condition of all resuscitation equipment, emergency airway adjuncts and emergency pharmacological agents. Displaying protocols on the management of anaphylaxis and cardiac arrest is strongly advised.6 The facility where sedation is performed must be equipped to meet the requirements of recommended safe sedation practice.1
The review of emergency procedures and protocols are fundamental to all sedation practitioners and members of the sedation team through practical and theoretical training. This highlights the importance of continuous education and training.
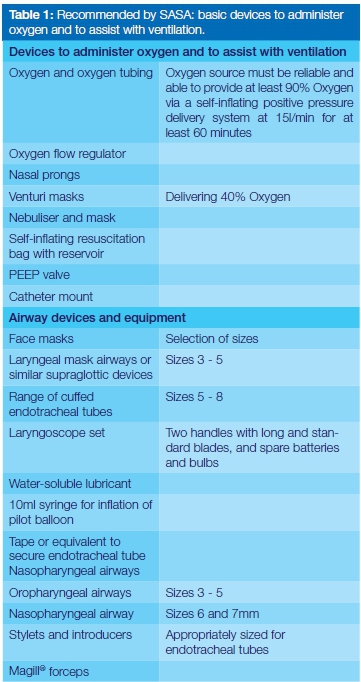
Table 1 is a recommendation from the SASA sedation guidelines of 2015 regarding the basic devices that should be present to administer oxygen and to assist with ventilation during any sedation in any procedure room.1 Sedation practitioners need to take note of this.
CONCLUSION
Adverse events in sedation can generally be prevented by careful preoperative assessment as well as attentive intraoperative monitoring and support.7 Protection of the airway begins with preoperative respiratory considerations, continues throughout the sedation with careful monitoring and immediate support to manage all types of complications as they arise. Collapse of the upper airway is common during sedation especially in the obese patient, and airway maintenance is a fundamental skill essential for those in sedation practice.4
Our next articles will focus on obesity and sedation, and the management of anaphylaxis.
ACRONYMs
ASA: American Society of Anaesthesiologists
COPD: Chronic Obstructive Pulmonary disease
OSA: Obstructive Sleep Apnoea
SASA: South African Society of Anaesthesiologists
References
1. South African Society of Anaesthesiologists Sedation Guidelines 2015. Guidelines for the safe use of procedural sedation and analgesia for diagnostic and. 2015;21(2):1-38. [ Links ]
2. Becker DE, Haas DA. Recognition and management of complications during moderate and deep sedation. Part 1: Respiratory considerations. Anesth Prog [Internet]. [ Links ] 2011;58(2):82-92. Available from: http://www.pubmedcentral.nih.gov/articlerender.fcgi?artid=3198131&tool =pmcentrez&rendertype=abstract\ nhttp://www.pubmedcentral.nih.gov/articlerender. fcgi?artid=3167157&tool=pmcentrez&rendertype=abstract
3. Hiremath AS, Hillman DR, James AL, Noffsinger WJ, Platt PR, Singer SL. Relationship between difficult tracheal intubation and obstructive sleep apnoea. Br J Anaesth. 1998;80(5):606-11. [ Links ]
4. Hillman DR, Platt PR, Eastwood PR. The upper airway during anaesthesia. Br J Anaesth. 2003;91(1):31-9. [ Links ]
5. Pattinson KTS. Opioids and the control of respiration. Br J Anaesth. 2008;100(6):747-58. [ Links ]
6. Mikhael MS, Wray S, Robb ND. Intravenous conscious sedation in children for outpatient dentistry. Br Dent J. 2007;203(6):323-31. [ Links ]
7. Becker DE, Haas DA. Recognition and management of complications during moderate and deep sedation. Part 2: Cardiovascular considerations. Anesth Prog. 2011;58(3):126-38. [ Links ]
 Correspondence:
Correspondence:
James A Roelofse
Private Bag X1, Tygerberg 7505.
Tel: 021 937 3085, C
ell: 083 458 2427.
E-mail: jar@sun.ac.za













